CLINICIAN’S CAPSULE
What is known about the topic?
Few physicians adhere to recommendations surrounding analgesia for pediatric lumbar punctures (LPs).
What did this study ask?
How willing are emergency physicians to provide analgesia for pediatric LPs?
What did this study find?
Compared to older children, the willingness to provide analgesia was suboptimal in a young infant.
Why does this study matter to clinicians?
Knowledge translation should focus on dispelling misconceptions and emphasize the importance of analgesia for young infants undergoing LPs.
INTRODUCTION
Children view lumbar punctures (LPs) as painfulReference Prestes, Balda and Santos 1 and distressing.Reference Po, Benini and Sainati 2 Compared to adults,Reference Menkes and Sarnat 3 subcutaneous lidocaine is underutilized in children,Reference Breakey, Pirie and Goldman 4 despite evidenceReference Baxter, Fisher and Burke 5 - Reference Pillai Riddell, Racine and Turcotte 8 and guidelines supporting its use.Reference Fein, Zempsky and Cravero 9 - Reference Batton, Barrington and Wallman 11 Numerous studies demonstrate a suboptimal provision of analgesia in neonates and children undergoing LPs.Reference Bhargava and Young 12 - Reference Baxter, Welch, Burke and Isaacman 18 However, reasons behind decisions to withhold analgesia remain unknown. With respect to LPs in children, we sought to explore 1) willingness to provide analgesia (particularly, subcutaneous lidocaine) by physicians in general and pediatric emergency departments (EDs), 2) types of analgesia, 3) reasons for withholding analgesia, 4) practitioner anxiety and perceived competence performing LPs, 5) practitioner perceptions of the patient’s pain during LPs, and 6) practitioner comfort with a child life specialist during an LP.
METHODS
Design and participants
This was an online survey of pediatric and general emergency physicians (EPs) listed in the Pediatric Emergency Research Canada (PERC) or Canadian Association of Emergency Physicians (CAEP) database as of January 2016. We hypothesized that there is a suboptimal willingness to provide analgesia to children undergoing LPs, particularly young infants.
Protocol
Potential participants were contacted by email from April 26 to May 31, 2016. According to the Modified Dillman Tailored Design Method,Reference Dillman 19 PERC members received surveys on days 3, 10, 17, 24, and 31. Due to administrative regulations, CAEP members received surveys on days 3, 10, and 38. Consent to participate was implied by the completion of any survey item. This study received approval from the Western University Health Sciences Research Ethics Board.
Instrument
The survey was developed de novo by four investigators (NP, VB, AS, and SA), according to Burns et al.,Reference Burns, Duffett and Kho 20 and available in English and French. It included three clinical vignettes of children who required an LP: a 3-week-old febrile male, a 3-year-old male, and a 16-year-old female, the latter two with with fever, headache, vomiting, and photophobia (see Appendix).
Statistical analysis
The primary outcome was the willingness to provide analgesia for an LP. Data were summarized using descriptive statistics and analysed using SPSS (version 24, Armonk, NY).
RESULTS
Response rate
The PERC and CAEP response rates were 150/222 (67.6%) and 272/1362 (19.9%), respectively.
Willingness to provide analgesia
For a 3-week-old male, 123/144 (85%) pediatric EPs and 231/262 (88%) general EPs reported a willingness to provide analgesia (Table 1). For a 3-year-old male, provision of analgesia was almost universal among pediatric EPs (142/144, 99%) and general EPs (256/262, 97.7%). Subcutaneous local and topical anesthetics were used by 100/144 (69%) and 117/144 (81%) pediatric EPs, respectively, and 207/262 (79%) and 144/262 (55%) general EPs, respectively. Among pediatric EPs compared to general EPs, mean (SD) competence on a 100-mm Visual Analogue Scale was higher [85.7 (14) mm versus 60 (26.5) mm, respectively], and anxiety was lower [32.8 (30) mm versus 56.3 (27.1) mm, respectively]. For a 16-year-old female, the willingness to provide analgesia was endorsed by all but one general EP. Subcutaneous local and topical anesthetics were provided by 117/144 (81%) and 131/144 (91%) pediatric EPs, respectively, and 241/262 (92%) and 61/262 (23.3%) general EPs, respectively. Among pediatric EPs and general EPs, mean (SD) competence was high [83.9 (14) mm and 88.1 (14.8) mm, respectively], and anxiety was low [30.6 (27) mm and 27.9 (24.6) mm, respectively]. Across vignettes and respondents, comfort with a child life specialist was high (>79 mm).
Table 1. Analgesia provision and perceptions for an LP performed on a 3-week-old febrile maleFootnote *
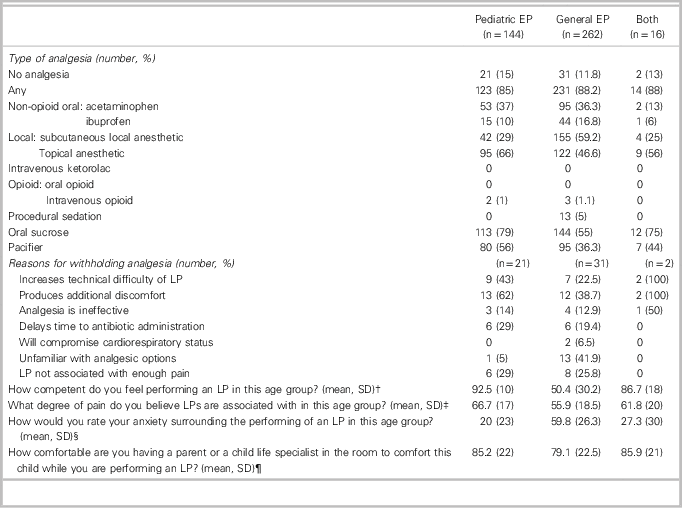
* Respondent could choose more than one option.
† Using a 100-mm Visual Analogue Scale anchored by 0 (not competent) and 100 (very competent).
‡ Using a 100-mm Visual Analogue Scale anchored by 0 (no pain) and 100 (worst pain).
§ Using a 100-mm Visual Analogue Scale anchored by 0 (no anxiety) and 100 (lots of anxiety).
¶ Using a 100-mm Visual Analogue Scale anchored by 0 (not comfortable) and 100 (very comfortable).
EP=emergency physician; LP=lumbar puncture; SD=standard deviation.
DISCUSSION
For an infant undergoing an LP, compared to a toddler and adolescent, there was less willingness to administer analgesia and less use of subcutaneous lidocaine. The American Academy of Pediatrics (AAP) recommends topical analgesia or subcutaneous lidocaine in children undergoing LPs, including neonates.Reference Fein, Zempsky and Cravero 9 Knowledge translation strategies should focus on dispelling misconceptions and improving awareness of analgesic options in young infants.
In young infants, limited use of analgesia for LPs has been describedReference Hoyle, Rogers and Reischman 17 , Reference Baxter, Welch, Burke and Isaacman 18 along with differences in a willingness to use subcutaneous lidocaine between general and pediatric EPs.Reference Quinn, Carraccio and Sacchetti 15 For what we believe refers to subcutaneous lidocaine, misconceptions include increased technical difficulty and producing additional discomfort. However, subcutaneous lidocaine is associated with greater procedural success,Reference Baxter, Fisher and Burke 5 , Reference Pinheiro, Furdon and Ochoa 21 - Reference Nigrovic, Kupperman and Neuman 23 and the risk of “minimal” painReference Fein, Avner and Khine 16 from administering local anesthetic using a 30-gauge needle may be preferable to multiple LP attempts, which are necessary in almost half of young children.Reference Carraccio, Feinberg and Hart 24 The belief that LPs are not painful in young infants has been previously described.Reference Breakey, Pirie and Goldman 4 However, neonates do experience pain from noxious stimuliReference Anand 25 , Reference Johnston and Stevens 26 and with detrimental long-term consequences.Reference Taddio, Katz, Ilersich and Koren 27
Multimodal approaches to analgesia are supported by the AAPReference Fein, Zempsky and Cravero 9 and Canadian Paediatric Society (CPS)Reference Batton, Barrington and Wallman 11 and can involve sucrose plus pharmacologic therapy.Reference Krishnan 28 Despite a lack of evidence for sucrose, its use was more prevalent among pediatric than general EPs (79% versus 55%), suggesting greater familiarity or availability.
General EPs reported less competence and greater anxiety performing LPs in a young infant, possibly explaining their reluctance to administer analgesia in infants. Actual administration of analgesia may be lower than our results suggest because medical record reviews report that 24% to 80% of children receive documented analgesia for LPs.Reference Bhargava and Young 12 , Reference Fein, Avner and Khine 16 , Reference Stevens, Abbott and Yamada 29
Barriers to the administration of analgesia to a young infant include a lack of familiarity with analgesic options (41.9% of general EPs) and a perception that it delays time to antibiotics (28.6% of pediatric EPs). Nurse-initiated protocols that facilitate early administration of topical agents such as MaxileneTM and electronic orders pre-populated with analgesic options may support adequate analgesia and optimal ED flow.
LIMITATIONS
The low CAEP survey response rate limits generalizability to general EPs and may have been due to fewer email reminders. The adequacy of analgesic choices was not reported because there is no clear consensus as to what constitutes adequate analgesia. Finally, non-validated scales were used to measure respondent beliefs surrounding LPs.
CONCLUSION
In contrast to older children, the willingness to provide analgesia for a young infant was not universal. Misconceptions that LPs are not sufficiently painful and incur additional discomfort and technical difficulty must be corrected. Our findings suggest a rationale for nurse-initiated protocols and strategies to improve provider knowledge surrounding analgesia in young infants.
Acknowledgments
This study is supported by the Schulich Research Opportunities Program Grant. This paper was previously presented at the International Forum on Pediatric Pain (IFPP) Annual Meeting in November 2017 in Halifax, NS.
Competing interests
None declared.
SUPPLEMENTARY MATERIAL
To view supplementary material for this article, please visit https://doi.org/10.1017/cem.2018.382



