INTRODUCTION
Hepatitis C virus (HCV) has become a leading cause of chronic hepatitis, cirrhosis and hepatocellular carcinoma [Reference Kim1, Reference Shepard2] with an estimated 170 million people infected worldwide. It is estimated that 26·4 million people are infected in China alone, representing ~2·2% (range 0·52–3·15) of the general population [Reference Xia3]. Deaths related to HCV exceeded deaths related to HIV in the United States [Reference Kim1]. HCV is hyperendemic in injection drug users (IDUs), and the prevalence can be as high as 90% in this population [Reference Xia3, Reference McCarthy and Flynn4]. A meta-analysis showed that the pooled prevalence of HCV infection in IDUs was 61·4% [95% confidence interval (CI) 55·7–67·2, max 98·7] in China, and its prevalence showed marked geographical variation [Reference Xia3]. There have been many studies that have examined the associations between socioeconomic, demographic and drug-related behavioural factors and HCV infection in drug users; however, some of these results are contradictory [Reference Xia3, Reference Zhuang5]. For example, one meta-analysis showed that IDUs sharing needles/syringes had a greater risk of being infected with HCV than non-sharing IDUs [Reference Zhuang5]. However, another meta-analysis indicated that no significant difference was found in the risk of HCV infection between needle-sharing and non-needle-sharing IDUs [Reference Xia3]. Some studies suggested that level of education was independently associated with HCV infection [Reference Paez6, Reference Alter7]; however, other studies showed no such association [Reference Cavlek8, Reference Dursun9]. These inconsistent findings might be the consequence of spatial heterogeneity in the effects or clusters of some risk factors or be related to other potential reasons including the conflicting results from different target populations. Our previous research suggested there was significant global and local geographical autocorrelation in HCV infections [Reference Zhou10]. The spatial autocorrelation, if not accounted for, may result in bias in the estimates and incorrect standard errors [Reference Weidmann11]. Currently, most studies have used non-spatial regression techniques to analyse risk factors of HCV infection making the assumption that the association is stationary across space. Few studies have used spatial regression methods to explore risk factors of HCV infection at the individual level assuming the relationship is non-stationary across space. Therefore, using geographically weighted logistic regression (GWLR), we aim to account for and describe the local variation in the relationship between demographic, socioeconomic and drug-use behavioural characteristics and HCV infection in drug users in an Yi Autonomous Prefecture, Sichuan province, China. This may provide new insights about who is at risk for HCV infection and where. Thus, our analysis is potentially useful for tailoring prevention and healthcare programmes to the needs of diverse groups and for ensuring accessibility of health services to those most in need.
METHODS
Study area and population
The Yi Autonomous Prefecture, located in the southwest of China, is on one of the main drug-trafficking routes from the ‘Golden Triangle’ to northwest and central China. It is one of the largest illicit drug production and distribution centres of China. A population of 4·9 million people live in this prefecture composed of 16 counties and a city and 618 townships. Approximately 50% of the population belongs to the Yi ethnic group. HIV/AIDS has been endemic in this region since the first HIV case was identified in drug users in 1995. Since late 2012, ten regular methadone clinics and one mobile methadone clinic have been established, the first of which was established in 2004. All patients attending the 11 clinics from 2004 to 2012 were selected as the study population, and detailed information on the infrastructure and procedures of these clinics and the patients has been reported elsewhere [Reference Zhou10, Reference Zhou12–Reference Pang16]. All these patients were tested for HCV infection 1 month after first entry into the clinic. Meanwhile, all these drug users were asked to take part in a questionnaire investigation. The questionnaires were administered face-to-face in a private room by a same-sex interviewer who was trained in administration of questionnaires. The information on residency of drug users was collected from their identification card.
Data collection and measurement
Data regarding HCV infection, demographic and socioeconomic factors, drug-use behaviours and residency of all subjects treated in the 11 national clinics during the period 2004–2012 were collected from the national methadone database [Reference Zhuang5, Reference Yin14]. Our outcome variable was HCV infection.
Our independent variables cover three domains of interest. The first domain was drug-use behaviours which include injection, sharing syringes and drug rehabilitation. The second involves demographic factors including gender, age, ethnicity, and marital status. Gender is a dummy variable with female as the reference group. Age was divided into four age groups (<30, 30–39, 40–49, ⩾50 years) where the <30 years group serves as the reference group, and three dummy variables are created. Ethnicity is classified as Yi, Han (reference group) and other using two dummy variables. Marital status was categorized into single (reference), married, divorced and widowed. The third domain focuses on socioeconomic factors, including occupation and education. Occupation was classified into farmer, service sector, unemployed, and other (reference) such as factory worker, government employee, etc. Educational achievement was divided into four levels (three dummy variables): no school (reference group), elementary school, junior high school and senior high school or above. Our independent variables also include ‘methadone clinic’ which was divided into 11 levels.
In order to explore the local associations between HCV infection and risk factors (as mentioned above) at the individual level, the location of each individual was defined as the geographical coordinate (i.e. latitude/longitude) of the centre of the township in which he/she resided; township is the smallest geographical unit in the present analysis.
Statistical analysis
Non-spatial logistical regression
Using SPSS software (SPSS Inc., USA), the prevalence of infection and characteristics of the patients in the methadone clinics were analysed, and multivariable non-spatial logistical regression was employed to analyse the association between HCV infection and risk factors and interactions between variables.
GWLR
A GWLR model was used to analyse the local associations between HCV infection and risk factors adjusting for spatial autocorrelation. The model is figured by [Reference Yang and Matthews17]:
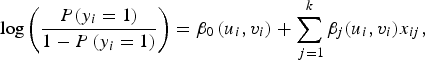 $$\log \left( {\displaystyle{{P({y_i} = 1)} \over {1 - P\left( {{y_i} = 1} \right)}}} \right) = {\beta _0}\left( {{u_i},{v_i}} \right) + \mathop \sum \limits_{\,j = 1}^k {\beta _j}({u_i},{v_i}){x_{ij},}$$
$$\log \left( {\displaystyle{{P({y_i} = 1)} \over {1 - P\left( {{y_i} = 1} \right)}}} \right) = {\beta _0}\left( {{u_i},{v_i}} \right) + \mathop \sum \limits_{\,j = 1}^k {\beta _j}({u_i},{v_i}){x_{ij},}$$
where y i and x ij , denote the HCV infection status and explanatory variables for individual i with location coordinates(u i , v i ), and β 0(u i , v i ) and β j (u i , v i ) are the location-specific intercept and coefficients.
The GWLR model was implemented with GWR 4·0 software (https://geodacenter.asu.edu/software/downloads/gwr_downloads). The kernel function used for geographical weighting to estimate local coefficients is ‘adaptive bi-square’. The bandwidth is the number of nearest neighbours to be included in the bi-square kernel. The ‘golden section search’ method was used to automatically determine the best bandwidth size based on Akaike's Information Criterion (AIC) corrected for small sample size bias, where the bandwidth with the lowest AIC was used in the final analysis. Geographical variability for each coefficient can be assessed by comparing the AICs between the GWLR model and the global logistic regression model assuming invariant model coefficients [Reference Yang and Matthews17]. The coefficient of an independent variable in the model represents the change in log odds of the response given a unit change in that variable. Taking the exponentiation of the coefficient yields the odd ratio (OR) corresponding to a unit change in the variable. The local estimates (OR) and P values are visualized in maps to demonstrate the geographical variations in the association between HCV infection and individual factors. The results are relatively insensitive to the choice of kernel functions (e.g. bi-square and Gaussian) for geographically weighted regression [Reference Yang and Matthews17]. All variables were entered first into the GWLR regression model, then the variable with the largest P value was removed from the model until only the variables with some local P values <0·1 remained within the GWLR model.
RESULTS
Prevalence of HCV infection
A total of 5401 patients with complete information regarding risk factors, home address, name of methadone clinic attended and results of their HCV test were obtained from the national database. These patients came from 405 of the 618 townships of the Yi Autonomous Prefecture. The prevalence of HCV infection in the population was 30·0% (1620/5401). Table 1 presents the infection prevalence of HCV in different characteristics of the national methadone clients. Clients with a history of IDU, or of sharing syringes or of drug rehabilitation had a higher prevalence of HCV infection than those without such a history. Patients who were married, of Yi ethnicity, employed in farming or had no schooling had a lower prevalence of HCV infection than those who were not (Table 1). Additionally, 44·6% of the patients had injection history, and 16·8% (909/5401) shared syringes (Table 1).
Table 1. The characteristics and prevalence of HCV infection of the national methadone clients in southwest China

Univariable and multivariable non-spatial logistical regressions
For the univariable non-spatial logistic regression, other factors were associated significantly with HCV infection except for gender (Table 2).
Table 2. The association of HCV infection and risk factors from univariable and multivariable non-spatial logistical regressions

OR, Odds ratio; aOR, adjusted odds ratio; CI, confidence interval.
For multivariable non-spatial regression, both IDU and drug rehabilitation were significantly (P < 0·001) positively associated with HCV infection [adjusted OR (aOR) 3·04, 95% CI 2·65–3·48; aOR 1·76, 95% CI 1·53–2·03, respectively] in drug-use behaviours (Table 2). Compared to others, both unemployed and service-sector work were significantly (P < 0·01) related to HCV infection (aOR 1·20, 95% CI 1·33–1·91; aOR 1·73, 95% CI 1·25–2·39, respectively) (Table 2). Being married was significantly (P < 0·001) negatively associated with HCV infection (aOR 0·70, 95% CI 0·61–0·81) compared to being single. Having senior high-school education or above was significantly (P = 0·039) positively related to HCV infection (aOR 1·28, 95% CI (1·03–1·59) compared to no school (Table 2).
Multivariable spatial logistical regression
The optimal bandwidth size was 170 (individuals) in this study. The value of AIC in the global regression was 5894·0, whereas AIC = 5707·2 for GWLR. Table 3 presents the factors which were significantly and locally associated with HCV infection. For a factor, the spatial regression model can achieve many local ORs. The minimum, medium and maximum presented in Table 3 were the lowest local ORs, the median local ORs and the highest local ORs among these local ORs, respectively. Of drug-use behaviours, IDU was significantly (P < 0·001) positively associated with HCV infection for all study individuals (Fig. 1), and drug rehabilitation was significantly (P < 0·05) positively related to HCV infection for 94·4% of study individuals in 94·5% of townships (Fig. 1).

Fig. 1. Geographical distribution of adjusted odds ratios of injection history and drug rehabilitation history associated with HCV infection from the geographically weighted logistic regression model.
Table 3. The local association of HCV infection and risk factors from the geographically weighted logistic regression model

OR, Odds ratio.
Of demographic factors, being married was significantly (P < 0·05) negatively associated with HCV infection for 92·8% of individuals compared to those who were single in 81·0% of townships; these townships were mainly distributed in the northeastern counties (Fig. 2). Yi ethnicity was significantly (P < 0·05) negatively related to HCV infection for 71·7% of individuals compared to Han ethnicity in 62% of townships; these townships were mainly distributed in the southeastern counties (Fig. 2). Being female was significantly (P < 0·05) positively associated with HCV infection only in 11·2% of townships, located mainly in counties E and F.

Fig. 2. Geographical distributions of adjusted odds ratios of being married and Yi ethnicity associated with HCV infection from the geographically weighted logistic regression model.
For socioeconomic factors, working in the service sector and unemployment (relative to factory workers and governmental employees) were significantly (P < 0·05) positively associated with HCV infection for only 5·8% of individuals in 14·3% of townships and 3·0% of individuals in 8·1% of townships, respectively; these townships are located mainly in the southern counties (Fig. 3). Senior high-school education or above (relative to no school) was significantly (P < 0·05) positively associated with HCV infection for 57·1% of individuals in 55·2% of townships located in the northeastern counties (Fig. 3).

Fig. 3. Geographical distributions of adjusted odds ratios of HCV infection for service sector and senior high-school education or above from the geographically weighted logistic regression model.
DISCUSSION
The non-spatial and the spatial analyses agreed on the role of IDU as a global (i.e. in the whole Yi Prefecture rather than in a specific township or county) high-risk factor for HCV infection, consistent with previous findings [Reference Xia3, Reference Zhuang5, Reference Paez6, Reference Zhou13, Reference Champion18]. Both models also suggested that sharing syringes might be not an independent predictor of HCV infection in this study population, in accordance with previous studies [Reference Xia3, Reference Thorpe19]. It seemed that the most likely factor affecting the significance of needle-sharing as a risk factor for HCV might be the prevalence of HCV in a given area. Some studies showed that sharing of injection paraphernalia (e.g. cookers, cotton) other than syringes may be an important cause of HCV transmission, and responsible for some proportion of new HCV infections [Reference Thorpe19–Reference Villano21]. These might partly explain why sharing syringes were not associated with the prevalence of HCV infection in half of the observed townships of the Yi Autonomous Prefecture in our previous study [Reference Zhou13]. Interestingly, drug rehabilitation appeared to be a risk factor in both non-spatial and spatial analyses, confirming previous findings [Reference Zhou13, Reference Yen22, Reference Backmund23]. One plausible explanation for this is that the detoxification programmes might increase the frequency of the sharing use of drug injection paraphernalia (cookers, cotton, rinse water, drug solutions) [Reference Chen24]. However, such speculation requires further studies to confirm.
The GWLR model revealed the geographical variations of some risk factors associated with HCV infection which cannot be detected by the non-spatial logistic model. For example, the non-spatial logistic regression analysis suggested that being married was negatively associated with HCV infection, consistent with some studies [Reference Bao25, Reference Kassaian26]. However, other studies suggested that marriage could be a risk factor for, or not related to, HCV infection [Reference Paez6, Reference Dursun9 Reference Abdel-Aziz27]. The spatial model showed that being married was negatively related to HCV infection for individuals primarily of Yi ethnicity living in the northeastern counties [Reference Zhou10], but it was not significantly associated with HCV infection in southern counties where the majority of residents are of Han ethnicity (Fig. 2) [Reference Zhou10]. This geographical variation of marital status associated with HCV infection might be related to the distribution of ethnicity. Whether the effect of marital status depends on ethnicity or culture needs future investigation. Examples of conflicting conclusions in previous studies that are possibly explained by spatial heterogeneity are also seen for the effects of ethnicity [Reference Xia3, Reference Lelutiu-Weinberger28] and gender [Reference Xia3, Reference Zhuang5, Reference Cavlek8, Reference Dursun9].
The non-spatial analysis indicated that senior high-school education or above was an independent risk factor for HCV infection, and the spatial analysis also showed that drug users with senior high-school education or above were more likely to be infected with HCV than those with no school in the northeastern counties of the Yi Autonomous Prefecture. These findings indicated that drug users with senior high-school education or above might be the priority population for intervention, especially in the northeastern counties of the Yi Autonomous Prefecture, like P, Q and R counties where drug users had high HCV infection prevalence [Reference Zhou10].
Our findings have some important implications. First, geographical variations of risk factors associated with HCV infection might provide some guidance for tailoring site-specific intervention strategies to better control or prevent HCV transmission with limited resources. For example, drug users who are single and live in the northeastern counties, where marriage was negatively related to HCV infection, could be prioritized for intervention. Second, it is necessary to conduct health education in IDUs, making them aware of the potential risk of sharing injection paraphernalia in HCV transmission. Third, spatial correlation and heterogeneity should not be ignored in future studies of risk factors for HCV infection.
This study had several limitations. First, it is difficult to confirm whether patients of the methadone clinics are truly representative of the overall population of drug users. There was, however, a study reporting that the HIV prevalence in patients attending methadone clinics is not significantly different from that in drug users who do not attend methadone clinics [Reference Zhuang5], and the prevalence of HIV and HCV infections were significantly correlated across townships in the study area [Reference Zhou10]. Second, the information regarding sexual behaviours was not available, and therefore we were unable to estimate or control for the effects of sexual behaviours on HCV infection. However, homosexuality (especially gay men) was rarely found in this study population, and an aggregate analysis indicated that there is no increased risk of sexual transmission of HCV in heterosexual couples in regular relationships [Reference Tohme and Holmberg29]. The association of HCV infection with IDU may be confounded by increased number of multiple sexual partners with increased likelihood of IDU; however, the significant geographical variation of IDU in the association with HCV infection was not found in our study. Third, the interactions between variables were not analysed in this study because the spatial model cannot currently analyse the interaction. Finally, assigning the same coordinates to everyone in a township might be increase multicollinearity and reduce variance; however, an average of 13·3 patients per township has little impact on both multicollinearity and variance. For example, for injection drug history, the aOR (95% CI 2·65–3·48) from the non-spatial model is also very close to the aOR (95% CI 2·21–4·29) from the spatial model.
CONCLUSION
The geographical variations of some factors like marital status and educational attainment associated with HCV infection were found in drug users in this study area. These geographical variations of risk factors associated with HCV infection might provide some guidance for tailoring site-specific intervention strategies to better control or prevent HCV transmission in areas with limited resources. Spatial correlation and heterogeneity should not be ignored in future studies of risk factors for HCV infection.
ACKNOWLEDGEMENTS
This work was supported by funding from the Shanghai Leading Academic Discipline Project (Project no. B118) in the analysis and interpretation of data.
DECLARATION OF INTEREST
None.









