Histoplasmosis is a systemic mycosis with a worldwide distribution. It is transmitted by inhalation of propagules of the dimorphic fungus Histoplasma capsulatum. Soil is the natural habitat of the fungus and human disease is associated with exposure to infected soil or excreta from birds and bats in endemic areas. The spectrum of disease ranges from asymptomatic acquisition to life-threatening disseminated disease. However, the majority of infections are subclinical [Reference Knox and Hage1]. Notably, histoplasmosis occurs in immunocompromised [Reference Loo2] and healthy individuals [Reference Knox and Hage1]. Clinically significant disease in healthy individuals is often a sequela of exposure to a high inoculum of H. capsulatum [Reference Knox and Hage1].
There are numerous reports of histoplasmosis outbreaks in individuals exposed to accumulated bat faeces, such as workers involved in cleaning or demolishing buildings [Reference Huhn3] or tourists visiting caves containing bats [Reference Oliveira4]. Histoplasmosis is a relatively common fungal disease in Brazil; however, it is not included in Brazil's mandatory disease notification system and no official data on the disease are available. Our group recently participated in a study evaluating the mortality due to systemic mycoses from 1996 to 2006 in Brazil. Histoplasmosis accounted for 4·3% of deaths, but, when associated with AIDS, the frequency increased to 10·1% [Reference Prado5]. During August 2003 to December 2008, bats were either captured with mist nets by the Zoonosis Control Centre–SP (ZCC-SP) as part of the rabies control programme or were sent by individuals and by other zoonosis control centres from other cities in São Paulo State to our centre for study. Some of these sick or injured bats were caught on the ground. The species recognition of the bats was made according to the identification key of Vizotto & Taddei [Reference Vizotto and Taddei6].
The city of São Paulo is the largest economic centre in Brazil and the most populous city of South America, with about 10·9 million inhabitants in an area of 1523 km2. The other cities in the state of São Paulo that participated in the study are Guarulhos with 1·2 million inhabitants (area 318 km2); Osasco with 700 000 inhabitants (area 65 km2); Jundiaí with 340 000 inhabitants (area 432 km2); and Mogi Mirim with 84 000 inhabitants (area 499 km2) [7].
Bats captured and sent to ZCC-SP were anaesthetized with ketamine (80 mg/kg), euthanized in a CO2 chamber and transferred to a laminar flow hood with air released through a HEPA filter (class II biosafety hood). The spleens and livers were aseptically removed and macerated in saline with chloramphenicol (200 mg/l). Each organ sample was cultured on brain heart infusion agar with chloramphenicol supplemented with 0·1% l-cysteine and 1% glucose and Sabouraud dextrose agar at 25°C and 37°C. The cultures were incubated for 60 days and observed weekly. Bats sent from outside the ZCC-SP were similarly processed immediately after receipt. The Scientific Committee of the Zoonosis Control Center and the ethical committee of the Institute of Biomedical Sciences of the University of São Paulo approved the study.
Presumptive colonies of H. capsulatum were plated on Mycosel agar for identification of the isolated fungi. After growth of colonies, slide micro-cultivation was performed and the characteristic structures of the fungi were identified to confirm the diagnosis.
A total of 2427 bats were collected. The majority (1728, 71·2%), were from the city of São Paulo and 699 (28·8%) were from neighbouring cities. H. capsulatum was recovered from 87 bats (3·6% of all bats examined). Infected bats were identified from five cities: São Paulo (70 bats, 80·5% of total infected bats), Guarulhos (10 bats, 11·5% of total infected bats), Jundiaí (four bats, 4·6% of total infected bats), Osasco (two bats, 2·3% of total infected bats) and Mogi Mirim (one bat, 1·1% of total infected bats).
The families of bats captured were Molossidae (1391 bats), Phyllostomidae (812 bats), Vespertilionidae (203 bats) and Emballonuridae (one bat). Twenty bats had no family identified. Twenty-three genera and 42 species of bats were identified. Gender determination identified 1126 males and 1279 females, with an additional 22 bats in which gender could not be determined. All 87 isolates of H. capsulatum were from bats in the Molossidae family (four genera and five species), which represented the largest group examined (57·3%). Sixty-four (62%) isolates were from Molossus molossus (18 males, 56 females), while the other four infected species were Nyctinomops macrotis (one male and nine females), M. rufus (one male), Tadarida brasiliensis (one male) and Eumops glaucinus (one male). We also determined bat age by assessing forearm epiphyses, since it is cartilaginous in immature bats and calcified in adults. Eight of the bats were young and 79 were adult.
The gender difference in infected animals is statistically significant (χ2 test, P=15·67, α=5%). The female predominance is presumably related to the longer time spent in the colony in care of the offspring, with increased time of exposure to H. capsulatum spores. In some species like N. macrotis, females live in maternity colonies from which males are segregated, which may also contribute to increased contamination of the females. Further study is necessary to validate this hypothesis.
The fact that the Molossidae family represented the largest group of bats examined was expected because this family is the most common in the urban area of São Paulo [Reference Pacheco8]. M. molossus was the most frequent species identified and this species is known to frequently shelter in roofs and ceilings of houses and other spaces within buildings. Therefore, the number of complaints about this bat is greater, resulting in increased capture by the ZCC-SP.
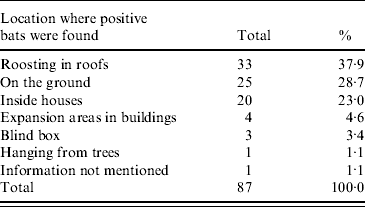
Infected or sick bats were captured in diverse environments. Locations for capture were in roofs, on the ground, inside houses, around the external area of houses, within blind boxes, and hanging from trees. Table 1 details the number of bats captured and the different types of location. Notably, most bats that had fungi in the organs were apparently healthy. In contrast, the bats caught on the ground appeared sick.
Table 1. Collection location for bats infected with H. capsulatum in São Paulo State from August 2003 to December 2008
The majority of infected bats were captured roosting in roofs in areas of dense human population, consequently increasing the risk of individuals in these areas for histoplasmosis. Importantly, the risk depends on the degree of exposure to contaminated soil or guano and the immunological status of the individual, such that high inoculum exposure and immunodeficiency significantly increase the risk of a life-threatening disease [Reference Knox and Hage1, Reference Loo2]. Several species of bats with systemic histoplasmosis have protracted excretion of viable fungi in their faeces [Reference Hoff and Bigler9]; however, it is possible that there is inter-species variation.
Of the five infected bat species identified in the present work, H. capsulatum infection has previously been reported in T. brasiliensis and M. molossus [Reference Canteros10]. This report is the first to identify histoplasmosis in N. macrotis, E. glaucinus and M. rufus. In 2007, histoplasmosis was identified in two N. macrotis and one E. glaucinus captured in the same shelter. Such findings underscore the risk to public health of urban shelters infected with bats and clearly indicate the urgent need for regular surveillance in these areas. The knowledge of the natural history of histoplasmosis in urban areas is important for the establishment of preventive strategies and disease control.
ACKNOWLEDGEMENTS
The following trainees provided assistance to perform the present study: Rodrigo Fernandes de Barros, Leyva Cecília Vieira de Melo, Leonardo Carvalho do Prado Nogueira. The authors acknowledge the technical support of Miriam Marto Sodré, Lyone Monica Suh and bioinformatics assistance by Maria Lucia de Oliveira, from the Zoonosis Control Center of São Paulo Municipality. The authors also acknowledge the management support from Marilene Fernandes de Almeida and Elisa San Martin Mouriz Savani. This work was supported by grants from FAPESP 06/58210-7 and 07/07588-2. C.P.T. and L.R.T. are research fellows of the CNPq.
DECLARATION OF INTEREST
None.



