Introduction
Primary health care (PHC) patients who are psychologically distressed often present with a combination of depressive, anxious and somatic symptoms (Lieb et al., Reference Lieb, Meinlschmidt and Araya2007; Löwe et al., Reference Löwe, Spitzer, Williams, Mussell, Schellberg and Kroenke2008; Hanel et al., Reference Hanel, Henningsen, Herzog, Sauer, Schaefert, Szecsenyi and Löwe2009). However, the predominant classifications of mental disorders, the International Classification of Diseases (ICD-10) (World Health Organization, 1992) and the Diagnostic and Statistical Manual of Mental Disorders (DSM 5) (American Psychiatric Association, 2013), do not provide a way to integrate these aspects of clinical presentations. To improve the assessment of common mental health disorders by PHC professionals, future classification systems need to provide categories that better correspond to clinical presentations in PHC settings.
The World Health Organization (WHO), as part of the revision of the ICD-10, is currently preparing the Eleventh International Classification of Mental Disorders for Primary Health Care (ICD-11 PHC) (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016). Two of the newly proposed diagnoses, anxious depression (AD) and bodily stress syndrome (BSS), have been tested through field trials in PHC settings of five large countries (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016, Reference Goldberg, Reed, Robles, Bobes, Iglesias, Fortes, Mari, Lam, Minhas, Razzaque, Garcia, Rosendal, Dowell, Gask, Mbatia and Saxena2017a, Reference Goldberg, Reed, Robles, Bobes, Iglesias, Fortes, Mari, Lam, Minhas, Razzaque, Garcia, Rosendal, Dowell, Gask, Mbatia and Saxena2017b). The inclusion of a single diagnosis of AD was supported by many studies that showed the high co-occurrence of depression and anxiety in PHC (Üstün and Sartorius, Reference Üstün and Sartorius1995; Kessler et al., Reference Kessler, Brandenburg, Lane, Roy-Byrne, Stang, Stein and Wittchen2005). A screening instrument has been developed for the identification of depression and anxiety based on two short 5-item scales suitable for administration by primary care physicians (PCPs) in settings where administration of written questionnaires may not be feasible (Goldberg et al., Reference Goldberg, Lam, Minhas, Razzaque, Robles, Bobes, Iglesias, Fortes, Mari, Gask, García, Dowell, Rosendal and Reed2012, Reference Goldberg, Reed, Robles, Minhas, Razzaque, Fortes, Mari, Lam, Garcia, Gask, Dowell, Rosendal, Mbatia and Saxena2017b).
Additionally, current diagnostic constructs for somatoform disorder, somatization disorder and medically unexplained symptoms have generated controversy regarding their clinical utility and validity. Arguments against these constructs include the following: (a) a lack of construct and predictive validity; (b) poor discriminant validity due to high comorbidity with mood and anxiety disorders and their overlap with functional somatic syndromes (irritable bowel syndrome, chronic fatigue syndrome and fibromyalgia); (c) particularly in the case of medically unexplained symptoms, the fact that the construct is based on the exclusion of medical etiologies rather than on positive biopsychosocial features; and (d) these constructs do not facilitate a positive therapeutic dialogue between clinicians and patients because they are unhelpful in describing symptoms and their causes and imply that patients exaggerate or imagine their symptoms (Kroenke, Reference Kroenke2007; Kroenke et al., Reference Kroenke, Sharpe and Sykes2007; Tófoli et al., Reference Tófoli, Andrade and Fortes2011).
BSS is a disorder proposed for the ICD-11 PHC to replace the ‘Medically Unexplained Symptoms’ diagnosis in the previous version of the classifications for PHC (ICD-10 PHC) (Lam et al., Reference Lam, Goldberg, Dowell, Fortes, Mbatia, Minhas and Klinkman2013). The change is based in part on studies carried out by Fink et al. (Reference Fink, Toft, Hansen, Ørnbøle and Olesen2007), who examined the latent structure of somatic symptoms not explained by known physical pathology. BSS provides a single overall category for different ‘functional’ and somatoform disorders that could be exacerbated by stress rather than being distinct diseases of non-cerebral pathology. For the ICD-11 PHC, the BSS defines the presentation of three or more somatic symptoms that are associated with distress and/or interference with daily functioning and are not explained by a known physical pathology (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016).
Using a standardized psychiatric interview, the field trials of the ICD-11 PHC showed that 80.1% of patients who met the definition of BSS had depressive or anxious comorbidity, most commonly AD (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016). These results and the observed overlap between depressive and anxious symptoms observed in a subsequent study (Goldberg et al., Reference Goldberg, Reed, Robles, Minhas, Razzaque, Fortes, Mari, Lam, Garcia, Gask, Dowell, Rosendal, Mbatia and Saxena2017b) raise questions about the extent to which BSS, depression, and anxiety represent distinct phenomena in primary care patients. Only one study has analyzed structural models to explain the relationship between somatoform and emotional disorders in PHC patients (Simms et al., Reference Simms, Prisciandaro, Krueger and Goldberg2012). This study found that a hierarchical bi-factor model was the best fit for the data. Depressive, anxiety and somatic symptoms were all loaded onto a general factor, along with three specific depressive, anxiety and somatic factors. This suggested the presence of a broad internalizing factor linking diverse emotional disorders and somatic complaints.
The purpose of this study was to investigate whether the depressive, anxiety and somatic symptoms proposed for BSS and AD in the ICD-11 PHC could be used in PHC as reliable indicators of these disorders. With this aim, we tested the fit and reliability of dimensional models of ICD-11 PHC depressive, anxious and somatic symptoms presented by participants of the ICD-11 PHC field studies.
Methodology
Data were collected as part of field studies for the ICD-11 PHC conducted between October 2013 and July 2015 in Brazil (São Paulo and Rio de Janeiro), the People's Republic of China (Hong Kong), Mexico (Jalisco), Pakistan (Rawalpindi) and Spain (Oviedo). This cross-sectional study consisted of three parts: (1) an evaluation of proposed brief scales for the identification of depression, anxiety, and AD in primary care (Goldberg et al., Reference Goldberg, Reed, Robles, Minhas, Razzaque, Fortes, Mari, Lam, Garcia, Gask, Dowell, Rosendal, Mbatia and Saxena2017b); (2) an evaluation of the proposed ICD-11 PHC categories of BSS and health anxiety and the relationship between these phenomena and depressive and anxiety disorders (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016); and (3) an evaluation of PCPs’ views and implementation of the proposed changes in these two areas for ICD-11 PHC (Lam et al., Reference Lam, Goldberg, Dowell, Fortes, Mbatia, Minhas and Klinkman2013; Goldberg et al., Reference Goldberg, Reed, Robles, Bobes, Iglesias, Fortes, Mari, Lam, Minhas, Razzaque, Garcia, Rosendal, Dowell, Gask, Mbatia and Saxena2017a). Data included in the present analyses were collected during the second part of the study.
All procedures used in these studies were approved by the WHO Research Ethics Review Committee and the appropriate local institutional review bodies in every participating country.
Participants
PCPs were instructed by local investigators to refer adult patients (older than 18 years) seen in a routine PHC practice for participation in the study. The inclusion criterion for part 2 was the presence of at least three somatic symptoms not accounted for by a known physical pathology, as rated by the PCP on a checklist that included 29 somatic symptoms under study for the proposed ICD-11 PHC diagnosis of BSS. PCPs could write in additional symptoms not listed, which also counted toward the minimum of three. (See section on Measures, below.)
Patients who agreed to participate were referred to a trained Research Assistant who, after explaining the procedures and obtaining informed consent, administered a computer-guided interview consisting of the Clinical Interview Schedule-Revised (CIS-R) (Lewis et al., Reference Lewis, Pelosi, Araya and Dunn1992), the 12-item WHO Disability Assessment Schedule 2.0 (WHODAS 2.0) (World Health Organization, 2010), and the 5-item anxiety and depression scales (Goldberg et al., Reference Goldberg, Reed, Robles, Minhas, Razzaque, Fortes, Mari, Lam, Garcia, Gask, Dowell, Rosendal, Mbatia and Saxena2017b) containing the symptoms proposed for depression and anxiety for the ICD-11 PHC.
The procedures for part 2 of the study and sample characteristics have been described in more detail elsewhere (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016).
Measures
We analyzed the latent structure and reliability of the item-level symptom data related to depression, anxiety and somatic symptoms using the two 5-item depression and anxiety scales administered by the Research Assistants and the 29 somatic symptom items rated by the PCPs.
5-item depression and anxiety scales
Depression and anxiety were assessed using two 5-item scales originally developed based on a study of PHC patients in 14 countries (Goldberg et al., Reference Goldberg, Lam, Minhas, Razzaque, Robles, Bobes, Iglesias, Fortes, Mari, Gask, García, Dowell, Rosendal and Reed2012). These scales were applied and validated against a structured diagnostic interview (Goldberg et al., Reference Goldberg, Reed, Robles, Minhas, Razzaque, Fortes, Mari, Lam, Garcia, Gask, Dowell, Rosendal, Mbatia and Saxena2017b). The scales address depressive and anxiety symptoms that have been suggested for the assessment of the new AD category of the ICD-11 PHC (Lam et al., Reference Lam, Goldberg, Dowell, Fortes, Mbatia, Minhas and Klinkman2013). Each scale includes two screening questions, with three additional questions to be asked if the reply to either of these is positive. (More details regarding the two 5-item scales can be found in Goldberg et al., Reference Goldberg, Reed, Robles, Minhas, Razzaque, Fortes, Mari, Lam, Garcia, Gask, Dowell, Rosendal, Mbatia and Saxena2017b).
Somatic symptoms screening
The somatic symptoms screening test contains a list of 29 somatic symptoms including those proposed by Fink et al. (Reference Fink, Toft, Hansen, Ørnbøle and Olesen2007) for the assessment of BSS. There are nine gastrointestinal symptoms, seven cardiorespiratory symptoms, eight musculoskeletal symptoms and five symptoms described as ‘general symptoms’ (headache, dizziness, memory impairment, concentration difficulties and fatigue). The PCPs indicated whether these symptoms were present and whether there was a medical explanation for the symptoms.
CIS revised
ICD-11 PHC diagnostic criteria were generated based on the CIS-R applied by research assistants. The Programmable Questionnaire System (PROQSY) CIS-R is a computerized version of the CIS (Lewis et al., Reference Lewis, Pelosi, Araya and Dunn1992), a fully structured interview designed to be used by lay interviewers to assess ICD-10 diagnoses. For this study, the algorithms were adapted to generate ICD-11 PHC diagnoses of AD, current anxiety, depressive episode and sub-threshold anxious depression (when significant symptoms of both anxiety and depression are present, but the diagnostic requirements for depression or current anxiety separately are not met) and no diagnosis.
12-Item WHO disability assessment schedule 2.0
This is a brief version of the 36-item scale developed by the WHO to rate disability levels experienced over the past 30 days due to health conditions. The 12-item scores were summed to generate a total score between 0 (no disability) and 48 (maximum disability).
Data analysis
In total, 797 patients presenting with somatic symptoms not explained by known physical pathology completed the study procedures. To examine the latent structure of depressive, anxiety and somatic symptoms presented by primary care patients, we used the Mplus software package, Version 7.4 (Muthén and Muthén, Reference Muthén and Muthén1998–2015), to perform confirmatory factor analyses (CFA). CFA are used to provide construct validity of psychological scales by correlating a set of continuous latent measures underlying sets of observed variables (i.e. items or symptoms in a questionnaire) (Brown, Reference Brown2015). Under the CFA approach, different models might be specified and tested regarding their reliability and fit. In a bi-factor model, a general factor reflects the target construct assessed by all the symptoms and the orthogonal (i.e. not correlated) group-specific factors (depression, anxiety and somatization in this case) represent subdomain constructs based on clusters of items with similar content (Rodriguez et al., Reference Rodriguez, Reise and Haviland2016a). The bi-factor model evaluates the unique contributions of the general factor and specific factors to scale each individual on a single trait, but at the same time, controls for the distorting effects of multi-dimensionality caused by specific item content (Reise et al., Reference Reise, Moore and Haviland2010). Thus, to assess whether a bi-factor model could explain the structure of depressive, anxious and somatic symptoms presented by PHC patients, it is important to understand the specific contribution of each construct of the model on symptom variances (Reise, Reference Reise2012) (i.e. how reliable and viable each specific domain is).
Simms et al. (Reference Simms, Prisciandaro, Krueger and Goldberg2012) provided a statistical explanation of why the bi-factor model was expected to be the best fitting latent structure for similar data when compared with other multi-dimensional models. This specification of the model is also aligned with the idea of the P-factor (Caspi et al., Reference Caspi, Houts, Belsky, Goldman-Mellor, Harrington, Israel, Meier, Ramrakha, Shalev, Poulton and Moffitt2012; Martel et al., Reference Martel, Pan, Hoffmann, Gadelha, do Rosario, Mari, Manfro, Miguel, Paus, Bressan, Rohde and Salum2017) to explain the comorbidity across mental disorders, where a general factor of psychopathology – the P-factor – accounts for meaningful variance across major forms of hundreds of psychiatric symptoms.
Based on this rationale, CFA were conducted to evaluate two bi-factor models of the latent structure of anxiety, depression and somatic symptoms by using the items of depression and anxiety scales as a proxy for depression and anxiety symptoms, respectively, and the somatic symptoms screening as a proxy for somatization. Two orthogonal models were tested, where correlations among factors were set to zero: (1) Model 1, where a general factor was loaded on each symptom along with three depression, anxiety and somatization specific factors and (2) Model 2, where a general factor was loaded on each symptom along with two anxious depression and somatization specific factors. The weighted least squares (WLSMV) estimator was used due to categorical observed indicators (i.e. set of items) specifying the variable nation as a cluster indicator dealing with complex structured data (i.e. participants nested in nations) as suggested by Asparouhoy (Reference Asparouhov2005, Reference Asparouhov2006). The evaluation of the model's fit was conducted using the following indices: the Chi-Square Test of Model Fit (p > 0.05), the Root Mean Square Error of Approximation (RMSEA < 0.06), the Comparative Fit Index (CFI > 0.90) and the Tucker–Lewis Index (TLI > 0.90) (Brown, Reference Brown2015).
Reliability and viability of the general and specific factors
Beyond examining model fit, it is important to evaluate the interpretability of total and subscale scores in a bi-factor model. That is, whether it is meaningful to report subscale scores in the presence of multi-dimensionality. This is typically assessed using reliability indices (Rodriguez et al., Reference Rodriguez, Reise and Haviland2016a). When fitting a bi-factor model, three sources of symptoms variance might be specified: (1) those related to the general factor; (2) those related to specific factors; and (3) those related to error (aka. residual variance). The purpose of the reliability analysis is to determine whether the symptoms proposed for depression, anxiety and somatic symptoms are reliable indicators of these domains. To evaluate reliability, the following indices were considered (Rodriguez et al., Reference Rodriguez, Reise and Haviland2016a, Reference Rodriguez, Reise and Haviland2016b): (1) explained common variance (ECV), which is an index of uni-dimensionality of the model (a ratio of the variance explained by the general factor divided by the variance explained by the general and the specific factors); (2) Lucke's omega, which indicates the percentage of total score variance (of the three scales) that can be attributable to all factors modeled and represents the reliability of the model; (3) the hierarchical omega coefficient, which indicates the degree to which each scale is interpretable as a measure of a single common factor; and (4) omega subscales to indicate the reliability of the subscale score remaining on the specific factor once the effects of the general factor are removed. Values of the omega indices can vary between 0 and 1, where higher scores indicate greater reliability. Key details about each index are described in Rodriguez et al. (Reference Rodriguez, Reise and Haviland2016a, Reference Rodriguez, Reise and Haviland2016b).
External validity
To test the external validity of the specified structural model, we analyzed the relationship between the latent structure of the models with ICD-11 PHC diagnoses and disability. The latent factors (the general measure and the specific factors) were used as predictors of AD compared with a depressive episode, current anxiety, sub-threshold anxious depression and no diagnosis using ICD-11 PHC criteria. For this analysis, the used estimator was the Maximum Likelihood generating then a logistic regression model estimating the subsequent Odds Ratio. Linear regression was modeled where the outcome variable was disability level (WHODAS 2.0 total score).
Results
Structural analyses
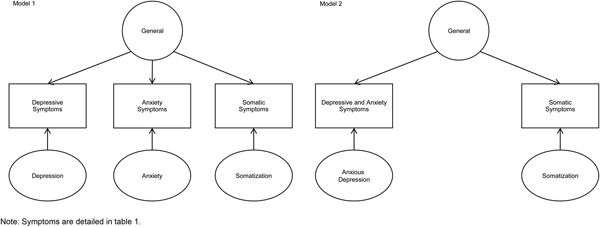
Both bi-factor specified models (Fig. 1) with all symptoms loading simultaneously on a general factor, along with one of three depression, anxiety and somatic specific factors (Model 1) or two anxious depression and somatic specific factors (Model 2), fit well to the data. For both models, the inclusion of item 5 of the depression scale regarding suicidal ideation resulted in unidentified models in the CFA. As Simms et al. (Reference Simms, Prisciandaro, Krueger and Goldberg2012) excluded this symptom for depression in PHC patients in their model, due to the low rates of its presentation, we also decided to exclude this item from our models. Because both models have the same number of degrees of freedom, they are not comparable one with each other.
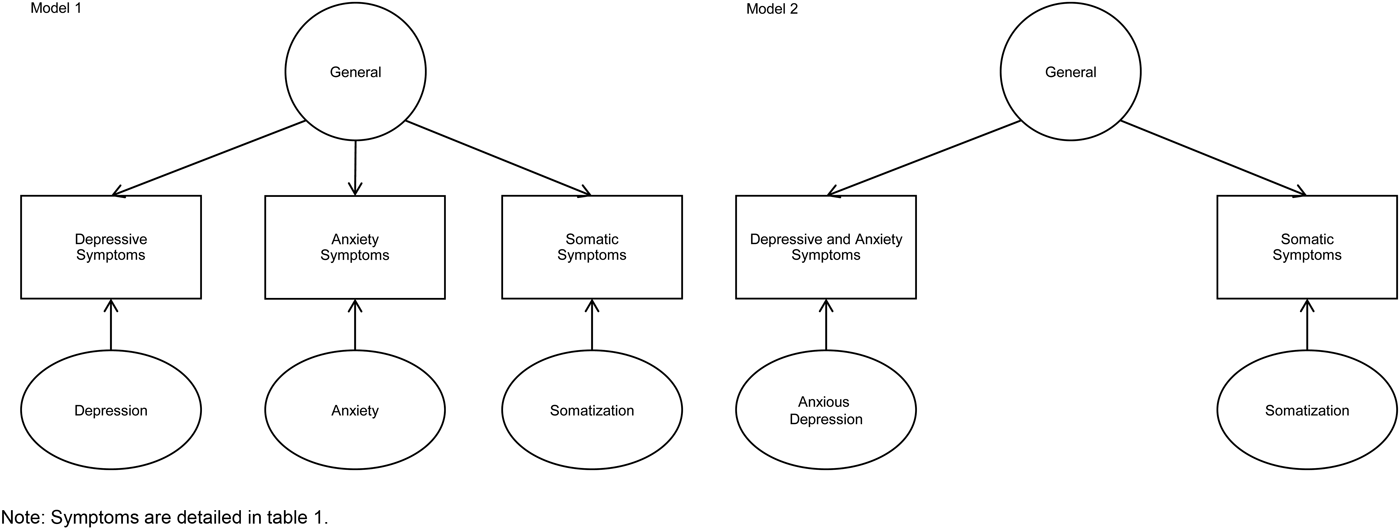
Fig. 1. Diagrams representing the bi-factor models structure underlying the depressive, anxiety and somatic symptoms in PHC patients.
Figure 1 shows the diagrams of both models. Model 1 with three depression, anxiety and somatic specific factors had the following fit indices: x 2 (627) = 741.016, p < 0.0011, RMSEA = 0.015, (CI90% = 0.010–0.019), CFI = 0.911, TLI = 0.900. Model 2 with two anxious depression and somatic specific factors had the following fit indices: x 2 (627) = 663.065, p = 0.1543, RMSEA = 0.008, (CI90% = 0.000–0.014), CFI = 0.954, TLI = 0.948.
Table 1 presents the prevalence of symptoms and the standardized factor loadings for both the general and specific factors of Models 1 and 2. Standardized factor loadings represent the degree to which each item is associated with its underlying factor; values closer to 1 represent stronger correlations with the underlying factor. In Model 1, depressive and anxiety specific factor loadings were higher than those accounted for by the general factor. Somatic symptoms had similar factor loadings on the general factor and the somatic specific factor, with the exception of gastrointestinal symptoms, where the factor loadings were higher on the somatic specific factor. The general symptoms (headache, dizziness, memory impairment, concentration difficulties and fatigue) had higher factor loadings on the general factor than on the somatic specific factor. In Model 2, when depressive and anxiety symptoms were considered to correspond to the same dimension, the specific factor loadings were also higher on the anxious depression factor but lower on the somatic specific factor. The screening items of the depression scale had slightly higher loadings on the general factor compared with anxiety items. In contrast, somatic symptoms had higher factor loadings on the general factor (with the exception of ‘diarrhea’) and lower on the somatic specific factor.
Table 1. Rates, general and specific factors loadings of each symptom and reliability indices of the models.
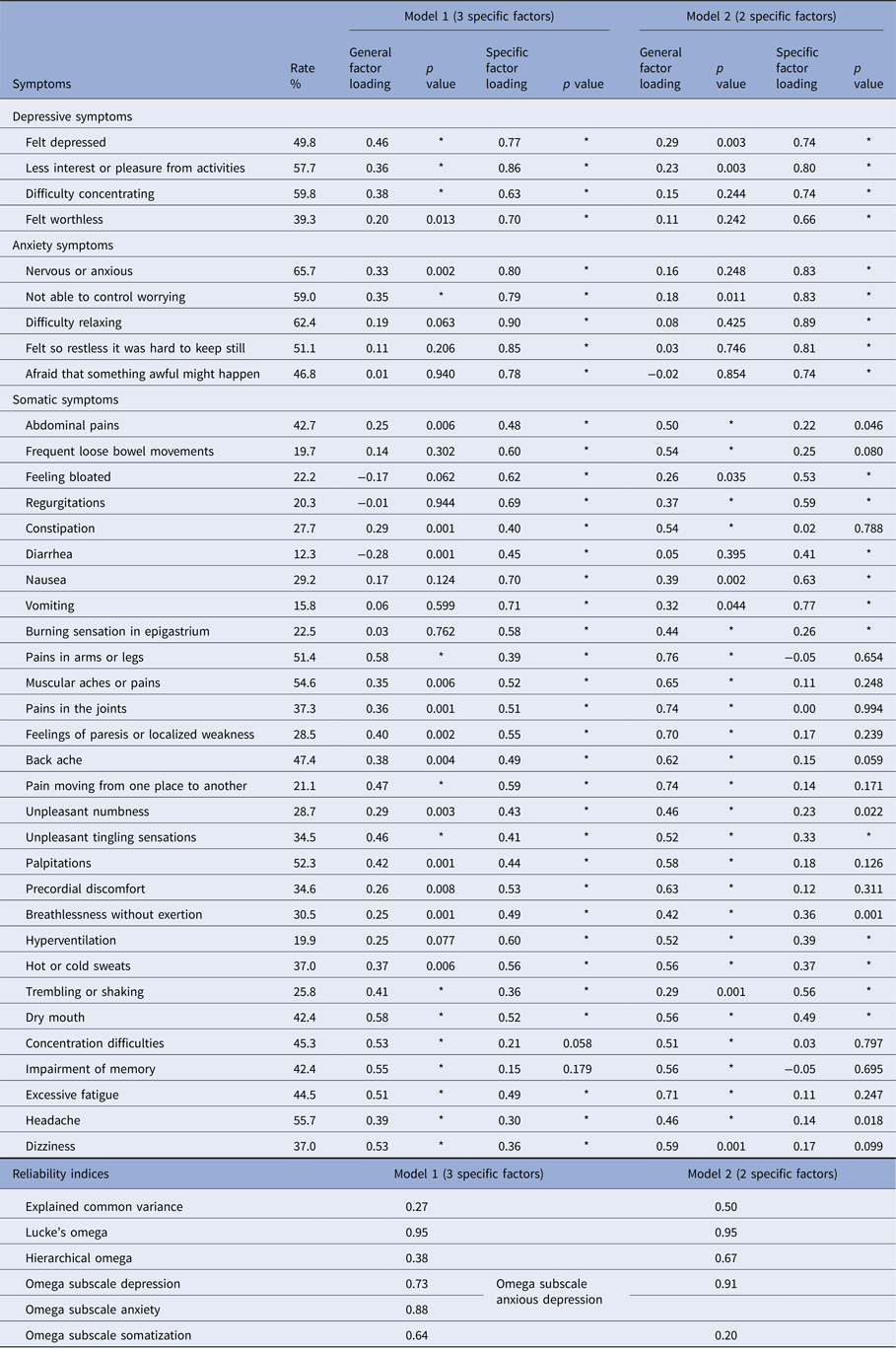
*p value <0.001.
Reliability and subscales viability
Table 1 shows the reliability indices of both models. Even when Model 2 showed higher ECV, both models could be considered as measurements of multi-dimensional models. In both models, Lucke's omega was 0.95, indicating that all common factors modeled accounted for 95% of the total symptom variance, and only 5% of the variance was due to random error. The hierarchical omega in Model 2 demonstrates that 67% of the total symptom variance can be attributed to individual differences in the general factor. In Model 1, the general factor showed less contribution to the symptom variances (hierarchical omega = 0.38). Regarding omega subscales, in Model 1, depression, anxiety and somatic symptom variances were associated predominantly with specific depression and anxiety factors after controlling for the general factor (omega subscale depression = 0.73; omega subscale anxiety = 0.88) and were moderately associated with the somatic specific factor (omega subscale = 0.64). This supports the claim that depression and anxiety scales are reliable indicators of these dimensional constructs. In Model 2, depression and anxiety symptom variances were associated predominantly with the specific anxious depression factor after controlling for the general factor (omega subscale anxious depression = 0.91). In contrast, somatic symptom variance had a smaller association with the somatic specific factor after controlling for the general factor (omega subscale somatization = 0.20). These results suggest that the somatic symptom variance is mainly explained by individual differences in the general factor and had only a residual relation with a specific dimension of somatization. Thus, considering these reliability indices, the somatic symptom subscale score would be considered an ambiguous reflection of that dimension, justifying the assessment of anxious depression in order to achieve a more accurate evaluation of a primary care patient who presents with somatic symptoms not explained by known physical pathology. In contrast, variation in anxious depression subscale scores can be attributed mainly to individual differences in an anxious depression specific dimension.
External validation of the models
Regression analyses were conducted to assess the relationship between the latent factors (the general measure and the specific factors) of the models with ICD-11 PHC diagnoses (assessed by the CIS-R) and disability (WHODAS 2.0 scores). For Model 1, the general factor strengthened the likelihood of AD diagnosis as compared with no diagnosis (OR 7.93, CI95% = 1.26–49.82, p = 0.03) and compared with current anxiety (OR 2.93, CI95% = 0.99–9.70, p = 0.05) but did not increase the likelihood compared with depression (p = 0.36) and sub-threshold anxious depression (p = 0.11). These findings suggest that AD, depression and sub-threshold anxious depression can be parsimoniously modeled as a single general syndrome that encompasses depression, anxiety and somatic symptoms. The levels of the depression specific factor increased the likelihood of an AD diagnosis compared with depression (OR 2.65, CI95% = 1.35–5.21, p = 0.01) and current anxiety (OR 2.83, CI95% = 1.26–6.36, p = 0.01) but remained the same for sub-threshold anxious depression (p = 0.34) and no diagnosis (p = 0.43). The anxiety specific factor reduced the odds of having an AD diagnosis compared with current anxiety diagnosis (OR 0.57, CI95% = 0.38–0.86, p = 0.01). The somatic specific factor predicted the occurrence of AD compared with no diagnosis (OR 2.08, CI95% = 1.05–4.13, p = 0.04) and current anxiety (OR 1.40, CI95% = 1.11–1.75, p < 0.001). The levels of somatic factor were similar for depression (p = 0.61), sub-threshold anxious depression (p = 0.94) and AD.
For Model 2, the general factor strengthened the likelihood of AD diagnosis compared with current anxiety (OR 4.98, CI95% = 1.47–16.90, p = 0.01) but did not increase the likelihood compared with depression (p = 0.31) and sub-threshold anxious depression (p = 0.65). For this model, the relationship between diagnosis and the specific factors was found only for the somatic specific factor, where higher levels of this factor strengthened the likelihood of an AD diagnosis compared with no diagnosis (OR 2.09, CI95% = 1.24–3.53, p = 0.006). Regarding disability levels, in Model 1, WHODAS 2.0 scores were predicted by the general factor (β = 0.34, CI95% = 0.16–0.52, p < 0.001) and by the depression specific factor (β = 0.27, CI95% = 0.03–0.51, p = 0.025) in a statistically significant manner, whereas anxiety and somatization specific factors failed to correlate with disability (β = 0.06, CI95% = −0.21 to 0.32, p = 0.669; β = 0.18, CI95% = −0.08 to 0.44, p = 0.178, respectively). For Model 2, disability levels were predicted by the general factor (β = 0.38, CI95% = 0.23–0.52, p < 0.001) in a statistically significant manner, whereas for the specific factors, we found a lack of statistical significance for the anxious depression specific factor (β = 0.18, CI95% = −0.08 to 0.43, p = 0.18) and the somatic specific factor (β = 0.1, CI95% = −0.11 to 0.30, p = 0.362).
Discussion
We examined the latent structure of depressive, anxiety and somatic symptoms presented by PHC patients and its relationship with ICD-11 PHC diagnoses and disability levels. Two bi-factor solutions were found with all depressive, anxiety and somatic symptoms loading simultaneously on a general factor, along with one of three specific depression, anxiety and somatic factors or along with one of two specific anxious depression and somatic factors. The general factor correlated with disability levels and the new anxious depression diagnosis of the ICD-11 PHC.
In addition, we analyzed the reliability of the symptoms proposed for the ICD-11 PHC to assess psychopathology in PHC patients. The three scales assessed, encompassing the symptoms proposed for the depression, anxiety and BSS categories of the ICD-11 PHC, once the effects of the general factor were removed, showed different reliability profiles. Depressive and anxiety symptoms assessed all together were reliable indicators of a specific anxious depression dimension. Even when depressive and anxiety symptoms were evaluated as corresponding to two different domains (Model 1), they remained reliable indicators of specific depression and anxiety dimensions, respectively. However, the somatic symptom screening would be an ambiguous reflection of a particular construct because the variance of these symptoms could be attributed mainly to individual differences in the general factor.
The low omega of the somatization subscale indicates that to achieve a reliable evaluation of a primary care patient presenting multiple somatic symptoms it is necessary to apply both assessments: anxious depression and somatic symptoms scales. In other words, it is not enough to diagnose a patient presenting multiple somatic symptoms without considering the presence of depressive and anxious symptoms. This does not suggest that somatic symptoms are not important, on the contrary, they are major contributors to disability and severity as was found in our previous study (Goldberg et al., Reference Goldberg, Prisciandaro and Williams2016). Moreover, it is important to observe that somatic symptoms have moderate factor loadings onto the general factor, which captures a general mental health issue. This is also consistent with our findings regarding the external validity of the models, where the general factor is a better predictor of disability and mental health disorders.
Fink et al. (Reference Fink, Toft, Hansen, Ørnbøle and Olesen2007) proposed that different patterns of symptoms described as different ‘functional syndromes’ share a latent underlying dimension, and also suggested that there is a high association between these various symptoms and emotional disorders. Simms et al. (Reference Simms, Prisciandaro, Krueger and Goldberg2012) studied the latent structure that could explain this association and found a latent structure similar to the one found in this investigation, supporting the idea of a broad distress factor that could explain the presentation of multiple somatic symptoms and emotional disorders in PHC patients. However, the current model is different from the Simms et al. model in two ways. First, we found good fit indices when depressive and anxiety symptoms were merged into one dimension. This finding is in line with the wide support to include the category of AD in the psychopathological nosology, especially in the context of PHC where the comorbidity of depression and anxiety is the rule rather than the exception (Gaynes et al., Reference Gaynes, Rush, Trivedi, Wisniewski, Balasubramani, Spencer, Petersen, Klinkman, Warden, Nicholas and Fava2007; Lieb et al., Reference Lieb, Meinlschmidt and Araya2007; Löwe et al., Reference Löwe, Spitzer, Williams, Mussell, Schellberg and Kroenke2008; Hanel et al., Reference Hanel, Henningsen, Herzog, Sauer, Schaefert, Szecsenyi and Löwe2009). Thus, this result provides evidence that depressive and anxiety symptoms are part of the same latent construct in PHC patients. Second, compared with depression and anxiety dimensions assessed by Simms et al. (Reference Simms, Prisciandaro, Krueger and Goldberg2012), the depression, anxiety and anxious depression specific factors in our model were stronger, e.g. the symptom loadings were higher on the specific factors compared with the general factor. This result is rarely found in the field of psychometric analyses of psychopathology measures using bi-factor models (Rodriguez et al., Reference Rodriguez, Reise and Haviland2016b). In spite of the multi-dimensionality of the models, when more items are grouped that share the common latent factor, total scores typically reflect variance due to the broad latent variable (the general factor). Consequently, subscale scores often have ambiguous interpretations because their variance mostly reflects the general rather than the specific trait (Rodriguez et al., Reference Rodriguez, Reise and Haviland2016b). Thus, as Simms et al. (Reference Simms, Prisciandaro, Krueger and Goldberg2012) found, typically in bi-factor models of psychopathology, the general factor is robust compared with the specific traits, and when the reliability indices are assessed (see Caspi et al., Reference Caspi, Houts, Belsky, Goldman-Mellor, Harrington, Israel, Meier, Ramrakha, Shalev, Poulton and Moffitt2014; Rodriguez et al., Reference Rodriguez, Reise and Haviland2016b; Martel et al., Reference Martel, Pan, Hoffmann, Gadelha, do Rosario, Mari, Manfro, Miguel, Paus, Bressan, Rohde and Salum2017), they present higher hierarchical omega values and explained common variance and lower omega subscales compared with those we found.
A possible explanation for this finding is that while Simms et al. (Reference Simms, Prisciandaro, Krueger and Goldberg2012) included in their model all the symptoms of the Composite International Diagnostic Interview adapted for primary care (CIDI-PC) related with depression, anxiety and somatization, the depression and anxiety scales assessed here capture more specific manifestations of these constructs. The two brief scales (Goldberg et al., Reference Goldberg, Lam, Minhas, Razzaque, Robles, Bobes, Iglesias, Fortes, Mari, Gask, García, Dowell, Rosendal and Reed2012) were created using the depression and anxiety symptoms according to the CIDI-PC, but eliminating those items produced by systemic physical disease (such as poor appetite, loss of weight, poor sleep and fatigue). Compared with the entire scales of the CIDI-PC, there is no overlap between depressive and anxiety symptoms. Thus, these scales allowed us to discriminate specific manifestations of depression and anxiety symptomatology and allowed us to control the effect of neurovegetative symptoms present in these disorders. In this sense, the symptoms proposed for depression and anxiety for the ICD-11 PHC are reliable indicators of these categories, and these scales are useful for PCPs to evaluate patients in PHC settings who present with somatic symptoms not explained by known physical pathology and emotional symptoms.
Nonetheless, somatic symptom variance was mainly explained by individual differences in the general factor and had only residual relation with a specific dimension of somatization. This made sense due to the observed comorbidity between emotional and functional disorders, as it is known that there may be an overlap in the etiology of depression anxiety and somatization (Stein and Muller, Reference Stein and Muller2008). Nevertheless, a possible explanation for the lack of reliability of the somatic scale corresponding to a specific construct independent of the general factor is that the items assessed did not include specific cognitive patterns presented in BSS patients. As proposed by Fink et al. (Reference Fink, Toft, Hansen, Ørnbøle and Olesen2007), for the ICD-11 PHC, the category of BSS should be restricted to patients who present with distress and/or significant disruption in daily life due to their symptoms and have persistent concerns about the medical seriousness of their symptoms beyond the somatic symptoms described (Lam et al., Reference Lam, Goldberg, Dowell, Fortes, Mbatia, Minhas and Klinkman2013).
This study has several limitations. First, we based our analyses on a sample of PHC patients from five countries, and future work is needed to replicate these findings in more diverse PHC settings. Nevertheless, we found that the structure of depressive, anxious and somatic symptoms was similar in PHC patients from these five countries, providing evidence that the structure of these symptoms is inherent rather than a manifestation of location-specific patterns. Second, the recruitment of participants was based on judgment from the PCPs that the patients exhibited somatic symptoms not explained by known physical pathology without further medical evaluation. However, this actually can be seen as enhancing the external validity of this study, replicating the problems faced by PCPs in their routine practice. Third, the selection of patients presenting multiple somatic symptoms not explained by known physical pathology could incline PCPs to select patients who fit into their own ideas about patients presenting this symptoms profile, besides their somatic symptoms, also must have some mental disorders. In this sense, it is advisable to replicate this study with a cross-sectional sample of all consecutive patients attending primary care.
Despite these limitations, this study provides evidence to better understand the clinical presentation of mental health problems in PHC and to integrate in the ICD-11 PHC a dimensional approach to sensitize primary care workers to recognize the manifestations of multiple somatic symptoms not explained by known physical pathology as an expression of an underlying latent phenomenon which would explain the common occurrence of depression, anxiety and somatization. This dimensional approach could contribute to the recognition of mental health problems, which is a first step towards the reduction of the treatment gap (Shidhaye et al., Reference Shidhaye, Mendenhall, Sumathipala, Sumathipala and Patel2013). Consistent with previous studies, these findings suggest that depression, anxiety and somatization are different presentations of a common latent phenomenon. Thus, this study provides support for the ICD-11 PHC conceptualization of mood disturbance, especially AD, as central among patients who present multiple somatic symptoms.
Acknowledgements
CZ is a doctorate student at the department of psychiatry, Universidade Federal de São Paulo, receiving a scholarship from the Brazilian National Research Council (CNPQ). JJM is a Senior Researcher by the CNPQ. The research described in this article was funded by the World Health Organization; the Psychiatry Research Trust of Institute of Psychiatry, London; the CNPQ, Brazil (Grant number 476905/2012-5), the Committee on Research and Conference Grants, University of Hong Kong, and the National Council of Science and Technology (CONACYT), Mexico (Grant number SALUD-2013-01-202283). Apart from the individuals affiliated with these institutions who are authors of this article, the sponsoring organizations had no role in the study design; collection, analysis or interpretation of data; in the writing of this article; or in the decision to submit the article for publication. The authors alone are responsible for the views expressed in this article, which do not necessarily represent the decisions, policy or views of the World Health Organization.
Conflict of interest
All authors have completed the ICMJE Form for Potential Conflicts of Interest and declare that they have no conflicts of interest to report.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.