The importance of child nutritional status as an indicator for tracking the nutrition and health status of populations is well recognized(Reference De Onis, Blössner and Borghi1). Malnutrition leads to a reduction of human performance, deterioration of health and reduced survival of populations(Reference Caulfield, de Onis and Blössner2, Reference Pelletier and Frongillo3), as well as hindering the potential for countries to reduce poverty and maximize socio-economic development(Reference Grantham-McGregor, Cheung and Cueto4). Childhood undernutrition negatively affects school performance, thus lowering adult incomes, which in turn has negative implications for national development(Reference Ezzati, Lopez and Rodgers5). The link between malnutrition, morbidity and child mortality makes undernutrition the underlying cause of over half of all child deaths(Reference Chopra and Darnton-Hill6). This is especially so in the Sub-Saharan Africa region, where it is estimated that 4·8 million children die before the age of 5 years each year(Reference Todd and Meera7).
Child undernutrition is one of Africa's most fundamental challenges for improved human development, thus slowing down achievement of the goal of reducing child malnutrition in most developing countries(Reference Kasirye8). The prevalence of childhood undernutrition has remained of public health significance in Kenya in spite of efforts by government and non-government agencies to deal with the problem(Reference Bryce, Coitinho and Darnton-Hill9). The high rates of child undernutrition together with high rates of child mortality continue to deter the government's efforts to provide quality health care towards the reduction of mortality and malnutrition levels(Reference Kabubo-Mariara, Ndenge and Mwabu10). While studies conducted previously have identified the magnitude and determinants of undernutrition in Kenya and other low-income settings(Reference Kabubo-Mariara, Ndenge and Mwabu10, Reference Gewa and Yandell11), few studies have examined the trends of undernutrition and how the effect of identified determinants on child nutritional status changes over time. The current analysis describes the trends of chronic and acute malnutrition among Kenyan children over a period of two-and-half decades and examines the changing patterns of the effect of selected household, maternal and child-related characteristics on child nutritional status based on data from four Demographic and Health Surveys (DHS).
Methods
The present analysis utilized data from the nationwide Kenya Demographic and Health Surveys (KDHS) conducted from 1993 to 2008–2009. A total of 8805 households were selected for inclusion in 1993, 9465 in 1998, 9865 in 2003 and 9936 in 2008–2009, with a household response rate of 96·3 % or above in all of the surveys. The 1993 and 1998 samples excluded the North Eastern Province and four other northern districts (Samburu and Turkana in Rift Valley Province; Isiolo and Marsabit in Eastern Province) because of security reasons. The excluded districts accounted for less than 4 % of Kenya's population.
The DHS utilizes a multistage stratified cluster sampling methodology in which samples of households within clusters (enumeration areas) are selected. Households are then systematically selected within each cluster and household residents are eligible to participate in the survey. Urban areas are oversampled and the present analysis was based on weighted data to cater for the different sample proportions. The analysis included children <5 years of age whose weight and height/length measurements were taken and whose mothers were interviewed and had their weights and heights measured.
Anthropometric measurements
Weights and heights were taken for all children aged <5 years and their mothers in participating households. Measurements were taken with participants wearing light clothing without shoes or socks. Weight was measured to the nearest 0·1 kg using a light bathroom-type scales, while length (children aged <24 months) or height (children aged ≥24 months) was measured to the nearest 0·1 cm using calibrated height boards(12). Undernutrition was determined as stunting, wasting and underweight defined by the WHO 2006 growth reference standards, which use the WHO Multicentre Growth Reference Study population. Stunting, wasting and underweight were defined as height/length-for-age, weight-for-height/length and weight-for-age less than −2 sd (Z-score) from the reference standards for children of the same age and sex, respectively(13). Weight-for-height/length Z-score was calculated for those with heights of 65 to 120 cm.
Background characteristics
Background characteristics included in the present analysis were urban or rural residence, province, gender of the household head, wealth index, source of drinking water, and availability and type of toilet facility.
Wealth index
Household wealth index is a socio-economic index constructed as an indicator of the level of wealth that is consistent with expenditure and income measures. In the DHS this is based on data about household ownership of assets and consumer goods such as source of drinking water, type of toilet facilities, type of fuel, ownership of various durable goods and other characteristics relating to socio-economic status of the household. A factor score generated through principal components analysis is assigned to each asset, and the resulting asset scores are standardized in relation to a normal distribution(Reference Rutstein and Johnson14). Each household is then assigned a score for each asset and the scores are summed for each household(15). The proxy indicator for the long-term standard of living of the household is based on this score. For the present analysis the wealth index was grouped into five categories, namely poorest, poorer, middle, richer and richest.
Household hygiene facilities
Household hygiene facilities included were the source of drinking water and availability and type of toilet facility. Improved sources of drinking water included piped water, tap water, bottled water and protected wells in the compound. Unprotected wells, springs, rivers, ponds, lakes and dams were grouped as non-improved water sources. Improved household toilet facilities included flush toilets and ventilated improved pit (VIP) latrines, while traditional pit latrines were categorized as non-improved household toilet facilities.
Maternal characteristics
Maternal characteristics included in the analysis were age, marital status, highest level of education obtained, BMI, work status and number of children <5 years of age living with the mother. Maternal BMI was used as a measure of the mother's current nutritional status at the time the child was measured. Maternal BMI was computed as weight in kilograms divided by the square of height in metres. BMI cut-offs were based on the recommended international cut-offs as follows: underweight was defined as BMI < 18·5 kg/m2, normal weight as BMI = 18·5–24·9 kg/m2, overweight and obesity as BMI ≥ 25·0 kg/m2. Pregnant mothers and those with babies two months postpartum were included in a separate category.
Child characteristics
Child characteristics included the child's age, gender, birth order, size at birth, and whether or not the child had diarrhoea, fever or cough in the last two weeks before the survey. Information on the child's relative size at birth as reported by the mother was grouped as small, average and large.
Data analysis
Data were analysed using the SPSS statistical software package version 18·0. Analysis was done at the descriptive, univariate, bivariate and multivariate levels. Pearson's χ 2 test was used to check for associations between household, maternal and child-related characteristics and child undernutrition status in the four surveys at the bivariate level. Binary logistic regression was used to examine associations between the explanatory variables and the undernutrition outcomes: stunting, wasting and underweight. The adjusted regression model included household characteristics (namely residence, wealth index, province, source of drinking water and toilet facilities), maternal characteristics (namely age, marital status, education, BMI, work status and number of children <5 years old living with the mother) and child-related characteristics (namely sex, age, birth order, size at birth and illnesses (diarrhoea, fever and cough)). The analysis on determinants was carried out for the four KDHS separately and then data were pooled for analysis of trends in prevalence. The analyses were done using complex samples analysis to adjust for the cluster sampling design used in the DHS.
Results
The current study included children aged 0–59 months with a mean age of 29·5 months in 1993, 28·3 months in 1998, 27·8 months in 2003 and 28·7 months in 2008–2009. The largest proportion of children was sampled from the Rift Valley Province (21·8 %, 25·7 %, 26·8 % and 28·3 % in 1993, 1998, 2003 and 2008–2009, respectively; Table 1). On average, more than 80 % of the children lived in rural areas compared with about 17 % in urban areas. The mean height and weight of the children in all surveys was 82 cm and 11 kg.There were no significant age differences noted by children's gender. The mean height-for-age Z-score increased slightly from −1·6 in 1993 to −1·4 in 2008–2009. The prevalence of stunting decreased by 4·6 percentage points from 39·9 % in 1993 to 35·3 % in 2008–2009 (Table 2). Underweight declined by 2·7 percentage points over the same period, while wasting levels did not change. A multivariate analysis of pooled data using the year of the survey as a variable and 1993 as the reference category showed a significant (P < 0·005) decline in the odds of being stunted or underweight with time (Fig. 1). Children were less likely to be stunted in the 1998, 2003 and 2008–2009 surveys and less likely to be underweight in 2003 and 2008–2009 (P < 0·05) compared with 1993. The unadjusted odds of stunting were 0·9, 0·8 and 0·8 in 1998, 2003 and 2008–2009, respectively (Fig. 1). The unadjusted odds of underweight were 0·8 times lower in 2003 and 2008–2009 compared with 1993 (Fig. 1).
Table 1 Distribution of household, maternal and child-related characteristics: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009

†1993 and 1998 surveys excluded North Eastern Province.
‡Excludes 1792 cases with missing data for wealth index in 1993.
§Excludes 32 cases with missing data for type of water source in 1993.
∥Excludes 14 cases with missing data for type of water source in 1998.
¶Excludes 1602 cases with missing data for child morbidity in 1998.
Table 2 Percentage of children <5 years of age with undernutrition, by household, maternal and child-related characteristics: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009

Note: table is based on children of interviewed mothers.
†1993 and 1998 surveys excluded North Eastern Province.

Fig. 1 Trends in unadjusted relative odds of stunting (![]() ), underweight (
), underweight (![]() ) and wasting (
) and wasting (![]() ) among children <5 years of age in Kenya. Model based on pooled data from four Kenya Demographic and Health Surveys (1993, 1998, 2003 and 2008–2009). **Unadjusted odds of stunting were significantly lower in 1998, 2003 and 2008–2009 compared with 1993 (P < 0·01); *unadjusted odds of underweight were significantly lower in 2003 and 2008–2009 compared with 1993 (P < 0·05)
) among children <5 years of age in Kenya. Model based on pooled data from four Kenya Demographic and Health Surveys (1993, 1998, 2003 and 2008–2009). **Unadjusted odds of stunting were significantly lower in 1998, 2003 and 2008–2009 compared with 1993 (P < 0·01); *unadjusted odds of underweight were significantly lower in 2003 and 2008–2009 compared with 1993 (P < 0·05)
Household characteristics
Place of residence, province, wealth index, source of drinking water, and availability and type of toilet facility were significantly associated with undernutrition. The proportion of stunted, wasted and underweight children was higher in rural areas compared with urban areas in all surveys (Table 2). The prevalence of underweight decreased from 20 % in 1993 to 17 % in 2008–2009 among the rural areas, while this prevalence remained at 10 % in the urban areas during all surveys. The slow decline in the prevalence of stunting at the national level was also evident in the regions except for Rift Valley Province, which showed an increasing trend in stunting from 35·0 % in 1993 to 37·8 % in 2003 and then a slight decline to 35·8 % in 2008–2009 (Table 2).
Undernutrition was negatively correlated with wealth index throughout the four surveys. Children in the poorest, poorer, middle and richer wealth quintiles had higher relative odds (1·5 times) of stunting (P < 0·05) compared with those in the richest quintile in the earlier surveys (1993 and 1998; Table 3). This trend changed in the more recent surveys (2003 and 2008–2009) where only children from the poorest wealth index were significantly more likely (P < 0·005) to be stunted in 2003 (1·6 times) and 2008–2009 (2·1 times; Table 3) compared with those from the richest wealth quintile. Slightly more than half (51 %) of the children living in households without toilet facilities were stunted in 1993, reducing to 48 % in 1998, 41 % in 1998 and 42 % in 2008–2009 (Table 2). Children in households without a toilet facility and with a non-improved toilet facility were 2·2 times and 1·5 times significantly (P < 0·05) more likely to be stunted in 1993. The effect of this factor changed in 2003 and 2008–2009 whereby the increased odds of stunting remained significant (P < 0·005) among children in households with a non-improved toilet facility (Table 3). The association between wasting and availability and type of toilet facilities was significant in all four surveys (all P < 0·05). More than a quarter (28 %) of the children living in households without a toilet facility were underweight in 1993, 1998, 2008–2009 while a quarter (25 %) were underweight in 2003 (Table 2). Regional differentials showed that children were significantly less likely to be stunted in Nyanza, Rift Valley and Western provinces in 1993 and 2008–2009 compared with Nairobi Province (Table 3).
Table 3 Relationship between childhood stunting and household, maternal and child-related characteristics: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009

ref., reference category.
Note: table is based on results of adjusted binary logistic regression model.
*P < 0·05, **P < 0·005, ***P < 0·001.
†1993 and 1998 surveys excluded North Eastern Province.
Maternal characteristics
Mother's education, current maternal nutritional status and the number of children <5 years old living with the mother had significant associations with undernutrition during the period under consideration. There was an increased likelihood of stunting, wasting and underweight if the child's mother had no education compared with secondary or higher levels. The proportion of stunted and underweight children among non-educated mothers declined significantly with time (all P < 0·001; Table 2). Children of uneducated mothers were more likely to be stunted: 1·6 times more in 1993, 1·7 times more in 1998 and 1·7 times more in 2003 (Table 3). While the odds of child stunting were not significant in 2008–2009 among children of non-educated mothers, the odds were significant (P < 0·05) among children whose mothers had primary education (Table 3). This pattern of maternal education as a determinant of stunting was repeated in regard to underweight (Table 5). Children of non-educated mothers were 2·3 and 2·2 times more likely to be wasted in 1998 and 2003 compared with those whose mothers had secondary or higher levels of education (Table 4). Children whose mothers were thin (BMI<18·5 kg/m2) or pregnant/two months postpartum were significantly more likely to be stunted (P < 0·005) compared with those whose mothers had a normal BMI (Table 3). Thin mothers were more likely to have wasted and underweight children in all four surveys (Tables 4 and 5). Children whose mothers were overweight/obese (BMI ≥ 25·0 kg/m2) were significantly less likely to be stunted in 1998 and 2003 (P < 0·005 and P < 0·001, respectively). This trend shifted in 2008–2009, where children of overweight/obese mothers were significantly more likely (P < 0·05) to be stunted compared with children of normal-weight mothers (Table 3).
Table 4 Relationship between childhood wasting and household, maternal and child-related characteristics: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009
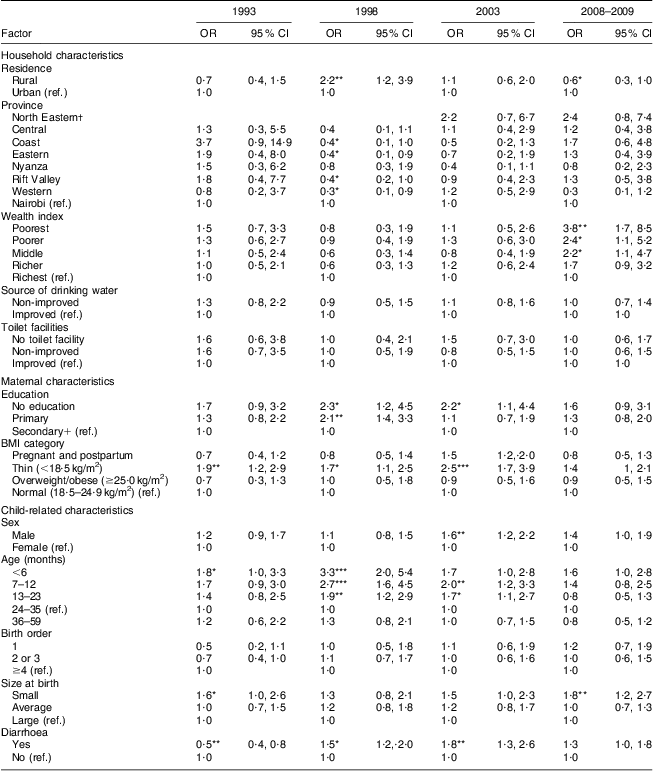
ref., reference category.
Note: table is based on results of adjusted binary logistic regression model.
*P < 0·05, **P < 0·005, ***P < 0·001.
†1993 and 1998 surveys excluded North Eastern Province.
Table 5 Relationship between childhood underweight and household, maternal and child-related characteristics: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009

ref., reference category.
Note: table is based on results of adjusted binary logistic regression model.
*P < 0·05, **P < 0·005, ***P < 0·001.
†1993 and 1998 surveys excluded North Eastern Province.
Child-related characteristics
There was a positive association between the child's gender, age and size at birth with undernutrition during the four KDHS (Table 2). Male children were more undernourished in all four surveys. Children aged 24–35 months had significantly higher odds of being stunted or underweight (Table 3 and 5). A significantly higher percentage of stunted, wasted and underweight children were small at birth during the four surveys (all P < 0·005; Table 2). Children who were born small in size were more likely to have undernutrition compared with those born large in all four surveys (Tables 3–5). The level of undernutrition was higher in children who had diarrhoea preceding the surveys compared with those who did not have diarrhoea. This relationship was statistically significant (P < 0·005) for stunting in 1993, 1998 and 2003, and statistically significant (P < 0·05) for wasting and underweight throughout the surveys (Table 2).
Discussion
The analysis shows a slow decline of chronic undernutrition by 4·6 percentage points as well as a slight decline in underweight (by 2·7 percentage points) in Kenya between 1993 and 2008–2009. The present study is one of the first to analyse the trends of childhood undernutrition in Kenya over three decades using national representative data. The persistent high levels of stunting and underweight are indicators of the slow progress in improving child nutritional status in Kenya. Findings from similar analyses in India, Bangladesh and Mozambique covering more than two decades reported slow national declines in undernutrition among young children(Reference Pathak and Singh16–18). This slow decline in undernutrition rates in Kenya has continued to undermine efforts geared towards reducing the prevalence of child undernutrition. For instance, the 1999–2004 Kenya Ministry of Health strategic plan(19) targeting to reduce childhood undernutrition by 30 % is far from achievement considering the 1·7 percentage point change in the prevalence of stunted children between 1998 and 2003 as per the current analysis.
The wealth index as used in the DHS compares the population within the same survey year in a relative sense. Thus as applied in the present analysis, it is difficult to compare groups in the same quintiles in different surveys. However it is a useful measure of relative economic differences within the same survey year. Disparities exist in the distribution of undernutrition among Kenyan children based on region (provinces), residence (rural and urban) and economic divide as measured by the household wealth quintiles. The trend shows a much stronger influence of the wealth index in the earlier surveys in 1993 and 1998 whereby children from the poorest, poorer, middle and richer quintiles were more likely to be stunted compared with the richest. This effect was reduced in 2003 and 2008–2009 when only children from the households with the poorest wealth index were more likely to be stunted compared with the richest. Clearly more efforts need to go into planning effective programmes that target the most vulnerable children. Separately, the availability and type of household toilet facilities was associated with chronic malnutrition. Children living in households with no or non-improved toilet facilities were more likely have short stature when compared with those having improved toilet facilities. Studies in Sub-Saharan Africa have found similar results. In Ethiopia, low child stature was associated with lack of toilet facilities and unprotected water sources(Reference Getaneh, Assefa and Taddesse20) while an analysis of DHS data from eleven countries in Sub-Saharan Africa identified lack of optimal sanitation facilities as a determinant of chronic malnutrition among young children(21). The slight decline noticed may be explained by the increasing social and human development efforts that have been going on in the country in recent years resulting in a marginal increase in the country's Human Development Index(22), an indication of people's improving standards of living. A further analysis of the trends of child nutritional status within the Sub-Saharan African region could provide further understanding of the regional changes in childhood nutrition indicators as well as explain some of the drivers of the observed slow reduction of undernutrition among Kenyan children.
The levels of acute malnutrition measured by wasting did not change much over the years, remaining at about 6 %. This form of malnutrition is caused mainly by recent inadequate food intake, infections or incorrect feeding practices and reflects the nutritional status of children within a short period of time. Kenya has been faced with repeated cycles of famine and drought resulting in insufficient food production at the household level and nationally. This, coupled with the global increases in food prices, has resulted in extended food insecurity in the country that may have contributed to the non-reducing levels of wasted children over the years.
The current study emphasizes the importance of maternal education on child nutrition outcomes in Kenya. These findings agree with results of an analysis by Giroux(Reference Giroux23) of the effect of maternal education on child stunting in the Sub-Saharan African region. Attaining a secondary or higher level of maternal education was associated with lower odds of childhood stunting and underweight. Higher maternal education is associated with maternal employment and higher household income. These findings concur with those of Gewa and Yandell(Reference Gewa and Yandell11) who found that low maternal education and poor maternal nutritional status were associated with higher odds of childhood undernutrition in Kenya. The effect of maternal education on childhood stunting and underweight is, however, changing over time in Kenya. In the earlier surveys (1993, 1998 and 2003), lack of education among mothers as well as attaining primary level of education were associated with poor child nutritional outcomes, while in the recent survey this effect was noticed among children of mothers with primary level education. This is in line with the changing dynamics of education in the country with the introduction of free primary education in 2002. There has been a reduction in the proportion of mothers without education in the country, which has declined from 17·4 % in 1993 to 12·7 % in 2008–2009. Attaining primary level of education is not adequate to give mothers higher human and capital development that in turn would translate into increased family incomes and improved child nutrition.
Maternal undernutrition is a persistent determinant of child undernutrition as seen in our study. Children whose mothers were thin (BMI < 18·5 kg/m2) were more likely to be undernourished. Although the study did not investigate the effect of maternal BMI during pregnancy on children's nutrition outcomes, mothers’ compromised current nutritional status was shown to be associated with increasing likelihood of undernutrition among the children. The analysis reveals a changing effect of maternal BMI on chronic undernutrition in children, whereby children with overweight mothers were stunted in the 2008–2009 survey. This suggests an emerging pattern of a dual burden of malnutrition, where, in the same household, the mother is overweight while the child is suffering from long-term nutrition deprivation. This coexistence of maternal overnutrition and child undernutrition in the same household describes the rapid nutrition transition in developing countries(Reference Bouzitou, Fayomi and Delisle24) and has been reported in such middle-income countries as Indonesia and Russia where between 9 % and 13 % of households contain both underweight and overweight members(Reference Doak, Adair and Bentley25).
Conclusions
The present study set out to analyse the trends and determinants of malnutrition among children <5 years of age in Kenya. The study found that the levels of stunting and underweight are decreasing slowly, with more likelihood of undernutrition among children from households in the poorest wealth index, those living in the Coast, North Eastern and Eastern provinces and those who are of small size at birth. The trends in effects of wealth index, maternal education and maternal BMI on child undernutrition suggest shifting patterns with a reduced effect of primary education of mothers and an emerging pattern of the double burden of malnutrition in the same households.
Policy implications
Considering these important findings, it is critical to translate the national strategies on nutrition interventions in favour of the most vulnerable people in the poorest households as well as those in the most affected regions. One of the goals of the national food and nutrition strategy 2008(19) is to increase households’ resource productivity. This goal and strategy are examples of a plan that can be targeted to the poorest households with a view to improve the nutritional status of the children. The Kenya government should also take heed of the evidence of changes in maternal education as this has very critical implications for reducing maternal and child malnutrition. Improving maternal education to beyond primary level will make a significant improvement to the nutritional status of children. In order to realize the benefit of improved schooling in a timely manner, education policy makers need to urgently explore methods of ensuring that women of reproductive age who did not have chance to attend secondary schooling have an opportunity to get an equivalent of secondary and higher levels of education through restructuring the education system to allow for adult-based education in the country. Further research to explore the regional disparities of the trends within the country as well as how Kenya compares with other countries in the region is recommended.
Acknowledgements
This research was made possible by a fellowship funded by the US Agency for International Development (USAID) through the MEASURE DHS project at ICF International. The study research protocol and use of DHS data were approved by ICF International. There are no conflicts of interest. The authors’ contributions are as follows: P.K.M., developing research protocol, background information, objectives, data analysis, developing tables and figures, writing up the discussion, recommendations, referencing; D.M., methods, subjects, identifying variables in the DHS databases. The authors would like to thank ICF International for making the data available and the staff team for their support and guidance in statistical analysis of the DHS data.








