Iodine is an essential micronutrient that is required for the synthesis of thyroid hormone. The deficiency of iodine leads to thyroid dysfunction as the thyroid gland cannot produce sufficient amounts of thyroid hormone( Reference Azizi, Sheikholeslam and Hedayati 1 – Reference Huang, Tseng and Chen 3 ), which causes poor physical growth, cognitive impairment, neuro-behavioural and intellectual disorders, and CVD( Reference Moleti, Lo Presti and Campolo 4 , Reference Andersson, de Benoist and Rogers 5 ). Moreover, iodine deficiency also increases the risk of reproductive failure (such as miscarriage, premature birth and stillbirth) among pregnant women( Reference Dillon and Milliez 6 ). According to the 2013 Lancet series on maternal and child nutrition, 28·5 % of the world’s population was iodine deficient( 7 , Reference Black, Victora and Walker 8 ). The WHO estimates showed that about 50 million people had some degree of mental impairment caused by iodine deficiency( Reference Feyrer, Politi and Weil 9 ). The 2013 UNICEF report showed that about 35 million newborns were unprotected from the lifelong consequences of iodine-deficiency disorders (IDD) globally( 10 ). Among them, sub-Saharan Africa had the highest number of unprotected newborns (about 14 million) followed by South Asia (with 11 million)( 10 ). In Bangladesh, the last IDD survey (from 2004–05) showed that the prevalence of IDD (as indicated by urinary iodine concentration below 100µg/l) among children and women of reproductive age (15–49 years) was 34 and 39 %, respectively( Reference Yusuf, Rahman and Chowdhury 11 ). The prevalence of IDD was 40 and 42 % in school-age children and women, respectively, in the Bangladesh National Micronutrients Status Survey 2011–12( 12 ). Although the rate of IDD has been decreasing over the years, the issue of IDD still persists at a magnitude of public health significance nuisance in developing countries such as Bangladesh( Reference Yusuf, Rahman and Chowdhury 11 , Reference Andersson and Zimmermann 13 , Reference Tran, Hetzel and Fisher 14 ). One possible approach to control this problem is to improve iodine status by universal salt iodization, which has been the most widely used strategy to control and eliminate IDD for the last 30 years( 10 , Reference Tran, Hetzel and Fisher 14 ). Although many countries passed legislation on universal salt iodization (expecting more than 90 % of households to have access to adequately iodized salt containing 15–40ppm of iodine)( Reference Tran, Hetzel and Fisher 14 , Reference De Benoist and Clugston 15 ), the overall percentage of households (worldwide) with access to iodized salt is still unsatisfactory. For instance, as of 2013, only 75 % of all households worldwide had access to adequately iodized salt, and this was 69 % in South Asia( 10 ).
In Bangladesh, a South Asian country, the status of iodine coverage is not encouraging. National household surveys have shown that the use of iodized salt (≥5ppm) and adequately iodized salt (≥15ppm) changed from 81·0 % (in 2004–05) to 80·3 % (in 2011–12) and 72·6 % (in 2012–13) for iodized salt, and from 51·0 % (in 2004–05) to 57·0 % (in 2011–12) and 54·3 % (in 2012–13) for adequately iodized salt( Reference Yusuf, Rahman and Chowdhury 11 , 12 , 16 ). The most recent Bangladesh National Salt Iodization Survey (NSIS) of 2015 showed that only 50·5% households in Bangladesh have access to adequately iodized salt, whereas only 65·0% households have access to iodized salt( 17 ). Although the scenario has not changed much in adequate iodized salt coverage, there is a notable decrease in level of some iodized salt coverage over the years, which is alarming( 17 ).
There have been a limited number of studies which investigated the availability of iodized salt among households in Bangladesh( Reference Yusuf, Rahman and Chowdhury 11 , 17 , Reference Knowles, Garrett and Gorstein 18 ). To best of our knowledge, no study has investigated the relationship between household socio-economic status (SES) and availability of iodized salt in Bangladesh using a nationwide survey. According to the Bangladesh Multiple Indicator Cluster Survey (MICS) 2012–13( 16 ), 27% of households in Bangladesh have no iodine content in their salt, which invites more studies to be conducted in this area, particularly in identifying the vulnerable households.
Household SES in Bangladesh largely depends on the head of the household( Reference Ahmed, Adams and Chowdhury 19 – Reference Kabir and Webb 21 ), who makes most of the household financial decisions( Reference Killewo, Anwar and Bashir 22 ). It is an important variable collected for household surveys like the Bangladesh Demographic and Health Surveys( 23 ), where mostly heads of households are male and Muslim( 24 , 25 ). The traditional provider of salt is the household head( Reference Torheim, Granli and Sidibé 26 ), and that is why in most intervention studies of iodine deficiency, the head is given the iodized salt to ensure proper distribution( Reference Wegmüller, Zimmermann and Bühr 27 – Reference Andersson, Thankachan and Muthayya 29 ).
The World Bank suggests that the governments of low- and middle-income countries need to put a high priority on salt iodization to promote sustainable health and economic development( Reference Zimmermann, Gizak and Abbott 30 ). It is expected that people in the higher wealth quantiles are more aware of iodized salt compared with the poorer households( Reference Hoddinott, Maluccio and Behrman 31 , Reference Girma, Loha and Bogale 32 ). Similarly, improved iodine status is generally observed in urban areas compared with rural areas, where goitre is more prevalent( Reference Tronko, Kravchenko and Fink 33 – Reference Erdoğan, Ağbaht and Altunsu 36 ), although exceptions do exist( Reference Saggiorato, Arecco and Mussa 37 ). Geographical divisions along with inequality are also expected to be differentiating factors for household coverage of iodized salt( 25 ).
The present study intended to explore the context of household-level availability of iodized salt in Bangladesh by analysing national survey data. The current paper assesses the determinants of the availability of iodized salt at household level in Bangladesh by considering household SES, demographic factors and geographic location using Bayesian mixed-effect logistic regression models. Such study will help policy makers to design intervention strategies for households in the context of Bangladesh.
Methods
Sampling
The data for the present study were extracted from the most recent Bangladesh MICS of 2012–13( 38 ). This survey aimed to attain national-level estimates for various health indicators of the seven divisions and sixty-four districts in Bangladesh, where a two-stage stratified cluster sampling design was used. The districts were identified as the primary sampling strata and a specific number of census enumeration areas were selected systematically using probability-proportional-to-size sampling within each stratum. After completing the household listing within the selected enumeration areas, a systematic sample of twenty households was drawn from each enumeration area. All surveyed households were requested to provide a sample of their cooking salt, which was used to test the adequate proportion of iodine. It was tested using salt test kits and the presence of potassium iodate content was quantified( Reference Knowles, Garrett and Gorstein 18 ). In the present study, we selected only those households that had results of the salt test as well as complete information on all selected covariates. A small proportion of households (about 1·1%) had no available salt in their households during the survey( 16 ), which were excluded from our analysis. The final sample size for the present study was 50 981.
Variables
Outcome variable
The outcome variable ‘availability of household-level iodized salt in Bangladesh’ was categorized into two scales: iodized salt (if household salt had >0ppm iodine) and non-iodized salt (if household salt had 0ppm iodine). Thus, the households were divided into two groups: households with iodized salt v. non-iodized salt.
Selected covariates
The household SES variables that were expected to be associated with the availability of iodized salt in the households were: wealth index (‘poor’, ‘middle’, ‘rich’), age of the household head (‘<25’, ‘25−34’, ‘35−44’, ‘45−54’, ‘55−64’ and ‘≥65’ years), sex of the household head (‘female’, ‘male’), education of the household head (‘no education’, ‘primary incomplete’, ‘primary complete’, ‘secondary incomplete’, ‘secondary complete or higher’), religion of the household head (‘Muslim’, ‘others’), place of residence (‘rural’, ‘urban’) and division (which is largest local government administrative area in Bangladesh; ‘Barisal’, ‘Chittagong’, ‘Dhaka’, ‘Khulna’, ‘Rajshahi’, ‘Rangpur’, ‘Sylhet’). The household wealth index was pre-calculated in the data based on asset variables and using principal component analysis( Reference Knowles, Garrett and Gorstein 18 ).
Statistical analysis
Bivariate and multivariable statistical analyses were performed in the present study. Initially, the bivariate associations between the availability of iodized salt at household level and the selected SES variables were tested using the χ 2 test. Then, mixed-effects binary logistic regression analysis was performed to examine the significance of the associated factors with the household-level availability of iodized salt. We applied the Bayesian framework with the Markov chain Monte Carlo (MCMC) algorithm instead of classical maximum likelihood procedures to attain the unbiased estimates of both variance components and predictors( Reference Browne and Draper 39 ).
Bayesian analyses require ‘prior’ distributions for all parameters. We used parameter expanded priors which were approximately flat (but still proper) for the sd ( Reference Hadfield 40 ). Inspection of the trace and density plots and effective sample size indicated convergence of models. We ran the models for 100 000 iterations with a burn-in (the number of initial iterations discarded) of 20 000 and a thinning (the number of saved estimates for analysis) interval of 500 to achieve low autocorrelation between recorded iterations. Three models were fitted to examine the impact of different predictors on the binary outcome and importance of the random effects. First, we fitted a random-intercept model with district-level variation of the outcome; second, a random-intercept model to assess the cluster-level variation; and finally, a two-level random-intercept model to evaluate the district- and cluster-level variation. The deviance information criterion determined the fitness of the models. All statistical analyses were performed in R version 3.3.0. We used MCMCglmm package in R for Bayesian models, which has previously been applied in health- and nutrition-related studies( Reference English and Uller 41 – Reference House, Jensen and Rapkin 43 ). The adjusted odds ratio of posterior mean (OR) in favour with its 95% credible interval (CI) were computed for the coefficient of each of the covariates. The Bayesian P value (P MCMC) was calculated to indicate the statistical significance of the variables.
Results
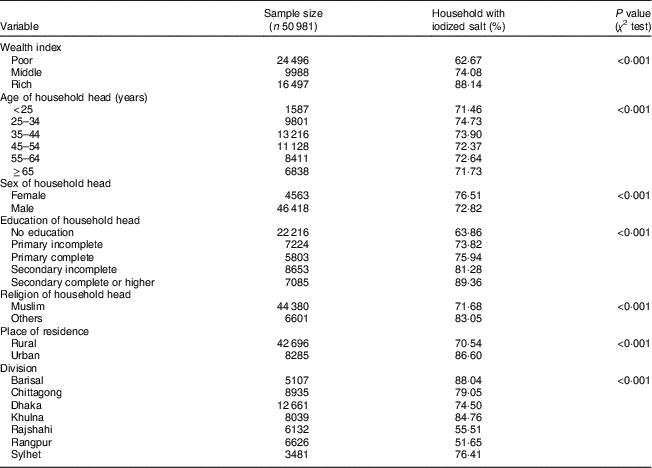
Among the selected sample of 50 981 households, 73·15% had some level of iodine in the salt sample they provided during the survey period (data not shown). Table 1 displays the bivariate analyses that show the outcome of iodized salt consumption in the households of various SES. The availability of iodized salt at the household level varied significantly (P < 0·001) across the different wealth groups. From Table 1 we can see that only 62·67% of households from the poor wealth class had iodine in their household salt sample, which was almost 25 percentage points lower than for the rich. The proportion of households who had some level of iodized salt coverage varied among households with female and male heads, being 76·51 and 72·82%, respectively. The proportion of iodized salt availability in households did not show much variation with age of the household head, as availability was about 71–75% for every group. The availability of iodized salt in households varied significantly (P<0·001) across the different educational groups of household heads. Household heads with secondary or higher education had higher coverage of iodized salt in their households (89·36%) compared with non-educated household heads (63·86%). In addition, household coverage of iodized salt in urban areas was 16 percentage points higher compared with rural areas. Barisal division had the highest household-level availability of iodized salt, whereas the lowest was in the north-west part of Bangladesh (Rangpur and Rajshahi).
Table 1 Bivariate analysis of the association of household-level iodized salt coverage in Bangladesh with household socio-economic status, 2012–13
The district-level variation in the availability of iodized salt in households was apparent in Bangladesh as depicted in Fig. 1. Particularly the north-west part of Bangladesh lacked household-level iodized salt. However, the worst condition persisted in Cox’s Bazar, the only district where the household-level iodized salt coverage was below 25%, followed by Chapai Nawabganj and Thakurgaon. The middle and southern part of the country, including Dhaka (the capital), Khulna and their adjacent areas showed higher coverage of iodized salt in households.

Fig. 1 (colour online) District-wise variation in the household-level iodized salt coverage in Bangladesh, 2012–13
Table 2 summarizes the association of different factors with household-level availability of iodized salt. The three Bayesian mixed models with different random effects showed consistent results. However, the third model with the lowest deviance information criterion was the best-fitted model, where the variation of both districts and clusters was adjusted for. The random variances in all models were significant, which justifies the application of mixed-effect models. In addition, the estimates of variance parameters differed significantly from zero, indicating that the unmeasured and unobserved factors shared by community and districts had an association with household-level iodized salt coverage in Bangladesh. Education, religion and sex of the household head, along with household wealth, residence and geographical division, were significantly associated with availability of household iodized salt in Bangladesh.
Table 2 The Bayesian mixed-effects logistic regression models fitted to the association of household-level iodized salt coverage in Bangladesh with household socio-economic status, 2012–13
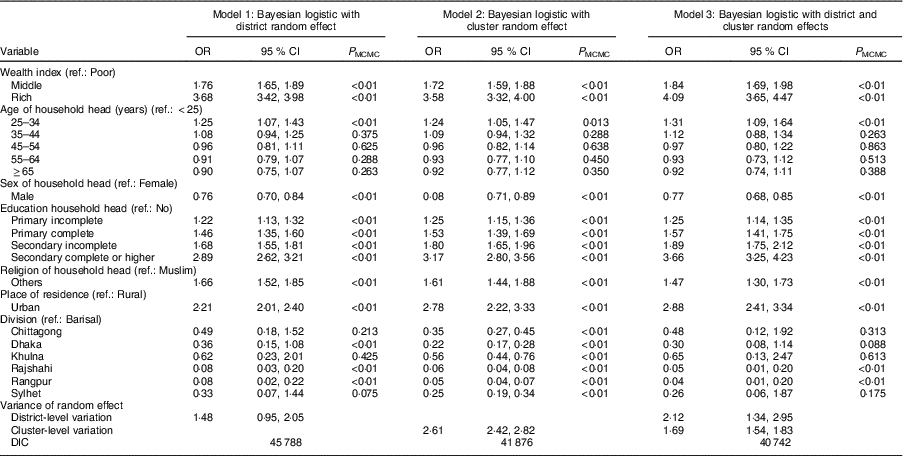
OR, adjusted odds ratio of posterior mean; CI, credible interval; P MCMC, Bayesian P value; ref., reference category; DIC, deviance information criterion.
The economic status of the households showed a significant association with the household availability of iodized salt. Especially, the middle and rich classes were 1·84 (95% CI 1·69, 1·98; P MCMC < 0·01) and 4·09 (95% CI 3·65, 4·47; P MCMC<0·01) times more likely to use iodized salt, respectively, compared with the poor (Model 3, Table 2). Availability of iodized salt in households with younger heads (25−34 years) was found to be significantly higher (31% more) than in households with the youngest heads (<25 years). Surprisingly, households had 23% (P MCMC<0·01) less chance of using iodized salt under a male head compared with a female head, although only 9% households had a female head in the sample. The odds of availability of iodized salt at household level increased significantly with education level (primary complete, primary incomplete, secondary complete or higher, secondary incomplete) by 1·25, 1·57, 1·89 and 3·66 times, respectively, compared with households where the head had no education. Religion of households was found to have significant (P MCMC<0·01) association with household-level access to iodized salt; in particular, households with other religious believers had 47% higher likelihood of using iodized salt compared with Muslim households. Significantly higher consumption (OR = 2·88; 95% CI 2·41, 3·34; P MCMC<0·01) of iodized salt was observed in urban respondents compared with rural counterparts. The coverage gap between Barisal (reference) and Rangpur or Barisal and Rajshahi divisions was significant in all three models, where locals of Rajshahi and Rangpur had lesser iodized salt availability at households. The significant cluster- (1·69) and district-level (2·12) variances reveal that the likelihoods of the availability of household iodized salt at these levels were correlated, which indicated that there were other factors associated with iodized salt coverage at community and district level not explained by the observed covariates included in the models. This result further suggested that unobservable factors related to the districts were more likely to be associated with a higher likelihood of household iodized salt availability than the cluster-level unobservable factors.
Convergence diagnostic tests were used to assess the convergence of the Markov chain as explained in the ‘Methods’ section. Trace plots and density plots for the parameters of the posterior distribution obtained by the MCMC algorithm are presented in the online supplementary material (Supplemental Figs 1–6). None of the trace plots displayed any significant upward or downward trend along the iterations, and the density plots showed almost symmetrical distributions. In particular, the trace plots exhibited the so-called ‘thick pen’, which indicated insignificant deviations from stationarity and that the MCMC algorithm could be considered as converged.
Discussion
The present study determined the relationships between iodized salt availability and different socio-economic factors of households in Bangladesh. We analysed the Bangladesh MICS data of 2012–13 by using Bayesian mixed-effects logistic regression, which revealed some important results that require more attention from policy makers. The study found that household-level iodized salt availability was significantly associated with age of the household head and their education status. In addition, a significant inequality in household-level iodized salt availability was noticed due to family income status as well as their place of residence. The study also observed that the availability of iodized salt in households varied considerably between geographic locations, such as districts of Bangladesh.
Only 20% of the global population had access to iodized salt in 1990 and it rose to 71% in 2012; however, the long-term commitment from governments in different countries remains debatable( Reference Zimmermann and Andersson 44 ). The worrying signs are worse for developing nations due to the rise in IDD( Reference Hetzel 45 ). For example, a longitudinal study conducted in Bangladesh concluded that urinary iodine concentration during pregnancy depends on women’s education and SES along with other factors( Reference Rydbeck, Bottai and Tofail 46 ). Similarly, another study in Cox’s Bazar showed that iodized salt is considered a sign of prestige in the local community as it demonstrated wealth and education( Reference Rasheed, Siddique and Sharmin 47 ). Furthermore, women seem to exert higher responsibility regarding household decisions (e.g. one of the findings of our study was that female household heads were more concerned regarding iodized salt than males), which is why micro-credits are highly concentrated on female borrowers in Bangladesh( Reference Pitt, Khandker and Cartwright 48 , Reference Kumar, Hossain and Gope 49 ). It could also be contributed to by the fact that traditionally females prepare the food for the family in Bangladesh and they tend to be more concerned regarding nutrition( Reference Hawas, Lemma and Mengesha 50 ). We reached a homogeneous conclusion with the literature that several household SES variables are associated with household-level iodized salt availability or consumption of iodized salt all over Bangladesh( 17 ).
Households’ access to adequately iodized salt is commonly dependent on several factors such awareness, price, convenience, utilization preferences, packaging and availability( 17 ). Differences in adequately iodized salt availability in households reported here by SES could be the result of these factors. Moreover, a recent survey in Bangladesh showed that poor households were almost twice as likely to use open salt (unbranded salt without any form of packaging) and more likely to source salt from non-formal retail channels such as the point of production( 12 , 17 ). Agreeing with these, we found that people with higher SES (higher wealth index and better educational status of household head) were more likely to purchase iodized salt rather than salt lacking proper quality of iodine. The survey considered in the present study lacked data on micro-level awareness, price of salt, convenience of location, utilization preferences, packaging or availability in the local market, which could solicit further investigations on this phenomenon in Bangladesh.
The poor and the illiterate living in the rural areas were the most vulnerable for iodine deficiency. This was an expected outcome as economically challenged households cannot afford to spend extra money to buy the slightly costlier iodized salt( Reference Rasheed, Hanifi and Iqbal 51 , Reference Sen, Das and Biswas 52 ), which is a common scenario in Africa and South Asia( Reference Kazungu, Mbakaya and Makokha 53 , Reference Yaye, Baraki and Endale 54 ). The lack of awareness creates a knowledge gap for these sections of households, and they become victims of IDD( Reference Roy, Chaturvedi and Agrawal 55 , Reference Haji, Abdurahmen and Paulos 56 ). The rural areas suffer from the same problem due to the lower economic status and the shortage of awareness campaigns or lack of information( Reference Tran, Hetzel and Fisher 14 ). This is visible in Fig. 1, where the divisional cities have higher coverage than other areas of Bangladesh. Myths like ‘Iodine is contained in the sea fish that we eat, so we don’t have to eat iodized salt’ persist due to illiteracy and lack of awareness( 57 ).
The purchasing capacity of the locals and lack of government monitoring allow salt production to be unmonitored, cheap and irresponsible. Although iodizing salt does not cost a lot, salt mills operate on slim profit margins in Bangladesh and they tend to avoid the iodizing procedure( 57 ). A study of 121 salt factories in four districts of Bangladesh found that none of the factories maintained adequate iodizing quantity, with most mills adding less than the required amount( Reference Jabin 58 ). It was also found that carelessness of the packaging process compromises the content of iodine. A survey report prepared by International Diarrhoeal Disease Research, Bangladesh (icddr,b) found that the household coverage for adequately iodized salt has decreased (non-significantly) to about 51% since 2011( 17 ). The survey found that 80% of the open salt in the sample had no iodine (<5ppm); and the weak salt law as well as the lack of clear guidance on enforcement of the regulations for violating it could be potential reasons for such a scenario. The law was introduced in 1989 and modified in 2013( 16 ). However, the lack of awareness campaigns is making it difficult for people in the most vulnerable parts of the community to have access to iodized salt, leading to IDD.
The unavailability of iodized salt in the remote regions coupled with households’ lack of purchasing power potentially explains the unsatisfactory scenario of iodized salt in Bangladesh. In the icddr,b survey( 17 ), the quantity of open salt sold in rural areas was twice the amount in urban areas. It attracts the poor people residing in rural areas to go for the cheaper option. Furthermore, rural residents in Bangladesh are comparatively poorer than urban residents( Reference Baulch 59 ), which integrates with the lack of general awareness or education and leads them to consume low-quality salt. This encourages the quality producers to stay in the urban market, where most consumers can afford it. Proper utilization of the salt law, greater availability of quality product at a reasonable price and extensive awareness campaigns should contribute to this context.
Limitation of the study
In the present study, availability of iodized salt was assessed through household salt primarily used during food preparation or as table salt; however, it did not account for potentially iodized salt consumed through processed foods. Consumption of processed foods is higher in urban areas, which means that urban residents have greater scope for intake of iodine through this salt (such as in ready meals, processed meats, cheese, salty snack foods, instant noodles, etc.), and processed foods are also consumed more frequently in large amounts (such as bread and processed cereal products)( 60 ). This creates a direct contrast between urban and rural diets that might affect the iodine consumption rate among various locations and act as a confounding factor in the fitted models. However, the secondary data set analysed in the present study lacks specific information on general awareness, price, convenience, utilization preferences, packaging or availability, which could potentially have some effects on iodized salt coverage in households. Future studies, with further data collection, could investigate the association between price of the salt and its affordability by the general population.
Conclusion
Bangladesh has recently been promoted to a low–middle-income country; however, socio-economic disparity is still evident, especially in the public health sector. Approximately 50% of households in Bangladesh lack adequately iodized salt. The present study assessed the impact of household SES on some level of iodized salt using a national survey of about 50 000 households. The Bayesian mixed-effect logistic model showed that after controlling for relevant variables, households’ education, wealth index and location are important components that contribute to the local household-level iodized salt coverage in Bangladesh. The north-west part of the country and Cox’s Bazar in the far south severely lack household iodized salt. The difference between rural and urban areas also suggests that the availability of iodized salt and the purchasing capacity of households are causing severe disparity in iodized salt availability. The salt law and clear guidance on enforcement of its regulations, along with local awareness campaigns, could improve the situation. Possible interventions regarding salt iodization should be conducted considering the district-level variations.
Acknowledgements
Acknowledgements: The authors would like to acknowledge UNICEF and the Bangladesh Bureau of Statistics (BBS) who conducted a nationwide survey and made their data available and freely accessible. The authors also thank anonymous reviewers and the editors for their insightful suggestions that helped develop the quality of the manuscript. Financial support: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Conflict of interest: The authors declare that they have no competing interests. Authorship: J.R.K. conceptualized the study, compiled the data, synthesized the analysis plan, performed formal analyses, interpreted the outcomes and participated in critical review of the manuscript. R.K.B. helped to conceptualize the analysis plan, performed the geographical mapping, interpreted the findings and drafted the manuscript. The manuscript was critically reviewed and edited by M.T.S. and M.H. All authors helped to write the manuscript. Ethics of human subject participation: Not applicable.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S1368980018003907





