It has been recognised for many years that patients with psychiatric illnesses, especially schizophrenia, smoke to excess. However, recently there has been a resurgence of interest in the high prevalence of nicotine addiction in patients with schizophrenia. It has become increasingly clear that heavy cigarette smoking is intimately associated with the schizophrenic illness and that this may have implications for the underlying neurobiology of schizophrenia.
Rates of cigarette smoking
The number of patients with schizophrenia who smoke is very high (see Box 1). One study reported the prevalence to be 88%, nearly three times the rate in the general population and higher than the elevated rates of smoking in patients with other psychiatric illnesses. The increased prevalence persists even after adjustment for marital status, alcohol use and socio-economic status (Reference Hughes, Hatsukami and MitchellHughes et al, 1986).
Box 1. Rates of smoking in schizophrenia
-
• The rate of smoking in people with schizophrenia is at least two to three times that in the general population
-
• Patients who smoke, smoke at heavier rates than in the general population
-
• Most patients start smoking in their teens, before the illness begins
A number of more recent cross-sectional studies from different countries have reported high rates of smoking in patients with schizophrenia (Reference Goff, Henderson and AmicoGoff et al, 1992; Reference Chong and ChooChong & Choo, 1996). One large study of 360 state hospital in-patients, of whom 237 were diagnosed as having schizophrenia or schizo-affective disorder, found that the overall prevalence of smoking was 85%, and 93% in young male patients with schizophrenia (Reference De Leon, Dadvand and CanusoDe Leon et al, 1995). Smoking occurs at much higher rates than other types of substance misuse or dependence, which have been shown also to be elevated among patients with schizophrenia.
In our own study (Reference Kelly and McCreadieKelly & McCreadie, 1999) we found that the average age when patients with schizophrenia started smoking was the same as in the general population, namely mid-teens; 90% of patients who smoked had started smoking before their illness began.
Patients with schizophrenia who smoke are also heavier smokers than those in the general population and those with other psychiatric disorders. In our own study, 68% of patients with schizophrenia who smoked were classed as heavy smokers (25 or more cigarettes daily) compared with only 11% of the general population who smoke. In another study (Reference Olincy, Young and FreedmanOlincy et al, 1997), patients with schizophrenia who smoked had much higher levels of the nicotine metabolite cotinine in comparison with other smokers, confirming our finding. Excessive smoking tends to be a lifelong habit among patients with schizophrenia. The proportion of those who quit is lower than in the general population; in our study of a population of patients with schizophrenia, only 8% of males were ex-smokers, compared with 31% of males in a local general population.
Why do patients with schizophrenia smoke?
Why do patients with schizophrenia smoke at these excessive rates? There are three possible explanations for the association: something about the illness leads patients to smoke; smoking is another risk factor for schizophrenia; or a third factor leads to both schizophrenia and smoking (see Box 2).
Box 2. Why do patients with schizophrenia smoke?
-
• Aspects of the illness might lead more patients to smoke
-
• Smoking might be an aetiological factor in schizophrenia
-
• Genetic and/or environmental factors might lead both to nicotine addiction and to schizophrenia
The first possibility has received most attention. It has been suggested that smoking may be a marker of a more severe illness process (Reference De LeonDe Leon, 1996). Smokers are more often young and male; they have an earlier onset of illness, increased numbers of hospital admissions and receive higher doses of neuroleptic medication (Reference Goff, Henderson and AmicoGoff et al, 1992; Reference Ziedonis, Kosten and GlazerZiedonis et al, 1994). In addition, smokers have more severe symptoms with higher scores on the Brief Psychiatric Rating Scale (Reference Overall and GorhamOverall & Gorham, 1962) for positive and negative symptoms (Reference Goff, Henderson and AmicoGoff et al, 1992; Reference Chong and ChooChong & Choo, 1996; Reference Ziedonis, Kosten and GlazerZiedonis et al, 1994).
Another suggestion is that patients smoke as a form of self-medication with nicotine, which may help regulate a dysfunctional mesolimbic dopamine system. It may increase dopamine release in the pre-frontal cortex and alleviate positive and negative symptoms (Reference Lavin, Siris and MasonLavin et al, 1996). Worsening of psychotic symptoms on nicotine withdrawal has been reported (Reference Dalack and Meador-WoodruffDalack & Meador-Woodruff, 1996). It has also been shown that nicotine administration enhances cognitive performance on a number of tasks. However, in general, patients with schizophrenia who smoke report similar reasons to other smokers (“addicted”, “relaxation” and “to calm down”), with only 17% of patients reporting that smoking improved psychotic symptoms.
As we have found that most patients who smoke began to do so before psychotic aspects of the illness appeared, premorbid characteristics are perhaps important. It is noteworthy that in our study patients who smoked were as children more poorly adjusted socially than those who were not smokers.
Patients with schizophrenia may smoke heavily as a result of antipsychotic medication, which produces marked dopamine receptor blockade. Possibly, a very high level of smoking is necessary to overcome this blockade and produce the reward effects. It has been shown that, compared with baseline, patients with schizophrenia smoke more after starting haloperidol (Reference McEvoy, Freudenreich and LevinMcEvoy et al, 1995). It has also been shown in a placebo-controlled study that after a single dose of haloperidol, normal subjects smoked significantly more during the following hour, as measured by blood nicotine levels (Reference Dawe, Gerada and RussellDawe et al, 1995).
A second explanation for the association between schizophrenia and smoking is that smoking acts as an aetiological risk factor for schizophrenia. It may be that repeated activation by nicotine of the mesolimbic system over a long time precipitates the onset of schizophrenia in vulnerable individuals. We found that the earlier the age of starting smoking, the earlier was the onset of psychotic illness in women (Reference Kelly and McCreadieKelly & McCreadie, 1999). Interestingly, nicotine acts like other drugs of addiction such as cocaine and amphetamine, activating the mesolimbic dopamine system (Reference Pontieri, Tanda and OrziPontieri et al, 1996); this effect appears to be of critical importance for the reinforcing and reward properties of the drug. Also, nicotine has been shown to increase burst activity in the dopamine neurons of the ventral tegmental area, a form of firing pattern of these cells that is physiologically associated with basic motivational processes underlying learning and cognition (Reference IversenIversen, 1996).
Third, genetic and/or environmental factors might predispose individuals to develop both schizophrenia and nicotine addiction. Much work in the genetics of both schizophrenia (Reference Maier and SchwabMaier & Schwab, 1998) and nicotine addiction (Reference ClarkeClarke, 1998) has focused on the dopamine receptor system.
Consequences of smoking
Morbidity and mortality
Smoking remains the single greatest preventable cause of death in our society. It appears to engender both general and specific health risks for patients with schizophrenia. There is no doubt that cigarette smoking causes considerable morbidity and mortality, but there are no epidemiological data addressing smoking-related morbidity and mortality in schizophrenia. Previous work has shown that among people with schizophrenia life expectancy is estimated as being 20% less than in the general population. There is an increase in deaths from natural causes and the most common causes are cardiovascular and respiratory disease, both smoking-related (Reference Mortensen and JuelMortensen & Juel, 1993). The markedly elevated prevalence of smoking is clearly an important potential factor in explaining the elevated mortality in schizophrenia.
Medication and side-effects
Smoking has been shown to decrease plasma levels of neuroleptics by inducing hepatic microsomal enzymes (Reference Salokangas, Saarijarvi and TaiminenSalokangas et al, 1997). Therefore, patients who smoke require larger doses of drugs than non-smokers to achieve the same therapeutic effect (Reference Lohr and FlynnLohr & Flynn, 1992). It has also been reported that smokers have been prescribed neuroleptics at twice the daily dose of non-smokers while exhibiting significantly less neuroleptic-induced parkinsonism. Spontaneous abnormal involuntary movements indistinguishable from tardive dyskinesia have also been reported in a general population sample of older males who smoke (Reference Nilsson, Waller and RosengrenNilsson et al, 1997). It would seem likely, therefore, that there is an association between tardive dyskinesia and smoking in schizophrenia. However, in three previous studies, only one showed that tardive dyskinesia was more prevalent among smokers (Reference Yassa, Lal and KorpassyYassa et al, 1987); two found no relationship (Reference Menza, Grossman and Van HornMenza et al, 1991; Reference Chiles, Cohen and RolandChiles et al, 1993).
Economic considerations
Cigarettes are not cheap. We have recently carried out some simple arithmetic in relation to smoking and schizophrenia (Reference McCreadie and KellyMcCreadie & Kelly, 2000). Our patients smoke on average 26 cigarettes per day. At £2.79 per packet, this works out at £1300 per year. Very few of our patients work. We reckon that probably up to one-third of state benefits is spent on cigarettes. Of the cost of a packet of cigarettes, 87% is tax. Thus, patients, through their smoking habits, are contributing very substantially to the cost of their own care.
Smoking cessation
Smoking cessation rates are poor in heavy smokers and even lower in those with psychiatric illness. Attempts to get patients with schizophrenia to stop smoking have met with only limited success. There is often a perception that it will be unsuccessful and will deprive individuals of one of their few pleasures. This view is inherently discriminatory. In our own study (Reference Kelly and McCreadieKelly & McCreadie, 1999) a third of patients reported that they wanted to quit for health reasons. Clearly, smokers with schizophrenia have a severe nicotine addiction, and pharmacological and psychological support with smoking cessation needs to be addressed.
Box 3. Management issues
-
• Smoking must be implicated in the increased mortality in schizophrenia
-
• Smokers require higher doses of antipsychotic medication
-
• A substantial proportion of the income of smokers with schizophrenia is spent on cigarettes
-
• Patients with schizophrenia have the right to be offered treatment for their nicotine addiction
There have been few studies that have looked at cessation methods (reviewed by Lavin et al, 1996). Smoking bans on in-patient psychiatric units have generated naturalistic reports; usually the most severely addicted patients are extremely resourceful and continue to smoke. Smoking cessation groups, nicotine gum, nicotine patches and clonidine patches have all been tried with both in-patients and out-patients, with poor results. For example, the six-month cessation rate was only 12-13% with group therapy alone (Reference Addington, el-Guebaly and CampbellAddington et al, 1998) or in combination with nicotine reduction therapy (Reference Ziedonis and GeorgeZiedonis & George, 1997). Outcome studies are urgently necessary to evaluate the effectiveness of smoking cessation programmes (e.g. in-patient v. out-patient programmes, nicotine replacement, behavioural techniques and so on). For the severely addicted, the following combinations may be tried: combined gum and patch therapy; bupropion and nicotine patch; nicotine nasal spray; or nicotine inhaler (details available from the author upon request).
The use of bupropion is interesting. In normal subjects, sustained-release bupropion, an antidepressant, alone or in combination with a nicotine patch, resulted in significantly higher long-term rates of smoking cessation (30.3 and 35.5%, respectively) than use of either the nicotine patch alone (16.4%) or placebo (15.6%) (Reference Jorenby, Leischow and NidesJorenby et al, 1999). In a recent case report (Reference Evins and TisdaleEvins & Tisdale, 1999), sustained-release bupropion was successfully used with a chronically ill male patient with schizophrenia. Why might an antidepressant such as bupropion be helpful in smoking cessation? It has been suggested that long-term administration of bupropion and nortriptyline, adrenergic antidepressants, produces a significantly increased responsivity to stimulation of the ventral tegmental dopamine cells. This is not seen with selective serotonin reuptake inhibitors (SSRIs). This may be why buproprion and nortriptyline but not SSRIs increase smoking abstinence. For a fuller comment on this possibility, see Glassman (1998).
We have recently reported (Scottish Schizophrenia Research Group, 2000) that the prevalence of smoking in first-episode patients is just as high as in chronic patients, but that the number of cigarettes smoked per day is no higher than that in smokers in the general population. Perhaps it is at this early stage that attempts to help patients to stop smoking should be made.
In conclusion, despite the often limited resources of patients with schizophrenia, they commonly view cigarette smoking as a necessity. Most patients with schizophrenia smoke at high rates and few manage to stop. This dramatically elevated prevalence of smoking among individuals with schizophrenia raises the intriguing possibility that nicotine use and schizophrenia have some shared underlying neurobiology.
Multiple choice questions
-
1. Patients with schizophrenia who smoke:
-
a smoke at rates higher than those with other psychiatric conditions
-
b in the early stages of the illness smoke more cigarettes daily than general population smokers
-
c start smoking at a later age than general population smokers
-
d quit at the same rates as general population smokers.
-
-
2. Nicotine may:
-
a regulate a dysfunctional mesolimbic dopamine system
-
b improve psychiatric symptoms on withdrawal
-
c impair cognitive performance
-
d prevent relapse.
-
-
3. Smoking cessation in schizophrenia:
-
a can be achieved more readily than in other psychiatric conditions
-
b is unwanted by more than two-thirds of patients themselves
-
c should probably be attempted at the early stages of the illness
-
d might include combined nicotine gum and patch therapy.
-
MCQ answers
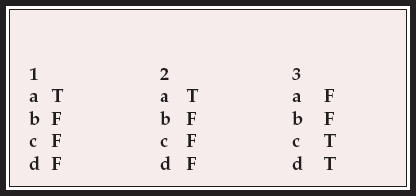
| 1 | 2 | 3 | |||
|---|---|---|---|---|---|
| a | T | a | T | a | F |
| b | F | b | F | b | F |
| c | F | c | F | c | T |
| d | F | d | F | d | T |



eLetters
No eLetters have been published for this article.