The association between adiposity and pro-inflammatory and pro-thrombotic risk factors for CVD has been well documented in cross-sectional studies(Reference Brooks, Blaha and Blumenthal1) in adults. The longitudinal association between change in adiposity and such parameters remains uncertain. The objectives of this study were to firstly examine the relationship between adiposity in adolescence and pro-inflammatory and pro-thrombotic risk factors in young adulthood and then to examine the relationship between change in adiposity during this timeframe and risk factor status in young adulthood.
The analyses are based on data from the Young Hearts (YH) cohort; a longitudinal study of CVD risk factors in a representative sample of young people in Northern Ireland. In total, 476 subjects (245 males and 231 females) were assessed at age 15 and then again in young adulthood (mean age 22.6 years). Indices of fatness at age 15 included BMI and body fat % that was derived from the sum of four skin folds thickness. Main outcome measures included C-reactive protein (CRP), fibrinogen and white cell count (WCC); these were assessed in a fasting blood sample only at young adulthood. Subjects were categorised as normal weight or overweight/obese using international BMI cut-offs for adolescents(Reference Cole, Bellizzi and Flegal2) and adults(3). CRP values were divided into two groups according to CVD risk; <3.0 mg/l lower risk and >3.0 mg/l higher risk(Reference Pearson, Mensah and Alexander4).
As shown in the first table below, significant associations were observed between adolescent adiposity measurements (BMI and body fat %) and adult pro-inflammatory and pro-thrombotic risk factors (CRP, fibrinogen and WCC) after adjusting for potential confounders. These associations were attenuated after further adjusting for adult adiposity.
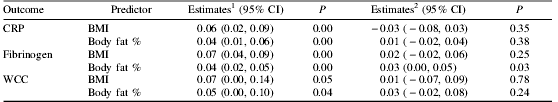
Data are Beta values and 95% CI. 1Adjusted for sex, social class, pubertal status, history of parental heart attack, smoking, adolescent blood pressure and blood lipoproteins. 2Further adjustment for adult BMI and body fat %.
The table below presents the OR and 95% CI for the presence of high CRP (>3.0 mg/l, level above the risk threshold) at adulthood according to change in weight status between adolescence and young adulthood. Odds of high CRP in adulthood were significantly higher in those who were overweight/obese at both time points and those who gained weight over time compared to those who remained normal weight.
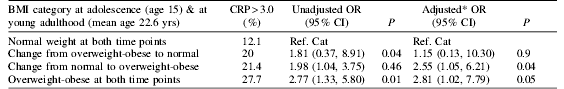
* Adjusted for gender, pubertal status, social class (adulthood), smoking (adulthood), alcohol intake (adulthood), parental history of heart attack, birth weight.
In conclusion, excess adiposity in adolescence may assist in predicting future CV risk status. Furthermore, remaining normal weight or losing weight over time may help promote favourable inflammatory states in later life. These results reinforce the need to prevent and address obesity early in life.



