MethodFollowing ethical approval, clinicians in each of Ireland’s four Health Service Executive (HSE) areas were contacted, informed about the study and were invited to participate. Clinicians identified all cases who had reached the transition boundary (i.e. upper age limit for that CAMHS team) between January and December 2010. Data were collected on clinical and socio-demographic details and factors that informed the decision to refer or not refer to the AMHS, and case notes were scrutinised to ascertain the extent of information exchanged between services during transition.
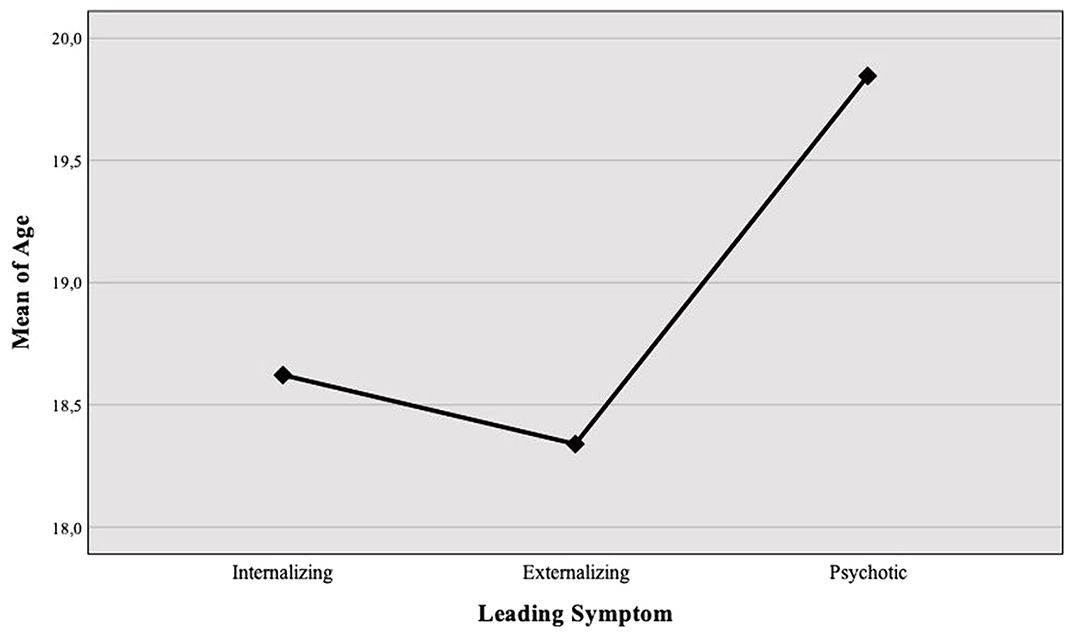
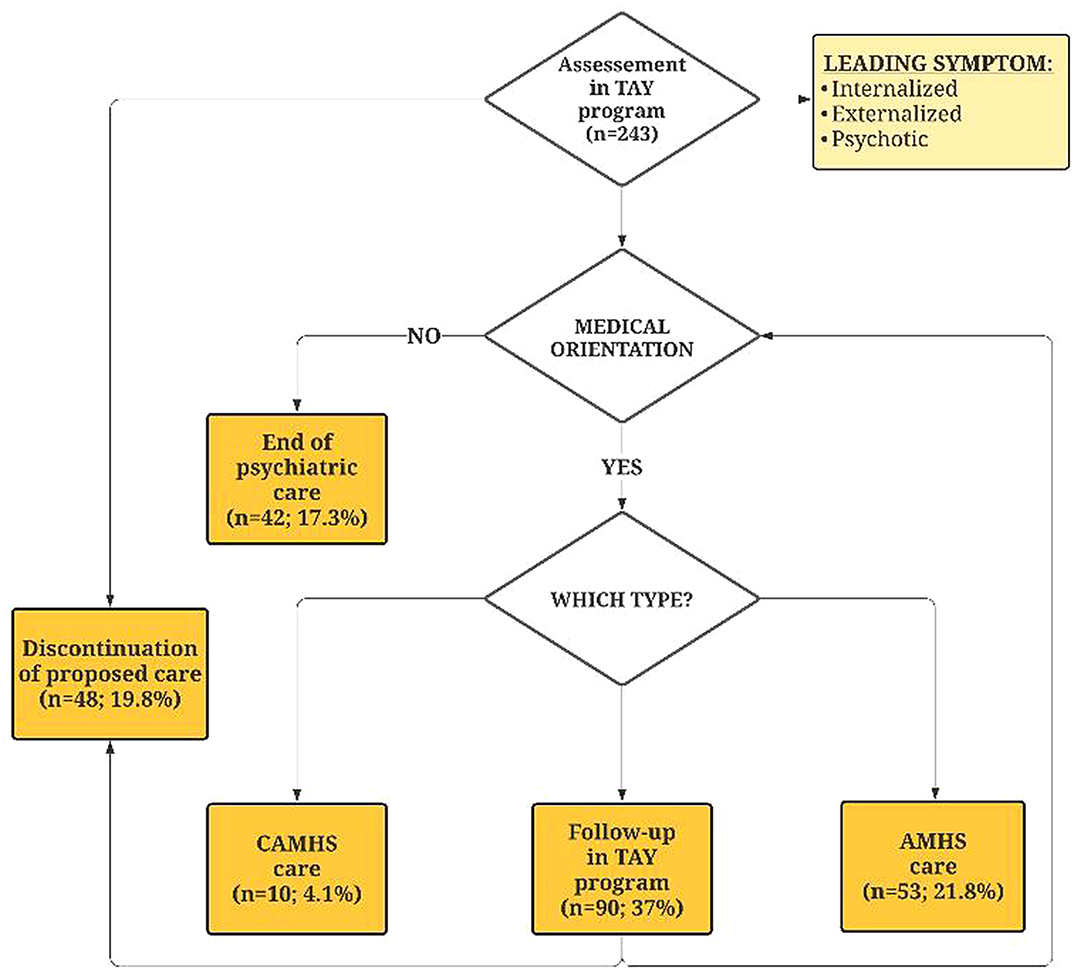
ResultsA total of 62 service users were identified as having crossed the transition boundary from nine CAMHS [HSE Dublin Mid-Leinster (n=40, 66%), HSE South (n=18, 30%), HSE West (n=2, 3%), HSE Dublin North (n=1, 2%)]. The most common diagnoses were attention deficit hyperactivity disorder (ADHD; n=19, 32%), mood disorders (n=16, 27%), psychosis (n=6, 10%) and eating disorders (n=5, 8%). Forty-seven (76%) of those identified were perceived by the CAMHS clinician to have an ‘on-going mental health service need’, and of these 15 (32%) were referred, 11 (23%) young people refused and 21 (45%) were not referred, with the majority (12, 57%) continuing with the CAMHS for more than a year beyond the transition boundary. Young people with psychosis were more likely to be referred [χ2 (2, 46)=8.96, p=0.02], and those with ADHD were less likely to be referred [χ2 (2, 45)=8.89, p=0.01]. Being prescribed medication was not associated with referral [χ2 (2, 45)=4.515, p=0.11]. In referred cases (n=15), there was documented evidence of consent in two cases (13.3%), inferred in another four (26.7%) and documented preparation for transition in eight (53.3%). Excellent written communication (100%) was not supported by face-to-face planning meetings (n=2, 13.3%), joint appointments (n=1, 6.7%) or telephone conversations (n=1, 6.7%) between corresponding clinicians.
ConclusionsDespite perceived on-going mental health (MH) service need, many young people are not being referred or are refusing referral to the AMHS, with those with ADHD being the most affected. CAMHS continue to offer on-going care past the transition boundary, which has resource implications. Further qualitative research is warranted to understand, in spite of perceived MH service need, the reason for non-referral by the CAMHS clinicians and refusal by the young person.