The term ‘wife beating’ was first used in the 1856 campaign for divorce reform in the UK, and its successor, ‘domestic violence’ has been conceptualised to be a problem of male perpetrators and female victims. The more recent term ‘intimate partner violence’ is used to differentiate violence between two people who are involved in a romantic relationship from other types of domestic violence such as child abuse and elderly abuse.
Intimate partner violence is identified in multiple settings, from the general practitioner's office (Reference Porcerelli, Cogan and WestPorcerelli et al, 2003) to in-patient psychiatric units (Reference Heru, Stuart and RaineyHeru et al, 2006). Patients agree that physicians should ask about such violence and believe that they can be helpful in dealing with it (Reference Burge, Schneider and IvyBurge et al, 2005). Indeed, compared with 5 years ago, family physicians are asking more frequently about intimate partner violence, resulting in improved patient mental health and acceptance of treatment (Reference Glowa, Frazier and WangGlowa et al, 2003). One significant hindrance to physicians asking about intimate partner violence is their lack of knowledge about the behaviour, how to refer patients and what treatments are effective. This article will increase the general psychiatrist's understanding of this type of violence and how to assess what treatment options are best for their patients.
Gender distribution
It is important to recognise that intimate partner violence is no longer considered just as a situation involving a male perpetrator and a female victim, although women remain more likely to be injured by partner violence than men (Reference Whitaker, Haileyesus and SwahnWhitaker et al, 2007). Since many community and clinical studies have found that intimate partner violence is often bidirectional, where each partner is both an aggressor and a victim, a broader definition is now considered more applicable. The US National Comorbidity Survey revealed rates of victimisation using severe physical aggression of 6.5% against women and 5.5% against men (Reference Kessler, Molnar and FeurerKessler et al, 2001). A meta-analysis of 82 studies including both community and clinical samples found that more women than men reported physical aggression in their relationships (Reference ArcherArcher, 2000). In an out-patient sample of couples seeking marital therapy, 64% of wives and 61% of husbands were classified as aggressive (Reference Langhinrichsen-Rohling and VivianLanghinrichsen-Rohling & Vivian, 1994). In 272 engaged couples, 44% of women and 31% of men reported physical violence towards their partners (Reference O'Leary, Barling and AriasO'Leary et al, 1989). Thus, there is a range of intimate partner violence from the classic male perpetrator and female victim, to the couple who engage in mutual violence through to the less common female aggressor and male victim.
Marital dysfunction
Without intervention, physical aggression in relationships continues. One study found that individuals who were physically aggressive before marriage remained physically aggressive 30 months after they had married (Reference O'Leary, Barling and AriasO'Leary et al, 1989). Another showed that nearly 50% of couples with severe physical aggression remained severely aggressive after 24 months (Reference Jacobson, Gottman and GortnerJacobson et al, 1996). It seems that the more severe or chronic the physical aggression is in newly-wed couples, the more likely it is to continue (Reference Quigley and LeonardQuigley & Leonard, 1996). Verbal and physical aggression before marriage predicts physical aggression 24 months after the ceremony (Reference Schumacher and LeonardSchumacher & Leonard, 2005). Another longitudinal study found that marital dysfunction was more common among aggressive than non-aggressive couples (70 v. 38%) especially in severely aggressive compared with moderately aggressive couples (93 v. 46%) (Reference Lawrence and BradburyLawrence & Bradbury, 2001).
Associated psychopathology
In addition to marital dysfunction, intimate partner violence is associated with individual psychopathology, with rates of 54–68% for major depressive disorders and 50–75% for post-traumatic stress disorder in female victims (Reference Nixon, Resick and NishithNixon et al, 2004). Excessive alcohol use is associated with intimate partner violence: with rates of 45% for men and 20% for women (Reference Roizen and MartinRoizen, 1993). Female victims and female perpetrators report excessive alcohol use (Reference Stuart, Moore and RamseyStuart et al, 2004). Women arrested for intimate partner violence have high rates of post-traumatic stress disorder, depression, generalised anxiety disorder, panic disorder, substance use disorders, borderline personality disorder and antisocial personality disorder (Reference Stuart, Moore and GordonStuart et al, 2006a ). None of these studies comments on whether the violence causes or is a result of the psychopathology. We do know, however, that witnessing or being a victim of intimate partner violence as a child is associated with perpetrating violence as an adult (Reference Ernst, Weiss and Enright-SmithErnst et al, 2006).
Regardless of the aetiology, when intimate partner violence is treated, there is a reduction in depressive symptoms (Reference Kernic, Holt and StonerKernic et al, 2003). Successful treatment of alcohol misuse and dependence with couples therapy also reduces such violence (Reference O'Farrell, Fals-Stewart and MurphyO'Farrell et al, 2004). No studies have examined whether intimate partner violence is reduced as a consequence of treating comorbid psychiatric illnesses such as depressive disorders or post-traumatic stress disorder, although one study suggests that an integrated approach to the treatment of trauma and comorbid disorders may be helpful for women victims (Reference Morrissey, Jackson and EllisMorrissey et al, 2005).
Research into treatment options
Victims
Studies that target victims of intimate partner violence usually have separation of the (female) victim from the (male) abuser as their goal. Simply assessing for intimate partner violence and offering a referral can interrupt the violence and its associated trauma (Reference McFarlane, Groff and O'BrienMcFarlane et al, 2006). In McFarlane et al’s study, 360 abused women recruited from US urban public primary care clinics were compared on two interventions: a referral card and a 20 min session with a nurse following a case management protocol. After 2 years, both treatment groups reported significantly fewer threats of abuse, assaults, risks for homicide and events of work harassment. Compared with baseline, both groups adopted significantly more safety-promoting behaviours. Therefore simple disclosure of abuse in primary care clinics is associated with the same reduction in violence and increase in safety behaviours (safety planning such as that outlined in Box 1) as a 20 min case management intervention.
Box 1 Safety planning
-
• Memorise important phone numbers of people to call in emergency
-
• If your children are old enough, teach them important phone numbers, including when to dial 999
-
• Keep information about domestic violence in a safe place, where your abuser won't find it, but where you can get it when you need to review it
-
• Keep change for pay phones with you at all times
-
• If you can, open your own bank account
-
• Stay in touch with friends. Get to know your neighbours. Don't cut yourself off from people, even if you feel like you want to be alone
-
• Rehearse your escape plan until you know it by heart
-
• Leave a set of car keys, extra money, change of clothes and copies of important documents with a trusted friend or relative: your own and your children's birth certificates, children's school and medical records, bank books, welfare identification, passport/green card, immigration papers, social security card, lease agreements or mortgage payment books, insurance papers, important addresses and telephone numbers
Brief telephone intervention with victims of intimate partner violence – six phone calls for an overall total time of 60 min over 8 weeks – increases safety-promoting behaviours (Reference McFarlane, Malecha and GistMcFarlane et al, 2004). This study randomly assigned 150 women who sought civil protection orders to the telephone intervention or to a control group. Analysis showed that the women in the intervention group (n = 75) practised significantly (P < 0.01) more safety-promoting behaviours than women in the control group at each assessment, and results were sustained at 18 months.
Reference Wathen and MacMillanWathen & MacMillan (2003) reviewed articles that focused on treatment of female victims from a primary care perspective. They found no high-quality evidence to evaluate the effectiveness of shelter stays in reducing violence. Among women who had spent at least 1 night in a shelter, they found fair evidence that those who received a specific programme of advocacy and counselling services reported a decreased rate of re-abuse and an improved quality of life. The benefits of several other intervention strategies were found to be unclear, primarily because of a lack of adequately designed research.
More specific interventions are also effective in reducing intimate partner violence. Pregnant women attending an antenatal clinic in a public hospital in Hong Kong reported less intimate partner violence after receiving a 6-week empowerment intervention, compared with a control group receiving standard care for abused women. Six weeks after childbirth, the experimental group reported higher physical functioning, less psychological (but not sexual) abuse, minor (but not severe) physical violence and had significantly lower postnatal depression scores (Reference Tiwari, Leung and LeungTiwari et al, 2005). This study, however, followed participants for 6 only weeks.
It is important to identify as broad a range of outcomes as possible when assessing the effect of an intervention. Women recruited from shelters who received a 10-week intervention using trained advocates were twice as likely to be free of violence as a control group at 2 years follow-up. However, after 3 years, the advocacy programme's effect did not continue. Nevertheless, the women who received the intervention had an improved quality of life and more social support (Reference Bybee and SullivanBybee & Sullivan, 2005).
Another approach to treatment is to match interventions to the woman's stage of change, i.e. pre-contemplative, contemplative, preparation, action and maintenance. An in-depth study examining 23 female victims of intimate partner violence suggests that women in the early or precontemplative stage benefit most from receiving information about what constitutes abuse (Reference Burke, Denison and GielenBurke et al, 2004). Interventions tailored to the other stages of change would likewise be stage-specific and possibly more likely to be effective, although this study did not test these assumptions.
In summary, simple interventions for female victims of domestic abuse or intimate partner violence (Box 2) are quite successful in the short-term. Even long-term effects are apparent on outcomes other than reports of violence. These studies certainly support the helpfulness of the simple action of identifying abuse. We found no studies that discussed treatment of male vicitms.
Box 2 Effective treatments for victims
-
• Assess and offer a referral
-
• Brief telephone intervention
-
• Increase social support
-
• 6-week empowerment intervention
-
• Provision of information about abuse
Perpetrators
Treatment for perpetrators of intimate partner violence is usually in gender-specific (i.e. all male) groups, and focused on educating the perpetrators about different ways to express anger and reduce interpersonal controlling behaviour. Treatment for male perpetrators is usually court-ordered and therefore not voluntary.
A meta-analysis of 22 studies of gender-specific treatment for male perpetrators indicates that treatment effect sizes are small (Reference Babcock, Green and RobieBabcock et al, 2004). The treatments evaluated were similar in orientation, all being based on the Duluth model. According to this model, the primary cause of male domestic violence is patriarchal ideology and societal sanctioning of men's use of power and control over women. These programmes are not considered to be therapy. Rather, group facilitators lead consciousness-raising exercises to challenge the man's perceived right to control or dominate his partner. A fundamental tool of the Duluth model is the ‘power and control wheel,’ which illustrates that violence is part of a pattern of behaviour including intimidation, male privilege, isolation, emotional and economic abuse, rather than isolated incidents of abuse or cyclical explosions of pent-up anger or painful feelings. The treatment goals of the Duluth model are to help men change from using the behaviours on the power and control wheel, which result in authoritarian and destructive relationships, to using the behaviours on the ‘equality wheel,’ which form the basis for egalitarian relationships (Reference Pence and PaymarPence & Paymar, 1993).
The meta-analysis included only studies in which treatment results could be compared with a control group or where those who dropped out of treatment were included in the analysis. Forty-eight studies were excluded because of weak methodological designs. For the remaining studies, there was no difference in effect size by treatment type. Of concern is the report that men-only treatment groups lead some men to support negative attitudes and aggressive behaviours towards women.
Conjoint treatment
Owing to the popularity of the Duluth model, conjoint (couples) treatment for intimate partner violence has been considered inadvisable. Three main reasons are given, all relating to the female partner: women will be inhibited from expressing themselves fully because of fears of reprisal from their husbands; women may come to feel partly responsible for their husband's aggression; and comments made by the women in the joint session may place them at risk of further violence. However, in a study that measured rates of fear in women who participated in group conjoint treatment, no higher rates of fear of the partner or increased rates of violence during or after treatment occurred (Reference O'Leary, Heyman and NeidigO'Leary et al, 1999).
Conjoint treatment for male perpetrators has been pioneered in several states in the USA. In California, a comparison study of 49 court-referred perpetrators found that gender-specific treatment and conjoint couples treatment were equally successful in reducing intimate partner violence (Reference Brannen and RubinBrannen & Rubin, 1996).
A conjoint treatment model
In Virginia, a model of conjoint treatment used when the male partner has perpetrated mild-to-moderate violence and both partners want to remain together is successful (Reference Stith, McCollum, Rosen and KaslowStith et al, 2004). The screening process in Stith et al’s study excluded severe violence and substance misuse. The model consists of two steps: the men and women first attend gender-specific groups and then participate in conjoint treatment, either in individual couples therapy or in multi-couple group therapy. The stages of treatment in the multi-couple group therapy are outlined in Box 3. No escalation in violence occurred when risk assessment screening and experienced therapists were used.
Box 3 The stages of multi-couple group therapy
-
• Stage 1 engages the participants in the therapy process and develops a vision of a violence-free relationship
-
• Stage 2 focuses on enhancing the non-violent marital relationship and couples are taught new skills in communication, negotiation and so on
-
• Stage 3 focuses on solidifying change, anticipating problems and determining whether further treatment is necessary
-
• Stage 4 is the termination stage, which focuses on affirmation of progress and change
(Reference Stith, McCollum, Rosen and KaslowStith et al, 2004)
Effective strategies for minimising risk include the use of a ‘no violence contract’ and a time-out tool (Reference Rosen, Matheson and StithRosen et al, 2003). Six months after treatment, male violence recidivism rates were significantly lower for the multi-couple group (25%) than for either the individual couple condition (43%) or the comparison group (66%). Marital aggression and the acceptance of wife battering decreased significantly among men who participated in multi-couple group therapy, but not among those who participated in individual couples therapy or the comparison group.
Does treatment work?
The San Diego Navy Experiment is frequently discussed as an example of the ineffectiveness of treatment for male perpetrators of intimate partner violence. In this study 861 Naval personnel who had assaulted their wives were assigned to one of three treatment conditions or to a control condition. The three treatment conditions were: a gender-specific (men's) group treatment; a conjoint (couples) group treatment; or ‘rigorous monitoring’, i.e. individual counselling, periodic record searches and ongoing interviews with spouses. In the control condition the only service provided was brief stabilisation and safety planning (Box 1) for the wives (Reference DunfordDunford, 2000). The men's group used a cognitive–behavioural model of change, and met weekly for 6 months and then monthly for 6 months for a total of 26 sessions. The didactic portion of the sessions addressed perpetrator attitudes and values regarding women and the men were taught skills such as cognitive restructuring, empathy enhancement, communication skills, anger modification and management of jealousy. The conjoint group also had 26 sessions and was organised in a similar way to the men's group, with didactic and process components. In the rigorous monitoring group, the men were seen monthly for 12 months for individual counselling, and their wives were called monthly and asked about new instances of abuse. Progress reports were sent monthly to the men's commanding officers. The men in the control group did not receive any treatment.
Dunford demonstrated significant reductions in violence across all three interventions, with no significant outcome differences between treatment formats and no difference noted compared with the control group formats. According to their wives, 83% of the men did not injure them again during the 1-year follow-up.
Summary
Rigorous studies using control groups have shown that male perpetrators do not respond to the traditional gender-specific Duluth model (Box 4). Multi-couple group therapy has been shown to be effective in select studies involving court-referred perpetrators. Aggressors who are mandated into treatment will require programmes that are sanctioned by the court. Both male and female perpetrators of violence who seek help voluntarily are likely to be more motivated and treatment more successful.
Box 4 Research results
-
• Meta-analysis of 22 gender-specific treatment studies yield a small treatment effect size
-
• California conjoint treatment equal to gender-specific treatment
-
• Virginia conjoint treatment shows significant results for multi-couple groups
-
• San Diego Navy study indicates no difference for three treatments over control group
Treatment for couples in the community
Few practitioners are trained in or support the use of couples therapy where intimate partner violence exists. Nevertheless, several studies have been conducted involving couples who have entered treatment voluntarily (rather than through victim protection or the legal system). These treatments are summarised in Box 5.
Box 5 Effective treatment for couples in the community
-
• Gender-specific treatment and group conjoint treatment
-
• Treatment of alcoholism with a sobriety contract, behavioural assignments and relapse prevention
Reference O'Leary, Heyman and NeidigO'Leary et al(1999) compared gender-specific treatment with 14-week conjoint group treatment in a community sample of 75 couples who were recruited via advertisements offering treatment for repeated acts of husband-to-wife physical aggression. Inclusion criteria were at least two acts of physical aggression in the past year. Both treatment groups followed a cognitive–behavioural programme focusing on psychoeducation, anger control techniques and communication skills. Both groups reported a reduction of physical violence at the end of the treatment and at 1 year follow-up, although only 25% of husbands remained violence free. The only difference found between groups was that husbands in conjoint treatment reported improved marital satisfaction. Thus, gender-specific treatment and group conjoint treatment had equivalent outcomes for husband-to-wife violence in the community.
Successful treatment of alcoholism can significantly reduce intimate partner violence (Reference Stuart, Meehan and MooreStuart et al, 2006b ). Reference O'Farrell, Fals-Stewart and MurphyO'Farrell et al(2004) enrolled 303 male married alcoholics into couples treatment. Greater treatment involvement was related to greater reduction in violence. The treatment consisted of a sobriety contract (Box 6), behavioural assignments and relapse prevention. The behavioural assignments were aimed at increasing positive feelings, shared activities and constructive criticism. At the end of treatment, each couple completed a continued recovery plan to be reviewed quarterly for 2 years. The reduction in violence was mediated by reduced problem drinking and enhanced relationship functioning.
Box 6 The sobriety contract
-
• The patient states their intention not to drink
-
• The spouse expresses support for their efforts to stay abstinent and records the daily performance of the contract on a calendar.
-
• Both partners agree not to discuss past drinking or fears
A small number of practitioners have well-established programmes for the treatment of intimate partner violence in couples, but these approaches have not been subjected to empirical study. Reference GoldnerGoldner (2004) at the Ackerman Institute for Family Therapy in New York states that ‘conjoint abuse work can create a transitional space between public and private – a space in which these couples can tell these horrible stories and retell and rework them from multiple perspectives’ (p. 371). The role of the therapist is to ‘help clients develop a rich psychological understanding of the abuse’ (p. 349) without blame or shame and without letting the perpetrators avoid responsibility for their actions. Goldner uses attachment theory and feminist theory (especially the work of Jessica Benjamin) and views the work of the family therapist as inserting a moral perspective. Goldner highlights clinical multiplicity, with abuse and coercion coexisting alongside intense love and genuine friendship, making it hard for friends and family as well as clinicians to maintain empathic objectivity for the couple. Goldner believes that the mutative factor in any therapy includes bearing witness and helping abusers accept responsibility for their actions.
Reference Jory and AndersonJory & Anderson (2000) practice couples therapy based on accountability and a theory of intimate justice. In this model, the therapist teaches the aggressor to be accountable for the aggression. This usually results in psychological distress, which the authors believe represents positive change in the aggressor. The victim then describes the ‘anguish of abuse’. Therapists simultaneously engage both the victim and the abuser by creating two therapeutic environments, one that affirms the victim and one that challenges the abuser.
A third approach is solution-focused treatment for perpetrators of intimate partner violence. This offers a ‘strengths perspective’, holding individuals accountable for finding solutions, rather than focusing on the problems (Reference Lee, Uken and SeboldLee et al, 2004).
Conclusions
Interventions for intimate partner violence range from simply asking about it and offering a referral to victims, to highly structured intensive couples treatment. The reported success of interventions is dependent on the population studied and the goal of the intervention. Most studies have involved female victims who have come to the attention of the authorities or male perpetrators mandated to treatment by the courts. In community studies, couples must be highly motivated to enter treatment for a condition that is socially stigmatised. The success of treating comorbidity such as alcoholism suggests the potential of including intimate partner violence within treatments for depressive disorders and post-traumatic stress disorders.
A guide for the clinician
Several conclusions can be drawn that are of help to the clinician faced with a patient who describes intimate partner violence. The following steps can guide the clinician.
Box 7 Risk factors for lethality
-
• Uncontrolled continuous use of alcohol or drugs
-
• Fear of serious injury from their partner
-
• Severe violence that has resulted in the victim requiring medical attention
-
• Conviction for a violent crime or violation of a restraining order
-
• Prior use of a weapon against the partner, prior threat to kill the partner
-
• Stalking or other partner-focused obsessional behaviour
-
• Bizarre forms of violence such as sadistic violence
-
1 Ask patients about relationship violence. They may prefer to discuss ‘aggression’ in their relationships, because of the stigma associated with the words violence or domestic violence and the fear that they or their partner may be reported to the police. Patients may prefer to differentiate between psychological, sexual and physical aggression. Patients are more likely to report violence on a questionnaire than during direct questioning.
-
2 If intimate partner violence is present, determine its severity and ask about fear of partner. Provide safety planning. The American Medical Woman's Association maintains a CPD programme on its website that provides a basic understanding of domestic violence (the Domestic Violence Health Care Provider Education Project at https://secure.amwa-doc.org/index.cfm?objectId=72F327C5-D567-0B25-52A723F34B87FFCD).
-
3 Identify risk factors (Box 7) that indicate a potentially lethal relationship that would preclude couples treatment (Reference Bogard and MederosBogard & Mederos, 1999).
-
4 If substance misuse is present, recommend abstinence and if possible refer for treatment, for example to Alcoholics Anonymous.
-
5 Ask the couple whether they wish to stay together and want to resolve the violence. If so, conjoint treatment can be recommended. The key components to conjoint treatment are the signing of a no violence contract, the use of negotiated time-out and strategies to manage anger. A family therapist specialising in managing intimate partner violence should provide this treatment.
-
6 Treatment of psychiatric comorbidity is important and both partners should be assessed for depressive disorder and post-traumatic stress disorder.
-
7 If the perpetrator is subject to court-ordered treatment, then the treatment programme must meet court approval. In this case, gender-specific group treatment is the most likely treatment available. Women who have been arrested for perpetration of intimate partner violence may not have access to appropriate treatment (Reference Finn and BettisFinn & Bettis, 2006).
Research into the aetiology and treatment of intimate partner violence is in its infancy because society has traditionally sought a legal solution to the problem, by punishing the perpetrator and rescuing the victim. As discussed above, intimate partner violence is commonly bidirectional and a legal solution will not help in such cases. Using couples therapy with couples who wish to stay together has been considered ‘off limits’ for many years because of fears that are often unfounded. Couples that themselves seek treatment to reduce intimate partner violence have different treatment needs compared with couples that enter treatment by court referral. Self-referred couples may be interested in improving many aspects of their relationship, are more motivated and have been able to identify a problem and seek out a solution.
The guidelines offered in this article provide steps for assessment (Box 8) and recommendations for treatment of couples that present to the clinician with intimate partner violence.
Box 8 Guidelines for assessing intimate partner violence
-
• Ask about relationship violence. Consider use of questionnaire
-
• If present, determine severity and ask about fear of partner
-
• Identify risk factors for potentially lethal relationship
-
• If substance misuse present, recommend abstinence and refer for treatment
-
• If the couple wishes to stay together and to resolve the intimate partner violence refer for conjoint treatment with a specialised family therapist
-
• Assess and treat common comorbidities: depressive disorder and post-traumatic stress disorder
Declaration of interest
None.
MCQs
-
1 Intimate partner violence:
-
a is frequently bidirectional
-
b is openly acknowledged by victims
-
c is always assessed in healthcare settings
-
d is not associated with alcohol misuse
-
e usually results in incarceration.
-
-
2 Court-ordered treatment of male perpetrators usually takes the form of:
-
a gender-specific group treatment
-
b community service
-
c individual psychotherapy
-
d jail sentence
-
e couples therapy.
-
-
3 Risk factors indicating a lethal relationship include:
-
a stalking or sadistic behaviour
-
b alcohol misuse
-
c fear or history of serious injury
-
d violation of previous restraining order
-
e all of the above.
-
-
4 Randomised controlled trials of intimate partner violence treatment have found that:
-
a gender-specific treatment is the most effective intervention for male perpetrators
-
b assessing and offering a referral for victims is effective
-
c couples therapy is always contraindicated
-
d psychiatric comorbidity is not relevant
-
e intimate partner violence cannot be treated.
-
-
5 The following are ineffective in couples therapy:
-
a a no violence contract
-
b anger management strategies
-
c communication skills training
-
d acceptance of responsibility for violence
-
e encouragement of expression of anger.
-
MCQ answers
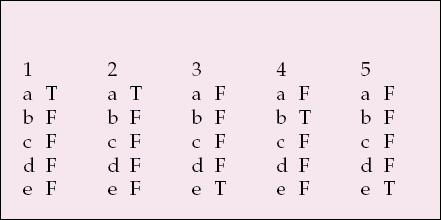
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | T | a | F | a | F | a | F |
| b | F | b | F | b | F | b | T | b | F |
| c | F | c | F | c | F | c | F | c | F |
| d | F | d | F | d | F | d | F | d | F |
| e | F | e | F | e | T | e | F | e | T |



eLetters
No eLetters have been published for this article.