No CrossRef data available.
Article contents
Carbapenemase genes and mortality in patients with carbapenem-resistant Enterobacterales, Atlanta, Georgia, 2011–2020
Published online by Cambridge University Press: 29 September 2023
Abstract
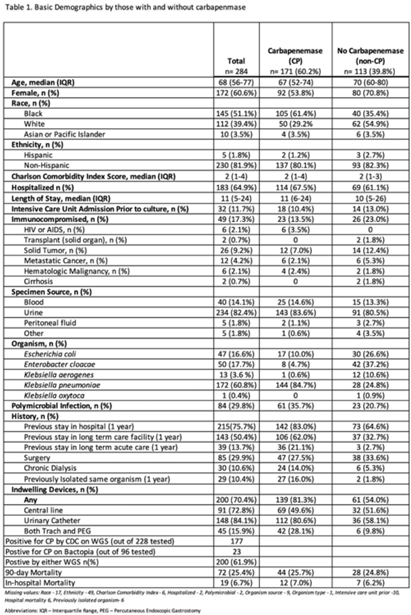
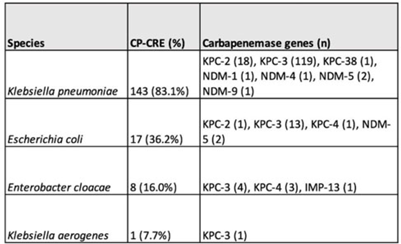
Background: Carbapenemase genes in carbapenem-resistant Enterobacterales (CP-CRE) may be transmitted between patients and bacteria. Reported rates of carbapenemase genes vary widely, and it is unclear whether having a carbapenemase gene portends worse outcomes given that all patients with CRE infections have limited treatment options. Methods: Using active population- and laboratory-based active surveillance data collected by the US CDC-funded Georgia Emerging Infections Program from 2011 to 2020, we assessed the frequency of carbapenemase genes in a convenience sample of CRE isolates using whole-genome sequencing (WGS), and we investigated risk factors for carbapenemase positivity. Only the first isolate per patient in a 30-day period was included. We compared characteristics of patients with CP-CRE and non–CP-CRE. Using multivariable log binomial regression, we assessed the association of carbapenemase gene positivity and 90-day mortality. Results: Of 284 CRE isolates, 171 isolates (60.2%) possessed a carbapenemase gene (Table 1), and KPC-3 was the most common carbapenemase gene (80.7%), with only 7 isolates possessing NDM (Table 2). No isolates possessed >1 carbapenemase gene, and most isolates were from urine (82.4%) (Table 1). Carbapenemase gene positivity was associated with lower age, male sex, black race, infection with Klebsiella pneumoniae, polymicrobial infection, having an indwelling medical device, receiving chronic dialysis, and prior stay in a long-term acute-care hospital, long-term care facility, and/or prior hospitalization in the last year. The 90-day mortality rates were similar in patients with non–CP-CRE and CP-CRE: 24.8% versus 25.7% (P = .86). In multivariable analysis, carbapenemase gene presence was not associated with 90-day mortality (adjusted risk ratio, 0.82; 95% CI, 0.50–1.35) when adjusting for CCI, infection with Klebsiella pneumoniae, and chronic dialysis use. Conclusions: The frequency of CP-CRE among CRE was high in this study, but unlike prior studies, the 90-day mortality rates wer similar in patients with CP-CRE compared to non–CP-CRE. Our results provide novel associations (eg, lower age, male sex, infection with Klebsiella pneumoniae, and indwelling medical devices) that infection preventionists could use to target high-risk patients for screening or isolation prior to CP-CRE detection.
Disclosure: None
- Type
- MDR GNR
- Information
- Antimicrobial Stewardship & Healthcare Epidemiology , Volume 3 , Issue S2: SHEA Spring 2023 Abstracts , June 2023 , pp. s12 - s13
- Creative Commons
- This is an Open Access article, distributed under the terms of the Creative Commons Attribution licence (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted re-use, distribution, and reproduction in any medium, provided the original work is properly cited.
- Copyright
- © The Author(s), 2023. Published by Cambridge University Press on behalf of The Society for Healthcare Epidemiology of America


