Introduction
The Canadian Association of Emergency Physicians (CAEP) recently published their third position statement in 20 years expressing concern over emergency department (ED) crowding.Reference Affleck, Parks and Drummond 1 In 2012, Canada was rated worst among 11 developed countries for patients waiting longer than four hours to be seen in the ED. 2 A recent international survey found more Canadians wait longer than six days to see their family doctor than in any of the aforementioned countries,Reference Schoen, Osborn and Squires 3 a situation that likely contributes to ED crowding.
One approach to decrease ED crowding is a fast track (FT).Reference Yoon 4 The concept is based on the “lean thinking theory,”Reference King, Ben-Tovim and Bassham 5 , Reference Dickson, Anguelov and Vetterick 6 and involves implementation of a separate patient stream where low-acuity and low-complexity patients are treated in a defined area.Reference Ieraci, Digiusto and Sonntag 7 Often this involves dedicated beds or chairs and a separate waiting room. Previous studies have shown that FTs can decrease wait times, length of stay (LOS), and crowding in tertiary care centers.Reference Yoon 4 , Reference Ieraci, Digiusto and Sonntag 7 - Reference Devkaran, Parsons and Van Dyke 9 There is also evidence indicating that FTs do not negatively impact higher-acuity patients.Reference Darrab, Fan and Fernandes 10 - Reference Kwa and Blake 13 However, there have been few studies to evaluate FTs in Canadian settings. Moreover, many FT studies are potentially confounded by simultaneous increases in either total physician and nursing hours or ED beds. More staff or space has a financial cost that may not be feasible depending on the setting involved. As a result, there is a paucity of strong evidence for or against FT implementation in community hospitals.Reference Affleck, Parks and Drummond 1 This study was designed to determine if FTs are an effective strategy to reduce wait times in a single physician coverage ED. Our hypothesis was that patient throughput after FT implementation would improve for low-acuity patients (Canadian Triage and Acuity Scale [CTAS] 4-5), without negatively impacting the care of higher-acuity patients (CTAS 2-3).
Methods
Design and setting
A retrospective cohort study of patients presenting to Strathroy Middlesex General Hospital (SMGH) in the year before and after implementation of a FT was undertaken. SMGH is a 54-bed community-based teaching hospital in southwestern Ontario, and serves a population of approximately 35,000 people. The hospital has a census of approximately 25,000 emergency visits per year, 24% of which are pediatric (<18 years), and is categorized as a medium-volume hospital according to the Ontario Ministry of Health and Long-Term Care. 14
The ED of SMGH is staffed predominately by a single family physicians. Physicians work shifts of 0700-1500 hrs, 1400-2200 hrs, and 2100-0700 hrs, resulting in two hours of overlapping coverage during handover and a total of 26 physician work hours per day. Nursing shifts from 0700-1900 hrs and 1900-0700 hrs are staffed by three nurses, while one additional nurse provides coverage during peak hours of 1100-2300 hrs, for a total of 84 nurse work hours per day.
Intervention
A fast track (FT) was launched at SMGH in June 2010, consisting of a reallocation of existing resources; there was no physical space or equipment added. There were 14 assessment areas before the intervention, and one additional room after restructuring, comprised of a room that was previously used for other needs, which was converted into the new chair-only assessment area. There were no additional nursing or physician hours after the intervention; one of the usual three to four nurses on staff was repatriated to FT during hours of operation, and provided care only to these patients.
From 2100-0900 hrs there were no department changes; patient flow proceeded as it had before, with the exception of the additional chair room mentioned earlier. From 0900-2100 hrs, FT was considered “open.” During this time, five of 15 assessment areas that were previously part of the acute area became dedicated to FT, including the new chair room. All FT rooms were physically adjacent to one another and separate from patients in acute care beds, effectively creating a physical area in the department comprised only of FT patients called “Green Zone” (Figure 1). Our FT included a number of chairs in the hallway outside FT rooms to function as a waiting area for patients in that zone.

Figure 1 Emergency Department layout showing Fast Track (Green Zone) area. SMGH–Strathroy Middlesex General Hospital
The intervention under study was a change in patient flow in the ED and its effect on throughput. Upon presentation, patients were triaged either to regular acute beds or the FT. Experienced triage nurses were provided additional training on selecting patients for the FT based on the complexity of patient complaints, and applying the lean thinking theory in a manner consistent with previous studies.Reference Dickson, Anguelov and Vetterick 6 , Reference Ieraci, Digiusto and Sonntag 7 FT patients were generally ambulatory, CTAS 4-5, and had straightforward presenting complaints deemed by the triage nurse to likely require few investigations and a disposition of discharge home. CTAS 1-2 patients were excluded from the FT. Physicians were expected to flow between the acute area and the FT, following some general rules. First, high-acuity patients were assessed in the acute area, in keeping with national CTAS time guidelines. 15 Once nurses had queued a number of FT patients into rooms waiting to be seen, the physician would go down the hallway to the FT area to assess and treat a number these patients sequentially. Generally, these patients had lower CTAS scores than others still waiting to be seen in the acute area, and often they had been waiting for less time. Following this, the physician would return to the acute area to manage high-acuity patients until the cycle was repeated.
Time period
Study periods chosen to represent before and after the intervention ended and started approximately six months from the intervention date. This time gap was utilized in part to allow each group to fall into only one calendar year, but also to provide a wash-out period surrounding the intervention date. Matched one-year study periods were chosen to control for the effects of seasonal variation and any imbalance between study groups that could arise from this, for example from higher patient volumes in the winter. To be sure that study groups were matched for time and evenly distributed throughout the year, the first seven days of all 12 months were included in each group, for a resulting total of 84 days in both the before and after periods. We chose this representative sample of each time period to avoid an overwhelming sample size and the resulting increased workload that would be required for data analysis. The before intervention group included patients from the days in 2009 mentioned earlier; the after intervention group included those in 2011.
Inclusion and exclusion criteria
Patients of all CTAS levels triaged at SMGH ED during FT hours of operation (9 a.m. to 9 p.m.) during the time periods of the study were eligible for enrollment. Patients were excluded if they had incomplete or incorrect charts, defined as any of the following: 1) disposition coded as assessed by physician with no assessment time noted; 2) disposition coded as not assessed by a physician, but an assessment time was recorded in error; 3) assessment time earlier than triage time, causing a negative wait time; 4) missing demographic information such as age or gender.
Outcome measures and calculations
The two primary outcomes for patient throughput were wait time (WT) and length of stay (LOS). Secondary outcomes were the proportion of WTs that met national CTAS time guidelines (MNCTG) and the proportion of patients that left without being seen (LWBS). In 1998, CAEP published national hospital WT standards, advising that each ED patient be assessed by a physician according to their CTAS. 15 These guidelines deem that CTAS 1 patients should be assessed immediately by the physician, CTAS 2 within 15 minutes, and CTAS 3, 4, and 5 within 30, 60, and 120 minutes, respectively. We deemed a priori that a clinically significant change in WT is one with an impact significant enough to have more patients be seen within the national CTAS time guidelines. Our other secondary outcome, LWBS, has been proposed in previous studies to be a marker of crowding.Reference Darrab, Fan and Fernandes 10 , Reference Fernandes, Price and Christenson 16
Data collection
The hospital electronic medical record system was utilized to create a database of visits during the study periods that included the following information: hospital identification number, age, gender, CTAS level, date and time triaged, date and time of first physician assessment, date and time of disposition, disposition code, and discharge diagnosis code.
FT status was not included on the hospital electronic medical record system, so a random number generator was used to select three days included in our “after” study period, for which all charts were reviewed to calculate the average patient flow through the FT. A total of 149 charts were reviewed by the primary researcher, and the following information was recorded: date of visit, CTAS level, and whether patient was seen in the FT or acute area.
Statistical analysis
Continuous variables (WT and LOS) were first tested for normality of distribution using the Kolmogorov-Smirnov test. Outcome measures were compared between groups using the Mann-Whitney U-test for non-normally distributed continuous variables, or Student t-test for normally distribution continuous variables. Nominal variables (MNCTG and LWBS) were compared between groups using the chi-square test, or Fisher exact test in the case of infrequent occurrences (<10). Descriptive statistics were reported for non-parametric continuous variables as median with interquartile range (IQR), and for parametric continuous variables as mean with standard deviation (SD). Nominal variables were reported as frequencies with percentage. All tests were considered significant at p value<0.05. Statistical analysis was done using SPSS Statistics (IBM, Version 21).
Subgroup analysis
Analyses of outcome measures were repeated within four a priori subgroups. Each subgroup consisted of the same patients as above, categorized by CTAS levels 2 through 5. The purpose of subgroup analysis was to determine, if an overall improvement in outcome measures was achieved across all CTAS levels, whether this significantly impacted any outcome measures within any individual levels. CTAS 1 cases were not included, as it was assumed implementation of a FT should have no impact on these cases, since they are seen immediately.
Ethics
The study was approved by both the University of Western Ontario Research Ethics Board for Health Sciences Research Involving Human Subjects, and the Strathroy Middlesex General Hospital Research Committee.
Results
A total of 7,432 ED visits met inclusion criteria; 3,670 before and 3,762 after, with 95 and 33 charts being excluded in each time period respectively. Demographic characteristics of the study participants in the before and after groups were similar (Table 1). A similar distribution of the most frequent problems between the two groups was also seen (Table 2).
Table 1 Demographic characteristics of the study participants.
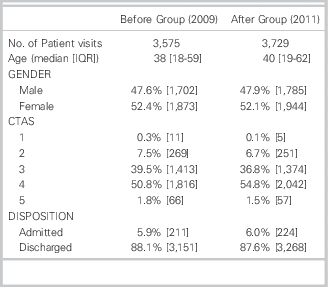
IQR: interquartile range
CTAS: Canadian Triage and Acuity Scale
Table 2 Top 10 most common coded disposition diagnoses for the study groups.
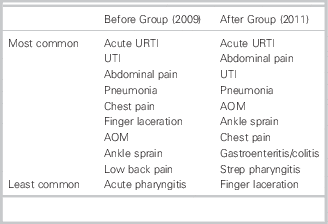
URTI: upper respiratory tract infection
UTI: urinary tract infection
AOM: acute otitis media
The chart review indicated that 43% (64 of 149) of patients flowed through the FT during its hours of operation. Of those, 84% (54 of 64) were CTAS 4, a much higher proportion than seen in the acute area.
Table 3 shows the primary and secondary outcomes for the study groups. The median WT decreased by six minutes after implementation of a FT (p=0.002). The median LOS decreased by 15 minutes (p<0.001) after implementation of a FT, and there was an absolute improvement of 3.6% in MNCTG (p<0.001). No difference was found in LWBS proportions before and after the intervention (4.6% to 4.4%, respectively; p=0.738).
Table 3 Primary and secondary outcomes in the study groups.
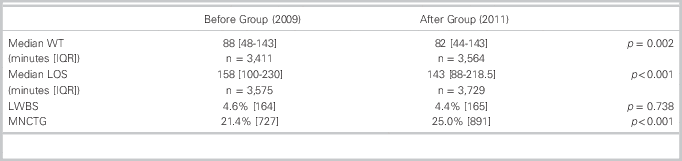
WT: wait time
LOS: length of stay
MNCTG: met national CTAS (Canadian Triage and Acuity Scale) time guidelines
LWBS: left without being seen
IQR: interquartile range
CTAS subgroup analysis indicated that only CTAS 4 patients had a significant change after the intervention. Higher levels (CTAS 2-3) were not negatively impacted for any of the primary or secondary study outcomes. Table 4 shows primary and secondary outcomes, categorized by CTAS level, for the study groups. The result trends of the CTAS 4 subgroup analysis matched those for the entire population, with the difference that the changes were more dramatic: WT decreased by 13 minutes (p<0.001) and LOS by 22 minutes (p<0.001) in the CTAS 4 group, while the MNCTG increased by 5.3% (p=0.001).
Table 4 Primary and secondary outcomes, categorized by CTAS level, for the study groups.

WT: wait time
LOS: length of stay
MNCTG: met national CTAS (Canadian Triage and Acuity Scale) time guidelines
LWBS: left without being seen
IQR: interquartile range
*statistically significant at p≤0.05 threshold
Discussion
Our results suggest that the addition of a FT can improve ED crowding by significantly decreasing WT and LOS, a finding consistent with similar studies in tertiary care settings.Reference Sanchez, Smally and Grant 8 - Reference Darrab, Fan and Fernandes 10 However, our study results suggests two important features that previous work has not investigated: 1) increased throughput can be accomplished even in a single physician ED; and 2) increased throughput can be accomplished even when no additional staff are added in the restructuring process. The FT restructuring at our study location involved little change in resources and no additional physical space, but rather simply a change in patient and staff flow. Although the intervention was only found to result in statistically significant changes for CTAS 4 patients on subgroup analysis, it merits consideration that CTAS 4 makes up over 50% of our ED visits, a proportion similar to other low-acuity community EDs across the country. Moreover, the improvements we found in ED metrics occurred in spite of an overall increase in volume of 1.7% (from 22,950 visits in 2009, to 23,335 in 2011).
The ability to improve throughput with no additional resources may be explained in part by improved physician efficiency. Rather than traveling in an unstructured manner throughout the ED based on a global queue, physicians managed batches of patients in the FT, ordered labs and imaging simultaneously on those patients, and returned later only when a number of patients could be reassessed, thus reducing travel time from one end of the department to the other. This is consistent with the lean thinking theory, which suggests it is inherently more efficient to serve batches of quick customers to reduce crowding.Reference King, Ben-Tovim and Bassham 5 , Reference Dickson, Anguelov and Vetterick 6
We did not find a decrease in number of patients LWBS after the intervention, a finding in contrast to other studies,Reference Affleck, Parks and Drummond 1 , Reference Ieraci, Digiusto and Sonntag 7 - Reference O’Brien, Williams and Blondell 11 , Reference Fernandes, Price and Christenson 16 even in subgroup analysis where the WT decrease was most dramatic. Thus an important question remains: does a decrease in WT of between six and 13 minutes result in a change in crowding that patients notice or deem to be significant? Previous studies have suggested that improvement in LWBS is related to patient satisfaction.Reference Affleck, Parks and Drummond 1 , Reference Darrab, Fan and Fernandes 10 , Reference Fernandes, Price and Christenson 16 , Reference Fernandes, Daya and Barry 17 It is possible that our study failed to show a clinically significant change for this metric due to an already low proportion of patients that LWBS at our hospital before the intervention (<5%). In addition, LWBS may not be the only indicator of patient satisfaction; two prior studies have indicated that the most important factor determining satisfaction is decreasing WT.Reference Dinh, Enright and Walker 18 , Reference Bursch, Beezy and Shaw 19 While we cannot come to a definitive conclusion about patient satisfaction, we believe that the decrease found in WT in our study is still clinically relevant, since it was associated with an improvement in meeting the national CTAS time guidelines. This relevance was underscored by a recent CAEP position statement suggesting that implementing and improving national WT benchmarks is an essential component of initiatives to improve ED crowding.Reference Affleck, Parks and Drummond 1 It is noteworthy that the increase in MNCTG we found for CTAS 4 patients (5.3%), and the obvious trending increase for CTAS 5 patients (10.9%), occurred without CTAS 2-3 patients suffering any detrimental effects, as measured by any of our primary or secondary outcomes. The significant improvement in MNCTG may be of particular importance to hospital administrators seeking to improve benchmark performance.
Limitations
Several limitations should be considered when interpreting our results. Our study was limited by the fact that it was a single-center retrospective observational study. Data collection was not blinded; however, the observers who recorded the original chart data were not aware of this study at that time. Our design relied upon accurate observations and transcriptions, and thus is subject to human error. We believed any small positive or negative errors in recording or transcribing times would balance out across our sample, and made efforts to remove gross errors through our exclusion criteria. Although no a priori calculation was done, we feel the study sample size of over 7,000 provided sufficient power for a study of this nature. It could be argued, however, that another limitation is that we only included a representative sample of each study period rather than every day of the year. Finally, patient-oriented health outcomes, in particular morbidity or mortality, were not evaluated; however, previous studies with a similar design have found no impact on either of these.Reference Sanchez, Smally and Grant 8 , Reference Devkaran, Parsons and Van Dyke 9
One possible confounder to consider is that family medicine resident work hours increased by approximately three hours per day from the before to the after period (nine hours per day before and 12 hours per day after FT implementation). This was not related to FT restructuring. It is possible that this increase could account for some the decrease in WT. However, the increase in coverage is rather small (<3% increase of total daily staff hours), so we feel that any effect from this would likely be minor. It should also be considered that, in contrast to attending staff, increase in resident hours leads to increased clinical teaching time, which may in fact increase WT.
An additional possible confounder to consider is that the addition of one assessment area (chair-only room) after the intervention may have accounted for some of the decrease in WT we observed. Unlike some tertiary care hospitals, we designed this study based on the assumption that the WT bottleneck in smaller community hospitals lies with the physician rather than the number of beds available, especially in a single physician department. Regardless, the impact of this one-chair increase was rather small, from 14 to 15 assessment areas (an increase of approximately 7%).
Conclusions
Implementation of a fast track in a medium-volume community hospital with single physician coverage can improve patient throughput by decreasing WT and LOS without negatively impacting high-acuity patients. Our results illustrate that this can be accomplished without an increase in physician or nursing hours, and with minimal change in ED space and resources. It is uncertain whether patients notice the decrease in crowding, but the increased throughput may be particularly relevant for hospital administrators wishing to improve benchmark standards.
Competing Interests: None to declare.







