CLINICIAN'S CAPSULE
What is known about the topic?
There is an organ donor shortage. End-of-life care discussions occur in the emergency department (ED), therefore there may be opportunities for donation.
What did this study ask?
What percentage of successful and missed adult organ donors come from the ED?
What did this study find?
This systematic review found that the ED is a significant source of both successful and missed organ donors.
Why does this study matter to clinicians?
ED healthcare providers should know their local organ donation referral protocol to ensure that donors are not missed.
INTRODUCTION
There is a significant gap between the number of people waiting for an organ and organ donors. In 2018, in Ontario, there were 1,639 people awaiting organ donation, 456 decreased donors, and 947 organs transplanted from deceased donors.1 In BC, in 2018, there were 669 people on the transplant wait list, and 27 people died while on the wait list.2 Although progress has been made in organ donation in Canada, a significant gap between organ donors and people awaiting organ transplantation still exists; therefore, further efforts are required to ensure that all potential organ donors are identified.
Many end-of-life care discussions occur in the ED.Reference Witjes, Kotsopoulos and Herold3 Witjes et al. (2017) found that, in 51% of the time, the decision to start end-of-life care was made in the ED.Reference Witjes, Kotsopoulos and Herold3 One study suggested that 60.5% of family interviews for potential brain dead donors occurred in the ED.Reference Fernandes-Carmona, Sevilla-Martinez and Pérez-Villares4 Another study showed that of all successful organ donors, 6/14 (27.3%) had the organ donor discussion initiated in the ED.Reference Tenn-Lyn, Doig and Shemie5 Furthermore, two studies have shown that patients referred from the ED are more likely to become successful donors than those referred from elsewhere in the hospital.Reference Miller, Gardiner and Gubler6,Reference Michael and O'Connor7 These studies highlight the role the ED has in ensuring that potential donors are not missed.
Previous systematic reviews have investigated organ donation from the intensive care unit (ICU) exclusively, or pooled organ donation from the ED and ICU together.Reference Cameron, Erdogan and Lanteigne8–Reference Van Erp, van Dullemen, Ploeg and Leuvenink10 There may be ED-specific factors that could impact organ donation. The purpose of this study is to determine what percent of successful donors come from the ED, whether there are any missed or potential donors, and what factors impact organ donation in the ED.
METHODS
Data sources and search strategy
We conducted this systematic review according to preferred reporting items for systematic reviews and meta-analyses (PRISMA) guidelines.Reference Halpern, Hasz and Abt11,Reference Moher, Liberati, Tetzlaff and Altman12 A medical librarian performed electronic searches of EMBASE, MEDLINE, and CINAHL on July 7, 2017. Duplicates were electronically removed during the search. Additional duplicates were removed manually during screening.
Our search strategy used Medical Subject Headings (MeSH) terms and free words in the title and abstract by combining terms in two categories. One category included terms related to organ donation such as “tissue and organ procurement,” “donor* or donat*,” “non-heart-beating,” and “brain death.” The other category was related to the types of injuries or terms related to emergency medicine. Terms included “wounds and injuries,” “trauma,” “brain hemorrhage,” “gunshot wound,” “ED or emergency room or emergency service or emergency medicine or emergency care or emergency hospital.” The full search strategy can be found in Appendix I.
Studies were included if they met the following criteria (Figure 1). Primary literature on adult (age ≥ 18 years) humans was included if they investigated organ donation and reported either number of actual donors, missed donors, or potential donors. Papers were excluded if they were case reports, not organ donation, outcomes not reported (technique for organ removal, organ donor criteria, factors affecting organ viability, determination of death, recipient-specific data, survey of attitudes, curriculum to increase donation, process of consent), not solid organ donation (living donor, forensic donation), tissue donor (skin, bone marrow, cornea, blood, stem cell, science, sperm), and ethical considerations. For the title and abstract screen, all papers reporting either number of actual, missed, or potential organ donors were included, regardless of the location in the hospital. The full paper was then screened for ED-specific data. If it was unclear whether data reported was ED-specific, authors were contacted to confirm whether there were ED-specific data. If there were no ED-specific data, the paper was excluded according to “ED data not reported.” The full text papers were also screened for data such that a percentage could be calculated. If papers only reported number of organ donors in the ED without reporting total number of actual or potential donors, the paper was excluded as “outcomes not reported.” The reference list of all included papers was reviewed for additional papers.
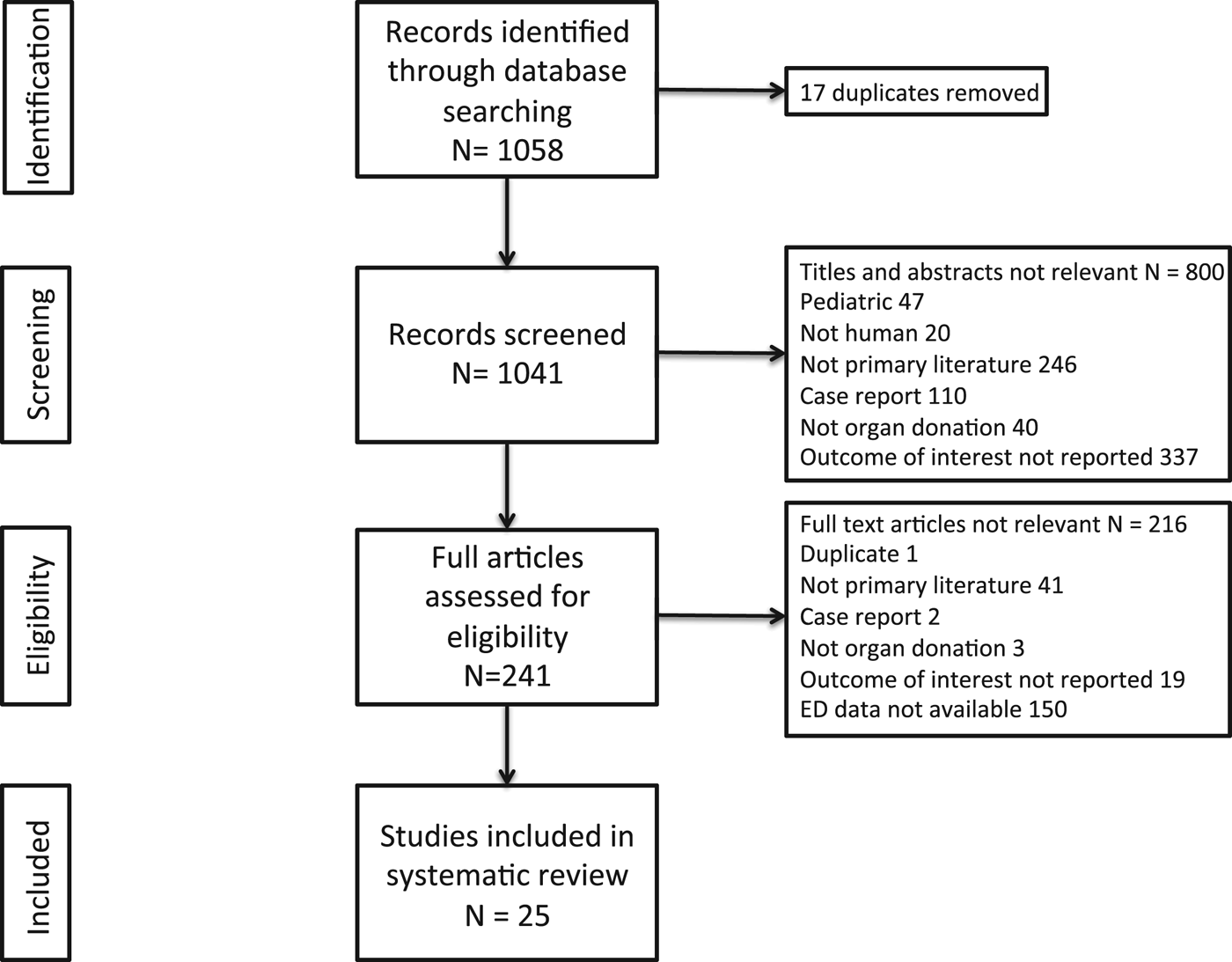
Figure 1. PRISMA flow diagram.
Two reviewers (JM, BE) independently screened papers for inclusion according to the criteria outlined previously, using Microsoft Excel©. Discrepancies were resolved by consensus.
Data abstraction and quality assessment
Data were abstracted from papers into an Excel database. If data were missing, authors were contacted. Data were abstracted for study design, population, and outcomes. Outcomes included percentage of successful organ donors coming from the ED and percentage of missed or potential donors in the ED (Tables 1–5). Papers were separated by neurologic determination of death and donation after circulatory determination of death. Donors were separated into these two populations, because screening criteria are different. In neurologic determination of death, the patient is declared as brain dead and in donation after circulatory determination of death the heart and blood circulation stop.Reference Thuong, Ruiz and Evrard13 In controlled donation after circulatory determination of death, circulatory death occurs in an expected setting, often after withdrawal of life support, whereas in uncontrolled donation after circulatory determination of death, death occurs in the out-of-hospital setting or after an unsuccessful resuscitation.Reference Thuong, Ruiz and Evrard13
Studies were assessed for quality using the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist,Reference Elm von, Altman and Egger14 and missing elements are highlighted in Tables 1–4.
Data synthesis and analysis
There was significant clinical heterogeneity between included papers regarding organ donor population. Heterogeneity existed regarding study design (prospective, retrospective, and convenience sample) and patient population (hospital-wide v. ED, trauma v. all-comers). Similarly, the majority of the studies did not specify organ donor exclusion and inclusion criteria. This precluded pooling of the studies to perform a meta-analysis. Descriptive data from individual studies are shown in Tables 1–5.
For the purpose of this systematic review, the definition of ED donor varies depending on the study design. In studies of successful organ donation, an ED donor is a donor that was referred to an organ procurement organization from the ED or had brain death declared in the ED. For the death reviews of missed and potential donors, an ED donor is a patient who died in the ED.
RESULTS
Search results
Our search results yielded 1,058 studies (see Figure 1). An additional 17 duplicates were removed, yielding 1,041 individual titles and abstracts to screen. Articles totalling 800 were excluded based on title and abstract, yielding 241 full articles to assess for eligibility. Full-text articles totalling 216 were excluded, yielding 25 articles that were included in the systematic review.
Neurologic determination of death
There were seven papers that reported successful organ donation from ED patients after neurologic determination of death.Reference Witjes, Kotsopoulos and Herold3,Reference Tenn-Lyn, Doig and Shemie5−7,Reference Summers, Johnson and Hudson15–Reference Henderson, Chao and Green17 In these studies, patients were referred for consideration of organ donation while they were in the ED. All seven studies mentioned the role of the ED in referring donors to an organ procurement organization or involvement of an organ donation coordinator to facilitate donation. Taken together, these seven studies suggest that the 4%–50% of successful organ donors come from the ED. A summary of successful neurologic determination of death papers can be found in Table 1.
Table 1. Summary of papers for successful neurologic determination of death donors
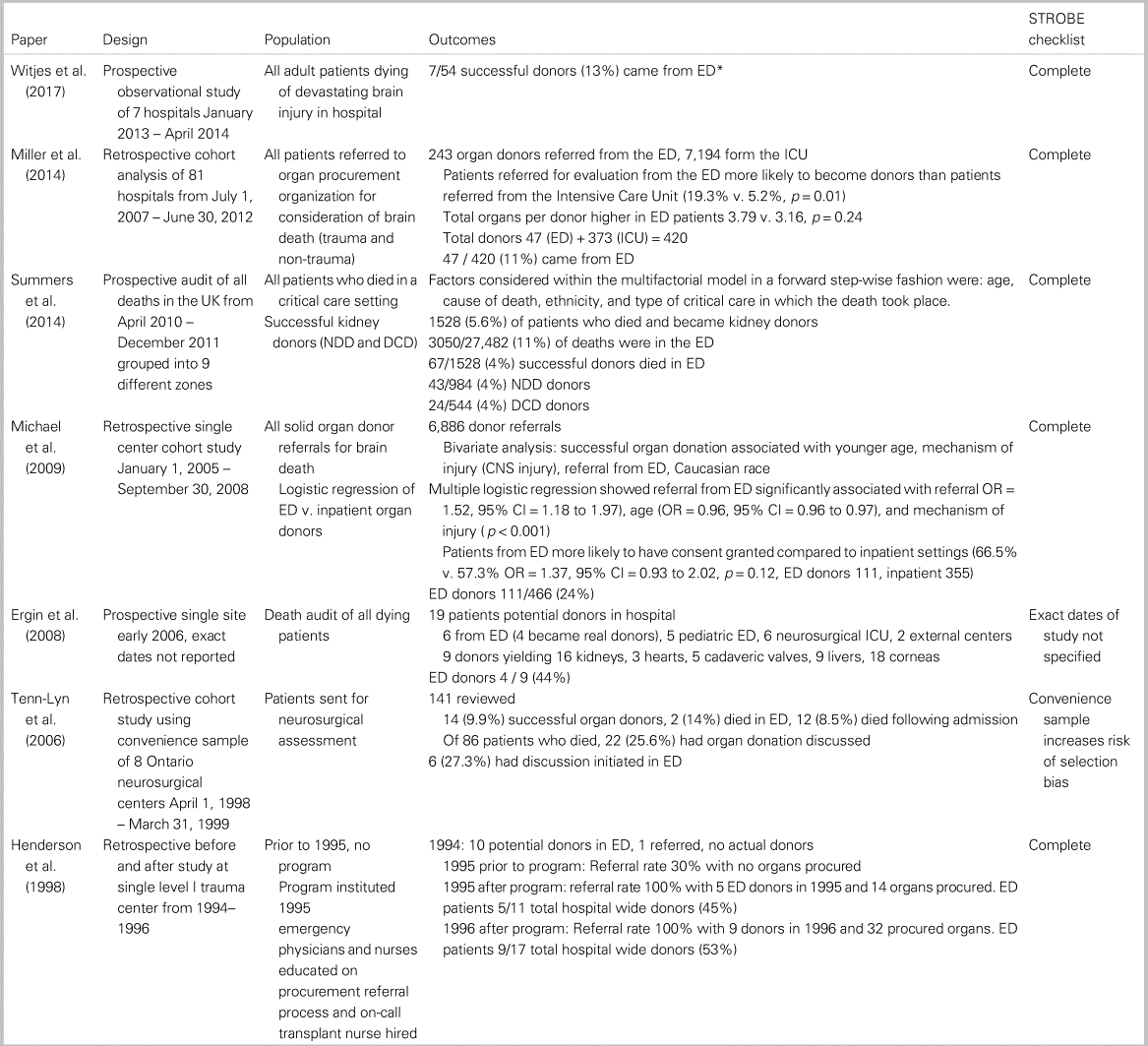
DCD = Donation after circulatory determination of death; ED = emergency department; NDD = donation after brain death.
*Emergency department data were obtained through correspondence with author.
There were five death reviews that investigated actual missed organ donors who died in the ED that were missed as a result of a failure to refer for consideration of organ donation.Reference Witjes, Kotsopoulos and Herold3,Reference Dell Agnolo, de Freitas and Toffolo18–Reference Riker and White21 Two of these studies determined that of all actual missed donors in the hospital, 13%–80.9% died in the ED.Reference Witjes, Kotsopoulos and Herold3,Reference Dell Agnolo, de Freitas and Toffolo18 One study found that 84% of donors dying in the ED were missed.Reference Garside, Garside, Fletcher and Finlayson19 Two studies found that 0%–2% of brain dead patients dying in the ED are missed. In all cases, these donors were missed due to a failure to refer. A summary of these papers can be found in Table 2.
Table 2. Summary of papers for missed and potential neurologic determination of death donors

DCD = Donation after circulatory determination of death; ED = emergency department; NDD = donation after brain death.
*Emergency department data were obtained through correspondence with author.
There were four death reviews that screened for potential organ donors using pre-specified organ donor criteria; however, the criteria varied between studies or was not specified in the paper.Reference Kim, Kim and Jang22–Reference Aubrey, Arber and Tyler25 Two studies found that 8%–86% of hospital-wide potential donors die in the ED.Reference Kim, Kim and Jang22,Reference Andrés, Sánchez Casado and Cebrián23 Two studies found that 2%–7.2% of patients who die in the ED could be potential donors.Reference Le Conte, Riochet and Labastire24,Reference Aubrey, Arber and Tyler25 A summary of these papers can be found in Table 2.
One study investigated all spontaneous intracerebral hemorrhage patients to determine how many potential donors were not approached due to not being ventilated.Reference Andrés, Sánchez Casado and Cebrián23 They found that 12/15 (86%) of these patients died in the ED.Reference Andrés, Sánchez Casado and Cebrián23 The authors of this study highlighted the ethical considerations in ventilating a person exclusively for organ donation.
Donation after circulatory determination of death
There were six studies that described successful donation after circulatory determination of death.Reference Alarhayem, Cohn and Muir26 All six studies involved an organ procurement organization or coordinator in the donation process. Three studies investigated patients with traumatic cardiopulmonary arrest who achieved return of spontaneous circulation and went on to become organ donors. Alarhyem et al. found that 12/333 (3.6%) donated 24 major organs.Reference Alarhayem, Cohn and Muir26 Love et al. (2016) found that 5/237 (2%) patients donated 16 major organs.Reference Love, Brown and Harbrecht27 Raoof et al. (2011) found that 19/213 (8.9%) donated 26 major organs.Reference Raoof, Joseph and Friese28 Taken together, 3.6%–8.9% of traumatic cardiopulmonary arrest patients dying in the ED become successful organ donors. Two studies reviewed successful kidney donation specifically. Summers et al. (2014) found that 67/1528 (4%) of successful donors (neurologic determination of death and donation after circulatory determination of death) died in the ED and 24/544 (4%) of the donation after circulatory determination of death donors came from the ED.Reference Summers, Johnson and Hudson15 Another study found that 8/41 kidneys came from patients dying in the ED, with 2/41 (4.9%) successfully transplanted.Reference Gerstenkorn29 These studies suggest that 4%–4.9% of successful donations after circulatory determination of death kidney donors come from the ED. One study investigated the use of in-ED cannulation for uncontrolled donation after circulatory determination of death. There were 18 potential candidates, and four organs were recovered (three kidneys and one liver). There were no organs transplanted due to prolonged warm time, but, as technology advances, this could improve in the future.Reference DeVita, Callaway and Pacella30 A summary of successful donation after circulatory determination of death donors can be found in Table 3.
Table 3. Summary of papers for successful donation after circulatory determination of death donors
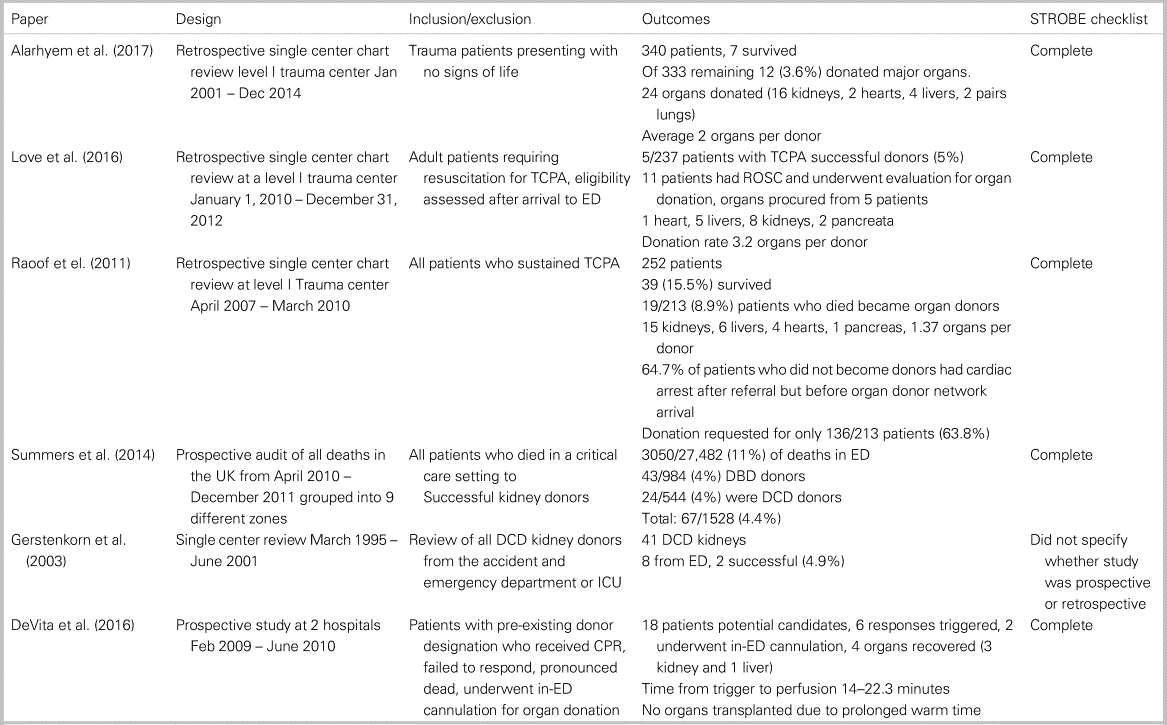
DCD = Donation after circulatory determination of death; ED = emergency department; ICU = intensive care unit; NDD = neurologic determination of death; TCPA = traumatic cardiopulmonary arrest.
There was one death review in traumatic cardiopulmonary arrest that investigated actual missed organ donors who died in the ED and were missed donors as a result of a failure to refer for consideration of organ donation.Reference Raoof, Joseph and Friese28 This study reported that 46.2% of traumatic cardiopulmonary arrest patients dying in the ED were not referred.
There were six death reviews that screened for potential donation after circulatory determination of death donors, using pre-specified criteria; however, the criteria varied between studies.Reference Halpern, Hasz and Abt11,Reference Aubrey, Arber and Tyler25,Reference Campbell and Sutherland31–Reference Blackstock, McKeown and Ray34 Three death reviews investigated potential controlled donation after circulatory determination of death donors hospital-wide and found that 2.3%–3.6% died in the ED.Reference Halpern, Hasz and Abt11,Reference Campbell and Sutherland31,Reference Daemen, Oomen, Kelders and Kootstra32 Similarly, two death reviews investigated potential uncontrolled donation after circulatory determination of death donors hospital-wide and found that 67%–75% died in the ED.Reference Campbell and Sutherland31,Reference Lacroix, Mahoney and Knoll33 Two death reviews investigated all patients dying in the ED and found that 0.3%–0.5% of them could be potential donors.Reference Aubrey, Arber and Tyler25,Reference Blackstock, McKeown and Ray34 A summary of missed and potential donation after circulatory determination of death donors can be found in Table 4.
Table 4. Summary of papers for missed and potential donation after circulatory determination of death donors

DCD = Donation after circulatory determination of death; ED = emergency department; ICU = intensive care unit; NDD = neurologic determination of death; ROSC = return of spontaneous circulation; TCPA = traumatic cardiopulmonary arrest.
Factors associated with successful and missed organ donation
Several studies investigated factors associated with successful organ donation (Tables 1–4). One study found that successful organ donation was associated with a referral from the ED instead of inpatient.Reference Michael and O'Connor7 There was also an insignificant trend towards ED referrals being more likely to have consent granted compared with inpatient settings.Reference Michael and O'Connor7 When compared with patients referred from the ICU, patients referred from the ED were more likely to become actual organ donors, and the total organs donated had a trend towards being higher.Reference Miller, Gardiner and Gubler6 Two studies investigated education programs, including an on-call transplant coordinator or nurse and found they increased organ donation.Reference Henderson, Chao and Green17,Reference Garside, Garside, Fletcher and Finlayson19 Three studies included in this review investigated specific reasons why potential organ donors are missed. One study found the main reasons that organ donation was not discussed were that the treating physician forgot (23/72), the incorrect assumption that the patient was too old (11/72), or the incorrect assumption that the patient was not suitable as an organ donor (7/72).Reference Witjes, Kotsopoulos and Herold3 Similarly, another study found that out of 19 charts with patients documented as “medically unsuitable” for organ donation, only 3 were actually medically unsuitable.Reference Riker and White21 Perceived barriers cited by healthcare staff included non-recognition as an organ donor, lack of confidence in offering organ donation, no contact for transplant coordinator, shortage of ICU beds, coroner involvement, and limited resources.Reference Aubrey, Arber and Tyler25
DISCUSSION
Interpretation
This systematic review investigated what percent of actual, missed, and potential organ donors come from the ED (Table 5). We demonstrated that the ED is a source of successful organ donors; patients referred from the ED are more likely to become successful donors, and they donate more organs than patients referred from elsewhere in the hospital (Tables 1 and 2). We also found that a significant proportion of patients die in the ED without exploring the possibility of organ donation and are often missed as donors due to a failure to refer for consideration of organ donation (Tables 3 and 4). Several themes emerged regarding why potential donors are missed. The most common were inaccurate assumptions regarding inclusion criteria and forgetting to refer the patient. All seven papers describing successful neurologic determination of death and all six papers describing successful donation after circulatory determination of death highlighted the importance of involving an organ procurement organization or coordinator in the donation process. The role of the ED healthcare team is predominantly in referral for consideration of organ donation to the organ donation organization or coordinator.
Table 5. Summary of all papers
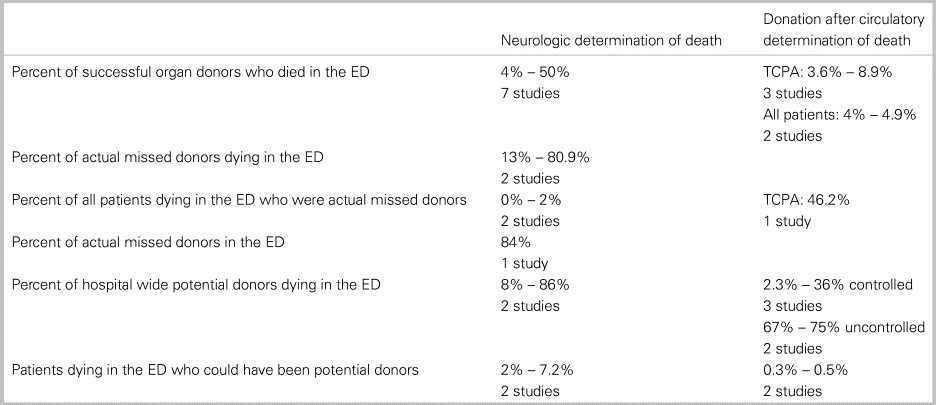
ED = emergency department;
TCPA = traumatic cardiopulmonary arrest.
Comparison to previous systematic reviews
Several systematic reviews have been conducted on organ donation previously; however, they describe techniques of organ extraction, discuss techniques to increase likelihood of successful donation, or pool all acute areas of the hospital.Reference Squires, Coughlin and Dorrance9,Reference Van Erp, van Dullemen, Ploeg and Leuvenink10,Reference Sandroni, D'Arrigo and Callaway35 The strength of this systematic review is that it is the first that we are aware of to investigate organ donation in ED patients specifically.
Limitations
There are several limitations to this systematic review. The studies had heterogeneous populations, used different inclusion criteria for organ donors, or did not mention their criteria, precluding a meta-analysis. There is a very large range in percentages of successful and missed donors in the studies, and it is difficult to draw meaningful conclusions on why these large ranges exist based on the data in the studies. Many of these factors impacting rates of donation may be out of the realm of the ED. Studies investigating missed or potential donors do not reflect on how many of each of those donors would be lost in the consent process, procurement process, or transplantation process, so the numbers of potential donors would be lower than reported. In addition, most of the studies included in this review were retrospective and are limited by the biases associated with conducting a retrospective study.
Clinical implications
Inaccurate assumptions regarding inclusion criteria and medical suitability can be addressed by involving an organ donation coordinator, organ donation nurse, or organ procurement organization involved early in the dying process.Reference Alarhayem, Cohn and Muir26 The role of the ED in many of the successful organ donation studies was in timely referral to the organization or coordinator. Involving a separate organization also removes some of the conflict of interest and ethical dilemma placed on the ED to simultaneously provide patient care and discuss organ donation.Reference Miller, Gardiner and Gubler6 Recent Canadian guidelines have been developed regarding the process of consent and approaching families.Reference Shemie, Robertson and Beitel36 The role of the physician is to ensure that the organ procurement organization has been contacted. These guidelines also recommend the healthcare team involved in patient care not approach the family regarding organ donation until an organ donation organization has been contacted. They suggest that any family meetings involve the donor coordinator, primary bedside nurse, and most responsible treating physician. It is clear that a multi-disciplinary approach is essential when discussing organ donation.
Resource utilization was another ethical dilemma identified in this systematic review. Although it seems intuitive that ICU admission for organ donation is costly, Melville et al. (2017) found that patients transferred to the ICU for consideration of organ donation did not use disproportionate resources when compared with patients transferred for palliative care.Reference Melville, Kolt and Anderson37 This perceived boundary should not prevent referral of dying patients to an organ procurement organization.
Research implications
Several knowledge gaps exist in organ donation from the ED. Future research should determine the optimal education curriculum to overcome misconceptions regarding organ donation. Also, the optimal timing of organ donation discussions during resuscitations should be elucidated. The feasibility and impact of uncontrolled donation after circulatory determination of death and donation in conjunction with Extracorporeal membrane oxygenation (ECMO) and Resuscitative endovascular balloon occlusion of the aorta (REBOA) are other areas of future research.
CONCLUSION
In conclusion, the ED is a source of actual and missed donors. Potential donors are often missed due to incorrect assumptions regarding eligibility criteria and failure of the healthcare team to refer patients for consideration of donation. Early incorporation of an organ procurement organization increases successful donation. ED healthcare professionals should be aware of the organ donation referral process at their institution to ensure that no organ donors are missed.
Acknowledgements
We would like to thank librarians Risa Shorr and Johanne Gohier for their assistance with the search criteria and obtaining the papers.
Presentation
This study was presented at the Canadian Association of Emergency Physicians (CAEP) 2018 on May 28, 2018.
Financial support
Funding to pull three articles ($39) was obtained from the Department of Emergency Medicine. Funding for presentation at CAEP was provided by the Department of Emergency Medicine in Ottawa.
Dr. Stiell holds a Distinguished Professorship and University Health Research Chair from the University of Ottawa.
Author contributions
JM was responsible for the study concept and design, acquisition of data, analysis and interpretation of data, drafting of manuscript, critical revision of the manuscript important for intellectual content, and data analysis. BE was responsible for the acquisition of data, critical revision of the manuscript important for intellectual content, and data analysis. SD was responsible for the study design and critical revision of the manuscript important for intellectual content. IS was responsible for the study concept and design, critical revision of the manuscript important for intellectual content, data analysis, and acquisition of funding.
Competing interests
None declared.
SUPPLEMENTARY MATERIAL
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2019.365








