Introduction
Purpose and Context
As of 2012, eight per cent, or 2,200,000 Canadians received some form of health care at home. Forty per cent of these people were senior citizens, with 27 per cent 75 years of age or older (Sinha & Bleakney, Reference Sinha and Bleakney2014). With a growing shift towards “aging in place,” more senior citizens are living at home with chronic health and social issues that require primary and community health services to be organized and coordinated in a manner that supports their needs. For example, in 2012, 12 per cent of Canadian senior citizens had received care for a long-term health condition over the previous year (Sinha & Bleakney, Reference Sinha and Bleakney2014). However, the majority of Canadian family physicians work without the support of an interdisciplinary team and may have little flexibility to devote extra time to complex or frail patients (Muldoon, Rowan, Geneau, Hogg, & Coulson, Reference Muldoon, Rowan, Geneau, Hogg and Coulson2006). In addition, home health services are generally funded through provincial/territorial health systems and are rarely coordinated in a manner that would allow for full interdisciplinary team care (Hollander, Reference Hollander2012; Romanow, Reference Romanow2002).
In 2010/11, we undertook a study to evaluate the quality and sustainability of secure audio conferencing as a way to increase care planning for patients whose care was shared between home health staff (home care nurses, community rehabilitation professionals, case managers) (HHS) providing health care services to patients with acute, chronic and palliative health needs, and family physicians working in small group or solo practices (FPs), in an urban multicultural setting.
The context in which the intervention took place was that of publicly funded primary care delivered through private FP clinics, and publicly owned and operated home health services delivered by health authority employees. Within the community where the intervention took place, time-limited home health services are provided on a short-term basis to patients who require acute, palliative, or rehabilitative support. Continuous home health services are provided on a longer term basis (usually more than three months) to individuals who are at significant risk of hospitalization or facility placement as a result of unstable chronic health conditions, and/or a combination of living situation and personal resources, or to individuals with stable chronic conditions who require support to continue living in the community (British Columbia Ministry of Health, 2012). All, or nearly all, patients seen by HHS have a FP.
Access to primary care was based on patient choice and an FP decision to accept that patient into their practice. A given FP might have patients from many different areas of the city. Some FPs provided after-hours care and/or made house calls and some did not. At the time of the study, a minority of FPs were using an electronic medical record (EMR). HHS patients were assigned by geography, with service provided primarily through home visits to patients. At the time, there was no routine use of teleconference technology by HHS for communication. HHS were utilizing an electronic clinical documentation system; however, few of the FPs could access it, and HHS were not able to access any FP records (EMR or paper based).
Interprofessional Collaboration
Interprofessional collaboration is defined as “a process by which individuals from different professions structure a collective action in order to co-ordinate the services they render to individual clients or groups” (Sicotte, D’Amour, & Moreault, Reference Sicotte, D’Amour and Moreault2002). For patients, the potential outcomes of integrated teamwork between HHS and FPs include decreased duplication of assessments, more efficient information transfer between services, reduction in medication errors and complications, reduction in the number of emergency visits and hospital admissions/readmissions, reduced length of hospital stay, reductions in medical procedures and adverse events, lower hospital-related mortality, improved chronic disease management, more effective pain and symptom control, delay in admission to long term care, and increased patient satisfaction (Accreditation Canada and Canadian Home Care Association, 2013; Jesmin, Thind, & Sarma, Reference Jesmin, Thind and Sarma2012; Ruggiano et al., Reference Ruggiano, Shtompel, Hristidis, Roberts, Grochowski and Brown2012; Suter et al., Reference Suter, Deutschlander, Mickelson, Nurani, Lait and Harrison2012). Teamwork between physicians and personnel in other health disciplines has a positive impact on palliative patient outcomes such as symptom and psychosocial management (Goldschmidt et al., Reference Goldschmidt, Groenvold, Johnsen, Stromgren, Krasnik and Schmidt2005) and ability to accommodate patients’ preferred location of death in home-based palliative care (Marshall, Howell, Brazil, Howard, & Taniguchi, Reference Marshall, Howell, Brazil, Howard and Taniguchi2008).
Successful collaboration requires an understanding of the scopes of practice of those involved (Baxter & Brumfitt, Reference Baxter and Brumfitt2008; Molyneux, Reference Molyneux2001; Neergaard, Olesen, Jensen, & Sondergaard, Reference Neergaard, Olesen, Jensen and Sondergaard2010; Suter et al., Reference Suter, Arndt, Arthur, Parboosingh, Taylor and Deutschlander2009). Such understanding leads to role clarity and facilitates trust and respect (Suter et al., 2009) which, along with a “shared care” culture, are key to fostering successful interactions between health professionals (Neergaard et al., 2010). Shared space and unscheduled shared time facilitate interprofessional collaboration (Goldman, Meuser, Rogers, Lawrie, & Reeves, Reference Goldman, Meuser, Rogers, Lawrie and Reeves2010; Oandasan et al., Reference Oandasan, Conn, Lingard, Karim, Jakubovicz and Whitehead2009; Rice et al., Reference Rice, Zwarenstein, Conn, Kenaszchuk, Russell and Reeves2010) by encouraging multiple opportunities for unplanned communication (e.g., in hallways between patient visits) (Goldman et al., 2010).
However, in Canada, FPs and HHS face numerous barriers to effective collaboration, particularly with respect to “shared space and unscheduled shared time” for patients who have acute or complex health care needs. FP offices and HHS teams in Canada are rarely co-located; moreover, they do not share a common clinical documentation system. Publicly funded home health services are provided through employees of provincial health authorities/regions (Hollander, Reference Hollander2012). In 2016, more than 90 per cent of Canadian FPs were remunerated through fees-for-services, and 60 per cent were in solo or group practices (Canadian Medical Association, 2016). The most common forms of interaction between HHS and FPs are still telephone calls and faxes (Ruggiano et al., Reference Ruggiano, Shtompel, Hristidis, Roberts, Grochowski and Brown2012). These organizational and operational circumstances result in a lack of timeliness of information exchange, a lack of direct contact between HHS and FPs, difficulty transferring information across different work locations, poor continuity given the variety of different home health professionals, a lack of opportunity for engagement with each other in proactive problem solving for deteriorating patients, and difficulty coordinating appropriate specialty referrals.
In these circumstances, opportunities for spontaneous communication are few. Such limited interaction about shared care of patients hinders the opportunity to develop role clarity and mutual respect for each other.
Research Objective and Questions
We implemented a practical, low-cost option for connecting FPs and HHS with the goal of increasing the quantity and quality of shared patient-related collaboration without changing documentation methodology or team location.
Two research questions are addressed in this article:
(1) Will use of a targeted communication strategy increase the quality of patient-related care planning and coordination between FPs and HHS?
(2) What parts of the targeted communication strategy do FPs and HHS evaluate as being most useful, and what would they require in order to sustain the strategy after the study is complete?
Methods
Participants
All HHS staff (48 full-time equivalent staff members including registered nurses, occupational and physical therapists, case managers, nutritionists, and program assistants [PAs]) and a convenience sample of 24 FPs providing service in one geographic area of a large multicultural Canadian city participated. Unlicensed community health workers, also part of HHS, were excluded from the intervention. Details on methods including sampling and recruitment strategies, challenges, and outcomes can be found elsewhere (Berg, Reference Berg2013; Berg et al., Reference Berg, Barer, Sheps, MacNab, McGregor and Wong2015).
Design
This study used a quasi-experimental design where we examined the effect of a communication-improvement intervention. The intervention included: a secure audio conference line for each intervention FP, pre-scheduled times to engage in audio conferencing about shared patients, provision of lists showing patients shared between HHS and intervention FPs, and use of a tool by HHS to structure audio conference discussions. The tool used by HHS was an adaptation of the original Situation-Background-Assessment-Recommendations (SBAR) tool. (Leonard, Bonacum, & Graham, Reference Leonard, Bonacum and Graham2001) The adapted tool was piloted by staff of another HHS team in the health authority prior to use in the study.
In FP offices, medical office assistants (MOAs) played a key role in scheduling the time for the audio conferences into their FP schedule, and liaising with HHS with regard to the details of the audio conferences (patients to be discussed and audio conference logistical details). Similarly, in the HHS office, PAs were important for coordinating logistics for the audio conferences. For example, PAs kept a whiteboard with the scheduled audio conference times for each intervention FP on which HHS would record the names of patients to be discussed. The PAs also faxed lists of shared patients and audio conference details to the intervention FP offices.
Mixed methods were used to evaluate the intervention. We assessed whether participants perceived that the intervention enhanced collaboration, what parts of the intervention worked, and how successes could be sustained. We also evaluated the impact of the intervention on the number of shared patients and the frequency of communications (see Berg et al., Reference Berg, Barer, Sheps, MacNab, McGregor and Wong2015). Pre-intervention activities included capturing demographic information and administering a modified version of a published survey (referred to henceforth as the “Collaboration Survey”) (Fairchild, Hogan, Smith, Portnow, & Bates, 2002). After the pre-intervention period, FPs were randomly allocated to the intervention or usual communication group until there were twelve in the intervention group.Footnote 1 The intervention lasted for eight months. Post-intervention activities included semistructured focus groups (with HHS) and interviews (with FPs), and readministration of the Collaboration Survey.
Collaboration Survey
The survey, originally designed by Fairchild et al. (2002), measured collaboration between FPs and HHS across four themes: satisfaction with communication, perceived control of utilization of home care services, potential impact of better communication, and improving communication. Because some of the survey questions were specific to the United States context, they were adapted to the Canadian environment and trialed on a convenience sample of FPs (3) and HHS (4), who suggested a small number of minor wording changes for clarity.
Interviews and Focus Groups
All FPs (both control and intervention) had an opportunity to participate in a post-intervention semistructured interview; post-intervention focus groups were scheduled with HHS by discipline. An interview/focus group guide was used to probe areas such as how FPs and HHS usually communicated and their satisfaction with patient-related care planning; changes occurring during the intervention period; the perceived impact of the intervention on their time, workload, and patient outcomes; and how the intervention might be sustained after the study. Data were audiorecorded, transcribed, and anonymized.
Analysis
Transcript coding was completed using a qualitative software package, HyperResearch 3.0 (ResearchWare, 2011). The data were coded based on a structure that was developed by three of the authors (S.B., S.T.W., M.M.) who independently read different transcripts. Systems theory (Begun, Zimmerman, & Dooley, Reference Begun, Zimmerman, Dooley, Mick and Wyttenbach2003) guided the coding. We viewed the HHS office and each individual FP office as dynamic and capable of learning, with learning being non-linear and context dependent. Data within the codes were read and reread by members of the research team in order to analyse similarities and differences. This process was iterative, informed by successive rounds of discussion among the co-authors.
With regard to the Collaboration Survey, the “satisfaction with communication” survey items were grouped to create one score, as with the original Fairchild et al. (2002) survey. The specific items in the collapsed score included eight Likert questions concerning ease and usefulness of communication either orally or in written form, such as orders. Each control and intervention FP’s pre-study results were compared with their own paired post-study results using the signed rank test for paired data. The HHS anonymous surveys were analysed using the Wilcoxon rank- sum test. Data were analyzed using R (version 2.14.2 for Mac) statistical software (R Development Core Team, 2012).
The qualitative and quantitative results were integrated in the overall analysis, in order to draw inferences reflecting both approaches (Ostlund, Kidd, Wengstrom, & Rowa-Dewar, Reference Ostlund, Kidd, Wengstrom and Rowa-Dewar2011). All procedures were approved by both the University of British Columbia’s Behavioural Research Ethics Board and the local health authority ethics committee.
Results
Participation in Collaboration Surveys
Forty-six and 36 HHS completed the pre-intervention and post-intervention surveys, respectively. Based on pre-intervention data, 94 per cent of HHS completing the survey were female, and had worked an average of nine years in home health. Based on full-time equivalents (41.87) for clinical staff (nurses, case managers, occupational and physiotherapists, and nutritionists) there was 100 per cent participation of HHS in the pre-study survey, and 85 per cent participation in the post-study survey.
Tables 1–3 provide a comparison of the pre- and post-study Collaboration Survey results for HHS, and indicate where the difference was statistically significant.
Table 1: Collaboration survey: Comparison of home health staff pre- and post-satisfaction with communication score results
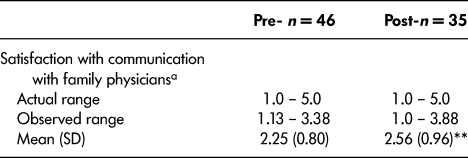
Note. A higher score is equated with higher satisfaction.
a Scale score (Items 1–8)
** p ≤ .05, Wilcoxon rank-sum test with continuity correction (two tailed)
Table 2: Collaboration survey: Comparison of home health staff pre- and post-score results related to potential impact of better communication

Table 3: Collaboration survey: comparison of home health staff pre- and post-score results related to improving communication
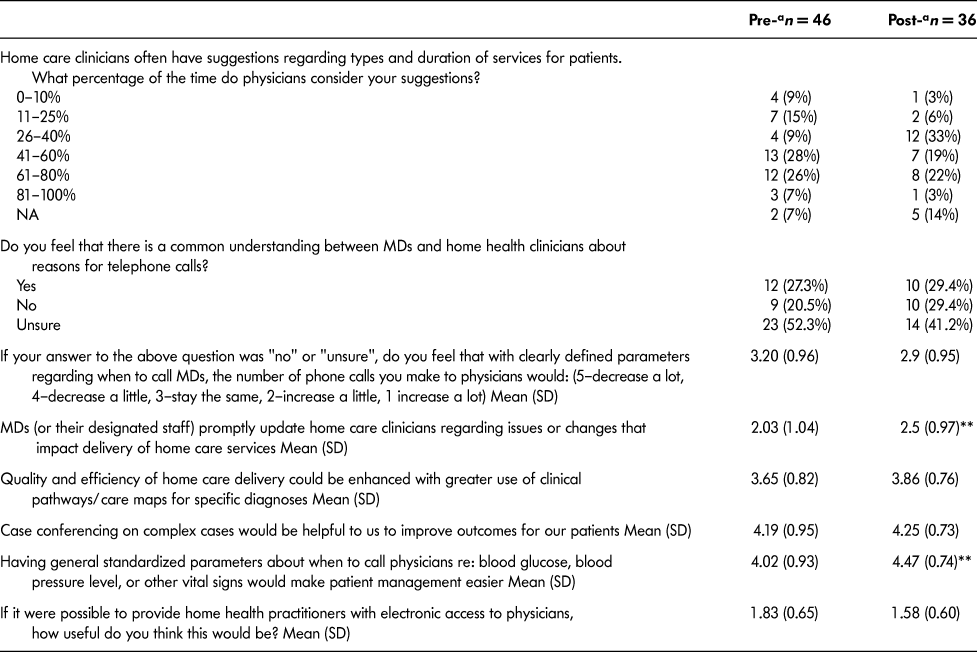
Note. a Unless otherwise specified, all item responses used a five point Likert scale (5–Excellent, or Strongly Agree; 4–Very Good, or Agree Somewhat; 3–Good, or Neither Agree Nor Disagree; 2–Fair, or Disagree Somewhat; 1–Poor, or Disagree Strongly)
** p ≤ .05, Wilcoxon rank-sum test with continuity correction (two tailed)
The response rates for FPs completing the surveys was 100 per cent of the 24 initial FPs for the pre-study surveys, and 100 per cent of the 22 FPs completing the post-study surveys. FPs had been practicing for 24 years on average, and 86 per cent were male.
Tables 4–6 provide a comparison of the pre- and post-study Collaboration Survey results by intervention group, and indicate where the difference was statistically significant.
Table 4: Collaboration survey: Comparison of pre- and post-survey satisfaction with communication scores by intervention group for family practitioner (FP) participants
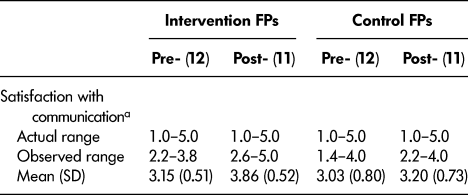
Note. A higher score is equated with higher satisfaction.
a Scale score items 1–5
Table 5: Collaboration survey: Comparison of pre- and post-survey potential impact of better communication scores by intervention group for family practitioner (FP) participants
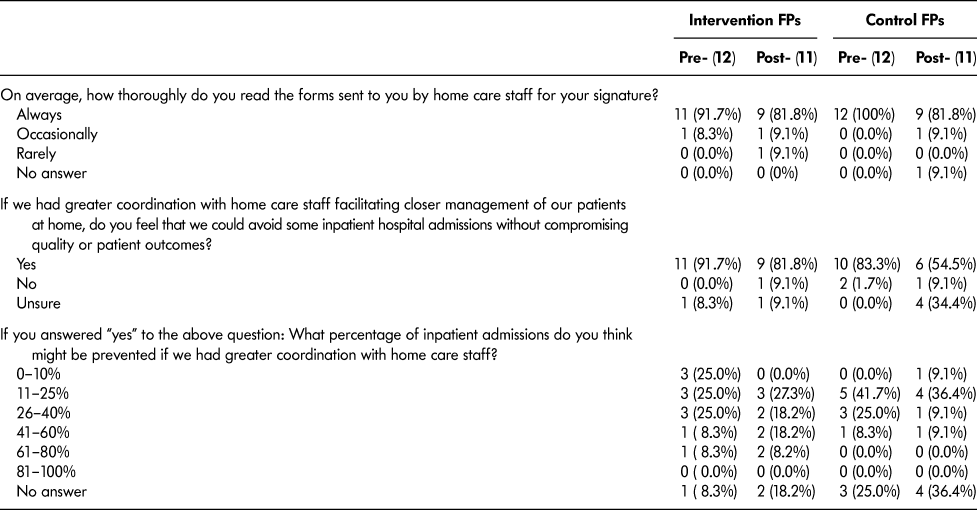
Table 6: Collaboration survey: Comparison of pre- and post-survey improving communication scores by intervention group for family practitioner (FP) participants
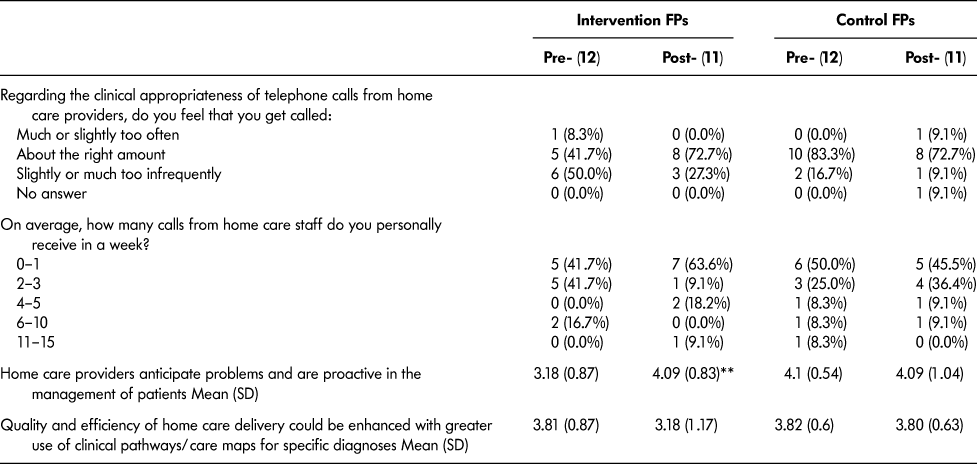
Note. Unless otherwise specified, all item responses used a five point Likert scale (5–Excellent, or Strongly Agree; 4–Very Good, or Agree Somewhat; 3–Good, or Neither Agree Nor Disagree; 2–Fair, or Disagree Somewhat; 1–Poor, or Disagree Strongly)
** p ≤ .05 Wilcoxon signed rank test with continuity correction for difference in pre- and post-test scores within each group
Participation in Interviews and Focus Groups
Four focus groups were conducted at the HHS worksite, each lasting about one hour: home care nursing (14 participants), rehabilitation (occupational and physiotherapy, 10 participants), case managers (13 participants), and PAs (4 participants). Eleven of the 22 FPs (50%) were interviewed, 3 from the control and 8 from the intervention arm. Interviews were conducted in each FP’s office, varying in length from approximately 30 minutes to one hour. Analysis of the qualitative data resulted in four main themes with a number of sub-themes associated with each main theme. Main themes included: “Working in Silos”, “Change is Hard at First”, “Tools as Bridges”, and “Imagining the Future.” Table 7 provides a summary of themes, with examples of what was captured under each.
Table 7: Themes arising from qualitative analysis of the data gathered in the focus groups (home health staff [HHS]) and interviews (family physicians [FP]) about usefulness and sustainability of the intervention
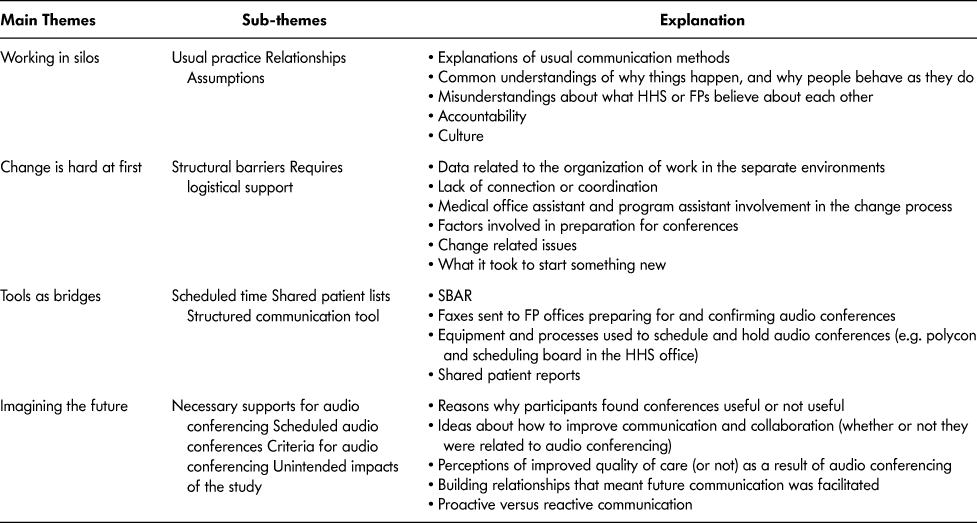
Note. SBAR = Situation-Background-Assessment-Recommendations
Results Integrated across Qualitative and Quantitative Sources
Generally, the qualitative and quantitative results were complementary in providing a picture of participants’ experience with the intervention. The following section provides a summary of the integrated qualitative and quantitative analysis, describing participants’ experience of the quality and sustainability of the intervention with respect to increased communication about shared patients.
Communication: Usual Practice
HHS and FPs agreed that telephone calls and faxes were the usual modes of communication. They also agreed on the main patient-related issues about which they traditionally communicated, including confirming changes to care plans for wound or catheter care; medications; weight bearing; communicating changes in patients’ medical, cognitive/behavioural, or functional status; managing documentation required for residential care or hospice admission, and other patient transitions.
Although telephone calls were considered an appropriate method for more urgent issues, both HHS and FPs identified problems such as difficulty connecting by telephone, and interference with work schedules. Faxes were chosen over telephone calls when more detailed information was required, when a record was required for clinical documentation, and to avoid difficulties encountered when trying to connect by telephone. For FPs with EMRs, faxes were seen as problematic because they then had to be scanned and the scanned data did not fit easily into the EMR structure.
That both HHS and FPs had issues with their usual communication practices was also reflected in the Collaboration Survey results. Improving Communication was the only HHS score that had mean responses in the higher ranges of the scale, even after the intervention. One sub-score (standardized parameters about when to call a FP about blood glucose levels or blood pressure [BP] levels, making patient management easier) in the grouping showed a statistically significant increase post-study.
Communication: Structural Barriers
Both HHS and FPs identified differing documentation systems, geographic boundaries, and work processes as key barriers to communication. Incompatible clinical documentation systems were often mentioned as a barrier to joint communication:
Intervention FP: “There are two parallel electronic records which don’t cross-communicate and we live in two different worlds, and I think that may be one of the reasons why there’s not much communication.”
Differing geographic boundaries was also problematic, because FPs often had patients in areas of the city (or outside the health authority boundaries) other than that covered by the study HHS team. Similarly, HHS were involved with hundreds of FPs at any given point in time across the health authority and FPs were not necessarily aware of which HHS site their patients were attached to.
Differing work processes in primary care compared with home health had numerous implications for communication. For example, because FPs book appointments in 10–15 minute increments, but actual appointment times vary, it was difficult for FPs to commit to specific times to communicate with HHS. Likewise, HHS visiting patients in their homes, or driving between patient homes, could not consistently time their calls to coincide with a break between FP appointments.
In addition, both HHS and FPs lacked awareness of the others’ usual work processes, leading to potentially erroneous assumptions about clinical practices. For example, HHS’ lack of familiarity with the FP fee structure led some to think that FPs would not participate in conferences because the time was not billable (home care nursing focus group), and although FPs could bill for such communication, most HHS and many FPs were unaware of this opportunity.
Satisfaction with Communication: Relationships
Both HHS and FPs noted increased positive relationships as a result of the audio conferencing, facilitating more specific and personalized communication outside of the audio conferences. For example, one case manager focus group respondent commented that after participating in a teleconference with an FP he had built rapport so that the FP was more likely to respond to his phone calls outside of scheduled audio conference times. This was echoed in a comment from an intervention FP:
“It [the intervention] helped in a couple of ways. It improved my written communication. I spent more time dictating notes back to them. And I think it was more personalized dealing with, you know, the specific [occupational therapist] who knew the patient rather than having a general response.”
The Collaboration Survey findings were consistent with the qualitative data in the “Control of Home Health Resources” items. For HHS, there was an increased belief that FPs update HHS promptly about issues or changes that affect delivery of home health (with the mean [SD] number of responses rising from 2.03 [1.04] to 2.5 [0.97]). The mean (SD) response among intervention FPs increased for the item “home care providers anticipate problems and are proactive in management of patients” (from 3.18 [0.87] to 4.09 [0.83]). These statistically significant results, along with the qualitative data, suggest that both parties perceived improvement in role clarity and relationships.
Need for Logistical Support
The HHS PAs provided logistical and training support to HHS, as well as episodic support/education to the FPs’ MOAs. In all HHS focus groups, the PAs’ role was the most consistently valued logistical support for the audio conferencing.
For MOAs, the idea of scheduling dedicated time during practice visit hours for a FP audio conference was, for some, difficult to fathom, even when it was explained that the FP’s time would be compensated. Several MOAs initially suggested adding time to their FP’s workday and booking conferences prior to patient appointments. Support from the research team was required to effect this change in practice.
Experience with Scheduled Audio Conferences
For both FPs and HHS, experiences with audio conferencing were mixed. Negative experiences were associated with miscommunication about the scheduled time, or participants being late or unavailable at the scheduled time. The positive experiences with audio conferencing were described using phrases such as “specific and efficient communication”, “focused”, “convenient”, “scheduled meetings bring structure”, “more comprehensive picture”, and “collaborative.”
Intervention FP: “It was good because there were a couple (of patients) at one time, there was a [physiotherapist] and an occupational therapist and a home care nurse.”
Rehabilitation Focus Group Respondent: “… often it’s just one team member calling him individually as opposed to the whole group hearing it together. It [the audio-conference] was useful.”
For both FPs and HHS, prior notice about which patients were to be discussed allowed more focused time for substantive communication. HHS mentioned several times that they had the FP’s full attention for the audio conference time, and that the FP had reviewed the patient’s chart. The participating FPs agreed that the audio conferences were superior to one-off telephone calls because they had an opportunity to be prepared.
Intervention FP: “it was a very direct approach to patients’ care and I didn’t feel like an island, alone, just treating the patient. That was the positive part.”
The Collaboration Survey results were consistent with the qualitative results in suggesting that both HHS and FPs experienced a positive change in perception of collaboration. Although both pre-and post-intervention, the HHS mean scores related to “Satisfaction with Communication” were in the lower range of the scale (below 3), there was a statistically significant increase in the mean score, from 2.25 (0.80) to 2.56 (0.96). The pre- and post-survey results for both control and intervention FPs were in the positive range (between 3 and 5), suggesting that FPs were generally satisfied with the collaboration with HHS even before the intervention. Although the FP differences between pre- and post-intervention results did not achieve statistical significance, the average satisfaction scores improved, and the increase was greater for intervention FPs (from 3.15 [0.51] to 3.86 [0.52]) than control FPs (from 3.03 [0.80] to 3.20 [0.73]).
Given the large number of FPs with whom HHS routinely communicate, pre-scheduled audio conferences at times convenient to each FP were not seen as practical by either FPs or HHS. For HHS, the emergent process was to provide a PA with several times that a conference would work, and ask her/him to coordinate with the appropriate MOA to book the FP’s time.
Program Assistant Focus Group Respondent: “Whenever I’ve called … and said, ‘I’m calling from [HHS team] unit, regarding such and such patient. One of our clinicians at our office is also involved with this patient and they would like to speak to the doctor about them through an audio-conference. These are the dates and times the clinician is available; is the doctor available at these times?’ And once you have confirmed a time I’ll tell the MOA ‘okay, here are the codes that you need, this is the phone number, this is the code you dial in, and I’m going to fax it to you right after I hang up with you.’”
The intervention FPs actively participating in audio conferences were prepared to book an ongoing time for conferences into their schedule:
“I would like to have an opportunity for regular interaction with all the units, at a specific time, by telephone. And if there isn’t anything that needs to happen, feel free to cancel it…”
In the future, having lists of shared patients faxed (or entered into an FP electronic medical record) automatically at regular intervals seemed to make the most sense to both FPs and HHS.
Experience with Shared Patient Reports and Structured Communication Tool
Respondents were asked to comment on several tools used to facilitate conferences, including FP-specific shared patient lists that were provided to all involved HHS staff and faxed to the FPs before pre-scheduled conferences, and the structured communication tool (SBAR) used by the HHS to prepare for audio conferences (Berg et al., Reference Berg, Barer, Sheps, MacNab, McGregor and Wong2015; Leonard et al., Reference Leonard, Bonacum and Graham2001).
The shared patient lists seemed to be valued more highly by FPs than by HHS. They provided FPs with an opportunity to view a list of those of their patients who were on the HHS caseload and confirm which HHS disciplines were involved with specific patients. HHS found the SBAR useful for organizing information prior to the audio conferences and to keep conferences focused. Despite FP respondents being unaware that SBAR was being used, they noted that the conferences were efficient and goal oriented.
Intervention FP: “… I’d anticipated they had a pre-meeting. … And I’m not sure how they did it at the other end, but the presentation over the phone was organized and efficient.”
Reasons for Audio Conferencing
Three types of patient issues were identified in interviews and focus groups as signalling the need for interprofessional audio conferencing: medical or functional complexity, social complexity, and patient transitions.
Medical and functional complexity generated the most discussion between HHS and FP respondents. Examples of specific medical issues included: insertion and management of feeding tubes, medication management including medications with risky side effects such as warfarin, and symptom control. Functional issues with elderly patients included patient cognitive or mobility changes, and assisting family caregivers to cope with functional and cognitive decline. HHS also noted that it was helpful to be able to discuss end-of-life plans for patients transitioning from chronic disease management to palliative care (rehabilitation focus group) and pain management (nursing focus group).
Control FP: “Someone whose ADLs are declining… or getting more demented. The family just can’t cope with it…so we’re now not able to deal with it at home. Two old persons, you know their spouse is 85, and the husband is 90, he’s not going to help… So, in a sense, for those ones that are elderly geriatrics and complex, if there is some way we can quickly liaison with the long-term care provider, whether it is an intake worker or what, is probably always needed.”
Regarding social complexity, the most frequent issue raised was maintaining a consistent approach across the interprofessional team for patients with psychological problems or personality issues:
Intervention FP: “A team approach is a lot easier [for managing] a “difficult” patient if your approach can be coordinated so you are consistent, because the worst thing that happens with the difficult patient is that they hear one thing from the nurse and a different thing from the doctor or [occupational therapist] or [physiotherapist]. So when we were able to communicate that way [in an audio-conference] we were able to discuss before we did some things, and be consistent. And that’s very useful.”
Rehabilitation Focus Group Respondent: “Where are we going with this person? We don’t know. Sort of felt like we were swimming, and we have this discussion together, but it was incredibly helpful to have the discussion with the GP, who was actually seeing it quite clearly.”
The third category, “patients in transition”, focused on coordinated care planning for new patients transitioning onto the FP caseload, and/or new patients on the home health caseload:
Intervention FP: “In managing new patients, if you have this get together beforehand you can plan how you are going to interact and what changes you are going to make or how you are going to approach the patient, whereas with the old system that pre-planning never happened.”
In addition, patients admitted to or discharged from acute care facilities were highlighted as benefitting from a conference to ensure coordination of up-to-date care plans. Transitioning patients to a new care setting, such as moving from home to assisted living, hospice, or residential care was also seen as a point at which communication was important.
In several cases, intervention FPs provided examples of where they perceived a difference in quality of care or outcome that was influenced by the care conferences. One example involved a complex patient who required a feeding tube:
Interviewer: “Did you, and this would be perceptual, but did you have a feeling that it influenced the outcomes, or the quality of care…”
Intervention FP: “Oh I think so oh yeah.”
Interviewer: “… that you as a team could provide to the patient?”
Intervention FP: “Oh absolutely… Well again, this tube feeding person. That’s a difficult thing to get started. Started out with swallowing difficulties, that was investigated forever. And then, you know, we finally made a decision that we should recommend to them that they do it this way, although I don’t like to do tube feeding at home or in the facility. But these people were focused that they were going to do everything possible and the only way to minimize the major difficulties that they have had with swallowing and aspiration and that kind of thing was to get into the tube feeding, and I think this team helped to get that happen. The way it was set up would have been very difficult to fax back and forth and... without having the discussion with the team to have a direction about how to do it. That was, that was a major example of management.”
Unintended Impacts during the Study
Once the intervention phase was underway, an extra audio conference code was provided, on request, to the HHS for use with non-intervention FPs and other care providers. Although the number of times HHS used the extra audio conference code was not formally documented, in the focus groups, its use was noted on several occasions (e.g., to coordinate respite care). HHS were blinded to the FPs who were part of the control group, and there is one instance in which a control FP participated in an audio conference with HHS through this route.
Discussion
Our goal was to evaluate the quality and sustainability of secure audio conferencing as a way to increase care planning about patients shared by FPs and HHS. The intervention was chosen to be practical and low cost, and despite the short timeline and small number of participants, was able to show some success. Other studies have also shown that introduction of initiatives to increase the quality of communication, which are low impact and practical, and incorporate the ability for users to shape the intervention, can be successful (Grudniewicz et al., Reference Grudniewicz, Tenbensel, Evans, Steele Gray, Baker and Wodchis2018; Lyngstad, Grimsmo, Hofoss, & Helleso, Reference Lyngstad, Grimsmo, Hofoss and Helleso2014).
Both the qualitative and quantitative findings suggest that HHS and FPs observed positive changes in patient-related collaboration during the intervention period. Qualitative data also confirm that participants found audio conferencing to be an efficient and effective way to coordinate care plans for some shared patients. Information provided by HHS in focus groups highlighted the challenge in implementing any sustainable change in highly structured systems. Pre-scheduling a time for a specific FP to talk on the phone with a few HHS members required significant change and commitment from FPs, MOAs, and HHS.
The data obtained in this study confirm previously identified barriers to interprofessional collaboration, such as non-aligned documentation systems, geographic boundaries, and workflows, and suggest that these barriers contribute to reactive communication patterns for HHS and FPs (e.g., telephone calls and faxes to confirm orders or decisions). Survey results showing increased satisfaction with communication, and strong agreement by both intervention FPs and HHS to update each other about patients suggest that FPs and HHS may have experienced increased role clarity and mutual respect as a result of this intervention. Both of these are factors required for successful interprofessional collaboration (Neergaard et al., Reference Neergaard, Olesen, Jensen and Sondergaard2010; Suter et al., Reference Suter, Arndt, Arthur, Parboosingh, Taylor and Deutschlander2009).
The focus groups and interviews suggest that pre-existing usual communication between HHS and FPs was primarily “reactive” in nature, such as confirming physician orders or providing information about a patient’s declining health status. HHS and FP respondents suggested that although telephone calls and faxes are still appropriate for just-in-time communication, the addition of audio conferencing provided an opportunity to move towards more “proactive” communication (i.e., coordinating care for a patient transitioning from hospital to home, coordinating a care plan for more complex interventions that could prevent hospitalization, or ensuring consistency in approach across FP and HHS for patients with psychological or personality issues). This is consistent with findings in a Norwegian study involving electronic communication between home care nurses and FPs that implemented electronic messaging between home care nurses and FPs. In the implementation group, home care nurses and FPs continued to use their traditional (phone calls, faxes, leaving messages with a secretary) communication methods in addition to electronic messaging (Lyngstad et al., Reference Lyngstad, Grimsmo, Hofoss and Helleso2014).
A key finding that has policy implications was the significant value that administrative staff (PAs and MOAs) bring to coordinating health professional collaboration. Unless there is infrastructure (such as time, training, and support) for roles that facilitate communication, collaboration will continue to be sporadic and reactive. Because often in times of fiscal restraint, professional staff may be protected more than administrative staff, the results of this study have implications for considering how interdisciplinary team members work together in effective teams.
Practical tools and logistical solutions (such as circulating patient lists, and use of PAs to organize the calls) suggest that engineering communication is important where co-location and opportunities for unplanned communication do not exist. Arguably, there is a role for cost effectiveness research to determine whether, in the end, addressing the shared space and unscheduled time issues noted, such as co-locating interprofessional teams, are less expensive than numerous infrastructure workarounds. However, as technological solutions (such as real-time electronic solutions) become more prevalent and dependable, co-location may become less necessary as an enabler of effective interprofessional collaboration.
After completion of the study and despite its short duration, the health authority spread audio conferencing as a new initiative designed to enhance integration between primary physician care and home health services. On a time-limited basis, home health budgets were provided additional funds for each conference (in person or over the telephone) used to engage FPs about a shared patient. The extra money received by the home health program was employed to provide short-term change management (such as backfill for PAs arranging the conferences, or for education and orientation of HHS about how to conference), supporting the restructuring of home health teams to work in a more integrated fashion with FPs. As part of this broader effort, FPs were consulted in the design and implementation of a standard process and common tools for audio conferencing. Resources were created to assist FPs and HHS in implementing telephonic communication (Vancouver Coastal Health, 2013). As of April 2014, audio conferences (known in the health authority as “GP care conferencing”) were being used in all communities across the health authority, and were documented as part of the electronic home health clinical record within the “Volume Cube.” A total of 1,793 GP care conferences were documented for the 2014/15 fiscal year, 2,089 were documented for the 2015/16 fiscal year, and 1,976 were documented for the 2016/17 fiscal year. It was noted that the recorded numbers may be lower than the actual numbers in some areas of the health authority because of documentation in a different location on the clinical record (S. Lim, personal communications, December 6 2017 and December 14 2017).
Limitations
The most significant limitation of this study design was the short (eight month) intervention phase, a product of limited timelines imposed by the research funding. To move from some increased role clarity and improved relationships to a shared understanding of how specific communication strategies could affect patient outcomes arguably requires time for FPs and HHS to fully integrate audio conferencing into their daily work routines, and to experience more practical examples of how integrated communication made a difference in patient care. The lack of significance in score changes for the “Potential Impacts of Improved Communication” survey questions may be at least partially explainable by the short timeline and small sample size.
For the purposes of analysing the results of the Collaboration Survey, the small sample size was also a threat to internal validity. However, in part this is mitigated through the use of mixed methods and multiple sources of information to analyse the impact of the intervention. The interviews and focus groups provided rich data that could be triangulated with quantitative results (Thorne, Reference Thorne2008) and that were, for the most part, highly consistent.
The majority of FPs involved in this study were male, with significant years of experience, and many were multilingual. In 2010, across Canada, approximately 60 per cent of FPs were male, and 56 per cent were between the ages of 45 and 64 years (Canadian Medical Association, 2019a, 2019b). Participants who were more experienced and male may have introduced a bias into the study that could limit generalizability.
Finally, this pilot did not include a number of team members who would add value to care conferencing. The most obvious exclusion was the patients about whom information was being exchanged. In addition, community health workers for those patients who receive personal care supports in the home are an important voice. In future research, inclusion of patients and a wider array of care providers would be beneficial.
Conclusion
Despite the limitations noted, this study provides qualified support for the use of audio conferencing as a means to address barriers to collaborative care planning about shared patients for HHS and FPs. Audio conferencing provided the opportunity for FPs and HHS team members to engage in proactive care planning and seems to have led to increased role clarity and respect, as well as higher levels of satisfaction with interprofessional collaboration. That audio conferencing was implemented on a larger scale in the health authority in which this study was embedded, very soon after the completion of the study, represents prima facie evidence of impact, but also demonstrates the potential impact of even small research enterprises that are embedded in care practice settings.









