Introduction
In April 2010, a new system of sickness certification was launched, requiring GPs to consider what aspects of work an individual is capable of, taking medical conditions into account (Department for Work and Pensions (DWP), 2010). The new note focuses on patients’ functional capacity and advises employers on what individuals can or cannot do in their work and what adaptations/adjustments may aid their return to work. It also attempts to increase communication between the GP, patient and employer. The aim is to reduce the ‘sick note culture’, avoid a slide onto out-of-work benefits and chronic worklessness and return people to work quicker. Yet, evidence suggests that GPs lack confidence, training and expertise when dealing with work-related health problems (Hiscock et al., Reference Hiscock, Hodgson, Peters, Westlake and Gabbay2005). Some GPs report experiences of conflict with patients over return-to-work assessments, particularly when symptoms are thought not to be genuine (Wynne-Jones et al., Reference Wynne-Jones, Mallen, Main and Dunn2010a). A recent systematic review highlighted a lack of well-validated tools to support GPs in their task of sickness certification (Letrilliart and Barrau, Reference Letrilliart and Barrau2012). Many GPs reported insufficient time and resources to be able to effectively address patients’ workplace health issues, despite government concern over growing costs associated with workplace sickness absence problems (Hiscock et al., Reference Hiscock, Hodgson, Peters, Westlake and Gabbay2005; Wright et al., Reference Wright, Moseley, Rupatharshini, Stabb, Campbell and Richards2009).
The longer people are out of work, the less likely they are to return and are more likely to become chronically ill (DWP, 2008). Targeted support given at an early stage helps prevent or reduce long-term sickness absence rates, benefit claims and spiralling annual business costs (Waddell et al., Reference Waddell, Burton and Kendall2008). Previous research shows better outcomes for individuals if they are supported while still in work, or have been on sick leave for four weeks or less (Seymour and Grove, Reference Seymour and Grove2005). In contrast, some GPs feel that support should be given after a seven-week absence, and then only to those with mild–moderate rather than severe symptoms (Letrilliart and Barrau, Reference Letrilliart and Barrau2012). Personalised case-managed support is thought to positively impact physical and mental health and help job retention, but UK literature on this is sparse (DWP, 2008; 2011). Return-to-work schemes are generally available for incapacity benefit claimants or the long-term unemployed, but not for those in employment and on sick leave (DWP, 2011).
Given the reported lack of GP expertise and confidence in the area of workplace sickness absence and the knowledge gap surrounding case-managed return to work support, this study set out to examine both of these issues. The study examined levels of GP engagement in what is historically for them an area of low professional interest (Wright et al., Reference Wright, Moseley, Rupatharshini, Stabb, Campbell and Richards2009). At the time of our study, there was no statutory service available to help employed people remain in or return to work after a period of sick leave. Our study data collection period coincided with GPs beginning to use the fit note rather than the ‘sick note’ for Med 3 sickness absence certification.
Method
We designed a feasibility-controlled trial to compare return-to-work rates between individuals supported by their GP and those supported by their GP and workplace health advisers (WHAs). Patients were clustered within general practices, and each practice was allocated either to GP support only (control group) or to GP and WHA support (intervention group). Ethical approval for the study was granted by Liverpool Adult Research Ethics Committee ref. no. 08/H1005/77.
We hypothesised that case-managed intervention in comparison with standard GP care would:
(a) promote better work retention;
(b) enable a quicker and more sustained return to work for those on short-term sick leave;
(c) achieve sustained return to work for those on long-term sick leave of four weeks or more;
(d) achieve more positive outcomes for individuals affected, including job change.
We aimed to test the feasibility of our design, recruitment, data collection methods and follow-up retention, with a view to subsequently conduct a full trial. The target population was sickness absentees and also those at work with a work-related illness (presentees).
Our primary outcome measure was number of days (weeks/months) off work through sickness absence in four months after index consultation. The Registrar General's Occupation Classification (Neighbourhood Statistics, 2009) system was used to identify subgroups. We collected data on a variety of secondary outcomes and baseline comparators to assess the impact of return to work (or not) and the intervention on symptoms and well-being.
We distributed trial information packs to 10 intervention and 29 control practices matched by postcode and Index of Multiple Deprivation Score (Neighbourhood Statistics, 2009) and with comparable population demographics. GPs were asked to distribute trial information packs to patients with workplace health issues.
Health status and job content data were collected for each patient using the SF-36v2 (Ware and Sherbourne, Reference Ware and Sherbourne1992), the EQ-5D (EuroQol Group, 1990) and Job Content Questionnaire (JCQ) (Karasek, Reference Karasek1985). Data were collected at baseline (at first referral) and at four months.
The SF-36 is a psychometrically robust and widely used quality-of-life instrument consisting of 36 items, in eight multi-item scales that measure physical functioning, role physical, body pain, general health, vitality, social functioning, role emotional and mental health. Scale scores are transformed and aggregated to produce two summary measures, the physical component score (PCS) and the mental component score (MCS). Scoring is between 0 and 100, with higher scores indicating better health.
The EQ-5D is a generic patient-reported outcome measure (PROM) that captures patients’ assessment of their own health on the day of assessment. It is included in the current implementation of PROM and is recommended by NICE (2010). The EQ-5D comprises five dimensions and three levels of perceived health status, from Level 1 indicating no problems to Level 3 indicating extreme problems. A unique health state is defined by combining one level from each of the five dimensions and converting it to a single summary index.
The JCQ measures social and psychological characteristics of jobs and addresses the demand/control model hypothesis, which predicts that job strain is more likely to occur when there is high psychological demand and low employee decision latitude. For the purpose of this trial, 12 JCQ items were used covering six dimensions: skill discretion (three items), decision authority (two items), decision latitude (skill discretion + decision authority), psychological demands (three items), supervisor support (two items) and co-worker support (two items).
Summary scores (mean, median, minimum and maximum) were calculated for the SF-36, EQ-5D and JCQ. The mean change in health scores (follow-up − baseline) was calculated for the SF-36 and EQ-5D and JCQ, adjusting for time off sick before first WHA consultation and length of follow-up to see whether change scores were modified by either covariate.
Basic summaries (mean, medians, counts, etc.) regarding age, sex, occupation and type of illness were produced for the intervention and control group at baseline. Four-month follow-up data were collected from the intervention group study completers, and their absence rate was calculated. To estimate absence rates, a negative binomial regression model was fitted to the data to accommodate any overdispersion. The negative binomial model regresses the number of days off work with an adjustment made for different lengths of follow-up per individual using an ‘offset’ term for follow-up length. The following covariates were also considered in the model as to whether they explained variation in the rate of absence from work: sex, age, length of time off work before recruitment, and occupation. Further, the clustering of patients with general practices was accounted for by including practice as an additional covariate. A 10% significance level was used because of the feasibility nature of the study.
Results
At three months, there were no GP referrals to either arm of the trial. It was unclear whether GPs had distributed packs to patients, or if patients had received the packs but had declined to take part. To boost participant numbers in the intervention group, with ethics committee approval, we sent study information packs directly to patients along with their WHA appointment, and this achieved the intervention group recruitment target (n = 60). We used a range of methods to boost the recruitment of controls. We approached 45 control practices, 29 postcode matched with intervention practices and an additional 16 practices contacted through the NIHR Primary Care Research Network. Despite this, only two control practices recruited three patients in total. Two practices declined to take part as controls because they were unwilling to deny their patients the opportunity to access the case-managed support service. Some practices cited time pressure as a reason for not taking part, but the majority failed to respond to emails, phone calls and letters, and thus their reasons for not taking part are unknown.
Because of the lack of GP engagement with the trial, we were not able to compare case-managed support with GP support for workplace sickness absence. Although disappointing, we felt it important to continue with the study to examine the concept of case-managed support for workplace sickness absence and the outcomes associated with this type of support.
Sixty intervention group participants out of a possible 120 took part at baseline, and of them 29 also participated at follow-up. Statistical analysis concentrated on the 29 study completers. Descriptive data have been provided for non-completers and for one control who completed both phases of the trial.
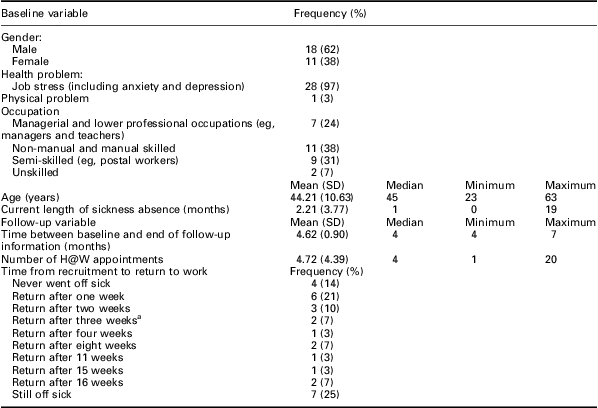
In the intervention group, more number of women took part at baseline and follow-up (Table 1). All three controls were female with an average age of 40 years. Mean age of intervention participants at baseline (n = 60) was 42.48 (SD 12.24; range 19–63). The mean age at follow-up was 44.21 (SD 10.62; range 23–63) (Table 1).
Table 1 Information for 29 intervention group participants who completed the study

aOne person was not off work on recruitment but went off work straight after, and then returned after three weeks.
At baseline and follow-up, the highest numbers in the intervention group were in the non-manual and manual skilled group and over 50% worked in the public sector. All three baseline controls worked in the public sector. The range of occupations at follow-up was broadly similar to that at baseline, with groups 2 and 3 in the majority (Table 1). The four (14%) presentees who stayed at work from baseline to follow-up were in either the skilled or unskilled occupational group and all worked in the public sector.
The mean length of sickness absence at baseline was 2.19 weeks (SD = 2.0; range 1 week–19 months). At baseline, three participants (5%) of the intervention group had physical health problems, two (3%) had physical problems and work-related stress and 55 (92%) had work-related stress of varying degrees (Health and Safety Executive, 2009) due to ‘bullying’ (ACAS, 2009) or ‘harassment’ (ACAS, 2009) at work. Using a negative binomial regression model, the estimated mean rate of absence from work in the intervention group (proportion of weeks off work during follow-up) was 41% (95% CI: 26–65%) of the total follow-up. Owing to the small number of controls recruited, a comparison between the intervention and control groups was not feasible.
Table 2 shows the estimated effect of each covariate on the absence rate in the intervention group. For the continuous covariates (age, length of time off work at baseline), the estimated incidence rate ratio describes how a 1-unit increase in the covariate affects the rate of absence. For example, for age, a one-year increase in age multiplies the rate of absence by 1.05 (95% CI: 1.01–1.11), and therefore the rate of absence is 1.05 times higher for every one-year increase in age. For categorical covariates, the incidence rate ratio shows the absence rate in one category relative to the absence rate in the reference category.
Table 2 Effect of covariates on absence rate

The variables age and length of time off work were statistically significant at the 10% significance level. A higher age and a longer time off work before recruitment were both associated with an increased rate of absence. In addition, there was a significant difference between ‘manual and non-manual’ workers versus ‘unskilled’ workers, with the former group having a rate only 21% of the latter.
Of the 29 intervention group completers, 18 (61%) returned to work between baseline and follow-up (Table 1), and of them three had changed jobs. For the 25 patients who were off work at baseline (ie, recruitment) or (the one person) who went off just after recruitment, the median time to return to work was 7.71 weeks (95% CI: 1.71–15.71). One person from the intervention group was made redundant. Seven (25%) were still off sick at follow-up for periods ranging from five months to two years. Four (14%) presentees had no episodes of sickness absence at either baseline or follow-up. One control who completed the trial was off sick at baseline and follow-up.
SF-36 physical health scores were within range or above standardised SF-36 scores (Figure 1, shaded area) at baseline. In contrast, the majority of SF-36 MCS scores (Figure 2) were below the normal range of standardised scores at baseline, indicating poorer levels of mental health compared with the general population. At follow-up, all but three participants’ MCS scores had improved and 21 of the 29 (72%) intervention group scores had moved within range.

Figure 1 SF-36 Physical Component Summary (PCS) scores at baseline and at follow-up.

Figure 2 SF-36 Mental Component Summary (MCS) scores at baseline and at follow-up.
The 30–39-year-old group showed most impairment in the EQ-5D anxiety/depression domain at baseline (I am extremely anxious or depressed). Fewer people reported anxiety or depression at follow-up (28%) in comparison with 48% at baseline. Presentee's scores were unchanged at follow-up.
Usable data from 28/29 intervention group study completers showed higher scores on 4/6 JCQ scales, indicating the presence of job strain at baseline and follow-up. The supervisor support and co-worker support scales had lower scores, indicating that both of these dimensions contribute less to the development of job strain compared with other scales in the measure.
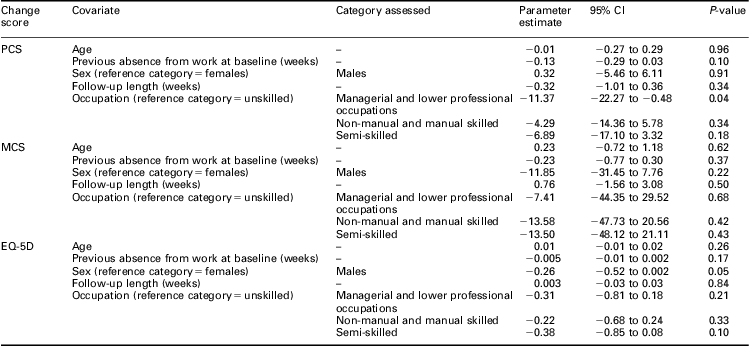
Change scores were calculated for the SF-36 and EQ-5D and JCQ (follow-up − baseline). A one-sample t-test was conducted for each change score (Table 3) to test whether there was significant evidence that they were different from zero. The only variable showing a statistically significant change was the MCS component of the SF-36, with significantly higher values at follow-up, indicating that mental health had improved over time. Using multivariable linear regression, covariates were examined that could possibly explain patients’ health score differences in the change of PCS, MCS or EQ-5D scores between baseline and follow-up (Table 4). Positive parameter estimates suggested that increasing (or having) the covariate increases the difference between baseline and follow-up score. Across all models, all but four of the covariates were not statistically significant (at the 10% level). For change in MCS score, no covariates appeared important. For change in PCS score, the comparison with unskilled versus managerial or lower professional occupations was statistically significant (P < 0.04), and previous length of absence from work at baseline had borderline significance (P < 0.1). For change in EQ-5D, there was a statistically significant difference for men compared with women (P < 0.05), and a borderline significance for semi-skilled workers as against unskilled workers (P < 0.1).
Table 3 Mean change in PCS, MCS, EQ-5D and JCQ scores

PCS = physical component score; MCS = mental component score; JCQ = job content questionnaire.
Table 4 Effects of covariates on health score differences

PCS = physical component score; MCS = mental component score.
Discussion
Our primary aim was to compare return-to-work outcomes for two groups of sickness absentees: one group supported by their GP alone, and another by GP and a case-managed support service. Despite several attempts and a variety of approaches, including financial incentives, we were unable to engage GPs in sufficient numbers to reach recruitment levels in the control arm of the trial. The lack of a comparison group meant we were unable to say which type of support had the best return-to-work outcomes, although the majority of those receiving case-managed support were back at work within a month.
GPs play a pivotal role in sickness absentees returning to appropriate work, as highlighted in recent reviews of the working age population (DWP, 2008). Some authors believe that changes to the sickness certification system must take account of GP attitudes and beliefs, including attitudes to litigation and possible conflict with patients (Wynne-Jones et al., Reference Wynne-Jones, Mallen, Main and Dunn2010a). Sickness certification decisions taken by GPs have an impact on an individual's psychosocial, financial and workplace health. However, workplace health appears to be an area of practice where GPs report a lack of knowledge, confidence and training in handling work issues with patients (Roope et al., Reference Roope, Parker and Turner2009; Money et al., Reference Money, Hussey, Thorley, Turner and Agius2010). Changes to the system involve challenges for the GP, particularly in the areas of long-term worklessness and rehabilitation (Cohen et al., Reference Cohen, Marfell, Webb, Robling and Aylward2012). Our results support previous evidence that suggests that GPs may avoid research in this complex area because of such issues. It is unclear why the majority of GPs failed to engage with the control arm of the trial. The additional time required to recruit control patients into a research study during a sick note-related consultation, with no apparent benefit to the patient or GP, may also be a strong deterrent. Our previous research into work and sickness absence has found patients wary of research into their absence, fearing loss of confidentiality for example, despite reassurance (Shiels et al., Reference Shiels, Gabbay and Ford2004). Anecdotal evidence from other ongoing work also suggests that GPs sign ‘Fit Notes’ without asking patients what type of work they do.
The study design was unsuitable in terms of recruitment. Given recruitment difficulties, the likelihood of bias in the intervention sample cannot be ignored. However, the information we collected from the intervention group provided an insight into workplace health problems, health outcomes and return to work rates. We conducted 21 hypothesis tests on data from 29 patients across the three models, and thus inevitably there will be some significant associations simply by chance. Some of the significant P-values are only borderline significant even at the 10% level, and clearly the results presented are thus exploratory findings.
Age and length of sickness absence at baseline were significantly associated with increased rate of absence, and male unskilled workers had the highest absence rates. Presentees’ scores were unchanged at follow-up, and the small number of presentees in the study makes it impossible to draw conclusions from their data. Poor mental health was evident in baseline scores. Unlike earlier studies (DWP, 2008), although mental health scores were significantly improved at follow-up, the number of contacts with WHAs had no bearing on return-to-work outcomes. GPs tended to refer a certain type of patient for WHA support (typically with work-related mental health problems), which meant that the amount of stress attributed to the workplace in this study was higher than levels previously reported (DWP, 2008; NICE, 2010). It is unclear why GPs chose to refer ‘stressed’ patients over others with workplace health problems; GP workload implications in complex work stress consultations or increasing numbers with work-related common mental health problems (Wynne-Jones et al., Reference Wynne-Jones, Mallen, Main and Dunn2010b) may lead GPs to refer to WHA services in order to reduce consultation time. These patterns of risk factors for prolonged absence mirror previous research (Shiels et al., Reference Shiels, Gabbay and Ford2004).
Our study strongly suggests that a traditional RCT approach is not feasible to explore and compare the impact of GP and case-managed support for workplace sickness absence. Our small, uncontrolled sample suggests that there are important phenomena to explore further, including GPs’ role in workplace sickness absence certification. Current research is underway funded by the DWP and informed by findings from this feasibility study to explore the impact of Fit for Work Service Pilots on a comparable group of patients.
Acknowledgements
The authors acknowledge the contribution of all study participants to both phases of the research and thank the Health at Work case managers and GPs without whose input the study would not have been possible. The study was sponsored by Liverpool Primary Care Trust and had ethical approval from Liverpool (Adult) Research Ethics Committee Ref 08/H1005/77. Liverpool and Sefton Primary Care Trusts gave Research Management and Governance permission.