Background
General practitioners (GPs) have long held a role in cigarette cessation by providing advice and treatment to their patients (Zwar and Richmond, Reference Zwar and Richmond2006). A patient encounter offers the GP an opportunity to record cigarette smoking status and to provide brief interventions. The National Institute for Health and Care Excellence (NICE, 2006) recommend that GPs provide appropriate opportunistic advice on cigarette cessation, assess a patient’s commitment to quit, offer nicotine replacement therapy (NRT) or behavioural support, and provide self-help material or referral to National Health Service (NHS) Stop Smoking Services (SSS). Patients who receive behavioural support from NHS SSS are three times more likely to quit cigarettes compared with being seen at their GP practice (Dobbie et al., Reference Dobbie, Hiscock, Leonardi-Bee, Murray, Shahab, Aveyard, Coleman, McEwen, McRobbie, Purves and Bauld2015). Simple primary care measures such as NRT vouchers could encourage supported quit attempts in cigarette smokers (Watson et al., Reference Watson, Bullen, Clover, McRobbie, Parag and Walker2010).
Novel tobacco and non-tobacco products are becoming increasingly common in Western settings; in the United Kingdom, it is estimated that 12% of the adult population have tried waterpipe tobacco smoking (WTS), 1% are smokeless tobacco (ST) users, and 21% of smokers currently use electronic cigarettes (EC) (Grant et al., Reference Grant, Morrison and Dockrell2014; Beard et al., Reference Beard, West, Michie and Brown2016; Leon et al., Reference Leon, Lugo, Boffetta, Gilmore, Ross, Schuz, La Vecchia and Gallus2016).
WTS also known as shisha, hookah, and narghile, involves smoking flavoured tobacco, the smoke of which is bubbled through water prior to inhalation (Kotecha et al., Reference Kotecha, Jawad and Iliffe2016). Its harms are well documented; lung and cardiovascular disease, and carbon monoxide poisoning to list some (Maziak, Reference Maziak2015). There are low levels of WTS enquiry in UK general practice settings (Jawad et al., Reference Jawad, Hamilton, Millett, Albeyatti and Ananthavarathan2014; Mughal et al., Reference Mughal, Meki and Kassamali2014).
ST is the oral consumption of tobacco. It is commonly chewed and mixed with other ingredients such as areca nut, betal leaf, and lime, with a varying spectrum of harm (‘Snus’ in Norway versus ‘paan’ in India) (Critchley and Unal, Reference Critchley and Unal2003). ST is associated with oral cancers, dental disease, and cardiovascular disease (Critchley and Unal, Reference Critchley and Unal2003). NICE (2012) encourages GPs to ask about ST, inform patients of the harms, refer to specialist services if appropriate, and record outcomes in patient notes.
EC allow users to consume nicotine without the toxins in tobacco smoke (Britton, Reference Britton2016). The role of EC in smoking cessation has been rigorously debated. Recent research suggests a significant association between EC use and successful quitting and a 2016 Cochrane review highlighted that EC can aid smokers to stop in the long term, however, the long-term safety of EC remains unknown (Beard et al., Reference Beard, West, Michie and Brown2016; Hartmann-Boyce et al., Reference Hartmann-Boyce, McRobbie, Bullen, Begh, Stead and Hajek2016). The Royal College of General Practitioners (RCGP) recognise EC as safer than conventional cigarettes and encourage GPs to recommend EC to patients if other cessation methods have failed in conjunction with support from SSS (Roope, Reference Roope2016).
While WTS and ST are associated with adverse, cigarette-like health outcomes (Siddiqi et al., Reference Siddiqi, Shah, Abbas, Vidyasagaran, Jawad, Dogar and Sheikh2015; Waziry et al., Reference Waziry, Jawad, Ballout, Al Akel and Akl2016), EC are recommended as an appropriate cessation aid (Roope, Reference Roope2016). Yet, decisions around tobacco cessation can be confusing, with some evidence showing that users may consider WTS an appropriate cessation aid to cigarettes (Asfar et al., Reference Asfar, Weg, Maziak, Hammal, Eissenberg and Ward2008), and EC an inappropriate cessation aid to cigarettes (Rooke et al., Reference Rooke, Cunningham-Burley and Amos2016). A paucity of research explores the views and actions of GPs and training GPs in the United Kingdom towards tobacco cessation beyond traditional cigarettes, with little focus on WTS, ST, and EC which are rising in prevalence (Grant et al., Reference Grant, Morrison and Dockrell2014; Jawad et al., Reference Jawad, Hamilton, Millett, Albeyatti and Ananthavarathan2014; Beard et al., Reference Beard, West, Michie and Brown2016; Leon et al., Reference Leon, Lugo, Boffetta, Gilmore, Ross, Schuz, La Vecchia and Gallus2016). This study aimed to examine GP and GP trainee perceptions of tobacco and EC products and their attitudes and behaviours towards cessation.
Methods
Design, sample, and setting
A cross-sectional study of GPs and GP trainees in England was undertaken between January and May 2016. An electronic anonymous self-administered questionnaire designed from the literature was developed and piloted amongst a representative sample of five GPs in the West Midlands for relevance and acceptability. Questionnaire items were reworded and reordered following pilot. The questionnaire was disseminated nationally through RCGP e-bulletins, Solihull and Birmingham Cross-City Clinical Commissioning Group (CCGs) newsletters, Vocational Training Schemes, Health Education England (HEE) distribution lists, and on authors’ personal Twitter accounts.
Questionnaire and measures
The questionnaire consisted of 13 items. Six items gathered sociodemographic characteristics such as GP status (GP/GP trainee), years in clinical practice (five year increments from 0 to 40 years), region of clinical practice (17 UK deanery regions), sex, ethnic group (17 UK census ethnicities), and past-30-day tobacco use (Yes/No).
All remaining questions used five-point Likert scales. Three items enquired about awareness of tobacco products and consultation barriers. One enquired about the awareness of WTS and five ST products (paan, ghutka, betal quid, khaini, and zarda) with answers ranging from ‘Not at all aware’ to ‘Extremely aware’; and another enquired about four barriers (lack of knowledge, confidence, time, and information) to discussing WTS during a consultation with answers ranging from ‘Strongly disagree’ to ‘Strongly agree’.
Two items enquired about GP attitudes. One enquired about the harm perception of four products (cigarettes, WTS, ST, and EC) with answers ranging from ‘Very harmless’ to ‘Very harmful’, and an additional ‘I don’t know’ option; and another enquired about the suitability of five cessation aids (NRT, varenicline/bupropion, WTS, ST, and EC) for a patient finding it difficult to quit cigarettes.
Finally, two items enquired about GP behaviour. One enquired about whether users of four products (cigarettes, WTS, ST, and EC) would be given cessation advice during a consultation, with answers ranging from ‘Never’ to ‘Always’; and the other enquired about whether users of these same four products would be routinely referred to cessation services (NHS SSS or in-practice smoking clinics), with answers ranging from ‘Strongly disagree’ to ‘Strongly agree’.
Statistical analysis
Prior to analysis we removed observations from GPs based in Scotland (n=14) and Wales (n=6) (due to the low response), and one observation from a GP practising abroad. This left 312 complete observations from England for analysis. In 2014, there were 59 011 registered GPs and 10 795 GP trainees (General Medical Council, 2015). Due to small numbers we collapsed the variable ‘region’ into seven groups (London, West Midlands, East of England, Thames Valley, South West [Severn], East Midlands, and Other), the variable ‘years in clinical practice’ into three groups (less than five, five to ten, and more than 10), and the variable ‘ethnicity’ into four groups (White, South Asian, Arab, and Other). To simplify analysis, we dichotomised all response options to questions involving a Likert scale. The dichotomisation of Likert scales was based on Cronbach’s α scores, indicating the best dichotomisation permutation based on internal consistency.
We reported the frequency and percentages of all categorical data variables and compared between-product harm perception and GP cessation behaviour using χ 2 tests (against cigarettes only). We then constructed four logistic regression models (one for each of cigarettes, WTS, ST, and EC) to determine the correlates of giving cessation advice in a consultation. The correlates included GP status, sex, region, years of clinical practice, ethnicity, past-30-day tobacco use, and the harm perception towards that product. Correlates were eliminated in a backward stepwise approach set at P<0.05, and were presented as adjusted odds ratios with 95% confidence intervals. All P-values were adjusted for multiple comparisons using the false discovery rate method (Benjamini and Hochberg, Reference Benjamini and Hochberg1995).
We used Stata 13.0 (StataCorp) for all statistical analyses.
Findings
Sample characteristics
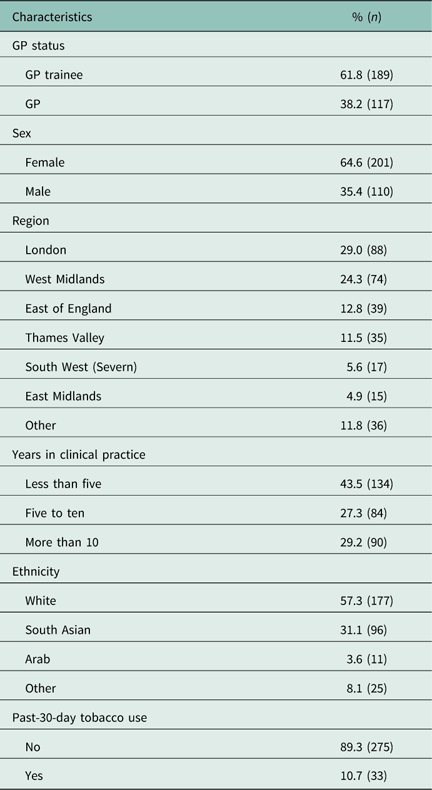
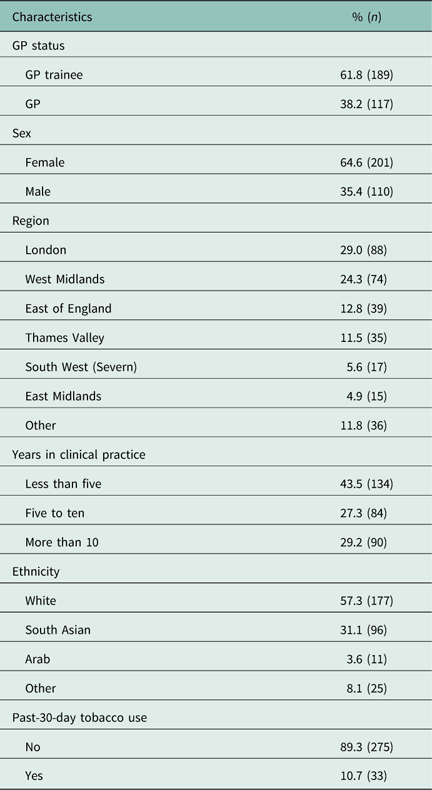
Table 1 shows the sample characteristics. In general, our sample consisted mainly of white (57.3%), female (64.6%), GP trainees with less than five years’ in clinical practice. Over half the sample (53.3%) were either from London or the West Midlands. About one in ten respondents (10.7%) were past-30-day tobacco users.
Awareness and consultation barriers
Awareness of WTS was reported by 62.5%. Barriers to discussing WTS in consultations included lack of information (76.3%), knowledge (62.8%), confidence (61.4%), and time (56.1%). Awareness of ST was lower: paan (32.0%), betel nut (23.5%), ghutka (10.4%), zarda (5.8%), and khaini (5.2%).
Attitudes: harm perception and cessation
Nearly all respondents reported cigarettes as harmful to health (96.8%), and this incrementally and significantly decreased to 82.0% for WTS, 68.3% for ST, and 35.0% for EC (P<0.001 for χ 2 comparisons for each product against cigarettes).
While 95.8% endorsed NRT as a cigarette cessation aid, this incrementally decreased to 71.4% for varenicline/bupropion, 33.8% for EC, 2.9% for ST, and 2.6% for WTS. Less than 2% (1.6%) endorsed none of these products as cigarette cessation aids.
Behaviour: cessation advice and referral
Nearly all respondents reported giving cessation advice to cigarette users during consultations (98.1%), and this incrementally and significantly declined to 33.7% for EC, 16.6% for WTS, and 11.8% for ST (P<0.001 for χ 2 comparisons for each product against cigarettes).
Over half (59.6%) reported routinely referring cigarette users to cessation services, and again this incrementally and significantly decreased to 9.7% for WTS, 5.2% for ST, and 4.9% for EC (P<0.001 for χ 2 comparisons for each product against cigarettes).
Table 2 shows correlates for clinicians giving cessation advice for four products by clinician characteristic. The odds of giving cessation advice to cigarette users were lower in past-30-day tobacco users (versus non-users). The odds of giving cessation advice to WTS users were higher in GPs (versus GP trainees) and those of South Asian (versus white) or Arab ethnicity (versus white). The odds of giving cessation advice to ST users were higher in GPs with over 10 years’ clinical practice (versus less than five years), and those of South Asian (versus white) and Arab ethnicity (versus white). The odds of giving cessation advice to EC users were higher in GPs (versus GP trainees), those who considered EC harmful to health (versus not harmful), and the odds were lower in those of South Asian ethnicity (versus white).
Table 2 Odds ratios of giving cessation advice by product and clinician characteristics
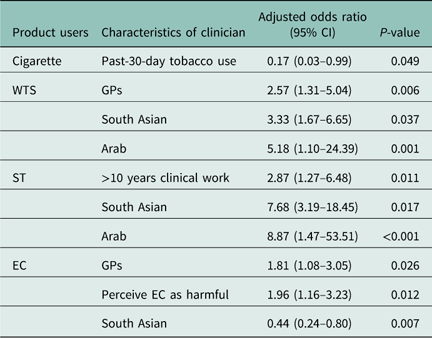
CI=confidence interval; WTS=waterpipe tobacco smoking; ST=smokeless tobacco; EC=electronic cigarette.
Discussion
Summary of findings
This cross-sectional study among 312 GP doctors in England showed that around two-thirds were aware of WTS but there were substantial barriers to discussing WTS in consultations including a lack of; information, knowledge, confidence, and time. ST awareness was generally low, although a third were aware of paan and a quarter of betal nut. Worryingly, GPs had lower harm perception, gave less cessation advice, and made less referrals for WTS and ST users compared to cigarettes. About a third thought EC were at least as harmful as cigarettes and only a third endorsed EC as an appropriate cessation aid. Variations in GP characteristics associated with cessation advice for each product included GPs of ethnic minorities and more senior GPs having higher odds of providing cessation advice for WTS and ST users.
WTS and ST are primarily used in patients from Arab and/or South Asian communities which can explain the overall low awareness, specifically for GPs who may not work within these communities (Siddiqi et al., Reference Siddiqi, Gupta, Prasad, Croucher and Sheikh2013). The attitudes and behaviours of GPs towards WTS, ST, and EC could be explained by a lack of knowledge and confidence on these products (Jawad et al., Reference Jawad, Hamilton, Millett, Albeyatti and Ananthavarathan2014; Hammal et al., Reference Hammal, Wild and Finegan2016). Ethnic minority GPs may be influenced by cultural experiences with ST and WTS and the experience gained through working more clinical years could explain the greater odds of providing cessation advice.
Strengths and limitations
To our knowledge this is the first study to measure GPs’ awareness, attitudes, and behaviours towards cessation across a multitude of tobacco and non-tobacco products. This gives us important insights to understand how and why certain GPs exhibit attitudes and behaviours to particular products, and provides a platform to explore these further in studies. Including GP trainees allows us to identify gaps in training and education and explore an inter-generational perspective towards cessation in primary care settings.
The main limitation is that this convenience sample is unlikely to be nationally representative and thus generalisable to the England GP population. Our recruitment methods, however, reached several regions in England aided by social media. Another limitation is social desirability bias, although we were unable to account for this in our study design. Finally, the questionnaire was not statistically validated and it is unclear whether measurement biases are present, however, we tried to mitigate this by pre-piloting our survey which helped improve its face and content validity.
Comparison with existing literature
In this study, harm perception towards WTS among GPs was better than that identified previously by a study among GPs in England, but the provision of cessation advice was lower (Jawad et al., Reference Jawad, Hamilton, Millett, Albeyatti and Ananthavarathan2014). This may be due to the non-standardisation of questions used to assess perceptions and behaviours to WTS, in addition to variation in sampling methods.
Comparing our findings to international ST studies is challenging due to the range of products. For example, Snus which is common in Sweden and Norway, is generally considered a less harmful form of tobacco use than south Asian ST (Ramström et al., Reference Ramström, Borland and Wikmans2016). Norwegian GPs who feel ST is less harmful than cigarette smoking recommend ST as a smoking cessation aid (Lund and Scheffels, Reference Lund and Scheffels2012). In India, where ST products are more likely to reflect those asked for in our survey, only a minority of physicians were shown to document a ST history (Panda et al., Reference Panda, Persai, Mathur and Sarkar2013).
More generally, two-thirds of GPs in Turkey do not feel discussing smoking cessation is effective and there are varied smoking cessation practices amongst GPs across Europe (Helgason and Lund, Reference Helgason and Lund2002; Barengo et al., Reference Barengo, Sandstrom, Jormanainen and Myllykangas2005; Gokirmak et al., Reference Gokirmak, Ozturk, Bircan and Akkaya2010). Discussions are felt to be too time consuming and ineffective (Vogt et al., Reference Vogt, Hall and Marteau2005). GPs want to protect the doctor–patient relationship and prefer to offer smoking cessation advice where patient presentations are smoking related or when the relationship between patient and doctor is felt to be robust (Coleman et al., Reference Coleman, Murphy and Cheater2000). We identified that nearly all (98%) provide cessation advice to cigarette users.
Since the inception of the UK NHS smoking cessation strategy the proportion of GPs deeming NRT to be a suitable cessation aid has risen from 77 to 96% identified in this study (McEwen et al., Reference McEwen, Akotia and West2001). McEwen et al. (Reference McEwen, West, Owen and Raw2005) identified in 2005 that 70% of GPs ‘regularly refer’ cigarette smokers to smoking cessation services in comparison to 60% in this study. Some primary care practitioners in America recommend the use of EC in cigarette cessation which interestingly mirrors the finding of a third of our respondents supporting the use of EC in cigarette cessation (Bascombe et al., Reference Bascombe, Scott, Ballard, Smith, Thompson and Berg2016).
GPs who use cigarettes give less tobacco cessation advice to their patients than GPs who do not smoke (53 versus 69%) (Pretti et al., Reference Pretti, Roncarolo, Bonfanti, Bettinelli, Invernizzi, Ceccarelli, Carreri and Tenconi2006). This resonates with our finding amongst GPs who have used tobacco in the past 30 days.
Conclusions (implications for research and practice)
We found low levels of cessation advice and referrals to cessation services, with substantial inter-product variation. A greater emphasis on tobacco cessation beyond cigarettes is needed in primary care.
Qualitative work exploring GP attitudes in depth would be important and may generate new hypotheses to explain the variations observed in this survey. Analysing general practice records for tobacco use status and cessation patterns would allow for longitudinal analysis, offering an insight into behaviours over time. This study has focused on GPs and further research is needed to understand the perspectives of the patient in general practice and other primary care workers.
To address the rising tide of WTS and ST, the harms of these products need greater visibility in general practice (Jawad et al., Reference Jawad, Choaie, Brose, Dogar, Grant, Jenkinson, McEwen, Millett and Shahab2016). An educational tool and patient decision aid for general practice can be made that can assist staff working in tobacco cessation to build knowledge and confidence enabling more constructive discussions with patients. The low awareness and perception of harm of ST is concerning, with the low awareness likely to be related to the perception of harm and cessation behaviours. We appreciate there are many guidelines for a GP to be familiar with in conjunction with workload pressures, however, we do feel especially amongst South Asian patients that ST should be enquired about (NICE, 2012; Torjesen, Reference Torjesen2012).
NHS SSS provide GPs with an opportunity to signpost patients for cessation treatment and we encourage GPs to utilise their local services for patients who use WTS, ST, and EC. Practices should revisit their new patient registration template to ensure tobacco status is asked and recorded. This provides an opportunity to provide cessation management. The RCGP GP Curriculum must include the growing use of different tobacco forms and EC and emphasise the need for training GPs to be competent in this area. It should not be overlooked that GPs may be tobacco users also and that support must be accessible, acceptable, and tailored to their needs. More needs to be done to highlight the role EC has in tobacco cessation with an element of caution on the long-term risks.
Acknowledgements
The authors would like to acknowledge Joanne Reeve, Lion Shahab, and Samuel Finnikin for providing comments on an early draft of the survey. The authors would like to thank the RCGP, HEE, Birmingham Cross-City CCG, and Solihull CCG for distributing the questionnaire electronically. The authors would also like to thank all the doctors who completed the questionnaire. F.M. is an NIHR In-Practice Fellow. The views expressed in this paper are those of the author and not necessarily those of the NHS, the NIHR, or the Department of Health and Social Care. The Public Health Policy Evaluation Unit at Imperial College London is supported by funding from the NIHR School of Public Health Research.
Financial Support
This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.
Conflicts of Interest
None.
Ethical Standards
Ethical approval was not sought but this research adhered to the ethical standards of the Helsinki Declaration of 1975, as revised in 2008.