In 1987 Stern et al (Reference Stern, Cottrell and Holmes1990) examined Asian and non-Asian referrals to the department of child psychiatry at the London Hospital. Bangladeshi referrals were found to be underrepresented with respect to the local population.
While 33% of school-aged children in Tower Hamlets in 1987 were Bangladeshi, they accounted for only 12% of referrals to the service. Ten years later, the proportion of school-aged children in Tower Hamlets of Bangladeshi ethnicity had increased from 33% to 52% (Education Strategy Group, 1997). However, we hypothesised that Bangladeshi children and families remained under-represented within the clinic population and that those who were referred, were less likely to remain engaged in treatment.
This study aims to examine and report upon any changes in patterns of referral and attendance over the intervening 10 year period.
Method
This study was a retrospective case note analysis of all referrals to the Child and Family Consultation Service at the Royal London Hospital during 1997. Data were collected by the three authors in a standardised way, recording the following demographic details: age, gender, ethnicity, postcode, referral source, presenting problem and ‘administrative outcome’. The final category was divided into non-attenders, early drop-outs (attended once only), late drop-outs (attended more than once but treatment unilaterally terminated by family), agreed termination and treatment ongoing (Reference Cottrell, Hill and WalkCottrell, et al 1998).
Data were analysed using χ2. Fisher's exact probability was used where sample size was small.
Results
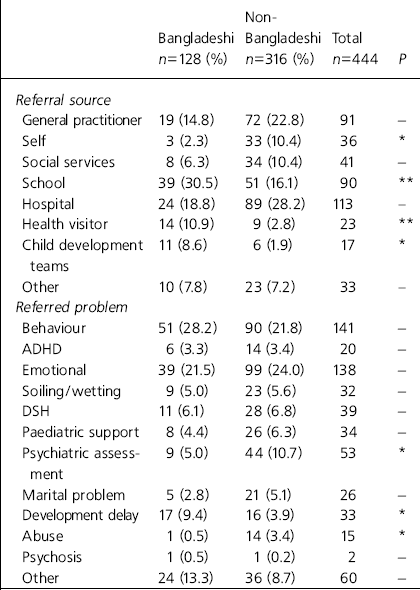
The results are summarised in Table 1. Of the 444 referred children, 128 (28.8%) were Bangladeshi and 316 (71.2%) were non-Bangladeshi. Two hundred and forty-three (54.7%) were male, 201 (45.3%) were female. There were no statistically significant differences between the two ethnic groups in either gender or age distribution.
Table 1. Referral information according to ethnicity
| Bangladeshi n=128 (%) | Non-Bangladeshi n=316 (%) | Total n=444 | P | |
|---|---|---|---|---|
| Referral source | ||||
| General practitioner | 19 (14.8) | 72 (22.8) | 91 | - |
| Self | 3 (2.3) | 33 (10.4) | 36 | * |
| Social services | 8 (6.3) | 34 (10.4) | 41 | - |
| School | 39 (30.5) | 51 (16.1) | 90 | ** |
| Hospital | 24 (18.8) | 89 (28.2) | 113 | - |
| Health visitor | 14 (10.9) | 9 (2.8) | 23 | ** |
| Child development teams | 11 (8.6) | 6 (1.9) | 17 | * |
| Other | 10 (7.8) | 23 (7.2) | 33 | - |
| Referred problem | ||||
| Behaviour | 51 (28.2) | 90 (21.8) | 141 | - |
| ADHD | 6 (3.3) | 14 (3.4) | 20 | - |
| Emotional | 39 (21.5) | 99 (24.0) | 138 | - |
| Soiling/wetting | 9 (5.0) | 23 (5.6) | 32 | - |
| DSH | 11 (6.1) | 28 (6.8) | 39 | - |
| Paediatric support | 8 (4.4) | 26 (6.3) | 34 | - |
| Psychiatric assessment | 9 (5.0) | 44 (10.7) | 53 | * |
| Marital problem | 5 (2.8) | 21 (5.1) | 26 | - |
| Development delay | 17 (9.4) | 16 (3.9) | 33 | * |
| Abuse | 1 (0.5) | 14 (3.4) | 15 | * |
| Psychosis | 1 (0.5) | 1 (0.2) | 2 | - |
| Other | 24 (13.3) | 36 (8.7) | 60 | - |
Of the referred children, 64 (14.4%) lived outside Tower Hamlets. Of these, only 2 (3%) children were Bangladeshi. Excluding these 64 children, Bangladeshi children accounted for 33.2% of Tower Hamlets' referrals.
Referral source was divided into eight categories (Table 1). Analyses of each referral source showed that significantly fewer Bangladeshi families referred themselves to the service, while significantly more Bangladeshi children and families were referred to the service by schools, health visitors and the child development team (CDT). The latter two sources showed a reversal in the expected trend by referring more Bangladeshi than non-Bangladeshi cases.
Referrals to the service were categorised at the point of referral into one of 39 ‘presenting problems’. These were contracted into 12 problems for this study (Table 1). The ethnicity differences in referral rates for psychiatric assessments were accounted for by extra-contractural referrals and for development delay by CDT referrals.
Of the 44 referred cases, 407 were offered an initial appointment. Of these, 293 families (69.5%) attended their first appointment, 25 (6.1%) declined an appointment and 99 (24.3%) did not attend. Of these, 61 families were offered another appointment, of whom 34 attended. The total attrition rate was 139/382 (36.4%), while agreed discharges/ongoing treatment accounted for 239/382 (62.6%).
The 407 cases offered an initial appointment were analysed for ethnicity, revealing significant differences in patterns of response. In the Bangladeshi sample 9 (7.7%) declined the appointment, 71 (60.1%) attended and 37 (31.6%) did not attend, while in the non-Bangladeshi group 16 (5.5%) declined the appointment, 212 (73.1%) attended and 62 (21.4%) did not attend (P<0.05). There were no differences between the ethnic groups in levels of ‘early’ or ‘late’ drop-out.
Referral source did have some influence on subsequent attendance rates at a first appointment. While 81/101 (80.2%) children referred by the hospital were seen at a first appointment, presumably mostly as in-patients, only eight out of 19 (42.1%) of those referred by health visitors attended (P<0.05). Of the 86 children referred to the service by school, 55 (62.5%) attended their first appointment. However, when these figures are analysed for ethnicity, it can be seen that only 22 of the 38 (57.9%) referred Bangladeshi families attended their first appointment compared to 33/48 (68.8%) non-Bangladeshi families (P<0.05). No other statistically significant differences were found.
Discussion
Over the 10-year period in question, Bangladeshi referrals increased from 12% in 1987 to 29% in 1997. Examining local referrals alone, in 1997 Bangladeshi families now made up over 33% of total cases, although still less than the expected proportion.
Possible reasons for the increase in Bangladeshi cases include attempts by the service to be more accessible and acceptable to the local population. The name was changed from the Department of Child Psychiatry to the Child & Family Consultation Service in an effort to reduce the perceived stigma of attending the service. Hospital signs have been copied into Bengali to help guide the public. Between 1987 and 1997 various Bangladeshi professionals have been part of the child mental health team, as well as Sylheti-speaking workers to help with interpreting and cultural advice (Sylhet being the province of Bangladesh from where the majority of the local Asian population originated). In addition, the local Bangladeshi people may have become more integrated into mainstream British culture with the passage of time.
Nevertheless, despite some apparent success of the department in attracting Bangladeshi referrals, with over 50% of children in the borough, this section of the population remains underrepresented. Despite evidence of increased social disadvantage when compared to indigenous populations, some studies have suggested that Asian families may experience a lower prevalence of child psychiatric disorder requiring professional help (Reference Butler and GoldingButler & Golding, 1986, Reference Hackett, Hackett and TaylorHackett et al, 1991). Alternatively, perhaps more work needs to be done to break down cultural barriers to accessing good child mental health care.
Stern et al (Reference Stern, Cottrell and Holmes1990) found no differences in referral source with regard to ethnicity, whereas several differences were apparent in our study. Schools, health visitors and the CDT referred a higher proportion of Bangladeshi children than most other referrers, for which there may be a number of possible explanations. Bangladeshi families may be actively seeking referral to the child mental health service through a source familiar to them. However, the poor attendance rate for the first appointment among Bangladeshi children referred by schools suggests that this is not the case. These referrers may be correctly identifying a level of need irrespective of ethnicity or highlighting a difference in the perception of what constitutes a disorder between themselves and parents.
CDT referrals show good uptake of first appointments irrespective of ethnicity. Bangladeshi children with development delay are usually allocated a ‘parent advisor’ from their own culture to help their parents with the difficulties of coping with a child with disabilities and to support the families in their dealings with professionals. This additional factor may be crucial in helping these families to understand the reasons for referral to child mental health and to support attendance.
As well as making up a smaller overall proportion of referrals than their population size would indicate, Bangladeshi families are less likely to attend their initial appointment. In any consultation where the individual has to initiate contact many factors may influence access, including previous experience, education and perception of the service (Reference Hillier, Loshak and RahmanHillier et al, 1994). These factors are likely to be amplified by cultural and religious differences in health-seeking behaviour.
When taken alongside the lower self-referral rate among the Bangladeshi population, these findings appear to suggest that many Bangladeshi families are less able or less willing to seek help from a child mental health service. Of the very few Bangladeshi families that did self-refer, all attended their first appointment.
Early and late drop-out rates showed no ethnic differences, indicating that when families did make it to their first appointment, likelihood of engaging in on-going work was unaffected by language and cultural differences.
Communication between referrer, family and our service is a crucial factor in aiding access to health services (Reference ChanChan, 1998). Liaison with the local Bangladeshi community reveals a widespread lack of awareness about the role and function of a child mental health service.
Possible solutions include distributing information leaflets written in Bengali about our service within the wider community. Information for our referrers to explain the service and how to access it would help reduce the number of inappropriate referrals. Particular emphasis could be given to specific professional groups such as health visitors or teachers to help them identify appropriate families to refer and prepare them for an initial appointment. Contacting families prior to an appointment to discuss the referral and help initiate engagement might help increase attendance at a subsequent appointment (Reference GatradGatrad, 2000). Ensuring an adequate mix of professionals from different ethnicities to reflect the local population has not always been easy to achieve. Recruiting trainees into the professions from the local community might help address this.
We hope that the implementation of some or all of these measures will ensure that by the end of the next decade, ethnicity is no longer a major obstacle to accessing a child mental health service.




eLetters
No eLetters have been published for this article.