Over the past few years, there has been a ‘root-and-branch review’ (Scoping Study Committee, 1999) of mental health legislation in England and Wales. In spite of the involvement of a large number of interested parties, many with strongly contrasting points of view, the process has resulted in a white paper (i.e. proposal for legislation) which embodies clear and consistent principles — albeit ones which, taken together, are substantially different from those of the present Mental Health Act and which do not seem to please everyone. A thorough critique of the proposals is beyond the scope of this paper, and can be found elsewhere (e.g. Royal College of Psychiatrists, 2001; Reference SzmuklerSzmukler, 2001; Reference ZigmondZigmond, 2001; Mind, 2001). However, in broad terms, the white paper represents a shift away from the Percy Commission's model of compulsory treatment being given only in the best interests of the individual patient and only as a last resort (Percy Commission, 1957) towards a model where protecting the public from the perceived dangerousness of patients assumes equal importance with providing care in the patient's best interests. The white paper, while carefully worded in an attempt to avoid conflict with the Human Rights Act 1998, would seem to permit a massive increase in the use of compulsory powers, by widening the criteria for detention, by effectively establishing community treatment orders, and by delegating the power to detain, not to psychiatrists (with their emphasis on the best interests of the individual patient) but to new quasi-judicial mental health tribunals (which may well develop a broader view of their responsibilities).
This paper makes the assumption that part 1 of the white paper will be enacted without any substantial alteration and that the use of compulsory powers will, at the very least, not be reduced. We have not considered the resource implications of part 2 of the white paper, relating to high risk patients and ‘dangerous severe personality disorder’. The Mental Health Act 1983 included more bureaucratic checks and balances than its 1959 predecessor, and required a significant increase in resources. Because there are similar fears about the white paper (Royal College of Psychiatrists, 2001), we have tried to evaluate these concerns in a formal way, despite the lack of clarity for some of the details in the proposals. We are unaware of the publication of any other structured attempt to do this.
The study
This audit set out to calculate the amount of time professionals had spent complying with the requirements of the current Mental Health Act (England & Wales) in a given setting and during a given period. It was then estimated how much time would have been required, had a new Act based on the white paper been in force. For practical reasons, and because a forensic psychiatric unit concentrates on detained patients, the Oxford Clinic was chosen for the study. This is a 30-bed, purpose-built, medium-secure forensic psychiatric unit with a catchment area (Oxfordshire and Berkshire) of approximately 1.5 million people. All patients in the unit are detained under the Mental Health Act, and the usual length of stay is 18-24 months. This is typical for medium-secure units, as compared with an average length of stay of nearly 8 years for the three English high-security hospitals. All 54 patients admitted to the unit in the 18 months prior to May 2001 were identified, around two-thirds of whom were still in-patients. The full medical notes for all these patients were obtained and scrutinised by Sean Whyte, anonymously recording every ‘statutory process’. This was administrative work, carried out by a professional, which related directly to detention under the Act, over and above work which would have been done as a matter of course during the clinical care of the patient. Detention (‘section’) papers, photocopies, letters and clear descriptions in notes were all accepted as evidence of statutory processes.
Separately, the average times required for each of the statutory processes were estimated after consultation with a selected group of colleagues from the two main professional disciplines relevant to the Act (psychiatrists and social workers). Between them, the chosen colleagues had experience of the different sections and parts of the Act, and of the different roles which could be played (e.g. responsible medical officer (RMO), second opinion approved doctor (SOAD) etc.). The cost of each process was estimated using the hourly rates at the mid-point of the salary scales for each of the professionals concerned or the relevant fees, where paid.
Finally, both authors jointly considered the most probable way that each of the patients in the audit would have been dealt with, had a new Act based on the white paper been in force; the figures were then recalculated on this basis. Box 1 illustrates how these calculations were made in the case of one individual patient.
Box 1 Calculations for one individual patient
| Events | Statutory processes (1983 Act) | Time | Probable equivalent under new Act | Time |
|---|---|---|---|---|
| Seen in prison by consultant psychiatrist; transfer to hospital recommended | Section 38 assessment by section 12-approved doctor | 2 hours | Report proposing remand for assessment | 2 hours |
| Convicted of ABH and criminal damage; court makes interim hospital order (section 38) | Section 38 assessment by second doctor | 2 hours | ||
| Transferred to medium-secure hospital | Second doctor later concurs that care and treatment order may be appropriate | 1 hour | ||
| Period of assessment in hospital | RMO and a colleague both make reports recommending a hospital order (section 37) | 2 hours each | Clinical supervisor makes a report recommending a care and treatment order | 3 hours |
| Patient refuses consent to long-term anti-psychotic medication | Second opinion doctor (SOAD) reviews patient and completes form 39 | 2¼ hours | Independent doctor reviews patient and completes consent-to-treatment form | 2¼ hours |
| Hospital reviews RMO's authority to detain patient | RMO and social worker write reports for and attend managers' meeting | 1½ hours for RMO, 8 hours for social worker | No equivalent — managers' meetings abolished | |
| Hospital order renewed | RMO completes section 37 renewal form | 3 hours | Clinical supervisor applies to mental health tribunal for extension of care and treatment order, after receiving reports from team | 2 hours (plus 1 hour by colleagues) |
| Independent doctor reviews patient and reports to tribunal | 2¼ hours | |||
| Patient appeals against, or requests review of, detention | RMO and social worker write reports for and attend mental health review tribunal | 2¼ hours for RMO, 8 hours for social worker | Clinical supervisor writes report for and attends mental health tribunal, after receiving reports from team | 2½ hours (plus 8 hours by social worker) |
| Totals | RMO | 8¾ hours | Clinical supervisor | 7½ hours |
| Other psychiatrists | 6 hours | Other psychiatrists | 4 hours | |
| Social workers | 16 hours | Social workers | 8 hours | |
| SOAD | 2¼ hours | Independent doctors | 4½ hours |
Findings
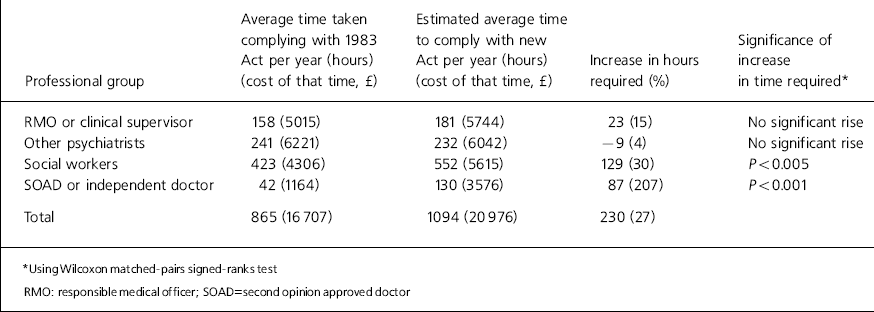
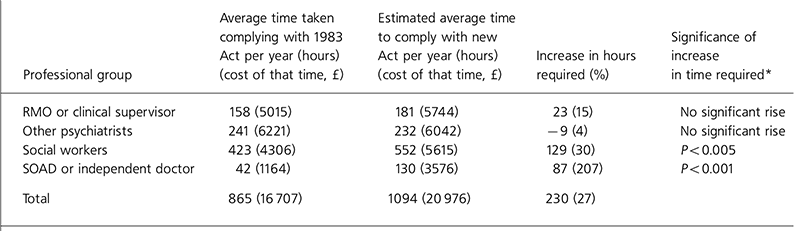
The main results of the audit are summarised in Table 1. The key finding is that the audit predicts a substantial rise (27% overall) in the amount of time professionals will have to spend to comply with the requirements of a new Act, but that this rise will only be significant for social workers and for independent doctors, working on behalf of the mental health tribunal (MHT).
Table 1. Difference in time taken to comply with new Act
| Professional group | Average time taken complying with 1983 Act per year (hours) (cost of that time, £) | Estimated average time to comply with new Act per year (hours) (cost of that time, £) | Increase in hours required (%) | Significance of increase in time required* |
|---|---|---|---|---|
| RMO or clinical supervisor | 158 (5015) | 181 (5744) | 23 (15) | No significant rise |
| Other psychiatrists | 241 (6221) | 232 (6042) | -9 (4) | No significant rise |
| Social workers | 423 (4306) | 552 (5615) | 129 (30) | P<0.005 |
| SOAD or independent doctor | 42 (1164) | 130 (3576) | 87 (207) | P<0.001 |
| Total | 865 (16 707) | 1094 (20 976) | 230 (27) |
We predict that social workers or, in some cases, their equivalent under a new Act, involved in the area included in the study will spend an extra 129 hours a year (a 30% increase in time required) complying with the requirements of a new Act. This is principally because they will need to contribute to the full care plans and reports demanded by more frequent MHTs, although this will be offset somewhat by the abolition of managers' meetings.
Even more significant is the prediction that the time required by independent doctors (similar to SOADs) who will be employed by the new MHTs will be tripled. They will have to spend a considerable time assessing patients and writing reports in advance of each MHT meeting. This is an entirely new function, distinct from the ‘medical member’ of the current mental health review tribunals, who does not write a formal report and is to be separately replaced by a third MHT member, and distinct also from the right of the patient to employ their own independent psychiatrist.
Comment
There are many limitations to this study, not least the biased nature of the in-patient forensic psychiatric sample and the necessarily subjective nature of our estimates of the times required to comply with a new Act. Our estimates make a number of assumptions which may well turn out to be incorrect. These include assuming that the white paper will be enacted unchanged, that working practices will not alter other than as required by the Act and that the frequency of use of compulsory powers of detention will not change.
Notwithstanding these limitations, however, our central findings are likely to hold true, that social workers and independent doctors will be required to spend substantially more time complying with a new Act, whereas psychiatrists responsible for the clinical care of patients will not be significantly affected. This is particularly true for professionals working with patients from medium-secure units. We believe that these findings are also likely to apply to the many patients in other forensic psychiatric settings.
Our findings do not apply directly to general adult psychiatric services, where compulsory powers are used less frequently and different parts of the Act are employed. However, in a similar way, where care and treatment orders are used, social workers and independent doctors are still likely to need a lot more time than they do at present.
The implication of these findings for policymakers, if they are even partly true, is that the implementation of a new Act on the lines described in the white paper will require extra resources, both financial (to pay for the additional social work and independent medical time) and human. Even without these additional pressures, there are already worrying shortages of SOADs and independent doctors available to the mental health review tribunal. Unless this resource issue is tackled before the new legislation is enacted, patient clinical care is likely to be adversely affected.
Declaration of interest
None.
Acknowledgements
We thank Lyn Taylor, Kathy Smith and the staff of the Littlemore Medical Records Department who assisted with locating notes, and our psychiatric and social work colleagues who helped us estimate times.





eLetters
No eLetters have been published for this article.