The assessment of growth in children is important for monitoring health status, identifying deviations from normality and determining the effectiveness of interventions(1). The significance of timely detection of poor growth in early life resides in its association with adverse functional consequences, including poor cognition and educational performance, low adult wages, lost productivity and, when accompanied by excessive weight gain later in childhood, increased risk of nutrition-related chronic diseases(Reference Victora, Adair and Fall2).
In 2004, we reported on child growth monitoring practices worldwide(Reference de Onis, Wijnhoven and Onyango3) in preparation for the construction of the WHO Child Growth Standards (hereafter referred to as the ‘WHO standards’). Results of a global survey conducted in 178 countries on the use and interpretation of growth charts in national programmes showed that growth charts are universally used in paediatric care. Over half of the countries relied on the weight-for-age indicator alone, two-thirds used the National Center for Health Statistics/WHO (NCHS/WHO) reference, and 63 % of charts classified child growth based on percentiles. Reported problems with the use of growth charts were both conceptual and practical(Reference de Onis, Wijnhoven and Onyango3).
Following the launch of the WHO standards in April 2006(4, 5), countries could choose to adopt the new standards and replace existing growth charts. Change implied a far-reaching shift in the way child growth is conceptualized as the WHO standards depict how children should grow, on average, in all countries, when properly fed and cared for, rather than merely describing how they grew at a particular time and place(4). Five years after the release of the WHO standards, we conducted a follow-up survey to document their worldwide implementation and describe the changes in child growth monitoring practices that have occurred since our first report.
Methods
A questionnaire on implementation of the WHO standards was sent to national health authorities in 219 countries and territories through the WHO regional and country offices. The questionnaire was developed centrally and pre-tested for comprehensibility with nutrition advisers based in the six WHO regions. For clarity and to improve responsiveness, all questions had pre-coded answers and were kept as short as possible. The original English text was translated into French and Spanish, and the translated versions were checked for accuracy by native speakers of these languages with expertise in child growth assessment and monitoring. The questionnaire was accompanied by instructions for completing it and a cover message explaining the survey's objectives. In addition, countries and territories that had already adopted the WHO standards were requested to send samples of their new growth charts or new child health records. Ministry of Health technical staff members responsible for national maternal and child health programmes were asked to complete the questionnaire or forward it for response to a relevant national institution (e.g. the Centers for Disease Control and Prevention (CDC) in the USA) or the national paediatric association. Whenever clarifications were needed, we interacted with national technical staff to verify unclear responses.
The survey was conducted from November 2009 to April 2011. Information was collected on: the status of adoption and the main reasons for non-adoption in case of a negative response; the year of adoption; the anthropometric indicators adopted (weight-for-age (WFA), length/height-for-age (LHFA), weight-for-length/height (WFLH), BMI-for-age (BMIFA), head circumference-for-age (HC), mid upper-arm circumference-for-age (MUAC), subscapular skinfold-for-age (SS) and triceps skinfold-for-age (TS)); the age range covered by each indicator; whether or not the charts were sex-specific; if the indicator was newly introduced; the growth reference the WHO standards replaced (e.g. NCHS/WHO, CDC 2000, Tanner, Harvard, national or local reference); the classification system applied (i.e. Z-scores or percentiles); and what steps had been taken to roll out the standards. Respondents also reported on the type of information included on the child growth charts and on the main impediments to implementing the new standards once adopted. Countries also provided samples of new child health records/booklets.
The English version of the questionnaire was designed as a pdf interactive form using Adobe Acrobat 7·0 Professional (version 7·1·0; Adobe Systems Incorporated), which allowed responses to be submitted electronically in xml (EXtensible Markup Language) format. These submissions were checked for consistency and incorporated directly into the master file (in Microsoft Excel format). The French and Spanish versions of the questionnaire were distributed in a Microsoft Word format that could be completed in soft or hard copy. Data from questionnaires that were returned in non-xml format (e.g. by fax, scan or courier) were keyed into the English interactive pdf template, validated and then exported via xml to the Microsoft Excel master file. Data were analysed using S-Plus (TIBCO S-Plus 8·2; TIBCO Software AG).
The WHO classification system was used to group the countries into geographical regions: AFR, African Region; AMR, Region of the Americas (North America, Latin America and the Caribbean); EMR, Eastern Mediterranean Region; EUR, European Region (Europe and Central Asia); SEAR, South-East Asia Region; and WPR, Western Pacific Region. The list of countries included in each of the WHO regions is available at http://www.who.int/about/structure/en/index.html.
Results
Of the 219 countries and territories contacted, 180 (82 %) responded to the questionnaire. The countries and territories that did not send responses represent only 0·65 % of the world's under-5 population as they are mainly small islands in the Caribbean and the Pacific or European countries with small populations (e.g. Andorra, Liechtenstein, Monaco, San Marino). Of the responding countries, 125 had adopted the WHO standards, twenty-five were considering their adoption and thirty had not adopted them; representing, respectively, 75 %, 17 % and 7 % of the world's under-5 population. Table 1 shows adoption status by geographical region. The countries that responded as not having adopted the standards by April 2011 were mainly in the European region (n 14), followed by Africa (n 7), the Western Pacific (n 5) and three in the Americas (Fig. 1). Only one country in the South-East Asian region had not adopted them. Preference for local references was the main reason given for non-adoption: 13/14 countries in EUR, 4/5 in WPR, all three in AMR as well as the one country in SEAR. In AFR the two main reasons for non-adoption were lack of resources and the recent reprinting of charts in current use.
Table 1 Coverage of the survey and adoption status of the WHO Child Growth Standards by geographical region (April 2011)
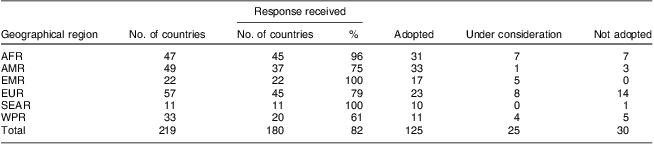
AFR, African Region; AMR, Region of the Americas (North America, Latin America and the Caribbean); EMR, Eastern Mediterranean Region; EUR, European Region (Europe and Central Asia); SEAR, South-East Asia Region; WPR, Western Pacific Region.

Fig. 1 Worldwide implementation of the WHO Child Growth Standards (April 2011)
Table 2 presents the anthropometric indicators used for assessing growth based on the WHO standards. WFA was adopted almost universally, with only twelve of the 125 countries not adopting this indicator. LHFA was also adopted by a large number of countries (n 104), as was WFLH (n 88). BMIFA and HC were adopted by fifty and fifty-seven countries, respectively, mainly in the AMR and EUR regions. Many countries reported using the opportunity of implementing the WHO standards to introduce the monitoring of new indicators (e.g. forty-two countries introduced LHFA, thirty-eight WFLH, thirty-six BMIFA and twenty introduced HC). The other indicators (MUAC, TS and SS) were seldom adopted.
Table 2 Anthropometric indicators used in monitoring child growth based on the WHO Child Growth Standards by geographical region (April 2011)
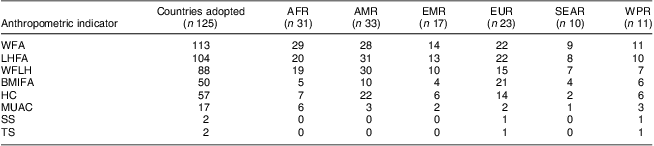
AFR, African Region; AMR, Region of the Americas (North America, Latin America and the Caribbean); EMR, Eastern Mediterranean Region; EUR, European Region (Europe and Central Asia); SEAR, South-East Asia Region; WPR, Western Pacific Region; WFA, weight-for-age; LHFA, length/height-for-age; WFLH, weight-for-length/height; BMIFA, BMI-for-age; HC, head circumference-for-age; MUAC, mid upper-arm circumference-for-age; SS, subscapular skinfold-for-age; TS, triceps skinfold-for-age.
The great majority of countries (n 121, 97 %) adopting the WHO standards chose to use sex-specific charts, that is separate charts for boys and girls. Most countries adopted the full age range from birth to 60 months, with only a few exceptions that opted for birth to 24 months (one country) or 2 weeks to 4 years (two countries). On the growth reference in use prior to adoption of the WHO standards, eighty-six countries reported using the NCHS/WHO reference, twenty used a local reference, fourteen used the CDC 2000 growth charts, and a few countries used the Harvard or the Tanner standards. Seven countries were unable to identify the reference or standard in use prior to the adoption of the WHO standards. A few countries had been using more than one reference (i.e. different reference populations for different anthropometric indicators or in primary v. tertiary health-care facilities).
On the classification system selected by countries adopting the WHO standards, eighty-four (67 %) countries opted for the Z-score classification system while twenty-eight (22 %) preferred to use percentiles. The remaining countries reported using both classification systems for at least some of the anthropometric indicators.
Activities undertaken by countries as part of their implementation of the WHO standards are presented in Table 3. The great majority of adopting countries (n 104, 83 %) redesigned their child health records to include the new charts and update recommendations on infant feeding, immunization and other health messages. As many as ninety-four (75 %) countries reported having formed a pool of national trainers that were cascading the training of the health workforce on the application of the WHO standards in their respective regions and districts. In addition, many countries (n 80, 64 %) had incorporated the new standards into pre-service training for family doctors, clinical officers, nurses and other health personnel. Other activities ranged from incorporating the standards into computerized information systems, to providing new or additional supplies of anthropometric equipment, to mobilizing resources to support the roll-out of the growth standards. The challenges encountered to the implementation process after official adoption of the standards are summarized in Table 4.
Table 3 Summary of activities undertaken as part of the implementation of the WHO Child Growth Standards (April 2011)

Table 4 Challenges in the implementation of the WHO Child Growth Standards after adoption by geographical region
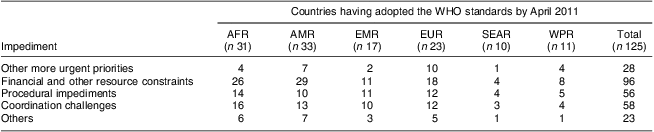
AFR, African Region, AMR, Region of the Americas (North America, Latin America and the Caribbean), EMR, Eastern Mediterranean Region, EUR, European Region (Europe and Central Asia), SEAR, South-East Asia Region, WPR, Western Pacific Region.
Discussion
In 2006 the WHO launched new growth standards for children irrespective of ethnicity, socio-economic status and feeding mode. By April 2011, at least 125 countries, representing 75 % of the world's under-5 population, had adopted the standards and were at varying stages of their implementation. It is very likely that some of the countries that were still considering implementing the standards when the survey was closed will have adopted them by the time the present paper is published.
In adopting the new standards many countries switched from using only WFA to using multiple indicators to better characterize growth patterns. Compared with an earlier report of growth monitoring practices(Reference de Onis, Wijnhoven and Onyango3), there has been a significant rise in the use of LHFA (from fifty-nine countries in 2000 to 104 in 2011). That figure is likely to continue to increase given the importance of monitoring WFA during the first year of life, and thereafter monitoring height in addition to weight, because faltering patterns are clearly different for LHFA and WFA(Reference Victora, de Onis and Hallal6) and short stature (or stunting) is associated with negative long-term outcomes(Reference Victora, Adair and Fall2, Reference de Onis, Blössner and Borghi7).
Similarly, many countries have introduced the indicator WFLH, which is essential to assessing severe acute malnutrition (i.e. wasting) as well as overweight and obesity. As many as thirty-six countries also introduced BMIFA, another important indicator for monitoring the growing epidemic of childhood obesity. In addition, BMIFA provides continuity with the monitoring of overweight and obesity in the 5–19 age range(Reference de Onis, Onyango and Borghi8). It is worth noting that in pre-school children, because WFLH and BMIFA provide similar information(Reference de Onis, Blössner and Borghi9), there is no need to monitor both indicators.
Another improvement relates to the use of separate charts for boys and girls. Most countries that in the earlier survey(Reference de Onis, Wijnhoven and Onyango3) reported using combined charts, have opted to use separate charts for boys and girls. Only four countries reported continued use of sexes-combined charts, mainly because of printing costs.
Compared with the previous report(Reference de Onis, Wijnhoven and Onyango3) many countries have switched from the percentile or per cent-of-median system to use the Z-score system for nutritional status classification. Z-scores are preferred because they permit clinical tracking of patients whose anthropometric classification lies beyond the measurable limits of the percentile range, as happens in the case of severely undernourished or obese children. Occasionally, countries report using both systems depending on the purpose, e.g. percentile charts for clinical use and Z-scores for public health purposes. With only a few exceptions, countries reported using the WHO charts for the age range birth to 5 years, and several (n 16) also have adopted the WHO 2007 growth reference for school-aged children and adolescents to monitor the nutritional status of children aged 5 to 19 years(Reference de Onis, Onyango and Borghi8).
The implementation of the WHO standards has taken different pathways depending on national health systems and decision-making processes. In almost all cases, the standards have been adopted nationwide. However, for countries with decentralized systems like Australia, Belgium and Spain, some parts of the country have adopted the WHO standards while others continue to use previous charts. Generally, most countries with decentralized administrations decided to adopt the WHO standards nationally, thus harmonizing the assessment of child growth in the country.
The scrutiny that the WHO standards have undergone is without precedent in the history of developing and applying growth assessment tools, whether national or international. Governments set up committees(10–12) to scrutinize the new standards before deciding to adopt them and professional groups that use anthropometric indicators conducted thorough examination of the standards. Through this process concerns were raised(13–Reference Binns and Lee16) and strengths were noted(Reference Dale, Grais and Minetti17–Reference Maalouf-Manasseh, Metallinos-Katsaras and Dewey27). The detailed evaluation made it possible to quantify the impact of the new standards on estimates of prevalence of malnutrition(Reference Black, Allen and Bhutta28–Reference Nuruddin, Lim and Hadden34) and their implications for child health programmes(35–Reference Ramachandran and Gopalan58).
Rolling out new growth charts is a complex task affecting all levels of a national health system. It concerns not only clinicians and health practitioners but also nutritionists, dietitians, public health specialists, child and health advocates, parents/caregivers and researchers. A great deal of coordination is necessary among all these stakeholders to ensure a smooth implementation. Many countries have redesigned their child health records, upgraded their anthropometric equipment, and retrained health staff to incorporate the WHO standards into their work. The WHO standards have also been incorporated into pre-service training programmes for medical and nursing professionals in several countries. Some countries have used the opportunity of switching to the new standards to raise awareness of the importance of child growth monitoring and redesign their surveillance systems to enhance decision making. Each aspect has required a considerable effort to implement and called for a reallocation of resources.
The introduction of new indicators such as BMIFA or length/height-based indicators posed considerable practical challenges with potential for measurement error and misclassification of children. A large-scale training programme was set in place by WHO, in coordination with UNICEF, that resulted in a network of facilitators to support training and other technical aspects of the standards’ implementation at regional and country level. The training package(59) emphasizes the importance of accurate measurement, plotting and interpretation for the correct identification of growth problems. If a child has a growth problem or trend towards a growth problem, the causes should be determined to take action to address them. Growth assessments that are not supported by appropriate response actions to prevent and treat excessive or inadequate growth are not effective in improving child health.
The implementation of the growth standards at country level required resources to design and produce new child health records, print large quantities of the new charts, buy anthropometric equipment (e.g. weighing scales) or produce them locally (i.e. height boards), translate documentation and tools (e.g. the training materials), and conduct national training workshops. Resource constraints (e.g. under-staffing in primary health-care facilities and shortage of equipment) have been an important bottleneck. UNICEF and other key partners played significant roles in supporting the standards’ implementation but there continues to be a need for support since significant costs are involved in the mass procurement of anthropometric equipment, in printing new charts, training health personnel, and especially in developing or strengthening programmes to deal with the growth problems identified through the application of the standards.
Acknowledgements
The work was supported by WHO and the Bill & Melinda Gates Foundation. The authors are WHO staff members. The authors alone are responsible for the views expressed in this publication and they do not necessarily represent the decisions or policies of the WHO. No author had a personal or financial conflict of interest. M.d.O. conceptualized the paper, guided the analyses and wrote the first draft of the paper. A.O. and A.S. developed the questionnaire and conducted the survey. E.B. analysed the data and wrote up the methods. M.B. and C.L. participated in the implementation of the growth standards. All authors participated in the interpretation of results, preparation of the manuscript and approved its final version. The authors are grateful to UNICEF, the governments of WHO Member States, non-governmental organizations and the numerous individuals who have participated in the roll-out of the WHO Child Growth Standards and facilitated their rapid global implementation.
Appendix
WHO Multicentre Growth Reference Study Group
Coordinating Team: Mercedes de Onis (Study Coordinator), Adelheid Onyango, Elaine Borghi, Amani Siyam (Department of Nutrition, WHO).
Executive Committee: Cutberto Garza (Chair), Mercedes de Onis, Jose Martines, Reynaldo Martorell, Cesar G. Victora, Maharaj K. Bhan.
Steering Committee: Coordinating Centre (WHO, Geneva): Mercedes de Onis, Jose Martines, Adelheid Onyango, Alain Pinol. Investigators (by country): Cesar G. Victora, Cora Luiza Araújo (Brazil); Anna Lartey, William B. Owusu (Ghana); Maharaj K. Bhan, Nita Bhandari (India); Kaare R. Norum, Gunn-Elin Aa. Bjoerneboe (Norway); Ali Jaffer Mohamed (Oman); Kathryn G. Dewey (USA). Representatives of UN agencies: Cutberto Garza (United Nations University), Krishna Belbase (UNICEF).
Advisory Group: Maureen Black, Wm. Cameron Chumlea, Tim Cole, Edward Frongillo, Laurence Grummer-Strawn, Reynaldo Martorell, Roger Shrimpton, Jan Van den Broeck.
Participating countries and investigators: Brazil: Cora Luiza Araújo, Cesar G. Victora, Elaine Albernaz, Elaine Tomasi, Rita de Cássia Fossati da Silveira, Gisele Nader (Departamento de Nutrição and Departamento de Medicina Social, Universidade Federal de Pelotas; and Núcleo de Pediatria and Escola de Psicologia, Universidade Católica de Pelotas). Ghana: Anna Lartey, William B. Owusu, Isabella Sagoe-Moses, Veronica Gomez, Charles Sagoe-Moses (Department of Nutrition and Food Science, University of Ghana; and Ghana Health Service). India: Nita Bhandari, Maharaj K. Bhan, Sunita Taneja, Temsunaro Rongsen, Jyotsna Chetia, Pooja Sharma, Rajiv Bahl (All India Institute of Medical Sciences). Norway: Gunn-Elin Aa. Bjoerneboe, Anne Baerug, Elisabeth Tufte, Kaare R. Norum, Karin Rudvin, Hilde Nysaether (Directorate of Health and Social Affairs; National Breastfeeding Centre, Rikshospitalet University Hospital; and Institute for Nutrition Research, University of Oslo). Oman: Ali Jaffer Mohamed, Deena Alasfoor, Nitya S. Prakash, Ruth M. Mabry, Hanadi Jamaan Al Rajab, Sahar Abdou Helmi (Ministry of Health). USA: Kathryn G. Dewey, Laurie A. Nommsen-Rivers, Roberta J. Cohen, M. Jane Heinig (University of California, Davis).
WHO Regional Offices staff: Ayoub Al-Jawaldeh (EMR), Kunal Bagchi (SEAR), Tomasso Cavalli-Sforza (WPR), Ferima Coulibaly-Zerbo (AFR), Aichatou Diawara Gbaguidi (AFR), Abel Dushimimana (AFR), Chessa Lutter (AMR), Charles Sagoe-Moses (AFR), Ursula Trubswasser (AFR), Trudy Wijnhoven (EUR).







