Depressive disorders, anxiety disorders, and stress and adjustment disorders are common psychiatric disorders in general practice. In Europe, the estimated proportions of patients visiting a general practitioner (GP) because of these disorders vary between 12 and 32%. Reference Berardi, Berti Ceroni, Leggieri, Rucci, Ustun and Ferrari1–Reference Nordstrom and Bodlund5 Depressive, anxiety, and stress and adjustment disorders cause emotional and social difficulties for patients and their relatives, loss of income and a poorer quality of life. These very common psychiatric disorders also place a large economic burden on society. Standard treatment of depressive, anxiety, and stress and adjustment disorders includes pharmacological treatment and/or different types of psychotherapy. For example, cognitive–behavioural therapy (CBT) has been recognised as an effective way of treating depressive disorders Reference Oei, Bullbeck and Campbell6 and is currently being introduced as a standard treatment in Swedish general practices. A meta-analysis of CBT for adult depression, based on 115 studies, found that CBT is an effective treatment for adult depression. The authors also concluded that CBT is the most studied psychotherapy for depression, and thus has the greatest weight of evidence. Reference Cuijpers, Berking, Andersson, Quigley, Kleiboer and Dobson7 In Sweden, clinical psychologists and social counsellors mainly give CBT on an individual basis. However, CBT therapists are in short supply and the individual therapeutic approach is expensive for the tax-financed healthcare system. A stronger focus on group therapy in general practice could help to save limited resources and might, according to a study involving participants from 46 general practices in Sweden, be implemented in the routine care of patients with depression. Reference Hansson, Bodlund and Chotai8
Mindfulness-based therapies might be suitable for group therapy sessions for psychiatric patients in general practice. An important advantage of mindfulness-based therapies over most other psychotherapies are that mindfulness may be accessible to larger groups of patients as they can, after introduction, practice mindfulness on their own. A practice review of the benefits of mindfulness found that mindfulness-based therapies decrease depressive symptoms and anxiety and reduce psychological distress. Mindfulness was also associated with less physical illness, improved well-being, increased self-control, decreased negative affect, better affect tolerance and improved concentration, focus attention and working memory. Among therapists, it was associated with increased empathy and better overall wellness. Reference Davis and Hayes9 A recent meta-analysis based on 19 studies found that mindfulness- and acceptance-based interventions are associated with robust and substantial reductions in symptoms of anxiety and comorbid depressive symptoms. Reference Vollestad, Nielsen and Nielsen10 Practising mindfulness regularly may decrease vulnerability to cognitive and emotional reactions leading to stress and other psychological problems. Reference Teasdale, Segal and Williams11 Merely by means of specific breathing techniques, the patient learns to focus and sustain attention and increase his or her awareness. Habitual and negative automatic reactions and responses to emotions and cognition can thereby be prevented. Instead, more balanced responses and reactions will be possible choices for the patient. Reference Teasdale, Segal and Williams11 Finally, recent research has shown that mindfulness has positive effects on affective experience. Reference Jha, Stanley, Kiyonaga, Wong and Gelfand12 as well as on cognition and pain. Reference Zeidan, Gordon, Merchant and Goolkasian13,Reference Zeidan, Johnson, Diamond, David and Goolkasian14 Mindfulness-based therapies have become increasingly popular as therapeutic strategies for a variety of medical and psychiatric conditions and include mindfulness-based stress reduction (MBSR) and mindfulness-based cognitive therapy (MBCT). Reference Chiesa and Serretti15–Reference Kuyken, Watkins, Holden, White, Taylor and Byford18 MBSR is a clinically based method with developed manuals and standardised techniques Reference Marchand19 and MBCT is based on an integration of CBT and MBSR. Reference Chiesa and Serretti15 One important advantage when implementing MBSR is that certified instructors can give MBSR after a 6-day course. The instructors may have a background as psychologists or social counsellors but may also be nurses, physiotherapists or doctors. In Sweden, MBCT is a method that is used to treat mild to moderate depression and chronic stress reactions. Reference Teasdale, Segal, Williams, Ridgeway, Soulsby and Lau20 However, mindfulness-based therapies are not well documented regarding their effectiveness in group therapy sessions given in general practice settings, where a majority of patients are treated. This study addresses this issue. The aim of this clinical randomised controlled trial (RCT) was to compare the effect of a structured mindfulness-based group therapy programme with treatment as usual (TAU, mostly individual CBT) in patients with clinical diagnoses of depressive, anxiety and stress and adjustment disorders in 16 general practices in Southern Sweden.
Method
Recruitment of general practices
This RCT was conducted in the county of Skåne, the most Southern region in Sweden. Skåne includes 150 general practices serving a population of 1.3 million people. Twenty-four general practices from all parts of the region were randomly selected in order to achieve a geographic representativeness of the whole county. J.S. informed all the directors at the 24 general practices via an email that provided details about the study and possible participation.
Recruitment of instructors
Seventeen of the contacted 24 general practices were interested in participating in the study and one dropped out at an early stage. The staff at the remaining 16 general practices (participation rate 16/24, 67%) were informed about the study by their clinical directors, who also suggested suitable occupational groups for the task as instructors (i.e. psychologists, social counsellors, nurses, physiotherapists and doctors).
Training of instructors
Our goal was to train two instructors per participating general practice. Two of the 16 general practices were relatively small and located close to each other and were therefore given permission to work together. In total, 30 instructors (mainly psychologists and social counsellors) received the training programme at our department (Center for Primary Health Care Research, Malmö, Sweden). The training was given during 6 days that were evenly spread between September 2011 and December 2011 and all sessions were led by Ola Schenström (O.S.) and L.M.J., one of the authors. O.S. was trained at the Center for Mindfulness in Medicine, Health Care, and Society, founded by Jon Kabat-Zinn at the University of Massachusetts, US. O.S. is a leading expert in mindfulness education in Sweden and L.M.J. is a psychiatrist and licensed psychotherapist with long clinical experience of mindfulness therapy.
A key part of the training is the future instructors’ own mindfulness training. The future instructors were trained in how to guide individuals and groups in mindfulness training so that the individual may develop a greater awareness of thoughts, feelings and bodily sensations and be able to cope better with stress and difficulties in everyday life. All the 30 participants in the 6-day course completed the course, passed the oral examination and became certified mindfulness instructors. The 6-day course was given to the 30 participants at no cost.
Recruitment of patients
Each participating general practice was responsible for the recruitment of patients who met the inclusion criteria (see below). The recruitment of patients started on 4 January 2012 and ended on 22 March 2012. Newly diagnosed patients as well as those who had a history of psychiatric disorders were eligible. However, only those who sought treatment for their psychiatric disorder during the recruitment period were considered for inclusion in the study. Typically, the patient called the general practice and talked to a nurse, who asked what type of medical problem the patient had. If the nurse suspected that the patient might be eligible for inclusion in the study, she or he booked an appointment with the doctor that was 10–15 min longer than usual in order to make sure that the doctor had time to inform potentially eligible patients about participation in the study. The patients also received written information about the study and were given the opportunity to ask questions. It was emphasised to the patient that participation was voluntary and could be terminated at any time during the study. If the patient agreed to participate, both the doctor and the patient signed a written informed consent. The patients were assessed for the need of pharmacological treatment and were prescribed psychotropic drugs if that was considered necessary. Sometimes the doctor also ordered thyroid laboratory tests, in order to exclude potential thyroid disease that might explain the psychiatric symptoms. If the thyroid tests were abnormal, the patient was not considered for inclusion in the study. After the consultation, the patient was asked to fill in three self-rated depression and anxiety scales: the Montgomery-Åsberg Depression Rating Scale (MADRS-S), Reference Montgomery and Asberg21 the Hospital Anxiety and Depression Scale (HADS, anxiety and depression subscales) Reference Zigmond and Snaith22 and the Patient Health Questionnaire (PHQ-9). Reference Kroenke, Spitzer and Williams23
Inclusion criteria
The four criteria below all needed to be fulfilled for inclusion in the study. The listed ICD-10 24 codes in the first criterion were based on clinical diagnoses, made by medical doctors.
-
(a) One or more of the following ICD-10 psychiatric diagnoses: F32.0, mild depressive episode; F32.1, moderate depressive episode; F32.9, depressive episode, unspecified; F33.0, recurrent depressive disorder, current episode mild; F33.1, recurrent depressive disorder, current episode moderate; F41.0, panic disorder; F41.1, generalized anxiety disorder; F41.2, mixed anxiety and depressive disorder; F41.3, other mixed anxiety disorders; F41.8, other specified anxiety disorders; F41.9, anxiety disorder, unspecified; F43.2, adjustment disorders; F43.8, other reactions to severe stress; and F43.9, reaction to severe stress, unspecified.
-
(b) Age 20–64 years (i.e. the population of working age).
-
(c) Ability to speak and read Swedish.
-
(d) One or more of the following cut-offs: a score between 13 and 34 on the MADRS-S scale; a score ≥7 on the HADS-A scale; a score ≥7 on the HADS-D scale; a score ≥10 on the PHQ-9 scale.
Exclusion criteria were: severe psychiatric symptoms requiring psychiatric care, risk of suicide; inability to participate at group sessions because of severe substance misuse; pregnancy; current psychotherapy of any kind; participation in any other psychiatric intervention study; thyroid disease (if newly diagnosed by the doctor).
Self-rated scales and cut-offs
MADRS-S
The MADRS was designed in 1979 by British and Swedish researchers in order to measure the severity and change over time of depressive symptoms in patients with mood disorders. Reference Montgomery and Asberg21 A self-rated version of this scale, MADRS-S, has often been used in clinical practice and the agreement between physicians’ and patients’ ratings is moderate to good. Reference Cunningham, Wernroth, von Knorring, Berglund and Ekselius25 The MADRS-S instrument has nine questions/items, with each item yielding a score of 0–6. The overall score ranges from 0 to 54 points. Usual cut-offs are as follows: 0–12 (no depression), 13–19 (mild depression), 20–34 (moderate depression) and >34 (severe depression).
HADS
The HADS was developed in 1983 to identify possible cases of anxiety and depression among patients in non-psychiatric hospital clinics. Reference Zigmond and Snaith22 It was divided into an anxiety subscale (HADS-A) and a depression subscale (HADS-D), both containing seven items. A review of 747 identified papers that used HADS concluded that ‘an optimal balance between sensitivity and specificity was achieved when caseness was defined by a score of 8 or above on both HADS-A and HADS-D’. Reference Bjelland, Dahl, Haug and Neckelmann26 Usual cut-off points for both HADS-A and HADS-D are as follows: 8–10 (mild anxiety/depression), 11–14 (moderate anxiety/depression) and ≥15 (severe anxiety/depression).
PHQ-9
The PHQ is a self-rated version of the PRIME-MD diagnostic instrument for common mental disorders. Reference Kroenke, Spitzer and Williams23 The PHQ-9 is the depression module, which scores each of the nine DSM-IV 27 criteria for depression as ‘0’ (not at all) to ‘3’ (nearly every day). Usual cut-off points for PHQ-9 are as follows: 0–4 (no depression), 5–9 (mild depression), 10–14 (moderate depression), 15–19 (moderately severe depression) and 20–27 (severe depression).
The rationale for using multiple scales to assess symptoms of depression and anxiety was that different scales are used in different clinical practices worldwide and we wanted to increase the generalisability of our results as well as the robustness of our findings. With the MADRS-S, an upper limit for the score was set in order to exclude those participants with severe depression, whereas no such upper limit was set for HADS-A, HADS-D and PHQ-9. The rationale for this decision was that previous research comparing the HADS-D and PHQ-9 has shown that they differ considerably in how they categorise severity and that further work is needed to assess the validity of these scales’ severity cut-off bands. Reference Cameron, Crawford, Lawton and Reid28
Randomisation
The certified mindfulness instructors called those participants that were eligible for inclusion in the study. The instructors were present at the participants’ first study-related visit to the general practice. This first visit was performed before any psychotherapy or counselling had been started and often took place in a group. During the visit, participants provided blood samples and filled in a questionnaire that included general questions about their health, current medication and sociodemographic characteristics. They were also informed as to whether they would be included in the intervention or control group. The randomisation protocol was designed by the Competence Centre for Clinical Research at Lund University and included a list with numbers 1–20 for each general practice. Each number corresponded to allocation to the intervention or the control group and participants were added to the list in the order in which they signed the informed consent form. Once allocated to one of the two groups, participants were not allowed to change group. The allocation was masked, that is, the investigators did not know during the allocation to which group they were assigning each patient.
Intervention
The programme used in the present study was based on the two mindfulness-based therapies MBSR Reference Kabat-Zinn, Lipworth, Burncy and Sellers29–Reference Kabat-Zinn31 and MBCT. Reference Chiesa and Serretti15–Reference Kuyken, Watkins, Holden, White, Taylor and Byford18 It included structured and controlled meditative exercises. The period of intervention varied somewhat between the different sites. The first and last mindfulness session took place on 26 January 2012 and 15 May 2012, respectively, in the 16 general practices. The mindfulness-based group therapy lasted 8 weeks and was given in 2 h sessions, once a week. The participants were also instructed to practice mindfulness at home for 20 min/day and were given a compact disc, a training manual and a diary for this purpose. On average, the participants undertook 102 individual-based mindfulness sessions (s.d. = 44, range 0–219). Two mindfulness instructors were present at each group session and each group consisted of a maximum of ten participants. The time for the sessions was flexible, in order to increase the participation rate. Individual attendance at each group session was recorded but not required. Participants were asked to wear comfortable clothes and to bring a mat or blanket for some of the exercises. All participants received pharmacological treatment, if deemed necessary, and follow-up by the doctor at the general practice.
Control group
The control group received TAU, which sometimes included pharmacological treatment and in most cases also psychotherapy or counselling. Most patients in the control group received CBT (n = 80). The average number of individual CBT sessions was six.
Follow-up
Immediately after the intervention, all participants were evaluated for psychiatric symptoms using the same questionnaires as described above. The participants were asked to come to the general practice to fill in the questionnaires.
Site visits
To ensure data credibility, patient integrity and patient safety, a research team consisting of one research nurse, one psychologist and one project administrator supported all sites at monitoring visits.
Ethical considerations and handling of personal data
The study was performed according to the principles of the Declaration of Helsinki. It was approved by the Ethics Committee of Lund University prior to its commencement on 5 October 2011 (application no. 2011/491). Written informed consent was obtained from all participants. All data were analysed anonymously. During the intervention, identification lists were kept in a locked place by the mindfulness instructors. However, all names and personal ID numbers (the Swedish version of social security numbers) were replaced with anonymous serial numbers, which were associated with all questionnaires throughout the study. The results are reported at the group level and it is not be possible to identify individuals.
Statistical analyses and power calculations
All analyses were repeated for the four outcome scales: MADRS-S, HADS-A, HADS-D and PHQ-9. Differences in baseline characteristics between the mindfulness and control groups were tested using Wilcoxon rank sum test for medians, Student’s t-test for means and χ2 test for proportions. Within-group analyses (median change between baseline and follow-up in the mindfulness and control group) were conducted using Wilcoxon signed-rank test. The rationale for having the main focus on medians rather than means was the ordinal nature of our data: all scales for assessments of depressive symptoms and anxiety were based on ordinal data. To test the robustness of our analyses, we also analysed the data based on mean scores and in a continuous manner; the results were almost identical (Table 4). Because of the potential correlation of measurements within individuals as well as within general practices, we used an ordinal mixed model (in this case a proportional odds mixed model) to examine the effect of mindfulness on the outcome (change from baseline), adjusted for the baseline score. Another advantage with mixed models is that all available data are used under the missing at random assumption, which means that data from those who drop out as well as data from those who complete the study can be used. All scales were categorised and odds ratios (ORs) were estimated using ordinal logistic regression models (the proportional odds model relaxes the assumption of identical log odds over all levels of the outcome). An interaction term between time and randomisation group was created to estimate the treatment effect.
In an explorative analysis we wanted to examine how the number of attended mindfulness sessions affected the outcome and also to separately analyse the control group according to CBT and other types of psychotherapy/counselling. We used median change from baseline (adjusted for baseline score) to explore this. This was obtained by applying a median regression model to the data and by then predicting the median for the different groups, adjusted for the sample mean for baseline score. Confidence intervals were obtained from bootstrapped standard errors.
Patients who had not responded on three or more items on the scales were counted as missing. For those who had missing values for one or two items, the mean number of points for the questions they had responded to was used to impute values for the missing questions. In a sensitivity analysis we also examined how influential observations and outliers affected our results. Cluster effects, i.e. people from the same general practice being more alike than people from different general practices, were assessed as variance between general practices. This variance was very small compared with the individual variance and did not change our results. Stata version 12 for Windows was used for all statistical analyses.
The power calculations were based on the assumption that the mindfulness group therapy would be no worse than TAU. We therefore performed a power calculation that was based on non-inferiority. The patients were expected to have mild to moderate depression, i.e. 13–34 points on the MADRS-S and a mean MADRS-S score of 20 at baseline. The treatment group was considered non-inferior to the control group at a difference of at most 3.5 points. Based on previous studies, we assumed that the improvement in the control group would be around 15 points after treatment Reference Thase, Larsen and Kennedy32 and judged that a difference between the mindfulness and control groups of 3.5 points would represent a clinically negligible difference between the two groups. In the non-inferiority analysis, we used a 97.5% one-sided confidence interval to examine whether the upper limit exceeded 3.5. With a standard deviation of 8, a power of 80% and an alpha (α) of 0.025, each group should consist of at least 83 patients. With an expected drop-out rate of about 30%, the final number of patients per group should be 119. Based on these assumptions, the study would have an effect size of 0.4, which corresponds to a ‘medium level’ (‘small to moderate level’ according to Cohen). Reference Cohen33 Using the Wilcoxon signed-rank test instead of a t-test gave almost the same efficiency (the asymptotic relative efficiency of the two tests never falls below 0.864). Reference Hodges and Lehmann34
Results
In total, 215 eligible patients at the 16 general practices were randomised to either mindfulness (n = 110) or the control group (n = 105). Figure 1 shows the randomisation, drop-out, missing items and observed cases. The main reasons for drop-out were work situation and lack of time. Other reasons included moving house, sickness, no desire for treatment and disappointment at being randomised to the control group. The number of participants who dropped out after the randomisation and baseline examination was higher in the mindfulness group (n = 18) than in the control group (n = 9). There were no significant differences in sociodemographic characteristics between those who dropped out and those who remained in the study. However, those who dropped out scored significantly higher at baseline on all scales than those who remained in the study. A total of 81 (MADRS-S), 83 (HADS-A and HADS-D) and 82 (PHQ-9) patients were included in the final analysis of the mindfulness group. For the control group, a total of 86 (MADRS-S, HADS-A and HADS-D) and 85 (PHQ-9) patients were included in the final analysis.
Table 1 shows baseline characteristics and missing data in the two groups. The mean age was 42 and 41 years in the mindfulness and control groups, respectively. Women as well as those with a middle or high level of education were in the large majority in both groups. Around two-thirds were married. More patients were not taking medication than those who were for depression or anxiety. There were no significant differences in sociodemographic characteristics or medication between the two groups. The P-values for treatment with antidepressants and tranquilisers were 0.882 and 0.937, respectively, which indicates that there were no statistically significant differences in pharmacological treatment between the mindfulness and the control group. Baseline scores

Fig. 1 CONSORT flow diagram showing randomisation, drop-out, missing items and observed cases in the mindfulness and control groups. MADRS-S, Montgomery–Åsberg Depression Rating Scale (self-rated version); HADS, Hospital Anxiety and Depression Scale; HADS-D, HADS subscale for depression; HADS-A, HADS subscale for anxiety; PHQ-9, Patient Health Questionnaire-9.
Table 1 Characteristics at baseline stratified by group (mindfulness and control)

| Mindfulness group (n = 110) |
Control group (n = 105) |
P Footnote a | |
|---|---|---|---|
| Baseline MADRS-S | |||
| n | 108 | 103 | |
| Missing, % (n) | 1.8 (2) | 1.9 (2) | |
| Median score (IQR) | 20 (11) | 23 (9) | 0.045 |
| Mean (s.d.) | 20 (7.7) | 22 (6.9) | |
| Baseline HADS-D | |||
| n | 110 | 105 | |
| Missing, % (n) | 0 (0) | 0 (0) | |
| Median score (IQR) | 8 (5) | 9 (4) | 0.050 |
| Mean (s.d.) | 8.5 (3.6) | 9.3 (3.7) | |
| Baseline HADS-A | |||
| n | 110 | 105 | |
| Missing, % (n) | 0 (0) | 0 (0) | |
| Median score (IQR) | 12 (6) | 13 (4) | 0.059 |
| Mean (s.d.) | 12 (3.7) | 13 (3.2) | |
| Baseline PHQ-9 | |||
| n | 110 | 105 | |
| Missing, % (n) | 0 (0) | 0 (0) | |
| Median score (IQR) | 12 (11) | 14 (7) | 0.127 |
| Mean (s.d.) | 13 (6) | 14 (5.2) | |
| Age | |||
| n | 110 | 105 | |
| Missing, % (n) | 0 (0) | 0 (0) | |
| Mean age, years (s.d.) | 42 (11) | 41 (11) | 0.475 |
| Gender | |||
| n | 110 | 105 | |
| Missing, % (n) | 0 (0) | 0 (0) | |
| Men/women, % | 19/81 | 10/90 | 0.076 |
| Education | |||
| n | 108 | 101 | |
| Missing, % (n) | 1.8 (2) | 3.8 (4) | |
| Low/middle/high, % | 7/44/47 | 11/33/51 | 0.267 |
| Marital status | |||
| n | 107 | 101 | |
| Missing, % (n) | 2.7 (3) | 3.8 (4) | |
| Married/single/divorced, % | 63/20/15 | 65/18/13 | 0.911 |
| Antidepressants | |||
| n | 95 | 95 | |
| Missing, % (n) | 13.6 (15) | 9.5 (10) | |
| Yes/no, % | 35/52 | 35/55 | 0.882 |
| Tranquillisers | |||
| n | 92 | 89 | |
| Missing, % (n) | 16.4 (18) | 15.2 (16) | |
| Yes/no, % | 16/67 | 16/69 | 0.937 |
MADRS-S, Montgomery–Åsberg Depression Rating Scale (self-rated version); HADS, Hospital Anxiety and Depression Scale; HADS-D, HADS subscale for depression; HADS-A, HADS subscale for anxiety; PHQ-9, Patient Health Questionnaire-9.
a. Tests for differences between mindfulness and control group.
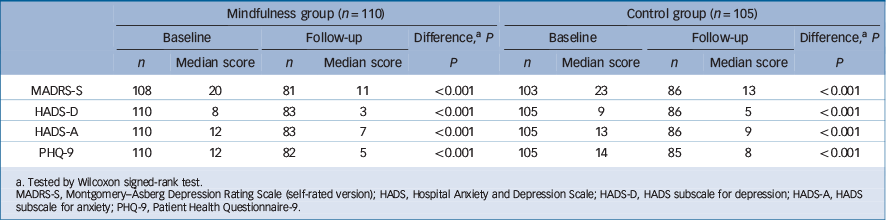
Table 2 Median scores and number of observed cases at baseline and follow-up in the mindfulness and control groups
| Mindfulness group (n = 110) | Control group (n =105) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Baseline | Follow-up | Difference,Footnote
a
P
P |
Baseline | Follow-up | Difference,Footnote
a
P
P |
|||||
| n | Median score | n | Median score | n | Median score | n | Median score | |||
| MADRS-S | 108 | 20 | 81 | 11 | <0.001 | 103 | 23 | 86 | 13 | <0.001 |
| HADS-D | 110 | 8 | 83 | 3 | <0.001 | 105 | 9 | 86 | 5 | <0.001 |
| HADS-A | 110 | 12 | 83 | 7 | <0.001 | 105 | 13 | 86 | 9 | <0.001 |
| PHQ-9 | 110 | 12 | 82 | 5 | <0.001 | 105 | 14 | 85 | 8 | <0.001 |
a Tested by Wilcoxon signed-rank test.
MADRS-S, Montgomery–Åsberg Depression Rating Scale (self-rated version); HADS, Hospital Anxiety and Depression Scale; HADS-D, HADS subscale for depression; HADS-A, HADS subscale for anxiety; PHQ-9, Patient Health Questionnaire-9.
for MADRS-S (23 v. 20, P = 0.045) and HADS-D (9 v. 8, P = 0.050) were significantly higher in the control group than in the mindfulness group. The most common therapy in the control group was individual CBT (CBT, n = 80; physical activity therapy, n = 2; none, n = 8.).
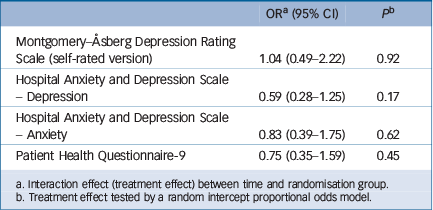
Table 2 shows median scores and number of observed cases at baseline and follow-up in the mindfulness and control groups. Before the treatment started, the scores indicated mild to moderate symptoms of depression and anxiety in the different subgroups. After the intervention had ended, the scores indicated no to mild symptoms in the different subgroups. For all three scales, the median scores decreased significantly in both groups; all P-values were <0.001. There were no significant differences (treatment effects) between the mindfulness and control groups (Tables 3 and 4) for any of the three scales. The estimated differences in Table 4 were based on mean values.
Table 5 shows median score changes from baseline, adjusted for baseline score, in the mindfulness group (by number of mindfulness sessions, i.e. 1–5 or 6–8 sessions) and control group (any treatment or CBT only). The control group in Model 1 includes those patients with any treatment (for example CBT, body awareness or counselling) whereas the control group in Model 2 only includes those with CBT. In both control groups, there was a statistically significant change in median score at follow-up, compared with baseline, for MADRS-S, HADS-D, HADS-A and PHQ-9, i.e. all the self-rated scales used in this study. Among those who had undergone 6–8 mindfulness sessions, there were also significant changes at follow-up for all the self-rated scales in both models. However, among those who had undergone 1–5 mindfulness sessions, there were statistically significant changes at follow-up only for the HADS-D scale. For MADRS-S, HADS-A and PHQ-9, there were no statistically significant changes at follow-up after only 1–5 mindfulness sessions. The absolute differences in median change among those who had undergone 6–8 mindfulness sessions v. those who had undergone only 1–5 mindfulness sessions were 2.55, 1.00, 2.80 and 4.31 for MADRS-S, HADS-D, HADS-A and PHQ-9, respectively (control group: any treatment). These differences were, however, not statistically significant (Table 6).
In an explorative analysis we examined separately those participants on antidepressants and those not on them. The results remained the same in both groups (data not shown). We also performed a non-inferiority analysis in order to test whether the mindfulness treatment was non-inferior to TAU. We used a 97.5% one-sided confidence interval to examine whether the upper limit exceeded 3.5. This test showed that mindfulness was non-inferior to TAU (upper limit 3.17). Finally, in a sensitivity analysis we examined whether any influential observations or outliers affected the results, which was not the case.
Table 3 Differences (treatment effects) between the mindfulness and control groups (odds ratios)
| ORFootnote a (95% CI) | P Footnote b | |
|---|---|---|
| Montgomery–Åsberg Depression Rating
Scale (self-rated version) |
1.04 (0.49–2.22) | 0.92 |
| Hospital Anxiety and Depression Scale
– Depression |
0.59 (0.28–1.25) | 0.17 |
| Hospital Anxiety and Depression Scale
– Anxiety |
0.83 (0.39–1.75) | 0.62 |
| Patient Health Questionnaire-9 | 0.75 (0.35-1.59) | 0.45 |
a. Interaction effect (treatment effect) between time and randomisation group.
b. Treatment effect tested by a random intercept proportional odds model.
Table 4 Differences (treatment effects) between the mindfulness and control groups (mean values)

| Mean difference (95% CI) s.e. | P Footnote a | |
|---|---|---|
| Montgomery–Åsberg Depression
Rating Scale (self-rated version) |
–0.67 (–3.17 to 1.83) 1.27 | 0.60 |
| Hospital Anxiety and Depression
Scale – Depression |
0.33 (–0.86 to 1.51) 0.60 | 0.59 |
| Hospital Anxiety and Depression
Scale – Anxiety |
0.24 (–0.94 to 1.43) 0.60 | 0.69 |
| Patient Health Questionnaire-9 | –0.18 (–1.98 to 1.62) 0.91 | 0.84 |
a. Treatment effect tested by t-test.
Table 5 Median score changes from baseline, adjusted for baseline score, in the mindfulness group (by number of mindfulness sessions) and control group (any treatment or cognitive-behavioural therapy (CBT) only)

| Observed cases | Model 1 (control group: any treatment) | Model 2 (control group: only CBT) | ||||
|---|---|---|---|---|---|---|
| n | Median change | P Footnote a | n | Median change | P Footnote a | |
| Montgomery–Åsberg Depression Rating Scale (self-rated version) | ||||||
| Control | 85 | –8.18 (–10.57 to –5.79) | <0.001 | 71 | –8.40 (–10.99 to –5.80) | < 0.001 |
| Mindfulness (1–5 sessions) | 12 | –5.89 (–12.39 to 0.62) | 0.08 | 12 | –5.75 (–14.88 to 3.38) | 0.22 |
| Mindfulness (6–8 sessions) | 68 | –8.43 (–9.98 to –6.88) | < 0.001 | 68 | –8.58 (–10.26 to –6.90) | < 0.001 |
| Hospital Anxiety and Depression Scale – Depression | ||||||
| Control | 86 | –3.74 (–4.53 to –2.95) | < 0.001 | 71 | –3.74 (–4.83 to –2.64) | < 0.001 |
| Mindfulness (1–5 sessions) | 13 | –3.94 (–6.68 to –1.19) | 0.005 | 13 | –3.94 (–5.82 to –2.05) | < 0.001 |
| Mindfulness (6–8 sessions) | 70 | –4.94 (–6.02 to –3.85) | < 0.001 | 70 | –4.94 (–6.27 to –3.60) | < 0.001 |
| Hospital Anxiety and Depression Scale – Anxiety | ||||||
| Control | 86 | –3.97 (–5.20 to –2.75) | < 0.001 | 71 | –3.88 (–4.89 to –2.87) | < 0.001 |
| Mindfulness (1–5 sessions) | 13 | –1.97 (–4.66 to 0.71) | 0.15 | 13 | –2.17 (–4.94 to 0.60) | 0.12 |
| Mindfulness (6–8 sessions) | 70 | –4.77 (–5.61 to –3.94) | < 0.001 | 70 | –4.74 (–5.62 to –3.85) | < 0.001 |
| Patient Health Questionnaire-9 | ||||||
| Control | 85 | –6.06 (–7.63 to –4.49) | < 0.001 | 70 | –6.39 (–8.08 to –4.70) | < 0.001 |
| Mindfulness (1–5 sessions) | 13 | –3.17 (–6.64 to 0.30) | 0.07 | 13 | –3.25 (–8.35 to 1.86) | 0.21 |
| Mindfulness (6–8 sessions) | 69 | –7.48 (–9.08 to –5.87) | < 0.001 | 69 | –7.39 (–9.15 to –5.63) | < 0.001 |
a. Test of adjusted median change from baseline using one-sample t-test.
Table 6 Comparison between different numbers of mindfulness sessions (treatment group only)

| Observed cases | Model 1 (control group: any treatment) | Model 2 (control group: only CBT) | ||
|---|---|---|---|---|
| Difference | P Footnote a | Difference | P Footnote a | |
| Montgomery–Åsberg Depression Rating Scale | ||||
| (self-rated version) 6–8 v. 1–5 sessions | –2.55 (–9.50 to 4.40) | 0.47 | –2.83 (–9.01 to 3.35) | 0.37 |
| Hospital Anxiety and Depression Scale – Depression | ||||
| 6–8 v. 1–5 sessions | –1.00 (–3.01 to 1.01) | 0.33 | –1.00 (–2.76 to 0.76) | 0.26 |
| Hospital Anxiety and Depression Scale – Anxiety | ||||
| 6–8 v. 1–5 sessions | –2.80 (–6.11 to 0.51) | 0.10 | –2.57 (–5.21 to 0.07) | 0.06 |
| Patient Health Questionnaire-9 | ||||
| 6–8 v. 1–5 sessions | –4.31 (–8.61 to –0.006) | 0.050 | –4.12 (–8.80 to 0.51) | 0.08 |
a. Test of differences between 6–8 and 1–5 mindfulness sessions using t-test.
Discussion
Main findings and comparison with findings from other studies
The main finding of the present RCT is that mindfulness group therapy given in a general practice setting, where a majority of patients with depression, anxiety, and stress and adjustment disorders are treated, is non-inferior to individual-based therapy, including CBT. To the best of our knowledge, this is the first RCT performed in a general practice setting where the effect of mindfulness group therapy was compared with an active control group.
Although a growing body of research has examined the effect of mindfulness on somatic as well as psychiatric conditions, scientific knowledge from RCT studies is scarce. For example, a 2007 review based on 15 various types of studies found that diversity in the methodologies and participant samples was evident. Reference Toneatto and Nguyen35 Although around half of the studies (8/15) reported a statistically significant reduction in symptoms of anxiety or depression after mindfulness-based therapy, none included an active control group. The authors of the 2007 review concluded that increased emphasis on research designs with active control groups would be necessary in future studies to assess the unique effect of mindfulness-based therapies compared with other types of therapies. In addition, recent studies of mindfulness-based programmes have concluded that further studies using an RCT design are warranted. Reference Kearney, McDermott, Malte, Martinez and Simpson36
Examples of previous studies include a study of 56 adults in the USA that found that MBSR treatment was associated with reductions in social anxiety and depression and an increase in subjective well-being. Reference Jazaieri, Goldin, Werner, Ziv and Gross37 A Norwegian study of 76 people, recruited through a newspaper advertisement, randomised participants to an MBSR programme or a waiting-list control group. Treatment completers showed medium to large effect sizes on measures of anxiety and a large effect size on symptoms of depression. The authors concluded that MBSR is an effective treatment for anxiety disorders and related symptomatology. Reference Vøllestad, Sivertsen and Nielsen38 A Danish clinical trial used a structured 8-week group-based mindfulness-based programme on 336 women who had been operated on for breast cancer. Reference Würtzen, Dalton, Elsass, Sumbundu, Steding-Jensen and Karlsen39 The 8-week intervention had statistically significant and clinically meaningful effects on depression and anxiety at follow-up, and medium to large effect sizes.
Limitations
The present study has some limitations. Although immigrants were included in the RCT, those who could not speak Swedish fluently were not invited to participate. In a country like Sweden, with a large proportion of immigrants, it would have been a better approach to include non-Swedish-speaking immigrants as well. However, as the Swedish immigrant population is very heterogeneous, it would not have been feasible to conduct a reliable study of the many different immigrant groups in Sweden within the scope of the present study. Another limitation is that we included patients with depressive as well as anxiety disorders. However, overlapping symptoms are relatively common among these conditions and our approach is in line with previous studies. The drop-out rate among those individuals who started treatment was 17.8% (18/101) and 9.5% (9/95) in the mindfulness and control groups, respectively. High drop-out rates could affect the generalisability of findings but we have no reason to believe that the drop-out rate was higher in the present study than in previous evaluations of different psychotherapies. There were slight differences in baseline scores for MADRS-S and HADS-D between the mindfulness and control groups. However, these differences were most likely random and relatively small and should not have affected our results, adjusted for baseline scores, to a large extent. The follow-up was relatively short and included an assessment of symptoms immediately after the 8-week intervention, which means that we cannot judge whether the improvement of symptoms will remain if the follow-up is longer. Finally, we had no access to treatment data from non-participating general practices and previous research from the UK has shown that there are variations in, for example, psychotropic prescribing by GPs. However, a study from the UK found that demographic factors were more powerful determinants of prescribing than characteristics of the practice itself, Reference Tsimtsiou, Ashworth and Jones40 which indicates that differences between practices should have a smaller impact than individual demographic factors on potential variation between practices. The limitations of the present study are, however, balanced by the many strengths. For example, the use of an RCT with an active control group is a major main contribution to this relatively under-researched field. Moreover, our study of 215 randomised patients with a medical diagnosis was performed in a monitored clinical setting of 16 general practices in urban as well as rural areas. Although this study was not designed to examine whether those who had undergone 6–8 mindfulness sessions had larger median changes v. those who had undergone only 1–5 mindfulness sessions, the results suggest that future studies could examine a possible dose-response relationship in a larger sample.
Implications
Patients who receive antidepressants have a reported remission rate of only 35–40%. Reference Fava, Rush, Trivedi, Nierenberg, Thase and Sackeim41 Additional treatment is therefore needed for non-responders as well as for those who are either unable or unwilling to engage in traditional psychotherapy. The findings of the present study therefore have several potential clinical implications and may be used in primary care patients with depressive, anxiety, or stress and adjustment disorders. Another important clinical implication is that certified instructors, that do not necessarily need to be psychologists or counsellors, can give mindfulness-based therapy to a group of patients with psychiatric symptoms common in primary care. We would also like to stress that CBT therapists are in short supply and that a stronger focus on group therapy given by certified instructors could help to save limited resources. However, it is important to note that not all patients are suited to participate in group sessions and it is thus important to offer an individual therapeutic approach to these patients. The present RCT provided evidence that mindfulness group therapy given by certified instructors is non-inferior to individual-based CBT. Future studies in other settings could provide more evidence on whether such an approach can provide effective treatment to a larger number of patients in a cost-effective manner.










eLetters
No eLetters have been published for this article.