Aggressive incidents in psychiatric hospitals are frequent and may be increasing (Reference FottrellFottrell, 1980; Reference Haller and DelutyHaller & Deluty 1988; Reference James, Fineberg and ShahJames et al, 1990; Reference AtakanAtakan, 1995). Previous research has yielded inconsistent and/or conflicting results but demographic and clinical variables, such as age, ethnicity, gender, diagnosis, psychopathology and ward environment, have been implicated (Reference Shah, Fineberg and JamesShah et al 1991; Reference DavisDavis 1991; Reference CrightonCrighton, 1995). The purpose of the present study was to examine prospectively the demographic and clinical variables associated with aggressive behaviour of in-patients in a general adult psychiatric unit serving a catchment area that comprises both urban and rural communities and distinguishable cultural/ethnic groups.
Method
For 9 months, all incidents of verbal and physical aggressive behaviour exhibited by patients in a 54-bed, adult acute psychiatric unit were assessed and rated routinely on the Overt Aggression Scale (OAS; Reference Yudofsky, Silver and JacksonYudofsky et al, 1986). Incidents were assessed by one of a small group of clinical staff who underwent a single training session. Each completed research form was discussed with the first author. The unit serves a population of 340 000, of which about 21% are ethnic Maori. Details of the service structure and functioning have been published elsewhere (Reference Mellsop, O'Brien and MathiesonMellsop et al, 2000). There are two general adult acute admission wards and an intensive care ward. The acute wards are staffed by a maximum of 19, 15, and 11 nurses during the day, evening and night shifts respectively. Nursing staff work 8-h shifts. The ethnic distribution of staff approximates that of the catchment population rather than of the patient population, with a male/female ratio of 1:4. The numbers of nursing staff vary according to bed occupancy. The OAS measures verbal and physical aggression including aggression against objects, self and other people. Information on patients’ characteristics, ICD–10 diagnoses (World Health Organization, 1992) and details of each aggressive incident were obtained. All patients admitted over the same period who did not exhibit any aggressive behaviour provided the comparison group. Drug screening was not routine but was carried out when the treating psychiatrist considered it indicated.
Data were analysed using χ2 and t-tests for group comparisons.
Results
Of the 535 patients admitted during the study period, 80 (15%) were involved in a total of 124 aggressive incidents. The demographic and clinical characteristics of patients are presented in Table 1. Of the 80, 44 (55%) had a history of previous violence and 54 (68%) had a history of substance misuse; 23% of admitted males but only 7% of females were aggressive at least once. Overall, 20% of Maori patients, 21% of the other non-European patients and only 11% of European patients exhibited aggressive behaviour. These differences were statistically significant. Schizophrenia accounted for 48%, bipolar affective disorder 27% and substance misuse (all with positive urine tests for cannabis) 14% of the total number of aggressive patients. About 30% of patients in each of the schizophrenia, bipolar and substance misuse categories were aggressive, and fewer than 10% in other diagnostic categories.
Table 1. Demographic and clinical characteristics of patients admitted during the study period
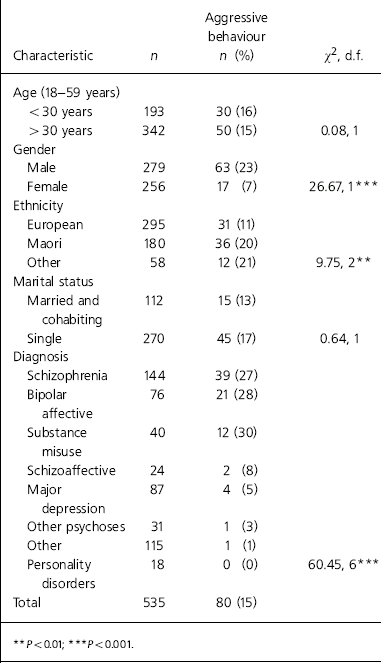
| Characteristic | n | Aggressive behaviour n (%) | χ 2, d.f. |
|---|---|---|---|
| Age (18-59 years) | |||
| < 30 years | 193 | 30 (16) | |
| > 30 years | 342 | 50 (15) | 0.08, 1 |
| Gender | |||
| Male | 279 | 63 (23) | |
| Female | 256 | 17 (7) | 26.67, 1*** |
| Ethnicity | |||
| European | 295 | 31 (11) | |
| Maori | 180 | 36 (20) | |
| Other | 58 | 12 (21) | 9.75, 2** |
| Marital status | |||
| Married and cohabiting | 112 | 15 (13) | |
| Single | 270 | 45 (17) | 0.64, 1 |
| Diagnosis | |||
| Schizophrenia | 144 | 39 (27) | |
| Bipolar affective | 76 | 21 (28) | |
| Substance misuse | 40 | 12 (30) | |
| Schizoaffective | 24 | 2 (8) | |
| Major depression | 87 | 4 (5) | |
| Other psychoses | 31 | 1 (3) | |
| Other | 115 | 1 (1) | |
| Personality disorders | 18 | 0 (0) | 60.45, 6*** |
| Total | 535 | 80 (15) |
Of the aggressive events, 59 (48%) involved patients with a history of violence and 83 (67%) involved patients with a history of alcohol or drug misuse. Table 2 summarises characteristics of aggressive events. Of the aggressive episodes, 40 (32%) occurred on the first day of admission and 83 (67%) in the first week; 52% took place during the evening shift and 27% and 21% during day and night shifts respectively. The majority (74%) of patients were involved in only one incident. Verbal aggression was the most frequent (57% involving nursing staff and 6% involving other patients). Physical aggression against staff accounted for at least 25% of the events and 15% of all aggressive events were rated as moderate-to-severe (OAS score >5). Patients who exhibited aggressive behaviour had a significantly longer total length of stay (median 14 days) than the nonaggressive patients (median 7 days).
Table 2. Characteristics of aggressive events
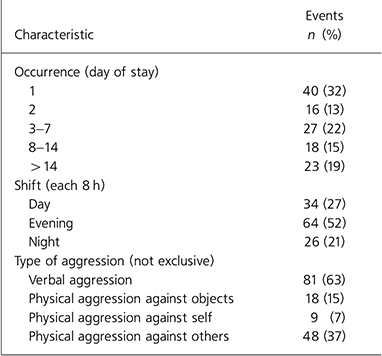
| Characteristic | Events n (%) |
|---|---|
| Occurrence (day of stay) | |
| 1 | 40 (32) |
| 2 | 16 (13) |
| 3-7 | 27 (22) |
| 8-14 | 18 (15) |
| > 14 | 23 (19) |
| Shift (each 8 h) | |
| Day | 34 (27) |
| Evening | 64 (52) |
| Night | 26 (21) |
| Type of aggression (not exclusive) | |
| Verbal aggression | 81 (63) |
| Physical aggression against objects | 18 (15) |
| Physical aggression against self | 9 (7) |
| Physical aggression against others | 48 (37) |
All of the aggressive patients were secluded at some point. Physical restraint by nursing staff was required in about a third of the events. The immediate administration of additional medication in the form of as required neuroleptics either orally or intramuscularly was used in about two-thirds of the aggressive events. There was no difference in mean OAS score between events involving patients who did and did not have a history of drug or alcohol misuse (t=1.64, d.f.=122, P>0.1). However, there was a statistically significant difference (t=–4.14, d.f.=122, P<0.01) between the groups in terms of history of violence, with events involving patients having a history of violence having a higher mean OAS score than events involving patients with no such history.
There was no relationship between ethnicity and history of violence for non-European patients (χ2=0.067, d.f.=1, P>0.1). However, there was a relationship between ethnicity and a previous history of drug or alcohol misuse, with Maori patients more likely (80%) to have such a history than European patients (51%; χ2=6.492, d.f.=1, P<0.05).
Discussion
This study provides further information about the correlates of aggressive behaviour in a general adult psychiatric unit in New Zealand. Although generalisation of the results should be undertaken with caution, the study provides the first published information on these specific issues. The association of violence with male gender is well recognised (Reference DavisDavis, 1991; Reference Shah, Fineberg and JamesShah et al, 1991).
The finding that Maori and other non-European patients were more likely to be involved in aggressive incidents is interesting. It may reflect more severe psychopathology in this group of patients, which in turn may reflect cultural differences in service access, service utilisation or real differences in phenomenology. A higher proportion of Maori patients had a history of substance misuse, which may be another significant factor. Previous studies have suggested that aggressive behaviour in inpatient units often involves patients with schizophrenia and bipolar disorders (Reference TardiffTardiff, 1999), particularly those who are acutely psychotic or manic. Similarly, in our study, patients with schizophrenia, mania and those with substance misuse were most frequently involved in aggressive events. There is evidence for an increase in substance-related psychotic disorders over time (Reference Cantwell, Brewin and GlazebrookCantwell et al, 1999), it is therefore not surprising that 7% of our total sample were in that category. As the study recorded only the single, coded primary clinical diagnosis, comorbidity could not be considered. Our finding that nearly 70% of the aggressive episodes took place within the first week of admission is consistent with the view that stage or phase of illness, in terms of acuity or remission, is a useful predictor of violence (Reference DavisDavis, 1991), especially in the short term. Acutely ill patients are particularly vulnerable and may feel provoked or intimidated, especially if they are psychotic and admitted involuntarily. All of our patients who were involved in aggressive events were compulsorily detained. This is probably a reflection of the use of risk and violence as criteria for compulsory admission. The finding that most patients exhibiting aggressive behaviour were likely to be secluded is consistent with several studies (Reference James, Fineberg and ShahJames et al, 1990; Reference El-Badri and MellsopEl-Badri & Mellsop 2002).
There is a consensus that a history of aggressive behaviour is the best predictor of future violence (Reference DavisDavis, 1991; Reference Shah, Fineberg and JamesShah et al, 1991; Reference CrightonCrighton, 1995). In our study, 55% of patients who were aggressive had a history of previous violence and nearly 70% had a history of alcohol or drug misuse. Substance misuse among psychiatric patients has consistently been shown to be a significant risk factor for aggression and disturbed behaviour (Reference SoykaSoyka, 2000). In our sample, 54 aggressive patients (68%) had a history of alcohol or drug misuse. Substance misuse probably exacerbates psychotic symptoms and/or interacts with personality and other social variables and treatment nonadherence (Reference SoykaSoyka, 2000). In our study, over half of the aggressive events occurred in the evening and in most cases were directed against the nursing staff. Threats of violence and verbal aggression predominated, with serious physical aggression being less common. In the evening, however, aggressive episodes peaked at certain times. The first peak coincided with the change of shift and medication time (4–6 p.m.) and the second with bedtime (10 p.m.); these are times at which hospital rules are enforced. Setting limits on patient behaviour and attempting to accomplish specific tasks (including the administration of medication) have been noted to provoke aggressive behaviour (Reference Sheridan, Henrion and RobinsonSheridan et al, 1990; Reference TardiffTardiff, 1992; Reference Lance, Gallop and McCayLance et al, 1995). Furthermore, the skill of staff and their training in limit-setting and aggression control technique are equally important (Reference Infantino and MusingoInfantino & Musingo 1985). Staff skills, their attitude and experience, and staff–patient interactions are interrelated. These issues and the impact of the way hospital rules/regimes are enforced require further examination.
The usage of seclusion in New Zealand may be a practice awaiting an evidential base or a change in service culture.
In this unit, the average admission rate was 4 patients per day and the average bed occupancy was 84% during the study period. We did not find any significant relationship between aggressive episodes and bed occupancy or admission rates.
Declaration of interest
None.





eLetters
No eLetters have been published for this article.