CASE REPORT
Four adult patients presented to the emergency department (ED) for muscle pain at different times over two days in August 2016. They were three females and one male. Two of them were sisters living in the same household. Their ages ranged from 22 to 41 years. They were all healthy before the index illness. All had eaten varying amounts of cooked crayfish at the same local restaurant before the onset of symptoms. Muscle pain was their chief complaint. Sites of pain included the neck, shoulder, leg, waist, and back. One patient had nausea. Otherwise, gastrointestinal (GI) or constitutional symptoms were absent. The history of crayfish consumption was first elicited from the sisters as they presented to the ED at the same time with similar symptoms. As for the other two patients who presented later than the two sisters, the history of crayfish consumption was sought retrospectively. All patients had normal vital signs. Motor weakness was not present. They were hospitalized under the care of the ED. Their peak creatine kinase (CK) level ranged from 1,452 IU/L to 15,534 IU/L. None had renal impairment. Their urine was not tested for myoglobin. Intravenous (IV) fluid was administered to all because of the elevated CK level. Urine alkalization was instituted in the patient who had the highest admission and peak CK level. IV fluid therapy was stopped for these four patients when their CK level demonstrated a downward trend. Analgesics were prescribed for their muscle pain, but none required an analgesic stronger than oral paracetamol. All had a stable clinical course and were discharged without complications. Their clinical characteristics and laboratory findings are summarized in Table 1.
Table 1 Clinical characteristics and laboratory findings of the four patients
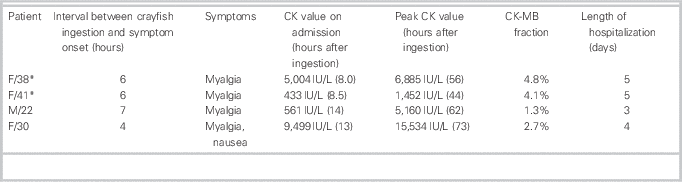
* These two patients are sisters.
CK=creatine kinase; CK-MB=creatine kinase MB isoenzyme.
DISCUSSION
These four patients experienced myalgia and rhabdomyolysis, or Haff disease, following the consumption of crayfish. Haff disease was first reported in what is now Kaliningrad more than 90 years ago.Reference Lentz 1 Thereafter, cases have been reported worldwide, although most cases have occurred in the United States and China. Sporadic cases or outbreaks were often subsequent to the consumption of certain cooked seafood.Reference Diaz 2 Many reported cases of Haff disease have been linked to the ingestion of cooked freshwater fish.Reference dos Santos, de Albuquerque and Pinto 3 , 4 Crustaceans, especially those freshwater bottom-feeders, are also associated with Haff disease. As for these four patients, crayfish was the culprit. In fact, crayfish accounts for most cases in China.Reference Chan 5 As crayfish have become a popular seafood dish, leading to their increased consumption, Haff disease may be considered an emerging crustacean-borne illness.Reference Chen, Yuan and Xie 6
Haff disease is a clinical syndrome characterized by myalgia and rhabdomyolysis that develops within 24 hours of the ingestion of cooked seafood. Its pathogenesis is believed to be because of a heat-stable toxin originating from saltwater algae that is present in seafood.Reference Diaz 2 It is believed to be a myotoxin that targets striated muscles. The exact nature of the toxin remains unclear. There has been postulation that palytoxin is the suspected agent in Haff disease.Reference Sud, Su, Greller, Majlesi and Gupta 7 However, in the seafood samples from 21 cases of Haff disease occurring in the United States, palytoxin was not identified.Reference Buchholz, Mouzin and Dickey 8 Further, palytoxin is a neurotoxin, but in Haff disease, neurotoxicity is absent. Therefore, it is less convincing that palytoxin is the cause of Haff disease.
In cases of Haff disease that develop after eating crayfish, besides myalgia, GI disturbance, e.g., nausea, vomiting, and abdominal pain, may be present.Reference Diaz 2 As evidenced by these four patients, myalgia is the most common presenting clinical feature. Unlike many other types of seafood-borne illnesses, neurotoxicity is absent. As the presenting symptoms of patients with Haff disease are sometimes non-specific, diagnosis in the ED may be difficult. In fact, Haff disease is rarely reported in Emergency Medicine literature. To avoid missing the diagnosis, Haff disease should be considered a differential diagnosis in patients presenting to the ED with myalgia, especially in the presence of GI symptoms. If it is suspected, an enquiry on seafood consumption within the 24 hours preceding symptom onset should be made, in addition to checking the CK level in the ED. In Haff disease, an elevated CK level indicating rhabdomyolysis is always present. In the four patients, their admission and peak CK levels varied widely. In general, CK is considered a marker of muscle injury severity. A higher level suggests more severe muscle damage. Whether this was the case in these 4 patients is uncertain. This is because the amount of crayfish eaten could not be ascertained. Thus, the amount of myotoxin to which they were exposed is unknown.
In the presence of seafood consumption and rhabdomyolysis, another differential diagnosis that emergency physicians need to consider is palytoxin poisoning. Palytoxins are a class of neurotoxins that may be carried by crustaceans, especially xanthid crabs, certain finfish species, anemone, and zoanthid corals.Reference Deeds and Schwartz 9 Palytoxin is a heat-stable neurotoxin produced by the Ostreopsis species of marine algae. Ingestion of xanthid crabs is the primary route of exposure. The toxins act on the membrane sodium-potassium pumps and convert ionic-specific pumps into non-specific cationic pores.Reference Deeds and Schwartz 9 The result is prolongation of depolarization leading to muscle spasm or seizure, which is absent in Haff disease. Rhabdomyolysis may develop as a result of the muscle spasms and seizures. Other clinical features include a bitter or metallic taste; GI disturbance such as abdominal pain, vomiting, and diarrhea; and bradycardia.Reference Alcala, Alcala, Garth, Yasumura and Yasumoto 10 , Reference Gonzales and Alcala 11 Treatment is supportive, and rhabdomyolysis can be prevented by adequate hydration.
Similar to rhabdomyolysis due to other conditions, renal damage is the most worrisome complication of Haff disease. Prevention of acute renal failure and its life-threatening complications, e.g., hyperkalemia, is therefore the mainstay of the treatment of Haff disease. Early IV fluid therapy is recommended for volume expansion. This is especially important in patients with Haff disease who are vomiting and at risk of dehydration. There is no guideline for the duration of fluid administration. It has been recommended that IV fluid should be continued until the CK level is below 1000 IU/L.Reference Walls, Hockberger and Gausche-Hill 12 However, it appears safe to discontinue IV fluid therapy when the CK level begins to drop, as exemplified by these four patients. The benefit of urine alkalinization in rhabdomyolysis is believed to be because of inhibition of the redox cycling of myoglobin and lipid peroxidation.Reference Walls, Hockberger and Gausche-Hill 12 However, its benefit in comparison to saline infusion alone is controversial. Urine alkalinization was used in the patient with the highest admission and peak CK level to help reduce the CK level. No conclusion on its additional benefits can be drawn because of the small number of patients studied. Overall, the prognosis of Haff disease is good. All four patients in this series were discharged from the hospital without any complications.
CONCLUSION
Four patients who experienced rhabdomyolysis, or Haff disease, after eating crayfish were described. Symptoms of Haff disease are often non-specific. In ED patients with myalgia, obtaining a history of seafood consumption and finding an elevated CK level are the key to the diagnosis of Haff disease. Prevention of acute renal failure with IV fluid for volume expansion is the mainstay of treatment.
Competing interests
None declared.



