Dementia has a huge impact globally: 46.8 million people were living with dementia in 2015, and this number is projected to almost double every 20 years (Prince et al., Reference Prince, Wimo, Guerchat, Ali, Wu and Prina2015). As national populations age and rates of dementia increase, it will become increasingly important to provide supports for people to live well with dementia. This means providing dementia care that is person-centred, seamless, and coordinated, and to provide support such that the needs of people with dementia and their caregivers are anticipated and met as they arise (Prince, Comas-Herrera, Knapp, Guerchet, & Karagiannidou, Reference Prince, Comas-Herrera, Knapp, Guerchet and Karaglannidou2016). The majority of people with dementia worldwide live in the community, most with the support of informal caregivers and/or community services (Gould & Basta, Reference Gould and Basta2013; Kasper, Freedman, Spillman, & Wolff, Reference Kasper, Freedman, Spillman and Wolff2015; Lepore, Ferrell, & Wiener, Reference Lepore, Ferrell and Wiener2017). A recent Canadian estimate suggested that, in 2016, 61 per cent of older adults (more than 261,000 individuals) with dementia were living in their own homes (Canadian Institute for Health Information, 2018), while data from the United States suggests approximately 81 per cent of individuals with dementia are community-dwelling (Lepore et al., Reference Lepore, Ferrell and Wiener2017). Community residence is particularly prevalent in low- and middle-income countries, with 94 per cent of people with dementia residing at home (and family providing most of the care) compared to 78 per cent in higher income countries (Alzheimer’s Disease International, 2009; Wimo, Jönsson, Bond, Prince, & Winblad, Reference Wimo, Jönsson, Bond, Prince and Winblad2013).
Individuals with dementia and their caregivers express a number of education and support needs that vary throughout the different stages of dementia, and services exist (particularly in higher-resource locations) that are intended to meet these needs. These include information resources, caregiver training/skill-building, support groups, counseling, respite care, care coordination programs, transportation services, delivery of groceries and meals, personal care, and care planning (Whitlatch & Orsulic-Jeras, Reference Whitlatch and Orsulic-Jeras2018). Such services can help support caregivers, as well as help people with dementia age in place. Although caregiver support and living well with dementia in the community are distinct concepts, many of these services benefit both caregivers and persons with dementia.
A growing body of literature suggests that education and support services for people with dementia and caregivers have positive effects, although these effects may be limited to specific outcomes, and some programs require further evidence of efficacy (Dam, de Vugt, Klinkenberg, Verhey, & van Boxtel, Reference Dam, de Vugt, Klinkenberg, Verhey and Boxtel2016; Dawson, Bowes, Kelly, Velzke, & Ward, Reference Dawson, Bowes, Kelly, Velzke and Ward2015; Dickinson et al., Reference Dickinson, Dow, Gibson, Hayes, Robalino and Robinson2017; Huis in het Veld, Verkaik, Mistiaen, van Meijel, & Francke, Reference Huis in het Veld, Verkaik, Mistiaen, van Meijel and Francke2015; Jensen, Agbata, Canavan, & McCarthy, Reference Jensen, Agbata, Canavan and McCarthy2015; Vandepitte et al., Reference Vandepitte, Van Den Noortgate, Putman, Verhaeghe, Verdonck and Annemans2016). For example, Dickinson et al. (Reference Dickinson, Dow, Gibson, Hayes, Robalino and Robinson2017) concluded in their meta-systematic review that well designed, multi-component psychosocial caregiver interventions increase psychological well-being in caregivers and delay institutionalization of people with dementia. Such interventions are an example of how support aimed specifically at caregiver well-being has also been found to help persons with dementia age in place longer. In a systematic review on respite care, day care (but not temporary admission respite) was found to decrease caregiver burden and stress as well as diminish reactive behaviours in people with dementia (Vandepitte et al., Reference Vandepitte, Van Den Noortgate, Putman, Verhaeghe, Verdonck and Annemans2016). A recent meta-analysis has suggested that although educational interventions for caregivers are not a panacea for supporting those with dementia to age in place, they have a moderate effect on caregiver burden and may decrease caregiver depression (Jensen et al., Reference Jensen, Agbata, Canavan and McCarthy2015).
While many support and education services for people with dementia and their caregivers have the potential to increase well-being and support living well with dementia, such services may not be readily available in lower-resource countries, and barriers to accessibility and use may exist even in high-income countries (World Health Organization, 2015). Rurality impacts the availability and accessibility of services, with geographic isolation, small and dispersed populations, and limited access to health professionals serving as barriers to rural health service delivery (Bourke, Humphreys, Wakerman, & Taylor, Reference Bourke, Humphreys, Wakerman and Taylor2012; Innes, Cox, Smith, & Mason, Reference Innes, Cox, Smith and Mason2006). Shortages of human health resources (including specialist services) and limited local health and support resources have been repeatedly reported in rural Canadian contexts (e.g., Canadian Home Care Association, 2006; Dal Bello-Haas, Cammer, Morgan, Stewart, & Kosteniuk, Reference Dal Bello-Haas, Cammer, Morgan, Stewart and Kosteniuk2014a; Morgan, Semchuk, Stewart, & D’Arcy, Reference Morgan, Semchuk, Stewart and D’Arcy2002; Morgan et al., Reference Morgan, Kosteniuk, Stewart, O’Connell, Kirk and Crossley2015). For example, Morgan et al. (Reference Morgan, Kosteniuk, Stewart, O’Connell, Kirk and Crossley2015) found that while most basic health care services were considered accessible to rural Saskatchewan residents affected by dementia, there was a paucity of services specifically for individuals with dementia and their caregivers (e.g., dementia screening, multidisciplinary team assessment, counseling and caregiver support groups, and dementia-specific long-term care services).
These issues are not unique to the Canadian context: Szymczynska, Innes, Mason, and Stark (Reference Szymczynska, Innes, Mason and Stark2011) identified limited access to diagnostic and post-diagnostic services for dementia as a significant issue for rural communities within Scotland, Canada, Tasmania, and Australia. Rural health care providers working with Canadian families affected by dementia have also reported professional isolation and the need for continuing education opportunities, which may affect their ability to provide best-quality care (Dal Bello-Haas et al., Reference Dal Bello-Haas, Cammer, Morgan, Stewart and Kosteniuk2014a; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Morgan, Innes, & Kosteniuk, Reference Morgan, Innes and Kosteniuk2011). These resource issues, along with transportation difficulties, may contribute to rural/urban inequities in dementia health care and support that have been identified in higher-income countries (Prince et al., Reference Prince, Comas-Herrera, Knapp, Guerchet and Karaglannidou2016).
Given the potential utility of support and education services for people with dementia and their caregivers to live well in their communities, it is important to identify the scope of services available to and needed by rural populations globally, and the existing barriers to their accessibility and use. Moreover, it is important to examine potential solutions to these barriers, in order to design dementia-related services that successfully meet support and education needs. The purpose of the current scoping review was therefore to investigate the support and education needs of people with dementia and their caregivers living in rural areas; availability and use of support and education services; barriers to access and use of services; and solutions to overcome these barriers. A scoping review allowed us to systematically map the research pertaining to these questions, to synthesize barriers and solutions that could be helpful for intervention development, and to identify gaps in knowledge.
Methods
This work was guided by Arksey and O’Malley’s (Reference Arksey and O’Malley2005) five-step framework for scoping reviews, with additional reference to Levac, Colquhoun, and O’Brien’s (Reference Levac, Colquhoun and O’Brien2010) recommendations. Additionally, the recently published guidelines for reporting scoping reviews (Tricco et al., Reference Tricco, Lillie, Zarin, O’Brien, Colquhoun, Levac and Straus2018) informed the final iteration of this article. The methodological stages outlined by Arksey and O’Malley involve (a) identifying the research question, (b) identifying relevant studies, (c) selecting the studies, (d) charting the data, and (e) collating, summarizing, and reporting the results. A protocol documenting the research questions and methods of this scoping review was created prior to commencing the review; this protocol was not documented for publication but can be requested from the corresponding author.
In line with Levac et al. (Reference Levac, Colquhoun and O’Brien2010), we adopted a team-based approach that involved the collaborative development of research questions, search strategies, and charting categories for this and other concurrent reviews. Our team consisted of all five authors, who met bi-weekly to discuss progress, challenges, and findings. Team members also acted as secondary independent reviewers during the screening process.
Identifying the Research Question
As suggested by Levac et al. (Reference Levac, Colquhoun and O’Brien2010), we carefully considered the review population, concepts, and outcomes of interest. People with dementia living in rural communities and their caregivers were the populations of interest, since support and education services are important for the well-being of both of these groups. To comprehensively explore dementia-related support and education services for residents of rural areas, six concepts were vital to consider: needs, availability, use, accessibility, barriers, and solutions. The following research questions were therefore developed: (a) What types of support service and education needs are being expressed by people with dementia and their caregivers in rural areas?; (b) What types of services are available and used?; (c) What are the reported barriers to service accessibility and use in these populations? and (d) What are the potential solutions to these barriers, identified by participants and reflected in support and education interventions?
Clarification of “support and education services” was achieved through a review of recent reports related to dementia care and support within the community (Health Quality Ontario, 2018; National Institute for Health and Care Excellence, 2010, 2013; United Kingdom Department of Health, 2013; World Health Organization, 2012;). Education services were defined as those providing education related to dementia, available services, self-care, resources and supports; or those providing care skills to people with dementia or their caregivers. Support services corresponded closely to those termed “human services” by Toseland et al. (Reference Toseland, McCallion, Gerber, Dawson, Gieryic and Guilamo-Ramos1999) and included daily/personal care, household tasks, social or recreational programs and support, transportation, end-of-life care, psychoeducation, individual support and counselling, support groups, and respite care.
Identifying Relevant Studies
Search terms were reviewed by a University Health Sciences librarian, and were related to dementia and Alzheimer’s disease, rurality, support (in the iterations described above), and education (see Table 1). After initial testing and refinement of terms, we performed the search on August 16, 2017, using the databases MEDLINE, CINAHL, PSYCINFO, and EMBASE. According to the purpose and scope of the review, we searched for articles from the past 20 years (1997–2017); this offered a relatively current perspective.
Table 1: Search terms used with EMBASE database

Note. “/” indicates MESH terms. All other terms were searched using .mp.
Study Selection
From the 2,381 references we identified, 1,261 remained after de-duplication in Endnote. These articles were uploaded into the review software DistillerSR. Titles and abstracts were reviewed by MB and a second reviewer (JK, VE) to determine whether they met the inclusion criteria (Table 2). Following the first round of exclusions, 174 articles remained for full-text independent review by MB and AFC. During both levels of review, all conflicts were resolved with a bias towards inclusion. Following full-text review (completed November 25), 83 articles remained at the onset of data charting. However, as noted by Levac et al. (Reference Levac, Colquhoun and O’Brien2010), the study selection and data charting are iterative processes, and we subsequently removed another 15 during charting mainly because they were descriptions of service models or too peripheral to the foci of this review (Figure 1).
Table 2: Criteria for inclusion in scoping review


Figure 1: PRISMA flow diagram of the study selection process
Charting the Data
The first author extracted relevant data from the 68 remaining articles, which were charted into a Microsoft Excel file that was pilot-tested and refined by the team prior to use. Charting categories included (a) author/s; (b) year; (c) country; (d) purpose of study; (e) type of study (descriptive or intervention); (f) brief description of intervention if applicable; (g) study sample (rurality, population description, sex, age, ethnicity, caregiving relationships, and dementia diagnoses); (h) definition of rural; (i) methodology; (j) service availability, accessibility, and use; (k) service needs; (l) barriers; (m) solutions; (n) outcomes (for intervention studies); (o) key findings/conclusions related to the scoping review questions; and (p) sex and gender-related findings. Data within these categories formed the basis of our analyses.
Collating, Summarizing, and Reporting the Results
As recommended by Levac et al. (Reference Levac, Colquhoun and O’Brien2010), we used extracted data to develop a descriptive overview of study characteristics (Table 3). Findings related to the main research concepts were derived through thematic analysis and description. Descriptive and intervention studies are reported separately because they largely answered different research questions. For each descriptive study (those that did not evaluate an intervention/programming), we reported data pertaining to education and support service needs, use, and availability, in addition to use and accessibility barriers that the study participants reported (Table 4). For each intervention study, a brief description and main outcomes are reported, along with ways the intervention incorporated solutions to use and accessibility barriers (Table 5). Finally, Table 6 depicts accessibility and use barriers with literature-based suggestions for how they can be ameliorated.
Table 3: Summary of study characteristics

a One article is represented in both columns, since its main foci pertained to both the assessment of educational needs and intervention evaluation.
b Includes everyone involved in service provision including frontline providers but also managers, directors of care, etc.
Table 4: Descriptive articles: Service needs, accessibility, use, and barriers

AD = Alzheimer’s disease, ADL = activities of daily living, CI = cognitive impairment, CG = caregiver, FTD = frontotemporal dementia, HSP = health/service providers, LBD = dementia with Lewy bodies, MCI = mild cognitive impairment, PND = persons without dementia, PWD = person/s with dementia, RN = registered nurse, VaD = vascular dementia
Table 5: Intervention articles: Outcomes and solutions to accessibility and use barriers
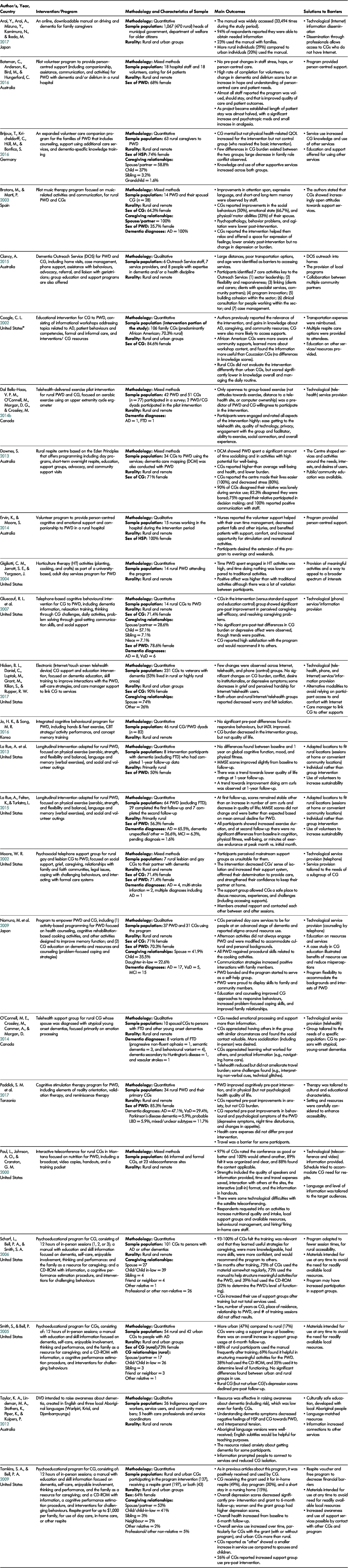
Note. AD = Alzheimer’s disease, ADL = activities of daily living, CG = caregiver, CI = cognitive impairment, FTD = frontotemporal dementia, HSP = health/service providers, IADL = instrumental activities of daily living, LBD = dementia with Lewy bodies, MCI = mild cognitive impairment, MMSE = Mini Mental State Examination, PND = person/s without dementia, PWD = person/s with dementia, RN = registered nurse, VaD = vascular dementia.
Table 6: Solutions to education and support service accessibility and use barriers

Findings
The 68 studies spanned multiple geographical settings, with the largest proportion (78%) conducted in North America (n = 38) and Europe (n = 15). Frequencies (see Table 3) illustrate a non-linear increase in the number of articles over the past 20 years. There was an emphasis on qualitative methodologies among descriptive articles and quantitative work in intervention articles. Of the quantitative intervention studies, three utilized a randomized control design (Brijoux, Kricheldorff, Hüll, & Bonfico, Reference Brijoux, Kricheldorff, Hüll and Bonfico2016; Glueckauf et al., Reference Glueckauf, Jeffers, Sharma, Massey, Shuford Davis, Wesley and Martin2007; Hicken et al., Reference Hicken, Daniel, Luptak, Grant, Kilian and Rupper2017), and one utilized a stepped wedge design (Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017). Although many studies described both education and support services, support services were more frequently addressed than education. Participants were primarily caregivers and people with dementia although many articles included health or service providers, and a minority involved other individuals including community members without dementia. Among participants with dementia, Alzheimer’s disease was the most frequently reported diagnosis, and some studies exclusively recruited people with Alzheimer’s and/or their caregivers (see Tables 4 and 5). When caregivers were included, the majority tended to be spouses/partners or daughters and daughters-in-law, with two studies focused specifically on sons (McDonnell & Ryan, Reference McDonnell and Ryan2014; Sanders & McFarland, Reference Sanders and McFarland2002).
The degree to which sex and gender were considered in this body of literature (and associated findings) was of interest, in line with efforts to better incorporate sex and gender into neurodegeneration research (Tierney, Curtis, Chertkow, & Rylett, Reference Tierney, Curtis, Chertkow and Rylett2017). Most authors reported the sex of participants. Consistent with the broader literature, the vast majority of caregivers studied were women, making up 61 per cent to 92 per cent of samples. Only one study (other than those focused on caregiving sons), from Australia, reported more male (10) than female (8) participants (Orpin, Stirling, Hetherington, & Robinson, Reference Orpin, Stirling, Hetherington and Robinson2014). Most studies also reported a higher proportion of female compared to male participants with dementia, as would be expected based on the higher prevalence of dementia among women (Prince et al., Reference Prince, Wimo, Guerchat, Ali, Wu and Prina2015). Few studies (Arai, Sugiura, Miura, Washio, & Kudo, Reference Arai, Sugiura, Miura, Washio and Kudo2000; Edelman, Kuhn, Fulton, & Kyrouac, Reference Edelman, Kuhn, Fulton and Kyrouac2006; Forbes, Morgan, & Janzen, Reference Forbes, Morgan and Janzen2006; Herron & Rosenberg, Reference Herron and Rosenberg2017; Li, Kyrouac, McManus, Cranston, & Hughes, Reference Li, Kyrouac, McManus, Cranston and Hughes2012; McDonnell & Ryan, Reference McDonnell and Ryan2014; Nordberg, von Strauss, Kåreholt, Johansson, & Wimo, Reference Nordberg, von Strauss, Kåreholt, Johansson and Wimo2005; Sanders & McFarland, Reference Sanders and McFarland2002; von Kutzleben, Reuther, Dortmann, & Holle, Reference von Kutzleben, Reuther, Dortmann and Holle2016) examined sex (biological status as male or female) or gender (the ways maleness or femaleness may be expressed through roles, behaviors, etc.) in relation to service needs, use, and barriers. Only one intervention study included sex as an independent variable (Tomkins & Bell, Reference Tomkins and Bell2009), and found that it did not significantly affect the intervention’s impact on depression, overall service use, or support group use.
Education and support programs/interventions for people with dementia and their caregivers in rural areas were evaluated in 24 articles from Canada, Spain, the United States, Tanzania, Australia, Korea, Japan, and Germany (see Table 5). All evaluations indicated favorable outcomes on at least some of the indices measured, suggesting benefits to rural populations. Support interventions for people with dementia included music therapy (Brotons & Marti, Reference Brotons and Marti2003); horticultural therapy within day programming (Gigliotti, Jarrott, & Yorgason, Reference Gigliotti, Jarrott and Yorgason2004); in-hospital support (Bateman, Anderson, Bird, & Hungerford, Reference Bateman, Anderson, Bird and Hungerford2016; Ervin & Moore, Reference Ervin and Moore2014); cognitive-behavioural and memory training (Jo & Song, Reference Jo and Song2016); physical and verbal exercise training (La Rue et al., Reference La Rue, Felten, Duschene, MacFarlane, Price, Zimmerman and Hafez2013; La Rue, Felten, & Turkstra, Reference La Rue, Felten and Turkstra2015), and cognitive stimulation therapy (Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017). Two support groups for caregivers were described (Moore, Reference Moore2002; O’Connell, Crossley, Cammer, & Morgan, Reference O’Connell, Crossley, Cammer and Morgan2014), and an exercise intervention was aimed at both caregivers and people with dementia (Dal Bello-Haas et al., Reference Dal Bello-Haas, Cammer, Morgan, Stewart and Kosteniuk2014a). Education-based interventions were primarily targeted towards caregivers and included information on dementia, patient behaviours, formal and informal care, resources and supports, driving, and nutrition (Coogle, Reference Coogle2002; Paul, Johnson, & Cranston, Reference Paul, Johnson and Cranston2000; Scharf, Bell, & Smith, Reference Scharf, Bell and Smith2006; Smith & Bell, Reference Smith and Bell2005; Taylor, Lindeman, Stothers, Piper, & Kuipers, Reference Taylor, Lindeman, Stothers, Piper and Kuipers2012; Tomkins & Bell, Reference Tomkins and Bell2009).
interventions implemented elements of both support and education, including (a) home visits; (b) case management and referral; (c) group and individual education on dementia and resources; (d) group support and counseling; (e) caregiver skill training on communication, problem solving, and behaviour management; (f) self-care; (g) advocacy; (h) day programming; and (i) respite (Brijoux et al., Reference Brijoux, Kricheldorff, Hüll and Bonfico2016; Clancy, Reference Clancy2015; Downes, Reference Downes2013; Glueckauf et al., Reference Glueckauf, Jeffers, Sharma, Massey, Shuford Davis, Wesley and Martin2007; Hicken et al., Reference Hicken, Daniel, Luptak, Grant, Kilian and Rupper2017; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009).
Education and Support Service Needs, Availability, and Use
Numerous education and support needs were identified, with a general need for greater information or support for persons with dementia and their caregivers frequently mentioned in qualitative work (see Table 4). The need for education about available resources and services was often highlighted by participants, including service/health providers (Burton, O’Connell, & Morgan, Reference Burton, O’Connell and Morgan2016; Coogle, Reference Coogle2002; Di Gregorio, Ferguson, & Wiersma, Reference Di Gregorio, Ferguson and Wiersma2015; Edelman et al., Reference Edelman, Kuhn, Fulton and Kyrouac2006; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Forbes et al., Reference Forbes, Morgan and Janzen2006; Gurayah, Reference Gurayah2015; Glueckauf et al., Reference Glueckauf, Stine, Bourgeois, Pomidor, Rom, Young and Ashley2005; Innes, Szymczynska, & Stark, Reference Innes, Szymczynska and Stark2014; O’Reilly & Strong, Reference O’Reilly and Strong1997; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011). When needs were ranked by importance or frequency, the top reported needs included information on dementia in general, treatments, coping with responsive behaviours and challenging symptoms, meaningful activities for the person with dementia, resources/supports, and caregiving and family dynamics (Buettner & Langrish, Reference Buettner and Langrish2001; Coogle, Reference Coogle2002; Edelman et al., Reference Edelman, Kuhn, Fulton and Kyrouac2006).
Our review suggests that while many needs were consistent across studies and participants (e.g., information about available resources), needs were also influenced by participants’ roles, geographical residence, and dementia stage. Edelman et al. (Reference Edelman, Kuhn, Fulton and Kyrouac2006) found that education and support needs often differed between Americans with dementia and their family caregivers, which is an important consideration for interventions. They also reported that while sex of the caregiver did not impact number of information needs, male care recipients reported interest in more topics compared to female care recipients. Sex was examined in another American sample by Li et al. (Reference Li, Kyrouac, McManus, Cranston and Hughes2012), who found that women were more likely to have unmet service needs compared to men. Two comparative studies suggested that rurality may also influence needs. Rural respondents in the United States rated education regarding understanding and treating dementia as most important while urban respondents most needed information on the emotional and psychological consequences of caregiving (Coogle, Reference Coogle2002); Buettner and Langrish (Reference Buettner and Langrish2001) found in their American sample that rural caregivers were almost twice as likely (79.3%) as urban caregivers (45.2%) to express the need for formal support with recreation for the person with dementia. Finally, information needs differed depending on the stage of dementia (Forbes et al. Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Forbes et al. Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012), and information was required at the time of diagnosis or prospectively in order to understand the progression of dementia, identify “next steps”, and plan for the future (Burton et al., Reference Burton, O’Connell and Morgan2016; Innes, Blackstock, Mason, Smith, & Cox Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Szymczynska and Stark2014; Sanders & McFarland, Reference Sanders and McFarland2002).
Rural participants faced resource challenges, with a majority of non-intervention studies reporting limited and insufficient availability of education and support services. Innes et al. (Reference Innes, Blackstock, Mason, Smith and Cox2005), for example, found that 78 per cent of participants (people with dementia and their caregivers in rural Scotland) reported gaps in available services. Similarly, only 48 per cent of physicians and 19.3 per cent of other health care providers in a rural Canadian sample reported that available support services for people with dementia and their caregivers were adequate (Dal Bello-Haas et al., Reference Dal Bello-Haas, Cammer, Morgan, Stewart and Kosteniuk2014a). Day programming and respite care (particularly in-home, evening, weekend, and emergency respite) were the specific supports most frequently identified as inadequate or unavailable, in articles from North America, Europe, and Australia (Dal Bello-Haas et al., Reference Dal Bello-Haas, Cammer, Morgan, Stewart and Kosteniuk2014a; Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Szymczynska and Stark2014; Mason, Blackstock, Cox, Innes, & Smith, Reference Mason, Blackstock, Cox, Innes and Smith2005; McDonnell & Ryan, Reference McDonnell and Ryan2014; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Morgan et al., Reference Morgan, Kosteniuk, Stewart, O’Connell, Kirk and Crossley2015; O’Reilly & Strong, Reference O’Reilly and Strong1997; Plunkett & Chen, Reference Plunkett and Chen2016; Putnam, Pickard, Rodriguez, & Shear, Reference Putnam, Pickard, Rodriguez and Shear2010; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011; Teel, Reference Teel2004). Several authors also reported insufficient or unavailable counseling and support services (Dal Bello-Haas et al., Reference Dal Bello-Haas, Cammer, Morgan, Stewart and Kosteniuk2014a; Morgan et al., Reference Morgan, Kosteniuk, Stewart, O’Connell, Kirk and Crossley2015; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011; Teel, Reference Teel2004).
Additionally, early stage support was inadequate in some communities (Herron et al., Reference Herron, Rosenberg and Skinner2016; Herron & Rosenberg, Reference Herron and Rosenberg2017; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005). Suggesting this is a rurality issue (and not an issue with dementia services in general), only 35 per cent of Bédard, Koivuranta, & Stuckey’s (Reference Bédard, Koivuranta and Stuckey2004) Canadian rural caregiver sample reported support services were available to them, compared to 88 per cent of their urban sample. Similarly, Alzheimer Society staff reported fewer services provided by other organizations (e.g., day programs) in rural compared to urban locations (Herron et al., Reference Herron, Rosenberg and Skinner2016). Particular gaps in services were reported for people with young onset dementia and those belonging to an ethnic or sexual minority group (McDonald & Heath, Reference McDonald and Heath2009; Moore, Reference Moore2002). Finally, limited choices in type, amount, and provider were identified even when services were available (Forbes et al., Reference Forbes, Ward-Griffin, Kloseck, Mendelsohn, St-Amant, DeForge and Clark2011; Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Innes, Sherlock, & Cox, Reference Innes, Sherlock and Cox2003; Kelsey & Laditka, Reference Kelsey and Laditka2006; Mason et al., Reference Mason, Blackstock, Cox, Innes and Smith2005; O’Reilly & Strong, Reference O’Reilly and Strong1997). Conversely, Orpin et al. (Reference Orpin, Stirling, Hetherington and Robinson2014) reported that caregivers in rural Tasmanian communities were generally satisfied with the availability, range, and quality of formal support they received, and Ervin & Reid (Reference Ervin and Reid2015) found that only a small minority of caregivers in rural Victoria, Australia, reported support services to be unavailable or did not use offered services.
The use of services among rural caregivers and persons with dementia varied significantly between study populations. Bédard et al. (Reference Bédard, Koivuranta and Stuckey2004) reported that only 15 per cent of the rural Canadian caregivers in their sample received formal support. Conversely, von Kutzleben et al. (Reference von Kutzleben, Reuther, Dortmann and Holle2016) found that only 15.5 per cent of the German caregivers in their study did not use formal services, although it should be noted that the latter study was conducted much more recently. Other proportions of service use in different populations/locations were as follows: All caregivers used at least two of the listed support and education services (Ervin & Reid, Reference Ervin and Reid2015, Australia); 35.8 per cent of caregivers used services (Li et al., Reference Li, Kyrouac, McManus, Cranston and Hughes2012, United States); 50 per cent of persons with dementia used services (Nordberg et al., Reference Nordberg, von Strauss, Kåreholt, Johansson and Wimo2005, Sweden); 37 per cent of caregivers used no services (Arai et al., Reference Arai, Sugiura, Miura, Washio and Kudo2000, Japan); over 25 per cent of families used no services (Sun, Kosberg, Kaufman, Leeper, & Burgin, Reference Sun, Kosberg, Kaufman, Leeper and Burgin2007, United States); and 23 per cent of caregivers used no services (Wenger, Scott, & Seddon, Reference Wenger, Scott and Seddon2002, United Kingdom). Nordberg et al. (Reference Nordberg, von Strauss, Kåreholt, Johansson and Wimo2005) found that men and women had comparable levels of formal care when dementia was “questionable”, but that men had more care compared to women with dementia at later stages of impairment.
When examining specific support services, those involving direct assistance to the person with dementia (e.g., help with activities of daily living or home care) and home maintenance were used most frequently (Arai et al., Reference Arai, Sugiura, Miura, Washio and Kudo2000; Burholt, Wenger, & Scott, Reference Burholt, Wenger and Scott1997; Ervin & Reid, Reference Ervin and Reid2015; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Forbes et al., Reference Forbes, Morgan and Janzen2006; von Kutzleben et al., Reference von Kutzleben, Reuther, Dortmann and Holle2016; Sun et al., Reference Sun, Kosberg, Kaufman, Leeper and Burgin2007; Wenger et al., Reference Wenger, Scott and Seddon2002). Reported use of support/self-help groups by caregivers and people with dementia was quite low, ranging from 4.8 per cent to 25 per cent (Buettner & Langrish, Reference Buettner and Langrish2001; Ervin & Reid, Reference Ervin and Reid2015; Forbes et al., Reference Forbes, Morgan and Janzen2006; Innes et al., Reference Innes, Sherlock and Cox2003; Sun et al., Reference Sun, Kosberg, Kaufman, Leeper and Burgin2007). Ervin and Reid found that even among Australian caregivers with self-reported moderate to severe depression, anxiety, and stress, less than half (36–46%) attended support groups and even fewer utilized counseling or home respite. Consistent with these findings, service providers in Canada reported that existing rural support groups were underutilized (Herron et al., Reference Herron, Rosenberg and Skinner2016).
Few studies comparing urban and rural samples, however, found differences in use of specific services. Burholt et al. (Reference Burholt, Wenger and Scott1997) reported that people with dementia living in rural areas of the United Kingdom were more likely to receive a package of five or more social care services compared to their urban counterparts. Kosloski, Schaefer, Allwardt, Montgomery, & Karner, (Reference Kosloski, Schaefer, Allwardt, Montgomery and Karner2002) found that American urban caregivers used more average monthly hours of day care and respite (46.2) compared to rural users (35.3); use appeared to be linked to attitudes about caregiving and perceptions of services. Buettner and Langrish (Reference Buettner and Langrish2001) found that over half of the American rural caregivers in their study participated in Alzheimer’s education activities, which was significantly higher than the urban caregivers. There were no significant differences in use of support groups, counselling, legal or financial planning, case management, home modification, and homecare and other forms of home support visits (public and private home help, social workers, meals on wheels, voluntary helper, respite night sitters) (Buettner & Langrish, Reference Buettner and Langrish2001; Burholt et al., Reference Burholt, Wenger and Scott1997; Forbes et al., Reference Forbes, Morgan and Janzen2006).
Barriers to Accessibility and Use
Our review suggests multiple barriers to accessibility and use of support and education services by people with dementia and their caregivers living in rural areas (Table 4). Barriers reflected five general themes, delineated below: (a) knowledge of services, (b) practicality and resources, (c) values and beliefs, (d) negative judgments and stigma, and (e) unacceptability of services. Since barriers were often reported within qualitative studies that had a broader focus, little information exists about which barriers are most significant from the perspectives of service users.
Knowledge of Services
Poor awareness of available or eligible services was described within six articles, spanning Canada, the United States, and Scotland (Di Gregorio et al., Reference Di Gregorio, Ferguson and Wiersma2015; Forbes et al., Reference Forbes, Morgan and Janzen2006; Glueckauf et al., Reference Glueckauf, Stine, Bourgeois, Pomidor, Rom, Young and Ashley2005; Herron et al., Reference Herron, Rosenberg and Skinner2016; Innes et al., Reference Innes, Szymczynska and Stark2014; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). Di Gregorio et al. (Reference Di Gregorio, Ferguson and Wiersma2015) concluded that a lack of awareness regarding services was common, and that there were limited presence and visibility of organizations providing dementia-related education and support in rural northern communities. Service providers reported higher visibility of their dementia-related support and education services in urban compared to rural areas, with lack of knowledge as a barrier to use (Herron et al. Reference Herron, Rosenberg and Skinner2016). Moreover, Forbes et al. (Reference Forbes, Morgan and Janzen2006) found not knowing where to go for services was a unique barrier for their rural sample of people with dementia. In addition to poor awareness of services, families may be unaware of their potential benefits (Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002).
Practicality and Resources
Practicality and resource barriers were factors that made it logistically difficult to access or use services. The most frequently reported were geographic distance and transportation, identified in 15 studies across Canada, Scotland, Tanzania, and Australia (Andrews, Morgan, & Stewart, Reference Andrews, Morgan and Stewart2010; Clancy, Reference Clancy2015; Di Gregorio et al., Reference Di Gregorio, Ferguson and Wiersma2015; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Herron et al., Reference Herron, Rosenberg and Skinner2016; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Cox, Smith and Mason2006; Innes et al., Reference Innes, Sherlock and Cox2003; Innes et al., Reference Innes, Szymczynska and Stark2014; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Morgan et al., Reference Morgan, Kosteniuk, Stewart, O’Connell, Kirk and Crossley2015; O’Reilly & Strong, Reference O’Reilly and Strong1997; Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017; Plunkett & Chen, Reference Plunkett and Chen2016; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011). Services were not always locally available; therefore, distance and long travel times made access difficult (Di Gregorio et al., Reference Di Gregorio, Ferguson and Wiersma2015; Herron et al., Reference Herron, Rosenberg and Skinner2016; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Cox, Smith and Mason2006; Innes et al., Reference Innes, Sherlock and Cox2003; Innes et al., Reference Innes, Szymczynska and Stark2014; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Plunkett & Chen, Reference Plunkett and Chen2016; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011). Transportation was a large part of this challenge, reported by Innes et al. (Reference Innes, Blackstock, Mason, Smith and Cox2005) as the service gap most frequently identified by people with dementia and their caregivers. O’Reilly and Strong (Reference O’Reilly and Strong1997) reported that remote caregivers found it challenging to access services in town because the necessary bus was available only twice a day. Similarly, Forbes et al. (Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012) noted that because of long distances between respite locations and service users, transportation was generally not offered by organizations. Other challenges with transportation included costs, access to a vehicle, travel time, poor roads, and dependence on others (Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Sherlock and Cox2003; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011; Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017).
Financial barriers were identified in eight studies, with costs of services prohibitive for some individuals in Canada, the United Kingdom, Scotland, Australia, and the United States (Andrews et al., Reference Andrews, Morgan and Stewart2010; Clarke & Bailey, Reference Clarke and Bailey2016; Forbes et al., Reference Forbes, Morgan and Janzen2006; Innes et al., Reference Innes, Cox, Smith and Mason2006; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; O’Reilly & Strong, Reference O’Reilly and Strong1997; Putnam et al., Reference Putnam, Pickard, Rodriguez and Shear2010; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011; Herron et al., Reference Herron, Rosenberg and Skinner2016). Morgan et al. (Reference Morgan, Semchuk, Stewart and D’Arcy2002) noted that cost was a barrier despite subsidization of services for their Canadian participants, which may be influenced by a reluctance to spend hard-earned money. Socioeconomic status and high costs of (remote) living negatively affected accessibility (Andrews et al., Reference Andrews, Morgan and Stewart2010; Herron et al., Reference Herron, Rosenberg and Skinner2016; & Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011), and Putnam et al. (Reference Putnam, Pickard, Rodriguez and Shear2010) noted that “making too much money” could also cause difficulty paying for services (e.g., reduced eligibility for subsidization).
Other practicality and resource barriers included lack of adequate respite so caregivers could access services (Herron et al., Reference Herron, Rosenberg and Skinner2016; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002), and difficulties getting the person with dementia to day care or out-of-home respite, which could be very disruptive (Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Orpin et al., Reference Orpin, Stirling, Hetherington and Robinson2014). Additionally, the structure of service provision was noted as a barrier. Insufficient time with health and service providers impacted information dissemination/education and provider awareness of needs (Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011), and the process of trying to obtain services (e.g., being on a waiting list) affected accessibility (Forbes et al., Reference Forbes, Morgan and Janzen2006; Wenger et al., Reference Wenger, Scott and Seddon2002).
Values and Beliefs
Independence was the most commonly described value (identified in six articles from Canada, the United Kingdom, and Australia) that hindered service use, as it was coupled with reluctance to ask for or accept help (Clarke & Bailey, Reference Clarke and Bailey2016; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Herron & Rosenberg, Reference Herron and Rosenberg2017; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; O’Reilly & Strong, Reference O’Reilly and Strong1997; Wenger et al., Reference Wenger, Scott and Seddon2002). Herron and Rosenberg (Reference Herron and Rosenberg2017) described how the salience of independence among their rural Canadian sample of people with dementia and their caregivers contributed to delays accessing support services. Similarly, Forbes (Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012) noted caregiver reluctance to impose on others and the desire to conserve resources until services were desperately needed. The emphasis on independence and self-sufficiency was often described as part of the cultural context of rural communities. Some of the qualitative studies from Canada and Japan suggested beliefs around gender and social roles may also deter service use, with men emphasizing independence and fear of emasculation (Herron & Rosenberg, Reference Herron and Rosenberg2017) and care perceived as women’s duty (Arai et al., Reference Arai, Sugiura, Miura, Washio and Kudo2000; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). Participants also valued privacy and had concerns around confidentiality related to service use (Glueckauf et al., Reference Glueckauf, Stine, Bourgeois, Pomidor, Rom, Young and Ashley2005; Herron et al., Reference Herron, Rosenberg and Skinner2016; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002).
Beliefs around caregiving and dementia, particularly the idea that family should be performing the caregiving role, could also be barriers to the use of support services as reported in studies from Canada, Scotland, and Australia (Andrews et al., Reference Andrews, Morgan and Stewart2010; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Szymczynska and Stark2014; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Orpin et al., Reference Orpin, Stirling, Hetherington and Robinson2014). Andrews et al. (Reference Andrews, Morgan and Stewart2010) described Canadian northern values around family and respect for older adults as being paramount, and dependence on family members as caregivers. Caregivers were reluctant to entrust responsibility to support providers and reported guilt related to doing so (Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Orpin et al., Reference Orpin, Stirling, Hetherington and Robinson2014); guilt was a reason that caregivers refused services (Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005). Denial and lack of awareness of symptoms were also barriers, when people with dementia believed they did not need services or information (Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Herron et al., Reference Herron, Rosenberg and Skinner2016; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002).
Negative Judgments and Stigma
Stigma was reported as a barrier to service use within 10 articles, spanning Canada, Japan, the United States, and Scotland (Arai et al., Reference Arai, Sugiura, Miura, Washio and Kudo2000; Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Forbes et al., Reference Forbes, Ward-Griffin, Kloseck, Mendelsohn, St-Amant, DeForge and Clark2011; Glueckauf et al., Reference Glueckauf, Stine, Bourgeois, Pomidor, Rom, Young and Ashley2005; Herron & Rosenberg, Reference Herron and Rosenberg2017; Herron et al., Reference Herron, Rosenberg and Skinner2016; Innes et al., Reference Innes, Cox, Smith and Mason2006; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009). For example, Forbes et al. (Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012) reported caregiver reluctance to disclose a diagnosis and need for help because of stigma around dementia. Fear of stigma was noted as a significant barrier to services where there might be people known to the prospective users (Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Forbes et al., Reference Forbes, Ward-Griffin, Kloseck, Mendelsohn, St-Amant, DeForge and Clark2011; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). Participants in two studies, from the United States and Canada, described the desire of family caregivers to protect the person with dementia from stigma as being characteristic of small rural communities (Glueckauf et al., Reference Glueckauf, Stine, Bourgeois, Pomidor, Rom, Young and Ashley2005; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). People with dementia also described avoidance of social and recreational activities due to fear of negative judgments (Herron & Rosenberg, Reference Herron and Rosenberg2017). Arai et al. (Reference Arai, Sugiura, Miura, Washio and Kudo2000) reported that their sample of Japanese caregivers were concerned about what other people would think or say about service use, perceived stigma around the use of support services (see also Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009), and feared negative judgments from professionals regarding their house (e.g., cleanliness) or caregiving. Stigma appeared to be of particular concern for daughters and daughters-in-law, who were expected to be dutiful caregivers. The authors’ quantitative findings showed that caregiver concern over the judgments of others deterred service use.
Unacceptability of Services
Perceptions of services as inappropriate or inadequate were identified in 17 studies, from Canada, Japan, Scotland, Ireland, the United States, Japan, and Australia (Clarke & Bailey, Reference Clarke and Bailey2016; Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Forbes et al., Reference Forbes, Morgan and Janzen2006; Herron & Rosenberg, Reference Herron and Rosenberg2017; Herron et al., Reference Herron, Rosenberg and Skinner2016; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Cox, Smith and Mason2006; Innes et al., Reference Innes, Sherlock and Cox2003; Innes et al., Reference Innes, Szymczynska and Stark2014; McDonnell & Ryan, Reference McDonnell and Ryan2014; Moore, Reference Moore2002; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009; Orpin et al., Reference Orpin, Stirling, Hetherington and Robinson2014; O’Reilly & Strong, Reference O’Reilly and Strong1997; Putnam et al., Reference Putnam, Pickard, Rodriguez and Shear2010; Wenger et al., Reference Wenger, Scott and Seddon2002). Information was not always in an appropriate format for families (for example, the reading level was too difficult or information was presented poorly), and service providers reported that standardized educational material could be intimidating (Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Herron & Rosenberg, Reference Herron and Rosenberg2017; Innes et al., Reference Innes, Szymczynska and Stark2014). Support services were perceived by many participants as unsuitable or inadequate because they were distressing or disruptive to the person with dementia, were not suited to their current stage of dementia, were not in a preferred format (e.g., in-home or individual support), and were inflexible (Clarke & Bailey, Reference Clarke and Bailey2016; Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Herron & Rosenberg, Reference Herron and Rosenberg2017; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Sherlock and Cox2003; McDonnell & Ryan, Reference McDonnell and Ryan2014; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009; Orpin et al., Reference Orpin, Stirling, Hetherington and Robinson2014; O’Reilly & Strong, Reference O’Reilly and Strong1997). Sons appeared to favour a problem-focused coping style (McDonnell & Ryan, Reference McDonnell and Ryan2014), and reported available support groups to be unhelpful due to their focus on emotional support rather than caregiver education (Sanders & McFarland, Reference Sanders and McFarland2002).
Lack of person-centredness also elicited perceptions of services as unsuitable; many caregivers and people with dementia felt services did not fit their or the person with dementia’s personal characteristics, interests, and needs (Clarke & Bailey, Reference Clarke and Bailey2016; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Herron & Rosenberg, Reference Herron and Rosenberg2017; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Innes et al., Reference Innes, Szymczynska and Stark2014; McDonnell & Ryan, Reference McDonnell and Ryan2014; Moore, Reference Moore2002). Caregivers and people with dementia in Herron and Rosenberg’s (Reference Herron and Rosenberg2017) Canadian research delayed accessing support services because they were perceived as inadequate for their needs, assumed lack of abilities (treated users like children), and did not reflect participants’ personal and gendered interests. Similarly, Innes et al. (Reference Innes, Blackstock, Mason, Smith and Cox2005) reported that 26/45 caregivers and people with dementia in their study in Scotland rejected services offered to them because they were unsuitable for their needs, inflexible, and not person-centred. Rurality made it more difficult to find services that were acceptable and a good fit, as options were limited (Innes et al., Reference Innes, Cox, Smith and Mason2006; Mason et al., Reference Mason, Blackstock, Cox, Innes and Smith2005; Putnam et al., Reference Putnam, Pickard, Rodriguez and Shear2010). Moreover, two Canadian studies reported that low continuity of rural support services, volunteers, and staff decreased accessibility and use, and fostered distrust (Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Herron et al., Reference Herron, Rosenberg and Skinner2016).
Solutions to Accessibility and Use Barriers
Potential solutions to barriers were suggested within descriptive studies and evident in the design and implementation of interventions and programs. Most of these solutions coalesced around six themes, described below: (a) technological service provision, (b) a “point of entry” to services, (c) accessibility considerations and assistance, (d) inter-organization collaboration, (e) education, and (f) tailored or person-centred services. A full list of solutions identified in the literature and the barriers they could mitigate are presented in Table 6.
Technological Service Provision
Many of the support and education interventions developed for rural populations employed the use of information and communication technologies, including the Internet as a means of information dissemination (Arai, Arai, Mizuno, Kamimura, & Ikeda, Reference Arai, Arai, Mizuno, Kamimura and Ikeda2017), telehealth/teleconference (Dal Bello-Haas, O’Connell, Morgan, & Crossley, Reference Dal Bello-Haas, O’Connell, Morgan and Crossley2014b; Hicken et al., Reference Hicken, Daniel, Luptak, Grant, Kilian and Rupper2017; O’Connell et al., Reference O’Connell, Crossley, Cammer and Morgan2014; Paul et al., Reference Paul, Johnson and Cranston2000), and telephone (Glueckauf et al., Reference Glueckauf, Jeffers, Sharma, Massey, Shuford Davis, Wesley and Martin2007; Moore, Reference Moore2002; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009). Arai et al. (Reference Arai, Arai, Mizuno, Kamimura and Ikeda2017), for example, created an online downloadable manual for family caregivers about driving and dementia; Paul et al. (Reference Paul, Johnson and Cranston2000) held an interactive teleconference for rural caregivers focused on nutrition for people with dementia; and Glueckauf et al. (Reference Glueckauf, Jeffers, Sharma, Massey, Shuford Davis, Wesley and Martin2007) developed a telephone-based cognitive behavioural intervention for rural caregivers. Participants in non-intervention studies also reported the usefulness of technologies to deliver information and support to rural populations (Herron et al., Reference Herron, Rosenberg and Skinner2016; O’Reilly & Strong, Reference O’Reilly and Strong1997; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011). Further supporting the use of technologies, Burton et al. (Reference Burton, O’Connell and Morgan2016) found that 100 per cent of the rural Canadian caregivers and people with dementia who were interested in cognitive rehabilitation would prefer this support via telehealth compared to in-person. Technical difficulties, however, were noted within Canadian and American studies as a potential issue with the use of telehealth/conferencing (Dal Bello-Haas, O’Donnell, Morgan, & Crossley, Reference Dal Bello-Haas, O’Connell, Morgan and Crossley2014b; Paul et al., Reference Paul, Johnson and Cranston2000; O’Connell et al., Reference O’Connell, Crossley, Cammer and Morgan2014). Using multiple modalities of support and education provision can mitigate technical difficulties and user discomfort with, or lack of access to, particular technologies (Hicken et al., Reference Hicken, Daniel, Luptak, Grant, Kilian and Rupper2017; Paul et al., Reference Paul, Johnson and Cranston2000).
A “Point of Entry” to Service Use
Service use may be facilitated by having a “point of entry”, such as a case manager, trusted health care or service provider, an Alzheimer Society First Link program, or initial participation in a support or education intervention. An outcome reported in several intervention studies was participants’ increased knowledge of, openness to, and use of additional support services (Brijoux et al., Reference Brijoux, Kricheldorff, Hüll and Bonfico2016; Brotons & Marti, Reference Brotons and Marti2003; Scharf et al., Reference Scharf, Bell and Smith2006; Taylor et al., Reference Taylor, Lindeman, Stothers, Piper and Kuipers2012; Tomkins & Bell, Reference Tomkins and Bell2009). Alzheimer Society service providers described the importance of early connections with families, through First Link, home visits, or telephone consultations (Herron et al., Reference Herron, Rosenberg and Skinner2016). Orpin et al. (Reference Orpin, Stirling, Hetherington and Robinson2014) similarly reported that almost all caregivers had developed a strong relationship with one provider, who was a connection point into the system (see also Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012). As part of their caregiver education and support intervention, Hicken et al. (Reference Hicken, Daniel, Luptak, Grant, Kilian and Rupper2017) included a care manager who monitored participants’ intervention progress, maintained regular contact with participants and answered their questions, and assisted with referrals. Further demonstrating the utility of such an approach, Sun et al. (Reference Sun, Kosberg, Kaufman, Leeper and Burgin2007) found that caregivers with a case manager reported greater use of other services.
Accessibility Assistance
Participants identified, and some interventions included, non-technological accessibility assistance to facilitate service use. Accessibility considerations for rural populations in Canada, Scotland, Australia, Tanzania, and the United States involved structural decisions around programming such as the provision of in-home and outreach or local services, reduced program sessions, and convenient timing of programming (Clancy, Reference Clancy2015; Innes et al., Reference Innes, Cox, Smith and Mason2006; La Rue et al., Reference La Rue, Felten, Duschene, MacFarlane, Price, Zimmerman and Hafez2013; La Rue et al., Reference La Rue, Felten and Turkstra2015; Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017; Paul et al., Reference Paul, Johnson and Cranston2000; Scharf et al., Reference Scharf, Bell and Smith2006). For example, La Rue et al. (Reference La Rue, Felten, Duschene, MacFarlane, Price, Zimmerman and Hafez2013) held intervention sessions (physical exercise and language and memory stimulation) in participants’ homes or convenient places in the community. Home visits were noted as an important solution to accessibility issues by Alzheimer Society service providers (Herron et al., Reference Herron, Rosenberg and Skinner2016). Pragmatic assistance with costs, transportation, and respite were also identified as important to ameliorate accessibility and use barriers, and were reflected in some programs (Coogle, Reference Coogle2002; Innes et al., Reference Innes, Cox, Smith and Mason2006; Kelsey & Laditka, Reference Kelsey and Laditka2006; Tomkins & Bell, Reference Tomkins and Bell2009). Approximately 75 per cent of the dementia service providers in Innes et al.’s (Reference Innes, Cox, Smith and Mason2006) research provided transportation to users, and more than half of the day program directors surveyed by Kelsey and Laditka (Reference Kelsey and Laditka2006) emphasized their efforts to reduce cost barriers. Tomkins and Bell (Reference Tomkins and Bell2009) included a voucher for respite costs as a branch of their intervention, which increased the use of other services.
Inter-organization Collaboration
Collaboration between organizations and sectors was suggested as a feature of high-quality service provision and a way to enhance service accessibility (Clancy, Reference Clancy2015; Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; Innes et al., Reference Innes, Cox, Smith and Mason2006; Mason et al., Reference Mason, Blackstock, Cox, Innes and Smith2005; McDonald & Heath, Reference McDonald and Heath2009; O’Reilly & Strong, Reference O’Reilly and Strong1997). Service providers in Innes et al.’s (Reference Innes, Cox, Smith and Mason2006) research reported that effective partnerships with other agencies allowed them to share knowledge, funding, and transportation schemes, strengthening the accessibility and quality of services (see also Mason et al., Reference Mason, Blackstock, Cox, Innes and Smith2005). Strong communication and ties between organizations could facilitate referrals to appropriate services and increase caregiver support at an early stage (Forbes et al., Reference Forbes, Finkelstein, Blake, Gibson, Morgan, Markle-Reid and Thiessen2012; O’Reilly and Strong, Reference O’Reilly and Strong1997). Recruitment of volunteer assistance in service provision was also perceived to increase the quality and quantity of services (McDonald & Heath), and as a potential strategy to increase their sustainability (La Rue et al., Reference La Rue, Felten, Duschene, MacFarlane, Price, Zimmerman and Hafez2013; La Rue et al., Reference La Rue, Felten and Turkstra2015).
Education
Public and caregiver education on dementia and available resources was identified as important to ameliorate knowledge, beliefs and values, and stigma barriers to service use (Herron et al., Reference Herron, Rosenberg and Skinner2016; Morgan et al., Reference Morgan, Semchuk, Stewart and D’Arcy2002). Participants in Morgan et al.’s (Reference Morgan, Semchuk, Stewart and D’Arcy2002) work suggested caregivers need education on available resources in a way that helps them make connections to their own life and illustrates potential benefits. The need for better community education (including increased visibility of people with dementia) was also noted as a way to reduce stigma. Such public and community education was provided, along with a variety of other services, by the Hawthorn House in Australia (Downes, Reference Downes2013). An educational DVD developed by Taylor et al. (Reference Taylor, Lindeman, Stothers, Piper and Kuipers2012) for Aboriginal Australians was also a resource for the public in addition to caregivers. Education on available resources for people with dementia and their caregivers was a major component of some interventions (Brijoux et al., Reference Brijoux, Kricheldorff, Hüll and Bonfico2016; Coogle, Reference Coogle2002; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009). For example, the educational intervention developed by Coogle (Reference Coogle2002) included directories of local resources in the target communities, and workshops included information on resources and services. Nomura et al. (Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009) used a case study example as part of caregiver education to illustrate the potential benefits of support service use and reduce misperceptions; this strategy reduced caregiver reluctance to use services.
Tailored and Person-Centred Services
Tailoring services to a specific population, and providing person-centred services, were important aspects of many interventions (Bateman et al., Reference Bateman, Anderson, Bird and Hungerford2016; Downes, Reference Downes2013; Ervin & Moore, Reference Ervin and Moore2014; Gigliotti et al., Reference Gigliotti, Jarrott and Yorgason2004; Moore, Reference Moore2002; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009; O’Connell et al., Reference O’Connell, Crossley, Cammer and Morgan2014; Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017; Paul et al., Reference Paul, Johnson and Cranston2000; Taylor et al., Reference Taylor, Lindeman, Stothers, Piper and Kuipers2012). Moore (Reference Moore2002) developed a support group tailored to the needs of rural gay and lesbian caregivers in the United States, who had previously struggled to access suitable supports. Similarly, sharing support with people who have similar circumstances, ages, and life situations was of immense benefit to spousal caregivers to people with atypical young-onset dementias (O’Connell et al., Reference O’Connell, Crossley, Cammer and Morgan2014).
Consideration of cultural factors in service provision, including language-appropriate resources, was also important (Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009; Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011; Taylor et al., Reference Taylor, Lindeman, Stothers, Piper and Kuipers2012). In the development of their cognitive stimulation therapy in rural Tanzania, Paddick et al. (Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017) considered the cultural context and educational backgrounds of participants by finding appropriate buildings for sessions, timing them to fit around household work, farming, and village ceremonies, and considering participants’ knowledge and experiences when designing tasks. Taylor et al. (Reference Taylor, Lindeman, Stothers, Piper and Kuipers2012) emphasized the importance of culturally safe services, and concluded that incorporating Aboriginal languages and localizing content enhanced participant engagement with their educational intervention. Paul et al. (Reference Paul, Johnson and Cranston2000) ensured that the language and level of information in their nutrition education was tailored to their target audience. A direct educational approach may also be advantageous, so that caregivers and people with dementia can ask questions and information can be tailored to families (Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Innes et al., Reference Innes, Szymczynska and Stark2014; Paul et al., Reference Paul, Johnson and Cranston2000).
Person-centred interventions which took into account users’ personal backgrounds, characteristics, interests, and desires were also described (Bateman et al., Reference Bateman, Anderson, Bird and Hungerford2016; Downes, Reference Downes2013; Ervin & Moore, Reference Ervin and Moore2014; Gigliotti et al., Reference Gigliotti, Jarrott and Yorgason2004; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009; Paddick et al., Reference Paddick, Mkenda, Mbowe, Kisoli, Gray, Dotchin and Walker2017). Gigliotti et al (Reference Gigliotti, Jarrott and Yorgason2004) included horticultural activities in day programming to provide a broader range of activities that participants perceived as meaningful. In the hospital support programs, volunteers learned the personal characteristics and interests of patients so they could engage them in meaningful and enjoyable conversation and activities (Bateman et al., Reference Bateman, Anderson, Bird and Hungerford2016; Ervin & Moore, Reference Ervin and Moore2014). A key element of the Hawthorn House was that services were individualized and supported users’ needs, interests, and desires; evaluation of these services was very positive (Downes, Reference Downes2013). Flexibility was identified as necessary to adapt services to rural contexts and individual needs (Clancy, Reference Clancy2015; Innes et al., Reference Innes, Blackstock, Mason, Smith and Cox2005; Nomura et al., Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009; Smith et al., Reference Smith, Flicker, Shadforth, Carroll, Ralph, Atkinson and LoGuidice2011). For example, after realizing the importance of spirituality to their elderly Japanese service users, Nomura et al. (Reference Nomura, Makimoto, Kato, Shiba, Matsuura, Shigenobu and Ikeda2009) adapted their cognitive rehabilitation intervention to include temples and shrines as settings for the recall of autobiographical memories. Person-centred services were identified as a priority by participants in McDonald and Heath’s (Reference McDonald and Heath2009) research, and a person-centred perspective was implemented in day programs by learning the past hobbies, interests, and current preferences of users, changing programming to match interests and desires, providing meaningful activities, creating comfortable settings, and regularly evaluating activities from users’ perspectives (Kelsey & Laditka, Reference Kelsey and Laditka2006).
Discussion
The current review investigated the education and support needs of people with dementia and their caregivers living in rural areas, the availability and use of education and support services, barriers to these services, and solutions to identified barriers. Findings suggested that in the majority of rural populations studied, there were limited and insufficient services available to people with dementia and their caregivers. Specific gaps included day programming and respite care, counseling and support services, early stage support, and services for minority groups. Moreover, low density of services meant that participants had little choice in services regardless of fit. This limited service availability is in contrast to studies not focused on rural populations, wherein the presence of available services is often not perceived as an issue (e.g., Brodaty, Thomson, Thompson, & Fine, Reference Brodaty, Thomson, Thompson and Fine2005; Macleod, Tatangelo, McCabe, & You, Reference Macleod, Tatangelo, McCabe and You2017; Robinson et al., Reference Robinson, Elder, Emden, Lea, Turner and Vickers2009). Organizational “rationing” of services, insular rural culture, transportation costs, and difficulty accessing communities were identified as barriers to service development in rural communities (McDonald and Health, Reference McDonald and Heath2009).
Use of education and support services varied widely between studies, from 15 per cent of rural participants (Bédard et al., Reference Bédard, Koivuranta and Stuckey2004) to 100 per cent of rural caregivers surveyed (Ervin & Reid, Reference Ervin and Reid2015). Home maintenance and services providing direct assistance to the person with dementia, generally in-home, were used the most frequently, while minimal use of support groups was reported. Although studies comparing service use among urban and rural samples found few significant differences, it should be noted that studies reporting no differences (Buettner & Langrish, Reference Buettner and Langrish2001; Burholt et al., Reference Burholt, Wenger and Scott1997; Forbes et al., Reference Forbes, Morgan and Janzen2006) did not compare the services identified most frequently as unavailable in rural communities: day programs and different types of respite. Kosloski et al. (Reference Kosloski, Schaefer, Allwardt, Montgomery and Karner2002) did find urban participants used more monthly hours of day care and in-home respite compared to rural participants, although they did not assess population differences in use/non-use. Use findings are therefore relatively consistent with reported availability of services. The large amount of informal support reported by participants in several studies (Bédard et al., Reference Bédard, Koivuranta and Stuckey2004; Innes et al., Reference Innes, Sherlock and Cox2003; Li et al., Reference Li, Kyrouac, McManus, Cranston and Hughes2012; Nordberg et al., Reference Nordberg, von Strauss, Kåreholt, Johansson and Wimo2005; Wenger, Burholt, & Scott, Reference Wenger, Burholt and Scott1998; Wenger et al., Reference Wenger, Scott and Seddon2002) may also contribute to minimal levels of formal service use. For example, 85 per cent of the rural caregivers in Bédard et al.’s (Reference Bédard, Koivuranta and Stuckey2004) research received only informal support (compared to 33% of urban caregivers), but reported more total weekly hours of support than their urban counterparts. Wenger et al. (Reference Wenger, Burholt and Scott1998) reported that approximately three quarters of the assistance received by people with dementia was informal, generally from a relative living in the same residence. Strong informal community support networks were also described in several studies, where family, neighbours, and other community members looked out for the person with dementia and provided needed assistance (Di Gregorio et al., Reference Di Gregorio, Ferguson and Wiersma2015; Herron & Rosenberg, Reference Herron and Rosenberg2017; Innes et al., Reference Innes, Sherlock and Cox2003).
It is important to note that in terms of service use and availability, most of the focus in the reviewed articles was on instrumental support, such as meal preparation and respite, psychological support in the form of counseling or support groups (mainly for caregivers), and education about dementia and treatment. There are other forms of support for persons with dementia and their caregivers (e.g., support with sleep, communication, exercise, driving cessation, legal decision-making) that were not examined in articles assessing accessibility and use of rural support services. Additionally, less research focus was devoted to the availability or use of supports for understanding and responding to care recipient distress and behaviours, despite this being identified as a need and addressed in some intervention studies (e.g., Hicken et al., Reference Hicken, Daniel, Luptak, Grant, Kilian and Rupper2017; Glueckauf et al., Reference Glueckauf, Jeffers, Sharma, Massey, Shuford Davis, Wesley and Martin2007). When available, such supports may also be underutilized, as suggested by Ervin and Reid’s (Reference Ervin and Reid2015) finding that few (10%) of their rural Australian caregivers surveyed had used a Dementia Behaviour Management Advisory Service offering phone support, and 15 per cent did not know this service was available. Such support is beneficial, with reviews illustrating an association between what are often called “responsive behaviours” and caregiver burden and mental health issues (Ornstein & Gaugler, Reference Ornstein and Gaugler2012; Van der Lee, Bakker, Duivenvoorden, & Dröes, Reference van der Lee, Bakker, Duivenvoorden and Dröes2014). It is important, therefore, to understand the extent to which such supports are available and utilized by rural caregivers.
As our understanding of how to best support persons with dementia and their caregivers grows, there is also increasing recognition of the importance of social inclusion. Although the need for social inclusion was identified in some of the qualitative work reviewed (e.g., Forbes et al., Reference Forbes, Ward-Griffin, Kloseck, Mendelsohn, St-Amant, DeForge and Clark2011), it was unclear to what extent formal supports to address social isolation were available and used by rural populations. Empirical attention to other types of formal support would contribute to a more holistic understanding of what rural caregivers and persons with dementia need, have access to, and use.
Many barriers to accessibility and use of services by people with dementia and their caregivers were evident, including (a) poor knowledge of services, (b) practicality and resource barriers, (c) values and beliefs, (d) negative judgments and stigma related to both dementia and use of services, and (e) service inadequacy or inappropriateness. Findings illustrate the importance of making services and pathways to access known to families, which was a need we frequently identified in the current review. Sun et al. (Reference Sun, Kosberg, Kaufman, Leeper and Burgin2007) concluded that rural families use formal services primarily as a result of outreach efforts by professionals, highlighting the need for proactive education strategies and connections to service providers. Lack of knowledge of services is not unique to rural areas, and in fact has been identified in the broader literature as a significant barrier to dementia service provision (Macleod et al., Reference Macleod, Tatangelo, McCabe and You2017; Phillipson, Jones, & Magee, Reference Phillipson, Jones and Magee2014; Robinson et al., Reference Robinson, Elder, Emden, Lea, Turner and Vickers2009; Sutcliffe, Roe, Jasper, Jolley, & Challis, Reference Sutcliffe, Roe, Jasper, Jolley and Challis2013). Similarly, perceptions of services as inflexible, inappropriate for needs, and not tailored or person-centred are barriers regardless of rurality, as are some of the values and beliefs around caregiving (guilt, reluctance to ask for assistance) and care recipient resistance (Bieber, Nguyen, Meyer, & Stephan, Reference Bieber, Nguyen, Meyer and Stephan2019; Boots, Wolfs, Verhey, Kempen, & de Vugt, Reference Boots, Wolfs, Verhey, Kempen and de Vugt2015; Brodaty et al., Reference Brodaty, Thomson, Thompson and Fine2005; Greenwood & Smith, Reference Greenwood and Smith2015; Macleod et al., Reference Macleod, Tatangelo, McCabe and You2017; Phillipson & Jones, Reference Phillipson and Jones2012).
Despite stigma’s having been reported as a barrier among urban residents in some studies (e.g., Boots et al., Reference Boots, Wolfs, Verhey, Kempen and de Vugt2015; Mukadam, Cooper, & Livingston, Reference Mukadam, Cooper and Livingston2013), Macleod et al. (Reference Macleod, Tatangelo, McCabe and You2017) did not find this in their urban sample and suggested an increased awareness and normalization of dementia and service use. Although stigma may be decreasing rurally as well, it may also be that diminished privacy and confidentiality makes stigma a bigger problem in rural communities as suggested within the articles we reviewed. Lack of choice among services in rural areas may similarly exacerbate issues with inadequacy or inappropriateness of services. Unsurprisingly, geographical and transportation barriers were salient and appear relatively unique to rural populations.
Recommendations
Strategies to mitigate accessibility and use barriers should be considered in the development and implementation of rural dementia services. In our review, we have identified a number of solutions to barriers, including (a) the use of information and communication technologies, (b) having a point of entry to service use, (c) accessibility assistance, (d) inter-organization collaboration, (e) education, and (f) the development of tailored and person-centred services.
We would like to specifically highlight several of these solutions. First, the use of technology in dementia care is rapidly increasing, and reviews suggest positive effects of technology-based support and education interventions (e.g., Boots, de Vugt, van Knippenberg, Kempen, & Verhey, Reference Boots, Vugt, Knippenberg, Kempen and Verhey2014; Lee, Reference Lee2015). Information and communication technologies can ameliorate geographical and transportation barriers, and facilitate tailored education and interventions. Although inconsistent access to broadband Internet in rural and remote Canada (an issue in many rural areas globally) has been identified as a barrier to information and communication technologies (Ogilvie & Eggleton, Reference Ogilvie and Eggleton2016), they remain a promising avenue of dementia-related education and support service development where feasible.
Second, supporting a point of entry to service use may increase knowledge about services, how to access them, and their potential benefits. Having a central point of contact to facilitate service access is desired by caregivers (Macleod et al., Reference Macleod, Tatangelo, McCabe and You2017; Robinson et al., Reference Robinson, Elder, Emden, Lea, Turner and Vickers2009). A point of entry could take many forms; Dementia Service Centres in Austria offer initial referral and screening for dementia, so that patients are brought into a hub of linked services even before a diagnosis is obtained (Auer, Span, & Reisberg, Reference Auer, Span and Reisberg2015). A recent Canadian Senate report (Ogilvie & Eggleton, Reference Ogilvie and Eggleton2016) encouraged the implementation of the Alzheimer Society of Canada’s First Link program across Canada. Such point-of-entry initiatives should be supported so that persons with dementia and their caregivers are aware of available services and their benefits and access is facilitated.
Third, working to develop dementia education and support that is tailored and person-centred is important to meeting the needs of families. Understanding both population or community-based needs and the specific needs of individual people with dementia and their caregivers is important for service provision (Morrisby, Joosten, & Ciccarelli, Reference Morrisby, Joosten and Ciccarelli2018). Person-centred services can be achieved by comprehensively assessing the needs, preferences, and abilities of service users, and providing culturally sensitive programs that can be adapted to sub-populations (Whitlatch & Orsulic-Jeras, Reference Whitlatch and Orsulic-Jeras2018). Our review suggests that flexibility and one-on-one contact are also ways to enhance the person-centredness of services. A non-person-centred approach is more than a barrier to service use; relationship-centred care is important to the experience of service use, individual well-being, and social inclusion (Ryan, Nolan, Reid, & Enderby, Reference Ryan, Nolan, Reid and Enderby2008). As the best outcomes for people with dementia occur when services are “timely, responsive, flexible, and tailored to individual need” (Dawson et al., Reference Dawson, Bowes, Kelly, Velzke and Ward2015, p. 25), these characteristics should be reflected in education and support services. A person or relationship-centred approach has been highlighted as a priority for dementia care in Canada (Canadian Academy of Health Sciences, 2019) and globally (Prince et al., Reference Prince, Comas-Herrera, Knapp, Guerchet and Karaglannidou2016), and should be emphasized in service development, provision, and the training of health and support care providers.
Evaluation of education and support services is also recommended. This may include ongoing informal evaluation by rural service users to ensure that their needs and interests are being met (see, e.g., Kelsey & Laditka, Reference Kelsey and Laditka2006), process evaluation to determine whether services are functioning as intended, or outcome evaluation to illustrate program impact and efficacy. Although multiple (including qualitative) methodologies offer important information about the effectiveness of services, few intervention studies used the randomized control designs that would be considered strong evidence of program efficacy. Another important direction for evaluation efforts is the increased inclusion of persons with dementia in research, as participants and even co-researchers (e.g., Mann & Hung, Reference Mann and Hung2018). The authors of a recent, non-rural-focused review of factors influencing access and use of formal community dementia services concluded that more attention to the perspectives of persons with dementia was required in research and service development (Bieber et al., Reference Bieber, Nguyen, Meyer and Stephan2019). Greater inclusion of persons with dementia and their caregivers as co-researchers may increase the person-centred focus of support services research, and reveal previously understudied aspects of support required by families. The importance of engaging persons living with dementia and their caregivers in meaningful ways, including as part of research efforts, was highlighted as a priority by the Canadian Academy of Health Sciences’ recent assessment of evidence and best practices to inform development of a Canadian Dementia Strategy (2019).
Additionally, efforts must be made towards the sustainability of high-quality services. Many empirically validated interventions are not established as part of ongoing service delivery despite their efficacy (Gitlin, Marx, Stanley, & Hodgson, Reference Gitlin, Marx, Stanley and Hodgson2015), which does not address the needs of people with dementia and their families and may lead to community distrust (Forbes et al., Reference Forbes, Blake, Thiessen, Finkelstein, Gibson, Morgan and Culum2013; Herron & Rosenberg, Reference Herron, Rosenberg and Skinner2016). Effective and person-centred services should be developed in partnership with existing community organizations and infrastructure to ensure that supports are sustainable.
Finally, better incorporation of sex and gender is required to understand their intersection with rurality and service needs, use, and barriers. The reviewed research suggests being a female person with dementia is related to unmet service needs while males receive more formal care, and that gendered norms around caregiving, independence, and coping strategies may affect rural individuals’ use of services. The broader (non-rural) literature also suggests potential influences of sex and gender on how people with dementia and their caregivers engage with services, such as the presence of higher unmet care needs for women with dementia and a greater propensity for women to have confidence in and use formal services, although female caregivers report lower use of in-home respite services compared to men (e.g., Baker & Robertson, Reference Baker and Robertson2008; Bartlett, Gjernes, Lotherington, & Obstefelder, Reference Bartlett, Gjernes, Lotherington and Obstefelder2018; Forbes et al., Reference Forbes, Jansen, Markle-Reid, Hawranik, Morgan, Henderson and Kingston2008; Greenwood & Smith, Reference Greenwood and Smith2015; Phillipson et al., Reference Phillipson, Jones and Magee2014; Zodikoff, Reference Zodikoff2007). There is limited research examining sex and gender in the context of dementia care, to the point where Bartlett et al. (Reference Bartlett, Gjernes, Lotherington and Obstefelder2018) have characterized this literature as “gender blind”; this must be redressed (Tierney et al., Reference Tierney, Curtis, Chertkow and Rylett2017). It is also important to assess potential sex differences in the acceptability and effectiveness of support and education services for people with dementia and their caregivers, in order to better meet the needs of these populations.
Limitations
Limitations include the non-inclusion of grey literature, which would help to build a comprehensive description of available rural services and gaps. The current review could be a good complement to environmental scans in specific geographical areas. Another limitation was the broad focus of the review, which meant relevant information was sometimes described in articles with little depth (e.g., stigma would be mentioned but not elaborated upon). Finally, we did not limit inclusion to any specific definition of rural; varying definitions meant that population density and distance from urban centres differed greatly between studies and was often not clarified. It should also be noted that although this review synthesized information across rural populations, rural communities are heterogeneous and have unique characteristics, strengths, and challenges. This is a particularly important caveat given the international nature of this review, although efforts have been made to identify the geographic context of reviewed studies, and study locations can be viewed in Tables 4 and 5.
Conclusions
This review illustrates the needs of rural people with dementia and their caregivers, and suggests limited availability of dementia-related support and education services in many communities. A number of barriers to the accessibility and use of existing services persist, some of which are unique or characteristic of rural settings and others which must also be addressed in urban communities. Although our review illustrates challenges with rural dementia support and education, promising solutions and innovations within rural service provision were also evident. These findings can help inform the development of dementia-related support and education services that are accessible to, and used by, rural populations. As dementia care continues to evolve in Canada and globally, opportunities should be pursued to improve rural dementia-related services through the use of information and communication technologies, accessibility assistance, inter-organization collaboration, supporting point of entry service models, and a person or relationship-centred approach to both research and care.









