By the 1980s, one-fifth of all general psychiatrists in England and Wales (Reference Strathdee and WilliamsStrathdee & Williams, 1984) and one-half in Scotland (Reference Pullen and YellowleesPullen & Yellowlees, 1988) were spending some proportion of their time working in primary care. Rather than limit this process, the growth of general practice fundholding fostered it and developments in general practice total purchasing and extended fundholding have encouraged it further (Reference Lee, Gask and RolandLee et al, 1999). At the same time, nationally there has been a gradual increase in referrals directly from general practitioners (GPs) to community psychiatric nurses (CPNs). Referrals from GPs constituted 37% of all referrals to CPNs in 1990 and 46% in 1996 (Brooker & White, 1997: further details available from L.G. upon request), even though there has been a trend away from the primary care service base (21% in 1990 compared with 14% in 1996).
Traditionally, psychiatrists and GPs have most commonly communicated by letter and, less commonly, by telephone. Additionally, they have sometimes met during joint domiciliary consultations, although, even on Mental Health Act assessment visits, is it not unusual for doctors to visit at different times. It is certainly possible and not at all uncommon for psychiatrists in training never to meet face-to-face with their patients' GPs.
Changing policy
Even with the best resources, mental health services cannot meet the need for mental health care in the community. Despite a real increase in the number of psychiatrists, the number of people with mental health problems seen by psychiatrists has probably changed little (Reference Williams and ClareWilliams & Clare, 1981). However, the expectations of general practice and the general public about how mental health services should be provided continue to change and develop. As mental hospitals close, anxiety is stirred up in the media about the failure of community care, while at the same time people become more sophisticated in their understanding of mental health problems and have higher expectations of what can be provided in the National Health Service (NHS). Simultaneously, we have seen the arrival of the primary-care-led NHS, which gives primary care considerable power to fashion the development of services locally, through both service provision and commissioning, with the establishment of primary care groups that will eventually develop into primary care trusts. In England these trusts will take over the provision of local general community services from the existing trusts where they have commonly been jointly managed with mental health. However, primary care trusts will be able to provide locally any form of service they choose, including mental health care. In Scotland the situation is different in that mental health and primary care are now jointly managed through primary care trusts; the position in Wales and Northern Ireland is slightly different again. Finally, the growth of local out-of-hours cooperatives, and other primary care providers, means that there are now even more new structures with which psychiatrists have to negotiate in the community.
The National Service Framework for Mental Health (NHS Executive, 1999) requires Òlocal health and social communities … to build capacity and capability in primary care to manage common mental health problems and to refer for specialist advice and assessment and care appropriately”. Suggested methods for doing this include: (a) development of local protocols; (b) managing referral to specialist services; and (c) specialist mental health services providing primary care liaison and support for primary care staff through professional development.
Why work with primary care?
The majority of mental health services in the UK now operate an approach based on community mental health teams (Reference Johnson and ThornicroftJohnson & Thornicroft, 1993). Although this way of working has a number of advantages, it has had a significant disadvantage in terms of increasing the rate of referral from primary care. We know that community mental health teams integrated into, or working closely with, primary care are less likely to focus on the care of those with severe mental illness (SMI) (Reference Onyett, Heppleston and BushellOnyett et al, 1994). Such teams also seem to experience a rise in the referral of patients with neurotic, personality and substance misuse disorders who would otherwise have been managed within primary care (Reference Jackson, Gater and GoldbergJackson et al, 1993). At a time when secondary care services are seeking to refocus on severe and enduring mental illness, primary care is pushing for more primary-care-based mental health services. This is leading to an inevitable tension between primary and secondary care, with community mental health team staff caught between the two in terms of competing demands.
GPs see and treat the majority of people in the community with mental health problems. However, only about 50% of GPs currently have a psychiatric placement during their vocational training and this may not prepare them for the mental health problems they commonly see in primary care. GPs expect mental health services to be accessible. Wright (1997) has outlined the problems that GPs perceive with services: these include the geographical remoteness of mental health hospitals, poor communication, lack of clarity about management, long waiting lists, problems with urgent referrals, too little contact with other mental health professionals (e.g. CPNs, psychologists) and too few patients discharged back to general practice care.
A patient who has been attending an out-patient clinic for many years may visit his or her GP as (or even more) often as the clinic. This raises the possibility that there is poor coordination of care between the two or, in fact, that clinic follow-up is no longer required. Another patient may rarely see his or her GP because he or she perceives (real or apparent) difficulty in accessing primary care. Both of these situations are inherently unsatisfactory.
Many of the mental health problems seen in primary care are relatively mild and self-limiting disorders and some patients probably do not benefit from unnecessary medicalisation of their problems. However, a significant minority of people with ‘minor’ psychiatric morbidity are suffering from chronic disorder associated with a not insubstantial level of disability (Ustun & Sartorius, 1995) and they require a considerable amount of emotional support. Many of these people would benefit from psychological therapies, yet the necessary expertise in evidence-based psychological therapies is currently concentrated in the specialist mental health sector. Another (overlapping) group that GPs (and psychiatrists) also find difficult to manage are patients with medically unexplained symptoms and patients presenting with somatised emotional distress, who will always visit their GP even when easy access to psychosocial therapies is available because they do not perceive the need for them.
Although there is a movement in the USA for mental health services to provide physical care for patients with chronic mental health problems, this is not the prevailing policy in the UK and many such patients may receive less than adequate general medical care. Furthermore, a proportion of people with severe and enduring mental illness are cared for solely within primary care. For example, for patients with a diagnosis of schizophrenia, research has demonstrated that the GP is the health professional most likely to be in contact 1 year after hospital discharge (Reference Melzer, Hale and MalikMelzer et al, 1991).
Three models have been described in the literature for how we can approach the need for mental health care in the wider community. In the replacement model the psychiatrist or other mental health professional takes over as the first contact professional, as in the walk-in community mental health centre. In the increased-throughput model GPs are encouraged to increase referral. Finally, in the consultation—liaison model mental health professionals leave the hospital and attempt to liaise with GPs in the community. All of these approaches have been tried out in the UK over the past 25 years. The limitations of the first two are apparent. This leaves us with exploring effective ways of liaising or working with primary care.
Methods of liaison
There are various ways of working, which differ in the intensity of direct patient contact.
Attaching mental health professionals to the primary care team
In the past many mental health professionals (e.g counsellors, CPNs, psychologists) were directly employed by the practice or contracted from trusts through fundholding arrangements, but this situation is now changing with a drive for equity of provision and access across primary care groups. These professionals may be attached to the primary care team to perform direct face-to-face care.
Shifted out-patient clinics
Running shifted out-patient clinics in psychiatry at local health centres may provide the opportunity for informal discussion between the psychiatrist and the primary care team about patients not seen in the clinic, but it falls short of the pure liaison model (see below). Other mental health professionals such as CPNs and, more commonly, psychologists may also choose to work in this way.
Triage
Operating some form of triage system could, for example, mean all referrals are first screened by the attached (or linked) CPN.
Consultation—liaison scheme
Some form of formal consultation—liaison scheme could be run, in which potential referrals are discussed before being referred as a first step in management. Or referral could be avoided altogether by discussing a management plan with the GP (Box 1). A psychiatrist, CPN, psychologist or all of these can carry this out. A further variant of this model provides for one-off assessment of patients, thus providing the GP with opinion and advice about management, with the understanding that the patients will be returned as soon as possible to the primary care team for on-going management. This option is probably considerably underutilised in normal out-patient practice because psychiatrists are not aware that GPs may value it (Reference GaskGask, 1986).
Box 1 The consultation—liaison model
There is regular face-to-face contact between the visiting psychiatrist and the GP and other members of the primary care team. The CPN and other members of the community mental health team may also be present. This discussion can be monthly or more frequently
Referral of individual patients to the psychiatrist only takes place after discussion at the face-to-face meeting
Some episodes of illness are managed by the primary care team without referral to the psychiatrist, but after discussion at the face-to-face meeting
When referral takes place there is feedback to the primary care team and management by it
Link workers
Assigning link workers (Reference Goldberg and GournayGoldberg & Gournay, 1997), most commonly CPNs, to liaise directly with practices to set up better channels of communication, shared care protocols and practice-based education, are all discussed in more detail below. A local facilitation worker who has specific expertise in addressing the needs of primary care may coordinate these.
These five methods, of course, overlap and any liaison service may operate in more than one of these modes. There is no standard blueprint and services develop according local needs and preferences.
Benefits and problems
All the parties involved have reported significant benefits from fostering closer relationships between the primary and secondary care teams (Reference Gask, Sibbald and CreedGask et al, 1997). Patients undoubtedly prefer to be seen in a health centre rather than in an out-patient clinic. Some people with mental health problems feel less stigmatised if they see a mental health professional in a primary care setting. Those who have lost touch with mental health services may be re-referred (Reference Tyrer, Seivewright and WollertonTyrer et al, 1984) and there is some evidence to suggest that liaison clinics may reduce admission rates (Reference Balestrieri, Williams and WilkinsonBalestrieri et al, 1988). GPs welcome the development of links with psychiatrists and CPNs (Reference Stansfield, Leek and TraversStansfield et al, 1992) and a small number may even want to be involved in joint assessment.
Although both GPs and patients really value it, direct attachment of staff to perform face-to-face patient care has the least evidence in support of it. There is evidence that specialist input into commonly occurring acute problems, such as depression, that present in primary care may not confer any additional benefits (Reference Scott and FreemanScott & Freeman, 1992; Reference Gournay and BrookingGournay & Brooking, 1994). Reception for liaison schemes and shared care may vary considerably between practices, with inner-city GPs being the least receptive (Reference Brown, Weich and Downes-GraingerBrown et al, 1999).
For mental health professionals, getting out of the hospital clinic into primary care takes time and fewer patients may be seen in a clinic based in primary care in the time available than would be seen at base. Evidence from other specialities suggests that shifted out-patient clinics may not be cost-effective because of the smaller number of patients and shift in case mix towards patients with less severe disorders. Simply shifting the clinic into the health centre without there being any opportunity for the primary care team to meet with and talk to the psychiatrist, even very informally in passing, may not be viewed very positively by either side. However, it can be difficult, except in the larger health centres, to find accommodation for an extra clinic during normal surgery hours when the GPs are likely to be around. It is also likely to prove less successful if sessions are delegated to psychiatric trainees to run because there is less chance of mixing the clinic with the informal advice/discussion about difficult cases that takes place when colleagues meet even briefly.
The challenge is to find a way of working with primary care that confers benefits without adding to the problems already experienced by many community mental health teams. A major concern has been that closer liaison with primary care will shift attention away from those with severe mental illness. This seems to have happened where community mental health teams have closely allied themselves with, or even based themselves in, primary care. Such services have commonly tended to encourage fast-track assessment by the specialist team rather than aiming to support primary care in managing the majority of problems. The evidence so far is mixed, with some studies reporting that models of liaison focus on the care of neurotic disorders and others finding no evidence of this (Reference Burns and BaleBurns & Bale, 1997).
Setting up a liaison service
There is no blueprint that can be applied when setting up a working relationship with primary care and a number of questions need to be addressed (Box 2). As Burns & Bale (1997) comment, Òclarity of purpose is essential but flexibility is a cardinal virtue É there are a series of diplomatic challenges ahead which need to be slowly resolved practice by practice and it's best to start with the easiest”. Change is a slow process and best achieved in a stepwise fashion.
It is crucial to understand the driving force behind the expressed need to work more closely with primary care: is it being driven by the GPs? This was certainly the case in many of the experiments set up during GP fundholding and total purchasing (Reference Lee, Gask and RolandLee et al, 1999). Practices engaged at this time tended to be better organised than their peers, computerised and based in more affluent areas with access to counselling and psychology on site. GPs involved in these early experiments may be keen to roll them out to the primary care groups into which they have been incorporated. However, this poses difficult questions of maintaining sometimes highly staffed services (funded with now-defunct fundholding budgets), while trying to ensure equality of both accessibility and service across a range of practices. Why do GPs want closer liaison with psychiatrists? Is it because they feel that they are not getting an adequate service? If so, in what way?
Box 2 Key questions in setting up a liasion service
Who/what is/are the key driver(s) behind the need to improve links with primary care?
What are the main agendas and expectations of the key players (mental health services, primary care group, service users, health authority, voluntary sector, social services)?
What are the key characteristics of the area (demography, epidemiology, etc.)?
How have services developed historically?
What is the history of cooperation?
What resources and expertise are available now?
What is the level of motivation for change?
Is the need to work together being driven by the agenda of the mental health services? Community mental health teams may complain about their workload and the quality and appropriateness of referrals.
Finally, and perhaps least helpfully, pressure may be coming from the health authority, which may have unrealistic expectations about the reduction in referrals that a top-down imposed solution of working together can achieve in the short-term. To some extent, with the advent of primary care groups and more opportunity for local negotiation between clinicians, this sort of imposed contract specification is less of a burden than it might have been in the past.
The motivation of individuals on both sides of the primary—secondary interface to change is a crucially important factor. In the evaluation of the total purchasing and extended fundholding initiative, two of the key factors appeared to be the achievement of interagency cooperation and key individuals leading the change (Reference Lee, Gask and RolandLee et al, 1999). However, while a lot can be learned from looking at what other services have achieved, it is perhaps more important to consider how they did it, rather than simply trying to replicate the service specification. Solutions must be sought and negotiated locally. Another potential problem may be the lack of local staff trained in working with (in a development, liaison or link worker role), rather than attached to, primary care (the traditional referral role).
Steps in service development
Identify the evidence base
This will consist of a combination of research, evidence from local needs assessment, previous examples of successful developments, national guidelines and recommendations regarding mental health in primary care.
Bring together the key players at a local level
The key players must be actively involved if the project is to work. There must be opportunities to facilitate the key players to meet to discuss the evidence, learn about each other's views and problems and work out some key principles. For example, Reynolds and Thornicroft (1999) have described how focus groups were set up in the Mental Health Link project in south London. This project attempted to address many of the well-known problems discussed above. The focus of the project was the needs of people with severe and long-term mental illnesses. It had two key underlying principles: first, that individual practices are so different that practice-level links are needed and second, that care in general practice and at the interface can be significantly improved with minimal resources. Combining the themes that emerged from these groups, together with ideas from other sources around the country, they identified a number of practical steps to improve joint working at the interface, which included several of the ideas listed below.
Local needs assessment
A key part of the evidence will be some form of local needs assessment. This has been an important focus of the Southbank Project (Box 3), a total purchasing pilot project in Lancashire that aimed to set up a comprehensive, locally based mental health team to liaise with two practices. It is difficult to get a sense of joint understanding of the problems facing mental health care without collecting data on the local picture. Former fundholders and total purchasers will have a pretty good idea of their utilisation of mental health services, although non-computerised practices will find this much more difficult. Unfortunately, the quality of information available from many mental health trusts is still far from satisfactory. It is beyond the scope of this article to describe needs assessment methods in depth, but it is feasible to access locally available information for each local area and this will be much easier if a network of information alliances can be built up (Reference Reynolds and ThornicroftReynolds & Thornicroft, 1999). This might include public health and planning staff in the health authority, trust and social service planning departments, local academic departments with expertise in both qualitative and quantitative methods, local voluntary organisations and the Community Health Council. A patchwork of information can be pieced together to build up a picture of the situation at both district and locality level. As part of this assessment a practice might carry out a range of audits to establish, for example, the local burden and quality of care provided for common mental disorders such as depression, as well as the burden of care provision for those with SMI. There is, of course, no clearly agreed definition of this. Although psychiatrists and other mental health professionals aspire to some form of definition based on disability, in everyday practice mental health staff tend to view SMI ad hoc in diagnostic terms (e.g. schizophrenia, manic depressive illness, organic disorders). This excludes a number of difficult problems, for example, patients with a range of diagnoses including personality disorder and drug misuse who are at risk of harming themselves and/or others and patients with chronic depression who are heavy users of both primary and secondary care services. It therefore becomes essential to spend time working on a locally agreed definition of SMI. This can then form a basis for the development of a practice-based register. This process is described in detail by Burns & Kendrick (1994). Trusts and practices will need to work together to develop a local audit of resources (including the voluntary sector), staff skills and available personnel at both primary and secondary care levels.
Box 3 Case example: the Southbank Project
The practice population consists of 20 000 (9 partners) patients split over two sites. The majority of people are residents of Penwortham, a suburb of Preston; the remainder are students at the University of Central Lancashire, most of whom reside in the town centre.
Stages of development
-
1 Needs assessment
-
2 Locally agreed definition of severely mentally ill
-
3 Establishment of case register containing basic information including, where known, diagnosis, GP, psychiatrist, keyworker, tier of care programme approach and a brief note about the last contact.
-
4 Agreed service specification
-
5 Assembly of the mental health team
Staffing
-
1 A coordinator (temporary development post), whose functions included:
-
• assembling the team and ensuring they meet regularly
-
• drawing up a project plan for the phased implementation of the service model
-
• briefing practice staff
-
• developing a consultation liaison model between primary care staff and the mental health team (with any or all of the elements described above)
-
• clarification of optimal care pathways
-
• developing quality of care for mental health problems to be managed solely in primary care, e.g. by helping to design audits, obtaining patient materials
-
• building links with local voluntary agencies and user groups
-
-
2 A community psychiatric nurse aligned to the practices
-
3 A psychiatrist
-
4 Psychology sessions
-
5 Counselling sessions
Development of the liaison model
Primary referral route to CPN
Shifted out-patient clinic
Opportunity for contact/discussion with GPs
Fast referral back to GP with follow-up plan
Regular education sessions
Involve service users
This is not always easy, but the views of local user organisations and existing service users may be sought about the accessibility and quality of service currently available to patients registered with particular practices.
The specific needs of particular groups, such as ethnic minority populations, the homeless and people with addictions, who may not be registered or find it difficult to register with a practice should not be overlooked. Particular themes will emerge as important in specific localities. It can be difficult to involve consumers of mental health care services provided at primary care level and finding ways of achieving this is a major challenge for the future as more mental health care takes place solely in primary care.
Some specific components of the collaboration
When the group has begun to develop its ideas about what is needed, there are a number of specific ways of working together that might be introduced to improve the quality of care both across the interface and for those patients entirely managed in primary care. Two of these (development of protocols and managing referral) are specifically mentioned in the National Service Framework. Development will require interested individuals to commit time to working together and we have found in Preston that a dedicated primary mental health development worker is central to this task.
Developing protocols
According to the NSF, the National Institute for Clinical Excellence will review existing protocols and kitemark examples of good practice. However, the research evidence suggests that protocols and guidelines are more likely to be effective if they are locally developed and owned, but possibly therefore less likely to be evidence-based because of local limitations. Nationally produced standards and guidelines need to be adapted for local relevance. Protocols will need to be developed over time for depression, postnatal depression, eating disorders, anxiety disorders and schizophrenia. Clearly, workers from both primary and secondary care must contribute to this task to ensure that mutual expectations of what each can provide are realistic and needs for training are identified.
Managing referral
There is no simple answer to the question of what is an appropriate referral. No external ‘test’ can be imposed. Again, if workers can meet together, armed with the evidence listed above, it is possible to come to a locally agreed solution — but there is currently little evidence as to whether this approach actually has an impact. Workers at the interface may also have little idea about who is the most appropriate person to refer to. Consultation (either in person or by telephone) can clarify this and also help in managing waiting lists. Locally, we have found a simple exercise between GPs and mental health workers attached to a practice very helpful: copies of recent referral letters are circulated with the addressee removed and all members of the group are asked to write down who they would refer each patient to and why. Sharing these views in the group can then help to dispel unrealistic expectations, educate about appropriate referral practice and develop more coherent care pathways.
Shared care plans
GPs need to know clearly what part they should play in the management of patients with SMI, and many may be willing to take a greater role in the management of patients with SMI who have relatively stable mental states. Development of the practice-based register will facilitate this process. Essex et al (1990) developed an innovative shared care record to be held by the patient, with the aim of increasing the effectiveness of long-term care of patients with SMI. Many patients found this acceptable and the concept of shared care records is familiar to GPs (e.g. for diabetes, pregnancy).
Training and education
Specific sessions can be organised around requested topics. These probably work best if linked to protocol development and implementation and/or acquisition of specific skills. It is crucial to emphasise the mutual learning process. Many mental health workers do not understand the limitations and difficulties of trying to manage complex emotional problems in the 10 minutes of the average GP consultation, so it is beneficial to involve as many people as possible in these sessions from both teams. A number of teaching packages have now been developed for training primary care workers in skills involved in, for example, the management of depression, people at risk of harming themselves and somatised emotional distress (Reference GaskGask, 1998). Training is probably most effective if based within, and involving, the whole primary care team, but practices vary in their willingness to be involved. There may be other opportunities locally to access unidisciplinary professional groups via postgraduate centres, health visiting and practice nurse forums, which can help to seed unengaged practices. The need to establish clinical governance within primary care may increase requests for holding such sessions in the primary care group.
Support and liaison sessions
What is actually discussed during these meetings and who attends will vary from place to place depending on whether the service is based in a relatively affluent or deprived area, the local service priorities, the interest, or otherwise, of the GPs in mental health and the available expertise. Both clinical and non-clinical (service development) issues may be discussed. Burns and Bale (1997) describe in detail how to set up and conduct such sessions.
Conclusion
We have no option now but to find ways of working more effectively with primary care. There is no universal blueprint that can be applied. Although psychiatry and general practice have a great deal in common, they also suffer a wealth of mutual misunderstandings. Setting up more effective channels of communication and sharing problems can begin to break down the barriers. But it will take time, flexibility and tolerance to achieve change.
Multiple choice questions
-
1. With regard to psychiatry in primary care:
-
a currently most GP trainees have a 6-month psychiatry post as part of their vocational training
-
b referrals to CPNs from GPs have increased over the past 10 years
-
c CPNs are more likely to be based in primary care than they were 10 years ago
-
d GPs and psychiatrists frequently see patients jointly
-
e traditional hospital psychiatry posts prepare doctors well for mental health problems in primary care.
-
-
2. With regard to methods of working with primary care:
-
a in the replacement model the mental health professional replaces the GP in the surgery
-
b in the increased throughput model GPs are actively encouraged to refer more patients to psychiatry
-
c a triage system is part of the replacement model
-
d a triage system is usually operated by the GP
-
e shifted out-patient clinics are more time- effective than traditional hospital clinics.
-
-
3. Current psychiatry in primary care literature suggests that:
-
a inner-city GPs are more likely to be enthusiastic about the development of liaison schemes with psychiatry
-
b GPs feel that too few patients are discharged back to general practice care
-
c the GP is the health care professional most likely to be in contact with a patient who has suffered schizophrenia, one year after discharge from psychiatric hospital
-
d community mental health teams working within primary care are more likely to focus on patients with severe enduring mental illness
-
e GPs perceive psychiatric hospitals to be geographically remote.
-
-
4. Steps in service development include:
-
a local needs assessment
-
b identifying ‘key players’ who need to be involved
-
c gathering relevant evidence from literature searches, national guidelines and previous examples of successful developments
-
d involvement of service users
-
e funding obtained from the total purchasing initiative.
-
-
5. Suggested ways of working more harmoniously with primary care include:
-
a at least weekly meetings between mental health professionals and GPs
-
b guidelines from psychiatrists for GPs on ‘appropriate’ referrals
-
c shared care records such as those already used in pregnancy and diabetes
-
d developing local protocols for the management of specific disorders such as depression, anxiety and schizophrenia
-
e feedback from psychiatrists to GPs on ‘inappropriate’ referrals.
-
MCQ answers
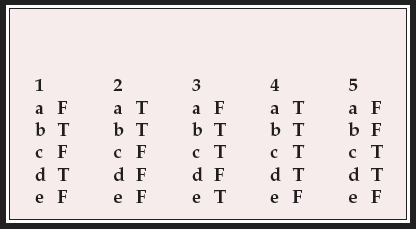
| 1 | 2 | 3 | 4 | 5 | |||||
| a | F | a | T | a | F | a | T | a | F |
| b | T | b | T | b | T | b | T | b | F |
| c | F | c | F | c | T | c | T | c | T |
| d | T | d | F | d | F | d | T | d | T |
| e | F | e | F | e | T | e | F | e | F |



eLetters
No eLetters have been published for this article.