The importance of systematic assessment of risk has been highlighted in guidelines by the Royal College of Psychiatrists (1996) and recommendations by the National Confidential Enquiry (Department of Health, 1999), and has been formalised in government advice on the implementation of the Care Programme Approach (CPA; Scottish Office, 1998). All recognise the importance of accurate documentation of past risk-related behaviour as important in assessing future risk, and Potts (Reference Potts and Crichton1995) has identified minimisation of historical risk as a factor that can weaken risk assessment.
As with other services nationwide, the Dundee Psychiatric Service has implemented the CPA, but has faced some difficulties related to the government's expectation of resource neutrality. One specific area of concern was that case files in Dundee, possibly in common with a significant number of other services, are still paper-based, bulky and poorly organised for the accurate extraction of past risk-related behaviour.
The aims of the current study were to develop a proforma for documenting past risk-related behaviour, and use this to extract appropriate information from case files, to document the time required and to see if such a systematic review produced results felt to be useful by colleagues. Temporary funding was obtained to enable the work to be done thoroughly without detracting from other duties and the final aim of the study was to produce recommendations on how to proceed when the temporary funding ceased.
Method
The study was carried out in Dundee - a Scottish city with a compact catchment of 183 000. Application of an updated version of the Mental Illness Needs Index indicates that Dundee is an area of higher than average deprivation, scoring as a whole 20% above the bench-mark (Tayside Health Board, 1998). In a recent census, the total number of patients on the community services caseload was 1457. Of these, 545 were suffering from schizophrenia or schizoaffective illnesses and 652 from bipolar disorder or severe depressive illness, confirming that a substantial majority were suffering from severe mental illness. One hundred and twelve patients are now being managed through the CPA - a more selective approach than applies in most English services. The current study describes the initial cohort of those patients referred for CPA.
A small, multi-disciplinary project group was set up as an offshoot of the CPA Steering Group to oversee the project. This comprised representatives from nursing, medical and administrative staff. Funding was obtained for a part-time research assistant (4 hours per week over one year, plus 2 hours per week of secretarial time) and an occupational therapist (T.D.) with extensive clinical and research experience in working with patients suffering from chronic severe mental illness was appointed and joined the project group. A proforma based on listing the main areas of risk, reviewing documentation from elsewhere and discussion with project group members was then developed. This was piloted on 10 sets of notes and the amended proforma was agreed with the group.
The proforma comprised two pages. The first page consisted of a list of main headings (violence/destructiveness with sub-categories for minor and major incidents, suicide/self-harm, severe self-neglect, risk to children, failure to take medication and unplanned loss of service contact), in which the dates of each incident were recorded under the appropriate heading, supplemented with a more detailed tick-list of categories of violence (arson, sexual assault, violence to family, violence to staff, violence to other patients and violence to general public). History of special hospital admission and imprisonment was also noted, as was any history of alcohol or drug misuse. The second page contained a brief narrative of each major incident or series of incidents in date order, comprising a brief description of the incident, mental state at the time and whether or not substance misuse was involved, for example ‘punched night nursing officer while deluded and disturbed’, ‘aggressive behaviour towards partner and partner's child - no further details recorded’, ‘fight with fellow resident at hostel - drunk but not psychotic’, ‘slashed wrist to release devils’. The proforma thus served as an index as to where further details of individual incidents could be found if required, and as an overview and concise summary of these incidents.
The project was discussed with colleagues in the community mental health teams and Division of Psychiatry and a referral procedure agreed. The case records of all patients being considered for CPA from 27 May 1998 to 30 March 1999 were referred for a historical risk assessment. We obtained all sets of notes for each patient and extracted relevant information, noting the time taken to complete the task. The secretary recorded the number of sets of notes and measured their weight for every fourth referral.
Anonymised examples of the completed proforma were circulated to the Division of Psychiatry and to Community Mental Health Team coordinators, and feedback was also sought from referring consultants on the value of the information contained in the proformas.
Results
Patients
Forty-three patients were referred, of whom 32 (74%) were male. The mean age was 41.6 years. The mean number of years in contact was 17.3, the mean number of admissions 12.2 and the mean number of in-patient months 55.6. Thirty-one patients were suffering from schizophrenia, five from personality disorder, three from bipolar disorder and four patients had another diagnosis.
Records
Risk incidents were found to be recorded in various parts of the in-patient, day patient or community sections of the file, and in medical or nursing files. It was not possible, therefore, to identify a single section of the file where risk-related information could be accessed. Despite the time allocated to the project, it was not possible to go through the nursing records in detail and social service records were not scrutinised, so it is conceivable that the current project has under-reported past risk. Quite frequently, helpful summaries that included risk-related information had been carried out, but had not been transferred to the current file and were filed inconsistently so that they would have been difficult to find in routine clinical practice.
The median number of volumes of notes was four per patient. One in four of the sets of notes was weighed - the mean weight of these notes was 8 kg. It took over an hour to extract information from each volume of notes - around 5 hours for each patient.
Incidents
The raw material of our survey consisted of brief summaries of each incident rather than a rating scale, but we have attempted to summarise the information in the table. An episode of violence was categorised as major if it was potentially life-threatening, even if no physical damage occurred, such as threatening with a loaded weapon or knife, or fire setting; one or two punches that resulted in bruising but had been provoked and were neither psychotically driven nor part of a sustained assault, were categorised as minor. Suicide attempts included everything from wrist-cutting episodes to serious overdoses and attempted hanging. Self-neglect was severe, for example: ‘living in squalor’, ‘refusing food’ or ‘feet swollen and oedematous’. Risk to children involved either the child being incorporated into the patient's delusional system and aggressive ideas being expressed or inappropriate hitting against a background of generally increased irritability.
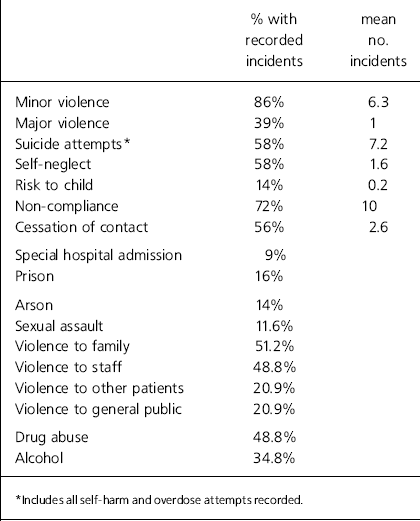
Table 1 summarises the type and frequency of incidents recorded. Bearing in mind that this was a non-forensic population, either in the community or being considered for discharge into the community, the range and variety of incidents is noteworthy. We did not separately analyse time lapsed since the incident, but in the majority of cases, incidents of significant harm to others had occurred some years previously.
Table 1. Summary of incidents
| % with recorded incidents | mean no. incidents | |
|---|---|---|
| Minor violence | 86% | 6.3 |
| Major violence | 39% | 1 |
| Suicide attempts* | 58% | 7.2 |
| Self-neglect | 58% | 1.6 |
| Risk to child | 14% | 0.2 |
| Non-compliance | 72% | 10 |
| Cessation of contact | 56% | 2.6 |
| Special hospital admission | 9% | |
| Prison | 16% | |
| Arson | 14% | |
| Sexual Assault | 11.6% | |
| Violence to family | 51.2% | |
| Violence to staff | 48.8% | |
| Violence to other patients | 20.9% | |
| Violence to general public | 20.9% | |
| Drug abuse | 48.8% | |
| Alcohol | 34.8% |
Feedback
Once anonymised examples were available, we canvassed the view of colleagues through the Division of Psychiatry and community mental health teams. They agreed that the exercise was useful and should be an integral part of assessment for the CPA.
Conclusions
It is possible to extract risk-related information from case records using a simple proforma. The approach yields relevant results (as would be expected in a group of patients referred for the CPA) that are felt to be useful by clinicians. Our proforma covered items very similar to those identified in the Risk Assessment Checklist cited by the Mental Health Reference Group (Scottish Executive, 2000). However, we feel that the addition of a brief summary of each incident, with dates (so that further details can be accessed), are clinically useful additions to the basic checklist. They assist in assessing risk in context - recognised to be important in risk management (Reference ShawShaw, 2000).
Retrospective extraction is, however, very time consuming as past risk-related information is neither systematically filed nor indexed and may be spread through several bulky case records. Clinicians are already usually involved in Trusts’ incident recording procedures, but information from these tend not to be subsequently readily accessible to clinicians. It seems clear that the emphasis should be on prospective clinical recording of incidents and more efficient case record management. We accept that this seems to be a self-evident conclusion. However, our study showed that it was not being implemented locally and another Scottish study has noted that a common record, shared by the multi-disciplinary team, is not yet in widespread use (Reference SteinStein, 1998). In addition to highlighting the general importance of allocating a higher priority to case record organisation and maintenance, we would like to make three specific suggestions that we feel would increase the likelihood of improving practice. First, risk incidents should be recorded prospectively and summarised at reviews. A system such as ours involves little ongoing input from clinical or records staff, but gives a good overview of incidents together with details of where to find further information if required. Second, the risk summary should be filed in a clearly-identified part of the case record (e.g. Care Plan or Key Documents) that is accessible in both inpatient and community settings. Third, if a new case record is made up for an existing patient, records staff should have clear advice that the risk summary should be one of the documents transferred to the new set of notes. Implementation of the above would require a close partnership between clinicians, records and secretarial staff, and to be cost-effective would need to be focused on those patients where risk assessment and management are likely to be a significant issue. Finally, we would recommend that audits of clinical practice (prospectively documenting risk incidents and summarising these at reviews) and of case record maintenance (standardised and accessible filing of risk documentation in the current set of notes) are included in the Clinical Governance Programmes of Trusts.
Declaration of interest
The study was supported by a grant from Dundee Health Care NHS Trust.
Acknowledgements
The authors would like to thank clinicians from the Dundee Psychiatric Service for their help and support and in particular, Morag Ross and Calum McFee, for community and in-patient nursing liaison, Dr Andrew Reid and Dr Anne McHarg for advice and for liaison with psychiatrists and Val Johnson for administrative support.




eLetters
No eLetters have been published for this article.