Introduction
This paper sets out to use a compendium study of nurse-led primary health care (PHC) models to highlight some of the ways in which nurse’s work with communities to improve health. These case studies, included in a compendium of nurse-led and/or midwife-led PHC models compiled as part of a World Health Organisation (WHO, 2007) project, provide illustrations of how community coproduction might occur. This project aimed to identify and review models and examples of good practice in PHC. These models and examples were analysed for key themes to identify pointers for success.Footnote 1 This paper focuses on one of the themes that strongly emerged, which the author has identified as being related to coproduction in health, and how nurses and midwives can be positioned to work with communities to jointly lead PHC.
In the Declaration of Alma-Alta (1978), PHC is defined as follows:
Primary health care is essential health care based on practical, scientifically sound and socially acceptable methods and technology, made universally accessible to individuals and families in the community through their full participation and at a cost that the community and country can afford to maintain at every stage of their development in the spirit of self-reliance and self-determination. (Downloaded 10th October 2008: http://www.who.int/topics/primary_health_care/en/)
Clause VII of the Declaration of Alma-Ata sets out seven key requirements of PHC and these are identified in Box 1 below.
Box 1 Seven key requirements of PHC (Alma-Ata, 1978)
Clause VII Primary health care
• Reflects and evolves from the economic conditions and socio-cultural and political characteristics of the country and its communities and is based on the application of the relevant results of social, biomedical and health services research and public health experience;
• Addresses the main health problems in the community, providing promotive, preventive, curative and rehabilitative services accordingly;
• Includes at least: education concerning prevailing health problems and the methods of preventing and controlling them; promotion of food supply and proper nutrition; an adequate supply of safe water and basic sanitation; maternal and child health care, including family planning; immunisation against the major infectious diseases; prevention and control of locally endemic diseases; appropriate treatment of common diseases and injuries; and provision of essential drugs;
• Involves, in addition to the health sector, all related sectors and aspects of national and community development, in particular agriculture, animal husbandry, food, industry, education, housing, public works, communications and other sectors; and demands the coordinated efforts of all those sectors;
• Requires and promotes maximum community and individual self-reliance and participation in the planning, organisation, operation and control of primary health care, making fullest use of local, national and other available resources; and to this end develops through appropriate education the ability of communities to participate;
• Should be sustained by integrated, functional and mutually supportive referral systems, leading to the progressive improvement of comprehensive health care for all, and giving priority to those most in need; and
• Relies, at local and referral levels, on health workers, including physicians, nurses, midwives, auxiliaries and community workers as applicable, as well as traditional practitioners as needed, suitably trained socially and technically to work as a health team and to respond to the expressed health needs of the community.
The development of PHC initiatives is important for a number of health and workforce related reasons. For example, in many countries, the obesity epidemic will substantially increase the proportion of the population, including younger people, at risk of developing chronic diseases and the proportion of the population with diabetes is expected to increase markedly over the next 20 years (Bambs et al., Reference Bambs, Cerda and Escalona2008). In the case of Australian Indigenous people, it has been claimed that the significantly lower expenditure on PHC (half that for non-Indigenous people), could be a contributing factor to the rising rate of hospitalisations for potentially preventable conditions, (Banks, Reference Banks2007). The rise of chronic diseases in many countries suggests that current models of care are inappropriate for addressing population health needs (WHO, 2007):
The rise of chronic diseases has uncovered further problems: the burden of long-term care on health systems and budgets, the costs that drive households below the poverty line, and the need for prevention in a situation in which most risk factors lie outside the direct control of the health sector. (Chan, Reference Chan2008)
In addition, the workforce is getting older and is unsustainable in its present form (Buchan and Calman, Reference Buchan and Calman2004; Nuntaboot, Reference Nuntaboot2006). For example, in Australia the average age across all nurses is over 45 years old and is increasing as fewer young people enter or stay in the profession (AIHW, 2008a). This is similar to the International Council of Nurses review of the ageing nursing workforce that identified that the average age of nurses in many countries exceeds 40 years (ICN, 2008). Furthermore, the distribution of health professionals is not well matched to the distribution of the population. Across Australia and Canada, the ratio of health professionals to population decreases with increasing geographical remoteness (MacLeod et al., Reference MacLeod, Keilig, Stewart and Pitblade2004; AIHW, 2008b).
With these issues in mind it is timely to rethink models of health care delivery (Chiarella, Reference Chiarella2007). Recently, initiatives such as the National Health and Hospitals Reform Commission and a review of maternity services have been established to develop a long-term health reform plan for a modern health system for Australia (AIHW, 2008b). Similar initiatives, such as the Prime Minister’s Commission on the Future of Nursing and Midwifery, are occurring in England (CNM, 2009) and a recent major review and analysis has been undertaken in the United States of America (Buerhaus et al., Reference Buerhaus, Staiger and Auerbach2009). There is recognition of the need for ‘joined up solutions’ (Buchan and Edwards, Reference Buchan and Edwards2000; Scott, Reference Scott2008) – across all levels of government, disciplines and sectors. Success factors in ‘things that work’ include the following: cooperative approaches; bottom-up community involvement; ongoing support; and good governance (Banks, Reference Banks2007). PHC has a major role to play in any health reforms as it can be the first level of contact of individuals with the national health system and constitutes the first element of a continuing health care process (Kendall, Reference Kendall2008).
The year 2008 was the 60th anniversary of the founding of the WHO and the 30th anniversary of the Declaration of Alma-Ata – a landmark in the global development of PHC (WHO and UNICEF, 1978). These anniversaries have created a revitalisation of interest in PHC and a desire to build on the Alma-Alta legacy. PHC is the theme of the 2008 World Health Report (launched on 21st October) and PHC was also the theme for International Nurses’ Day in 2008 on the 12th May – Florence Nightingale’s birthday. As a result of this renewed emphasis, the contribution of nurses to PHC has been the focus of a number of key publications (eg, Kendall, Reference Kendall2008; NZ Ministry of Health, 2009; WHO, 2009). As the 2015 deadline for achieving the Millennium Development Goals draws nearer, the Director–General of WHO has called for ‘a renewed emphasis on PHC as an approach to strengthening health systems’, building on the legacy of Alma-Ata and the struggle for health for all to help achieve the goals (Chan, Reference Chan2007) and the World Health Assembly has refocused on placing individuals at the centre of health care and emphasising integrated horizontal PHC programmes with the existing vertical models (WHA, 2009).
The WHO compendium project
The WHO compendium project arose at the request of Dr Jean Yan, Chief Scientific Officer for Nursing and Midwifery, WHO, to strengthen the contribution of nursing and midwifery to PHC worldwide. Professor Chiarella was invited to compile a compendium (collection) of exemplars of nursing and midwifery-led PHC work. The compendium is part of a year-long project led by the Office of the Chief Scientific Officer for Nursing and Midwifery at WHO entitled now more than ever as the contribution of nurses and midwives to PHC, led by Dr Yan, Professor Chiarella and project consultant Jane Salvage.
The overall project aim was to maintain, improve and scale up the contribution of nurses and midwives to PHC worldwide. The project’s primary purpose was to support and strengthen PHC service delivery by nurses and midwives worldwide, within the context of the inter-professional team, by providing exemplars of best practice in PHC. The target audience for the project’s deliverables varies according to each product and activity, but includes nurses and midwives delivering PHC services; other practitioners and support workers; service planners and managers; health professional organisations; training institutions; policy-makers and opinion-leaders; and civil society organisations that represent users of PHC services.
A compendium may be defined as ‘a book containing a collection of useful hints’, a selection of objects in one container’ and ‘a comprehensive summary of a larger work’. This compendium provides a summary and analysis of PHC case studies collected from around the world, highlighting in particular the contributions of nurses and midwives to strengthening health systems. The questions asked in developing this compendium were ‘what are examples of best practice in PHC worldwide, and what are the common elements of and barriers to successful PHC service delivery’. The compendium was intended to be the first step in an ongoing collection of PHC case studies. This paper does not set out solely to describe all elements of the compendium. That is achieved through the WHO publication (WHO, 2009). Rather, this paper, after broadly describing the work contained within the compendium, takes one aspect identified by case study authors as a major contributor to the success of the PHC initiatives.
Methods
Design
The design used was a survey of recommended case studies using a purposive sample of contributors identified by the Regional Nurse Advisers (RNAs) from each of the six regions of WHO. The RNAs were contacted by the Chief Scientific Officer for Nursing and Midwifery at WHO and asked to supply names and contact details of people who they considered to be leading successful nurse-led PHC models in their regions. The researcher then contacted each identified individual (n = 38) and asked them if they would participate in the compendium and provided them with the case study survey, attached as Appendix 1.
Survey instrument
The survey instrument sought information on the following: the aims of the service, programme or project described in the case study; the type of work involved; the five major needs of the population served by nurse and midwife-led PHC; funding and staffing arrangements; and the extent to which the contributor considered the project met the criteria for PHC based on Clause VII of the Declaration of Alma-Ata (Box 1). The survey instrument consisted of both closed and open responses, one of the latter of which asked the contributors for ‘pointers for success’.
Analysis
To ensure that the information that went into the compendium accurately reflected the content of each completed survey, the researcher made a summary of each case study that included the aim of the project, staffing, funding and outcomes (as available). This was then sent to the designated contact person for validation and amendments were made as required. Sometimes further information on funding and outcomes in particular was provided as a result of the validation process. The summaries were provided as an annex to the compendium report.
Each submitted case study was analysed to identify its key themes. Data were collected and compared on the main needs of the populations served, which were quantitatively analysed and produced in table form, and the extent to which the projects met the PHC criteria, which were thematically reported and cross analysed against the current WHO’s global agenda priority areas (WHO, 2006). These priority areas are highly similar in content to the original PHC criteria in Alma-Ata (WHO, 1978), but include issues such as ‘harnessing science and technology’ and ‘strengthening governance, leadership and accountability’ – two issues that were evident in the analysis of the case studies. The use of technology in PHC will be discussed in a later paper, but the question of governance, particularly in relation to coproduction, is a central theme of this paper. Case study contributors were also invited to submit their reports, published articles, photographs and other materials relating to their projects or services. This rich and interesting information has been drawn on in the summaries.
Results
A total of 38 teams from 29 countries completed and submitted the survey within the deadline. Table 1 shows the representation from each region and country, indicating the global spread of the studies and the very wide range of settings, contexts, cultures and levels of development they encompass.
Table 1 Case studies collected January–March 2008
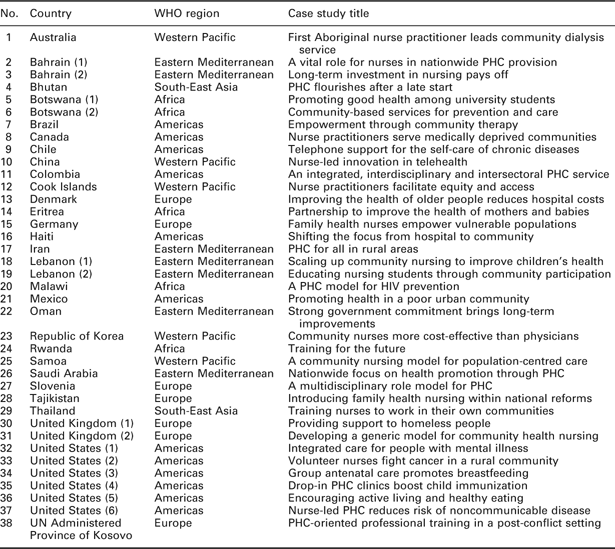
WHO = World Health Organization; PHC = primary health care.
The main needs of the population served were identified and are reported in Table 2. This shows that the main needs tended to be related to health education, disease prevention, self-care, family planning, reproductive health and treatment of injury.
Table 2 Top five needs of the populations served in the case studies

Foci of the case studies
Health promotion
Health promotion was a major focus for all the case studies, either in the services that were being delivered or as a key component in educational programmes. Examples of health promotion for the elderly and the prevention of non-communicable disease featured significantly. Active health promotion in the elderly was a feature of the Skævinge project, begun in one municipality but now a national PHC project (Denmark) also adopted in Japan. Other programmes were designed to support people living with diabetes (Bahrain), cardiovascular disease (United States) and renal disease (Australia) and to work with groups where high disease rates were prevalent, such as cervical cancer (United States) and substance abuse (United Kingdom).
Service type
The type of service provided in relation to the prevention and control of locally endemic diseases ranged from prevention and control of HIV/AIDS (Botswana and Malawi), tuberculosis (Haiti and Samoa) and vector-borne diseases (Malawi and Republic of Korea) to prevention and management of non-communicable diseases (Chile, China, Cook Islands and United States). Appropriate treatment of common diseases and illness such as hypertension, diabetes mellitus, HIV, diarrhoea, upper respiratory diseases, skin conditions was a regular feature of many of the services.
An emerging but common aspect of PHC was the provision of mental health services by nurses. Examples of this included work with homeless people (United Kingdom), victims of domestic violence and rape (Botswana, Colombia and United States), and people suffering in the aftermath of war (Kosovo). Nurses also provided group therapy and counseling for local communities, as a result of needs assessment based on family visits or community needs assessment based on community consultation.
Key interventions
The problems of nutrition were a regular focus of intervention, both in terms of a lack of food supply on the one hand (Eritrea, Haiti and Malawi) and poor nutrition due to eating the wrong types of food, leading to obesity in children, on the other hand (United States). Other projects were involved in ensuring safe water supplies and basic sanitation (Colombia), particularly in areas of conflict (Eritrea, Kosovo and Lebanon).
Maternal and child health was a major focus across many projects (Colombia, Eritrea, Oman, Thailand and United States). Reproductive health care was prevalent such as the avoidance of teenage pregnancies (Samoa), learning breastfeeding and parenting skills (United States), family planning (Republic of Korea), treatment of sexually transmitted diseases (United States) and screening for breast and cervical cancer (Mexico and United States). Immunisation was a standard intervention in all the programmes targeting maternal and infant health, some funded through large national health promotion programmes (Lebanon), others being local initiatives such as an immunisation drop-in centre (United States). School health was a significant focus, with active involvement in school education, diet and exercise programmes (Bahrain, Botswana, Cook Islands, Samoa and United States).
Telehealth care was an innovative mechanism described by two projects as a strategy for delivering PHC. One telehealth programme supporting people living with type 2 diabetes studied the effect of the nurse-managed telephone support model on self-efficacy, perception of health, healthy eating, physical activity, foot care and the use of health services (Chile). In another service extending from Hong Kong to rural areas in Mainland China, telehealth nurses took care of healthy communities and people with subclinical symptoms and chronic conditions, such as diabetes mellitus, stroke, incontinence and pain.
Workforce issues
The development of a suitably qualified and skilled workforce is a critical issue in the establishment of PHC. Several of the case studies described programmes engaged in training nurses for PHC roles (Bahrain, Cook Islands, Germany, Kosovo, Tajikistan, Thailand and United Kingdom).
Another practical professional development solution was the education and introduction of nurse practitioners, who were able to case-manage patient groups from admission to treatment and through to referral or discharge (Australia, Canada, China, Cook islands, Republic of Korea and United States). However, in terms of the provision of essential medications by nurse practitioners, this varied significantly. For example, nurse practitioners were often able to prescribe medications, subject to availability. However, while some programmes had medications supplied through national schemes (Cook Islands), and some were able to supply specific medications such as antiretroviral therapy (Botswana), others had to go to great lengths to obtain medications for their disadvantaged communities. Other countries were working towards legislation to enable nursing staff to prescribe medications (Bahrain).
Coproduction and health
The primary aim of this paper is to explore the way in which nurses and midwives worked with communities in PHC. This was not a question originally sought from contributors but instead emerged from the open questions that asked about ‘pointers for success’. A key feature of many of these open-ended responses in the case studies was the emphasis on the methods and processes for engaging with individuals and communities. Many of the methods of engagement used reflect an approach in which individuals and community groups are treated as the experts, particularly in relation to their understanding of their own environments or their disease and its impact on their lives and needs.
This active relationship between health professionals and communities has been described as the ‘coproduction’ of health. The broad definition formulated by Bouvard (Reference Bouvard2007) builds on a number of earlier definitions, particularly that of Joshi and Moore (Reference Joshi and Moore2003):
the provision of services through regular, long-term relationships between professionalised service providers (in any sectors) and service users or other members of the community, where all parties make substantial resource contributions. (Joshi and Moore, Reference Joshi and Moore2003:5)
An important element of service that health care providers have traditionally overlooked is providing the information, skills and know-how necessary to empower health care consumers and their communities to effectively perform their coproduction responsibilities to maintain their own health (Bopp, Reference Bopp2000). The coproduction of health forms part of a continuum of community engagement, with the activities differentiated by the purpose for which engagement takes place (Popay, Reference Popay2006). Information provision and exchange lie at one end of the continuum, next comes consultation, then coproduction and community control at the far end. This differentiation is similar to the model of participation proposed by Arnstein in the 1960s (Arnstein, Reference Arnstein1969). The Arnstein model described the stages by which non-participation can move to full participation and decision-making powers. These stages involve information, consultation and partnership in a hierarchical continuum. Similarly, the community engagement continuum moves from approaches used to engage with the community towards an increasingly strong ethos of development and empowerment (Popay, Reference Popay2006). The greater the participation, empowerment and control, the greater the impact on service outcomes, health status and the reduction of health inequalities.
The key philosophy underpinning coproduction of health is that both parties, the health professional and the community member, bring knowledge and expertise essential for influencing the determinants of health. This emerges in a personal reflection from the Slovenia case study:
Children’s personalities are, above all, formed at home (the family), in the kindergarten and by their neighbourhood. The most important role is played by their parents, who can provide them with a positive home environment at the psychological, physical and social levels. Thus knowledge obtained from parents during a baby’s antenatal and postnatal periods is of great importance. It enables organization of health care services with health education and preventive activities. (WHO, 2009: 22)
The education and support of traditional birth attendants (TBAs) in Eritrea is another exemplar of valuing local knowledge. TBAs are selected based on age, physical fitness and social acceptability before they are trained and deployed by the community, members of the health facility and the women’s association. Their value as people who bring their knowledge and skills to the health endeavour is outlined by the author of this case study: ‘They are drawn from the community to serve that community. The TBAs bring on board issues and concerns of the community and share it with hospital management. This mechanism fosters full community participation in the planning and implementation of health services to the community’.
In Thailand, local organisations have selected and funded local people to study to become ‘nurses of and for the community’. The programme content is directly influenced by the health needs of their community, to which they will return on completing their education. The first cohort of graduates working back in their communities since 2006 are providing home-based care to those with chronic disease, elderly people, children, people with disabilities and other disadvantaged groups and also caring for people presenting with minor illnesses. Local surveillance is now conducted for both communicable and non-communicable diseases and health promotion activities are carried out. The respondents reported that the number of hospital admissions has been reduced as a result of surveillance of both communicable and non-communicable diseases, and health promotion activities.
A ‘community therapy’ project in Brazil exemplifies a scenario where the community identifies its needs and the health professionals respond to a community agenda for health. Nurses work with community members who choose to attend a local therapy group to provide support and facilitated discussion. The work is based on Freire’s philosophy of resilience and liberty (Freire, Reference Freire1970). Community therapy is offered to anyone who is suffering; children, young people, adults and old people of both sexes take part in the therapeutic meetings. Most participants are elderly adults, generally housewives, who work at home, or are retired, with low incomes and low educational levels. About 25 people take part in each meeting; these are held weekly and at last two hours. Residents usually attend within their own community. The service is provided by three professors of nursing from the Department of Nursing of the Federal University of Paraíba. Students undertaking the graduate programme in mental health nursing and postgraduate research students are also involved. Participants show improvement in their general health status; their capacity to maintain a relationship; and their social interaction skills. They also report feeling empowered, self-determined and independent, with greater respect for themselves and their limitations. The model is now being adopted in other communities in Brazil.
Discussion
The project described here provides a snapshot of 38 PHC case studies from 29 countries based on a survey sent to 38 organisations from 29 countries. These examples illustrate that services and strategies are most successful when the people being served are involved and their contribution valued. This kind of reciprocity leads to mutual rewards such as the provision of PHC services as well as helping to build communities and to strengthen community empowerment. While it was not foreshadowed as an aspect of the original survey instrument, the responses relating to ‘pointers for success’ were so directly comparable to the concept of coproduction for health that the authors considered it was an important and unforeseen outcome of the survey.
This work is the first step in an ongoing collection of PHC case studies which highlight: care models, examples of best practice and the common elements of successful PHC service delivery and the contribution of nurses and midwives to PHC worldwide. The compendium has been launched as a web-based resource. WHO would like to receive many more such exemplars, and is creating further opportunities for the submission of case studies for another project activity – a global award scheme to recognise outstanding individual and team contributions by nurses and midwives to best practice and innovation in PHC.
Obviously this study is not without its limitations. Clearly, the selection process was based on the RNA’s recommendations and assessments of what constituted a ‘successful’ PHC model. Similarly some of the models did not provide quantitative analysis of outcomes and some were undertaken by local teams who did not have academic support but who were nevertheless engaged in significant PHC initiatives. However, this work also has significant strengths, not the least of which are that the completed surveys provide a rich and varied overview of the types of nurse-led PHC work that is being conducted globally and that all those invited to participate completed the survey and provided information. In addition the analysis of the responses was validated through feedback and implementation of recommended changes.
The democratic engagement and empowerment of both staff and community was a key requirement for success identified in most projects. Models based on coproduction in health is one of the ‘things that work’ (Banks, Reference Banks2007) in PHC. The achievement of health in these projects required engagement of the community and was not considered to be the domain solely of health care professionals, planners and policy-makers. Commitment and motivation were essential, and were developed through culturally appropriate and sensitive engagement with communities.
The need to build on existing local resources was critical to success. This was part of the process of recognising that services ought not to be imposed on communities, but developed in response to their identified and owned needs. Community self-esteem and self-belief – factors that were also considered essential indicators of good health – were also built by the process of community engagement, education and information provision. Ownership of programmes by local communities was also seen as fundamental to sustainability.
While the evidence relating to the success of the programmes ranged along a continuum from extensive quantitative and persuasive qualitative data at one end of the spectrum to anecdotal reports and expressions of personal opinion at the other (WHO, 2009), the evidence of community engagement was often provided in detail as part of the text of the case studies. Although there are many examples of the outcomes that relate directly to empowerment and coproduction of health within the compendium (WHO, 2009) one example can be found in the CenteringPregnancy®, which aimed to increase the psychosocial well-being and healthy behaviour of disadvantaged women in Chicago as a strategy for reducing adverse maternal and infant outcomes and disparities among racial/ethnic groups. The programme is based on woman-centred care and the empowerment of women throughout their reproductive lives, and draws on concepts of midwifery care, feminism, social support theory and self-efficacy theory. All antenatal care providers (group facilitators) were nurse-midwives, and co-facilitators were nurses and other clinic support staff.
The project adopted a group visit model for obstetrically low medical risk women that provided more health promotion; group peer support; a collaborative patient–provider relationship; and self-management training and activities. Women were taught to perform self-care activities and try out new skills in the supportive environment of the group. They also had access to information that is typically not shared, such as their medical charts. The concerns of the group set the priorities for the educational sessions who then participated in decision-making and learned to advocate for themselves and their families. All these strategies emphasised self-determination and partnership between provider and the women.
In the original study 110 women received group antenatal care. Women reported that they enjoyed sharing their pregnancy experience with other women. One said, ‘I loved the programme because every time you come you can share your story’. They appreciated that group members were like them, and felt they learned about pregnancy by sharing experiences and concerns. Another woman said, ‘I learned a lot about the pluses of breastfeeding … I changed my mind … I’m still breastfeeding him’. Compared to women in individual care, women in the study attended significantly more antenatal visits (9.7 versus 8.3) and gained significantly more weight during pregnancy (32.2 lbs versus 28.5 lbs). They were significantly more likely to have initiated breastfeeding during hospitalisation (59% versus 44%), and 44% were exclusively breastfeeding at hospital discharge, compared to 31% of the women in individual care. Data such as these are available in the WHO compendium report (2009) for many of the other case studies.
However, there are some barriers to be overcome in implementing models of community engagement. Several contributors emphasised the need to have faculty engaged in the PHC programmes so that students could be rotated through them, thus preparing the recruitment of future cohorts of nurses and midwives into PHC, building a sustainable workforce and embedding these types of initiatives in the communities and education systems. There were also a number of reports of medical and some nursing staff having difficulty in letting go of conventional and stereotypical thinking about who ought to perform those tasks (World Health Organisation, 2008). This issue has been much studied and discussed (see, eg, Chiarella, Reference Chiarella2002) and has been described as the ‘myth of the meritocracy’ – the possibility of work being taken on by another group, unless similarly qualified, is unthinkable because they are seen as incapable of meeting the challenge (Hall, Reference Hall1997).
Yet there is ample evidence and experience to show that different personnel and community members are capable of equal, high quality participation in health care decision-making and delivery (Chiarella, Reference Chiarella2002). Claims to maintain the status quo are often made on the grounds of safety and quality, so it is important to gather evidence about outcomes to ascertain whether this resistance to change is based only on protecting professional power and privilege. Other barriers include lack of sustainable funding and resources; access to medications and medical supplies and equipment and inadequately prepared staff.
Despite these barriers, from the work described here, community nursing could take the lead in working with communities to develop PHC models of care. However, to achieve this, nursing has to get organised nationally, be proactive, drive the debate and ‘hold the mirror up’ to government to show them what is already being achieved. For example, the Scottish model, whereby community health nursing is becoming the mainstay of the Scottish nursing workforce, is focused on providing services that meet local needs and complement and reflect national priorities as set out in government policy (NES Education for Scotland, 2006). This new discipline will build on the strengths of community nursing to work as part of nursing and multi-disciplinary, multi-agency teams and work directly with individuals and their carers; and will adopt a public health approach which supports self care and enablement. This is a welcome development in the development of PHC and the nursing workforce, which is responding to the needs of communities and is promoting ownership of programmes. These factors indicate a renewal and extension of the original ideals laid down at Alma-Ata in 1978 and highlight the interlinkage between the concepts of participation and coproduction.
Conclusion
Coproduction models of health care have a lot to offer PHC as well as the capacity to fulfill many of the PHC criteria such as universal access, community participation and fostering self-reliance and self-determination. Health care organisations and professionals must experience a paradigm shift in both their approach to providing health care and in their understanding of the health care consumer and their communities as co-producers and be prepared to embrace the concept of community partnership, moving towards community control, to make these models become a reality.
Acknowledgements
Jane Salvage received WHO funding to work on this project as a Consultant. Mary Chiarella worked pro bono as a Visiting Scholar to WHO on this project.
Appendix 1





