Older adults commonly experience stressors related to a decline in physical, cognitive, and functional abilities, loss of purpose and independence, bereavement, societal ageism, and financial hardships (Almeida et al., Reference Almeida, Schaie and Willis2011). Chronic stressors have cascading effects on physical and mental outcomes, including worse overall well-being, increased depression, and greater physical disability and mobility limitation (Dautovich et al., Reference Dautovich, Dzierzewski and Gum2014; Frias and Whyne, Reference Frias and Whyne2015; Kulmala et al., Reference Kulmala2013). Stressful events increase the likelihood of chronic metabolic, pulmonary, and cardiovascular diseases (Scott et al., Reference Scott2013). These stressors are often unavoidable in modern Western societies, given the realities of aging, so identifying methods to enhance older adults’ ability to manage stressors is essential.
Resilience is the process of adapting well in the face of adversity, trauma, loss, and other sources of stress (Ong et al., Reference Ong, Bergeman and Boker2009; Rutter, Reference Rutter2007). Resilience is a modestly heritable personality trait and is partially malleable (Chmitorz et al., Reference Chmitorz2018; Johnston et al., Reference Johnston2015). Resilience is associated with lower levels of anxiety, depression, and general psychological distress, and has a mediating effect on physical and mental health in people who have experienced trauma as children or adults, and those managing chronic health conditions (Hjemdal et al., Reference Hjemdal2011; Mujeeb and Zubair, Reference Mujeeb and Zubair2012; Stewart and Yuen, Reference Stewart and Yuen2011; Wingo et al., Reference Wingo2010). Resilience decreases perceived stress, and people who are less impacted emotionally by daily stressors have lower incidence of mood disorders 10 years later (Charles et al., Reference Charles2013), indicating the long-term value of pursuing methods of decreasing perceived stress.
Among older adults, high resilience has been shown to be a significant determinant of well-being, and is associated with lower levels of perceived stress as well as greater happiness, and better quality of life (Jeste et al., Reference Jeste2013; Lavretsky, Reference Lavretsky2014; MacLeod et al., Reference MacLeod2016; Smith and Hollinger-Smith, Reference Smith and Hollinger-Smith2015). Similarly, other constructs characterizing positive psychology and psychiatry (Jeste, Reference Jeste2018), including wisdom, optimism, personal growth, and happiness, positively impact well-being, mental health, and physical functioning among older adults (Depp et al., Reference Depp, Harmell and Jeste2014; Engel et al., Reference Engel2011; Jeste et al., Reference Jeste2015; Laird et al., Reference Laird2019; Reichstadt et al., Reference Reichstadt2010). Therefore, enhancing these outcomes may promote successful aging (Depp and Jeste, Reference Depp and Jeste2006; Reichstadt et al., Reference Reichstadt2010). However, only about a third of the older adults score high on resilience measures (Hildon et al., Reference Hildon2010; Jeste et al., Reference Jeste2013), indicating that increasing resilience may be a promising strategy to enhance well-being and quality of life among older adults.
Existing literature on methods to improve resilience among older adults is limited. The only study we found was a pilot study examining the use of a 1-week savoring intervention, which reported that adults over age 60 years who completed the brief intervention with high fidelity (i.e. engaged in the intervention for at least 6 days, 60% of the sample) showed reduced depression and improved resilience and happiness, unlike the other 40% participants, indicating that consistent engagement is important (Smith and Hanni, Reference Smith and Hanni2019). More broadly, a few interventions in older adults targeting related positive psychology/psychiatry domains have found evidence of benefit (Ho et al., Reference Ho, Yeung and Kwok2014; Killen and Macaskill, Reference Killen and Macaskill2015; Meléndez Moral et al., Reference Meléndez Moral2015).
The population of older adults living in senior housing communities is increasing (Jeste et al., Reference Jeste2019; Jeste and Childers, Reference Jeste and Childers2017), presenting an important opportunity to improve physical and mental healthcare in these communities (Borson et al., Reference Borson2019; Guo and Castillo, Reference Guo and Castillo2012). Implementing positive prevention strategies in senior housing communities offers a method to assist older adults in maintaining health, well-being, and independence as they age (Dong, Reference Dong2017; Guo and Castillo, Reference Guo and Castillo2012). However, we are aware of only two relevant studies, which examined a novel positive psychology intervention for older adults living in community centers or nursing homes in Hong Kong (Ho et al., Reference Ho, Yeung and Kwok2014) and a psychological fitness intervention in a retirement community (Short , Reference Short2012).
Therefore, our team developed a manualized psychological intervention, Raise Your Resilience (RYR), intended to improve resilience and related outcomes among older adults living in senior housing communities. We sought to design our trial based on the principles of pragmatic clinical trials (Mdege et al., Reference Mdege2011; Patsopoulos, Reference Patsopoulos2011). These are randomized controlled trials that focus on participants in real world, with few exclusion criteria, randomization at group rather than individual level, and administration of the intervention by unlicensed non-research staff. Development of RYR was driven by empirical literature including consistent findings that experience of positive emotions, savoring of positive experiences, and use of adaptive coping skills are associated with greater resilience among older adults (MacLeod et al., Reference MacLeod2016). This study assessed effects of RYR among older adults residing in independent living sector of five senior housing communities across three states. These individuals were expected to have relatively high resilience at baseline, though they still experienced a range of significant stressors. Our primary hypothesis was that older adults who participate in RYR would report higher levels of resilience and well-being and lower level of perceived stress at the end of the 1-month intervention. Exploratory aims included determining whether (a) the improvements in primary outcomes were maintained during the follow-up period; (b) RYR improved other positive psychiatry domains including wisdom, optimism, psychological growth, and happiness; and (c) baseline demographic variables, psychosocial measures, treatment adherence, and treatment satisfaction moderated changes in outcomes.
Methods
The Institutional Review Boards of the University of California San Diego and the Mather Institute approved this study. Every participant signed a written informed consent form.
Participants
Inclusion criteria were: an English-speaking individual over age 60 years who resided in independent living in one of the five senior living communities in suburban settings (Cardiff, CA; San Diego, CA; Evanston, IL; Wilmette, IL; and Tucson, AZ), and able to provide a written informed consent to participate. Exclusion criteria were: a diagnosis of dementia or any other serious or disabling illness that would prevent participation in the study. A priori power analyses determined that a sample of 90 participants would provide 90% power to detect a small to medium effect size (Cohen’s d 0.2–0.5) with a two-sided alpha = 0.05 (Cohen, Reference Cohen1988; Tu et al., Reference Tu2004). The recruited sample consisted of 89 participants with mean age of 84.9 (SD = 7.0) years. The sample was mostly female (77.5%) and almost entirely White (97.8%). There were no Hispanic/Latino participants. Half (50.6%) of the participants had completed at least some college, while an additional 44.9% had a postgraduate degree. Over half (58.4%) were widowed, 32.6% were currently married, 7.9% were divorced, and one participant had never married.
Participants were recruited from the specified senior housing communities through brief presentations and flyers. Selected staff members from each senior living community were trained in recruiting procedures including ethics guidelines. These staff contacted each potential participant to elicit interest in participating. Interested potential participants met with staff to complete the informed consent process and schedule baseline assessment.
Measures
In addition to demographic variables, participants completed a set of self-report measures. The first primary outcome, resilience, was measured using the 10-item Connor-Davidson Resilience Scale (CD-RISC; Campbell-Sills and Stein, Reference Campbell-Sills and Stein2007). The second primary outcome, well-being, was assessed using two measures: the 12-item Short-Form Health Survey (SF-12; Ware et al., Reference Ware, Kosinski and Keller1996), a measure of physical and mental well-being, and the Perceived Stress Scale (PSS; Cohen et al., Reference Cohen, Kamarck and Mermelstein1983). Positive psychosocial measures to examine our exploratory aim included the San Diego Wisdom Scale (SD-WISE; Thomas et al., Reference Thomas2019); the Subjective Happiness Scale (Lyubomirsky and Lepper, Reference Lyubomirsky and Lepper1999); the Psychological Growth subscale of the Attitudes to Aging Questionnaire (Kavirajan et al., Reference Kavirajan2011); and the Life Orientation Test – Revised (LOT-R; Glaesmer et al., Reference Glaesmer2012). Treatment adherence was assessed by monitoring the number of RYR sessions attended, and number of daily diaries completed during the 31-day intervention period. Participants in a subset of sites were also asked to complete a 6-item measure of treatment satisfaction, which was developed specifically to assess satisfaction with RYR (e.g. relevance of content, usefulness of activities). Most measures were completed at months 0 (baseline), 1 (pre-intervention), 2 (post-intervention), and 5 (3-month post-intervention follow-up); treatment satisfaction was assessed at month 2.
Intervention
RYR included savoring, gratitude, and engagement in value-based activities to improve resilience. Group members were taught to savor by recording one event each day that made them feel happy and one accomplishment or activity that made them proud in a daily diary. Gratitude practices were incorporated because they are associated with improved physical and mental health (Jans-Beken et al., Reference Jans-Beken2019; Killen and Macaskill, Reference Killen and Macaskill2015). Due to past findings that perceived age discrimination negatively impacts well-being and mental health via more negative perceptions of aging (Marquet et al., Reference Marquet2018), RYR incorporated explicit discussion of the impact of age discrimination and associated stereotypes along with methods to fight those stereotypes and improve perceptions of aging. RYR was delivered in three 90-minute sessions at weeks 1, 2, and 4 by a trained residential facilitator, and focused on three positive psychology-oriented topics: aging as a time of continued growth and enjoyment; making small changes to increase positive emotions; and engagement in values-driven activities. At the beginning of RYR, participants set short-term individualized goals to make life more enjoyable and meaningful. The group facilitator assisted in identifying and encouraging concrete values-driven activities to achieve participants’ short-term goals. At the end of 1-month RYR, the participants were encouraged to continue the daily diary during the 3-month follow-up period and beyond.
Procedure
This study used a modified stepped-wedge trial design, which is an alternative method of conducting cluster-randomized trials (Copas et al., Reference Copas2015; Hemming et al., Reference Hemming2015; Woertman et al., Reference Woertman2013). This approach allows for all participants to receive the intervention while still having data from a control period to compare the intervention data to. Specifically, a modified stepped-wedge trial clusters intervention delivery at multiple time points. All trial clusters undergo a control period and control assessment completion. Each “cluster” was one RYR group, and start dates for each group were spread across five time points across 14 total months. Unlike a classical stepped-wedge design, start dates were not uniformly staggered; they were chosen based on the readiness of each site. The control period consisted of treatment as usual. Each group underwent baseline assessment at month 0, followed by pre-intervention assessment at month 1, post-intervention assessment at month 2, and follow-up assessment at month 5. Thus, the control period (month 0 to 1) under the modified stepped-wedge design had the same length as the intervention period (month 1 to 2) for all groups to minimize potential practice effect (Elman et al., Reference Elman2018).
There were nine RYR groups across the five sites with 6–12 participants per RYR group. Trained, unlicensed facilitators from each local senior housing community conducted the groups. These facilitators were trained in delivering the manual by research staff, before the trial was initiated. (The manual can be made available to interested readers on request.)
Analytic plan
Generalized estimating equations (GEE) were employed (Tang et al., Reference Tang, He and Tu2012) to examine changes in target variables over time. As GEE does not impose any mathematical distribution requirements such as normality for valid inference (type I error), it provides more robust estimates for a broader class of data distributions than alternatives such as the generalized linear mixed-effects models (Tang et al., Reference Tang, He and Tu2012; Zhang et al., Reference Zhang2011). We also checked missing data mechanism and could not reject the missing completely random assumption (Tang et al., Reference Tang, He and Tu2012), which was not surprising given low rates of dropouts (i.e. 84.3% of participants had complete data). Thus, GEE provides valid inference for the current study.
Separate GEE models were used to identify changes in the primary outcome measures (i.e. CD-RISC, PSS, SF-12 Mental Well-being, and SF-12 Mental Well-being) during the intervention period (month 1 to month 2) and from pre-intervention (month 1) to follow-up (month 5). Changes during the intervention period (month 1 to month 2) were compared to changes during the control period (month 0 to month 1) to assess whether changes were attributable to the intervention. The same approach was repeated to identify changes in the exploratory outcome variables during the same time periods.
Separate moderation models for each type of moderator (i.e. demographic, psychosocial, treatment adherence, and treatment satisfaction) were estimated using GEE, including interactions between potential moderators and time. Demographic variables included in the moderation analysis were age, sex, and marital status. Psychosocial variables included in the moderation analysis were baseline PSS, SD-WISE, SF-12 Mental Well-being, and SF-12 Physical Well-being scores. Treatment adherence variables included two objective measures – that is, number of sessions attended and number of daily diaries completed. Treatment satisfaction was measured via the total score of the satisfaction measure. Effect size was calculated using Cohen’s d, using the standard deviation of the change in scores by computing pooled standard deviations.
Results
The number of dropouts over the 5-month trial period was small (n = 9, or 10%). The primary outcome, the CD-RISC score, did not change significantly during the intervention period (month 1–month 2) in comparison to the control period (month 0–month 1); however, it increased significantly from month 1 to month 5 (follow-up), Estimate = 1.052, SE = 0.454, p = 0.021, Cohen’s d = 0.115. The PSS score decreased significantly during the intervention period compared to the control period, Estimate = −1.705, SE = 0.607, p = 0.005, Cohen’s d = −0.192. Please see Figures 1 and 2 for a depiction of CD-RISC and PSS, respectively, over time.
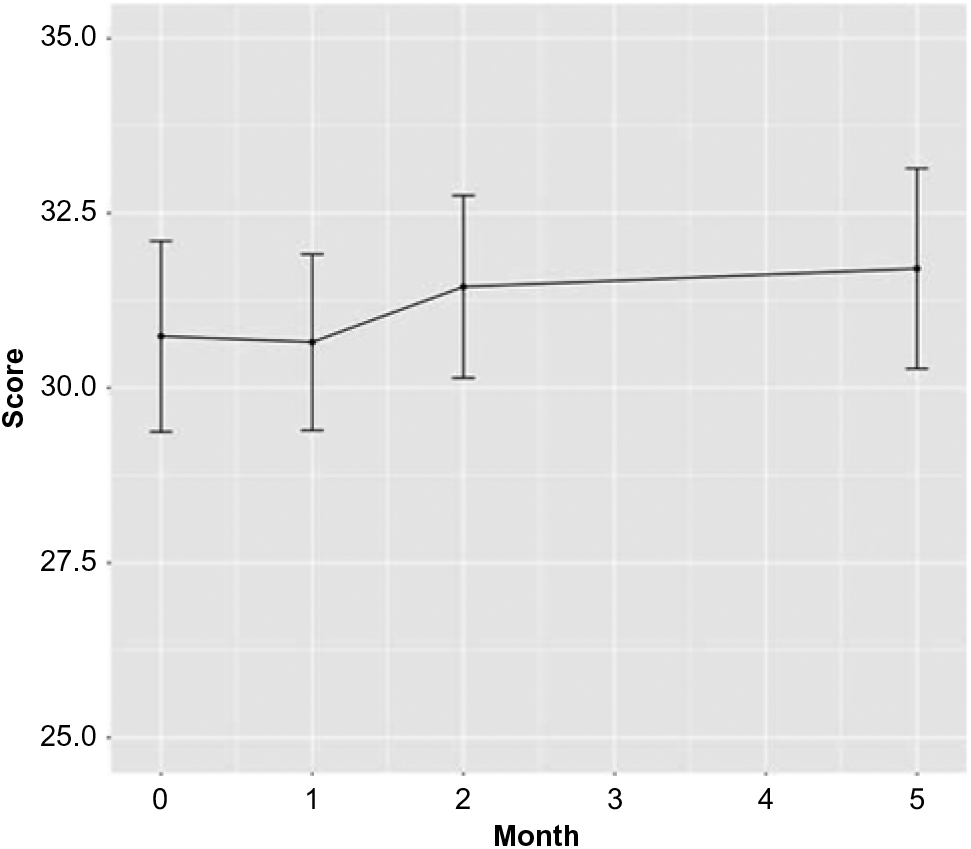
Figure 1. Change in resilience.
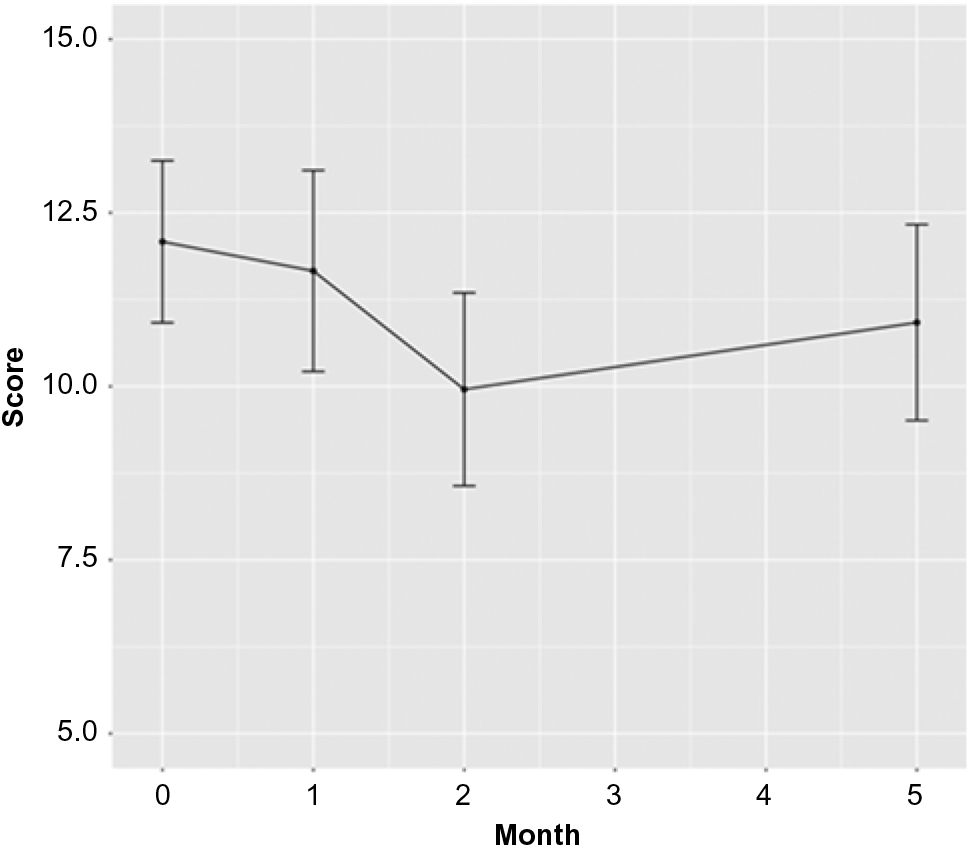
Figure 2. Change in perceived stress.
The SD-WISE total score increased significantly during the intervention period compared to the control period, Estimate = 0.112, SE = 0.038, p = 0.007, Cohen’s d = 0.251. Among SD-WISE subscales, Emotional Regulation (p = 0.002, Cohen’s d = 0.208) and Social Advising (p = 0.042, Cohen’s d = 0.180) improved during the intervention period compared to the control period, while Tolerance of Divergent Values approached significance over that period, p = 0.060, Cohen’s d = 0.221. The other SD-WISE subscales, Decisiveness, Insight, and Prosocial Behaviors, did not show significant changes, all ps > 0.05, Cohen’s ds = |0.05–0.17|. Table 1 includes SD-WISE total and subscale scores over time.
Table 1. SD-WISE total and subscale means and standard deviations over time
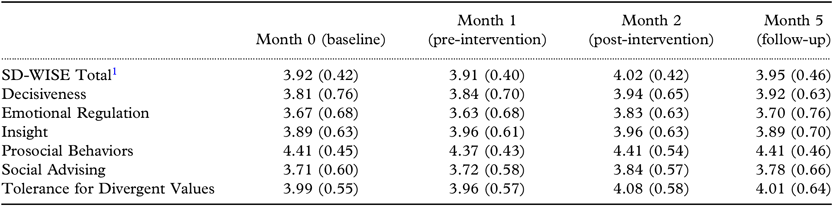
SD-WISE = San Diego Wisdom Scale (Thomas et al., Reference Thomas2019).
The SD-WISE total score increased significantly during the intervention period compared to the control period, Estimate = 0.112, SE = 0.038, p = 0.007, Cohen’s d = 0.251. Among SD-WISE subscales, Emotional Regulation (p = 0.002, Cohen’s d = 0.208) and Social Advising (p = 0.042, Cohen’s d = 0.180) improved during the intervention period compared to the control period, while Tolerance of Divergent Values approached significance over that period, p = 0.060, Cohen’s d = 0.221. The other SD-WISE subscales, Decisiveness, Insight, and Prosocial Behaviors, did not show significant changes, all ps > 0.05, Cohen’s ds = |0.05–0.17|.
1 The score range for SD-WISE total score and each subscale is 1–5, with higher numbers indicating higher level of wisdom.
Changes in SF-12 Physical or Mental Well-being, CES-D Happiness subscale, Psychological Growth, and LOT-R scores did not show significant change during the intervention period or from month 1 to month 5 (follow-up) compared to the control period, all ps > 0.05. All main effect model parameters are presented in Table 2.
Table 2. Main effect model parameters
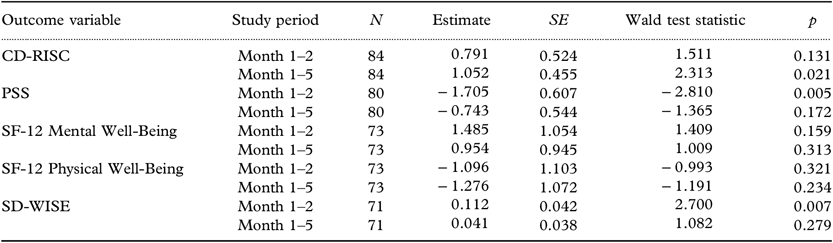
CD-RISC = Connor-Davidson Resilience Scale (Campbell-Stills and Stein, Reference Campbell-Sills and Stein2007); PSS = Perceived Stress Scale (Cohen et al., Reference Cohen, Kamarck and Mermelstein1983); SD-WISE = San Diego Wisdom Scale (Thomas et al., Reference Thomas2019); SF-12 = 12-item Short-Form Health Survey (Ware et al., Reference Ware, Kosinski and Keller1996).
Regarding treatment adherence, 66 participants (74.2%) attended all 3 RYR sessions, 9 participants (10.1%) attended 2 sessions, and 6 (6.7%) attended 1 session. Sixty-five (73.0%) participants turned their daily diaries in, and another six participants (6.74%) reported completing the journal but did not turn it in due to privacy issues. Of those who returned their daily diaries, the mean number of days completed (of a potential 31) was 23.1 (SD = 9.5) or 74%, and median was 28 days. The modal value of daily diaries completed was 31. Satisfaction with RYR was generally high. The average score of the satisfaction measure was 3.1 (SD = 0.53) on scale from 1 to 4 (4 indicating highest satisfaction).
Examination of potential moderator effects found no evidence that baseline demographic or psychosocial variables, treatment adherence, or treatment satisfaction moderated change in CD-RISC between pre-intervention (month 1) and post-intervention (month 2) or between pre-intervention (month 1) and follow-up (month 5), all ps > 0.05.
Discussion
This modified stepped-wedge pragmatic trial conducted in five senior housing communities across three states in the US examined RYR, a novel group intervention intended to improve resilience and associated positive outcomes among older adults. Compared to the control period, resilience improved among participants from pre-intervention to 3-month follow-up, and perceived stress and wisdom improved from pre-intervention to post-intervention. Effect sizes for these outcomes were small. There were no changes in physical and mental well-being. Examination of potential moderating effects yielded no significant moderators.
Although the effect sizes of the outcomes that changed significantly were small, this may be attributable, in part, to the high baseline resilience of the sample. The median baseline CD-RISC score was 32 (on a range of 0–40). This mirrors Arias Gonzalez and colleagues’ conclusion (Reference Arias González2015) that ceiling effects in CD-RISC may prevent capturing the full range of resilience, particularly for nonclinical populations. Still, it is notable that among these highly resilient participants, further significant improvements were detected, consistent with our goal of preventing decline in health and well-being by fostering protective psychological mechanisms.
Although scores trended upward from pre-intervention to post-intervention, changes in resilience were only significant from pre-intervention to 3-month follow-up. This indicates the value of continued use of the practices taught in RYR, including use of a daily diary and engagement in value-based behavior. Smith and Hanni (Reference Smith and Hanni2019) also found evidence that resilience continued to increase in the 3 months following participation in a 1-week savoring intervention. Treatment adherence did not moderate changes in resilience in our study, unlike Smith and Hanni’s findings. This could be because of the considerably high adherence in our sample, and thus limited variance. Additionally, again unlike Smith and Hanni, we did not measure post-intervention engagement in treatment activities like daily diary completion. Additionally, some participants reported reluctance to turn in their daily diaries due to privacy concerns. Measuring diary use while maintaining participant privacy is a delicate balance in need of further fine-tuning.
Significant improvements in perceived stress and wisdom occurred from pre-intervention to post-intervention. The pursuit of improving resilience is ultimately rooted in the goal of reducing stress and its widespread and deleterious impacts (Dautovich et al., Reference Dautovich, Dzierzewski and Gum2014; Frias and Whyne, Reference Frias and Whyne2015; Kulmala et al., Reference Kulmala2013). Our results show changes in both areas; improving positive outcomes (i.e. resilience and wisdom) and reducing negative ones (i.e. perceived stress). Reduction of stress, even with the small effect size, can boost older adults’ health and help them function independently longer (Almeida et al., Reference Almeida, Schaie and Willis2011).
This study has several limitations that should be acknowledged. First, the findings require replication. We did not use traditional randomization. However, the modified stepped-wedge design allowed for examination of changes during a control period, indicating that the improvements in perceived stress and wisdom were related to participation in RYR. We did not use an active control group for comparison. Examining change during the intervention period alone and from baseline to follow-up inflates the likelihood of a type I error, although inclusion of effect sizes improves interpretation confidence. The small size of the effects is also a limiting factor for clinical significance. Due to the potential ceiling effects, examining the impact of RYR in a sample with lower baseline resilience and those in assisted living facilities would be valuable. Additionally, the outcome measures used were based on self-report. In future, at least semi-objective measures such as reports by family members and facility staff might be useful. Our treatment adherence measures might not have been sufficiently sensitive. Perhaps daily monitoring of practices during intervention and follow-up periods via ecological momentary assessment (Moore et al., Reference Moore2016) might provide more sensitive assessment of treatment adherence. Additionally, we did not measure continued completion of daily diaries after the end of the intervention, which would have elucidated post-intervention engagement.
Notwithstanding these limitations, this study adds to the literature in several ways; primarily, by presenting a novel resilience intervention targeted specifically for older adults. Additionally, to our knowledge, this is the first study to examine a manualized resilience intervention delivered within senior housing communities and provided by non-licensed retirement community staff trained by the research team. We employed a pragmatic trial design, modified stepped-wedge design, which is participant-friendly and feasible, especially for group interventions. The number of dropouts was small, and both treatment adherence and satisfaction were high. These findings support the feasibility of conducting high-caliber pragmatic intervention trials in senior housing communities.
Prevention and intervention strategies delivered in senior housing communities by non-licensed residential staff have the ability to reach many older adults who might not be able to or might not choose to access mental healthcare. This approach provides preventive care for older adults at risk, increasing their ability to handle the common stresses of aging while continuing to pursue meaning and growth, and without requiring these communities to hire licensed mental health providers. All these characteristics heighten the implementation and dissemination potential of RYR while increasing accessibility for older adults who may have limited mobility and access to transportation. Such interventions will play an important role in promoting resilience and other facets of positive psychiatry in late life.
Conclusions
This study presented a novel psychological intervention, using pragmatic trial design, intended to improve resilience in older adults in an important setting: senior housing communities, where growing numbers of older adults will live, providing a vital opportunity to increase accessibility of intervention strategies to support successful aging. There was improvement in perceived stress and wisdom, and over a longer period, in resilience. The study sample had relatively high baseline resilience, which both enhanced the meaningfulness of these small effects, and also indicated that effects may be larger among older adults with lower baseline resilience or those in assisted living facilities. Consideration of interventions that can be implemented within senior housing communities is important to enhancing the health and well-being of older adults who may struggle to access formal mental healthcare.
Conflicts of interest
Authors CO and JS acknowledge being employees of a funding source, Mather Institute. No other conflicts of interest exist for any authors.
Source of funding
This work was supported, in part, by the Mather Institute and by the National Institute of Mental Health T32 Geriatric Mental Health Program (grant MH019934 to DVJ [PI]), and an R01 grant (R01MH094151-01 to DVJ [PI]), and the Sam and Rose Stein Institute for Research on Aging, University of California San Diego.
Description of authors’ roles
ET contributed to study design, wrote the first draft of the manuscript, oversaw statistical analyses, and created tables and figures. DG contributed to development of the RYR intervention and study design, oversaw data collection, and contributed to manuscript writing. EL contributed to study design, statistical approach, and manuscript writing. TW completed the majority of statistical analyses, created tables and figures, and contributed to manuscript writing. XT supervised all statistical analyses and overall statistical approach, and contributed to manuscript writing. RD supervised data collection and data entry, contributed to statistical analyses, and contributed to manuscript writing. CO contributed to development of the RYR intervention and study design, coordinated and oversaw data collection, and contributed to manuscript writing. JS contributed to development of the RYR intervention and study design, coordinated and oversaw data collection, and contributed to manuscript writing. DJ contributed to development of the RYR intervention and study design, coordinated and oversaw data collection, contributed to statistical analysis approach, and contributed to manuscript writing.
Sponsor’s role
Two of the co-authors of this paper are employees of the Mather Institute (CO and JS). They were not involved in the data analysis or the preparation of the paper; however, they edited the paper. They were involved in the design, methods as well as subject recruitment and data collection at Evanston, Wilmette, and Tucson sites for this study.
Impact statement
We certify that this work is novel clinical research. This research makes two major contributions to the literature. First, it demonstrates the feasibility and acceptability of an innovative pragmatic clinical trial in senior housing communities, using a multisite stepped-wedge design and employing a manualized group intervention administered by unlicensed residential staff trained by research team. Second, it provides evidence that a novel, brief psychological intervention can improve resilience and wisdom, and reduce perceived stress, albeit with small effect size, among independent living adults with relatively high levels of baseline resilience.
Acknowledgments
We gratefully acknowledge Cheryl Jennifer McClune, MSW, for her contributions to the RYR manual, and Belmont Village Senior Living for their support and dedication to this project.






