It has been suggested that the experience of psychosis may have toxic effects on the brain (e.g. Reference WyattWyatt, 1991; Reference Lieberman, Sheitman and KinonLieberman et al, 1997). Such a possibility is of considerable interest because it could provide a rationale for early intervention in the treatment of psychosis (e.g. Reference McGorry, Edwards and MihalopoulosMcGorry et al, 1996; Reference Malla, Norman and VorugantiMalla et al, 1999). The relationship of duration of untreated psychosis (DUP) to cognitive functioning is of interest both because any neural toxic effects of DUP are likely to be reflected in cognitive functioning, and because of evidence that cognitive performance can be an important predictor of community functioning (Reference GreenGreen, 1996) and level of recovery after treatment (Reference Moritz, Krausz and GottwaizMoritzet al, 2000). In this paper we present findings from a study of first-episode patients to whom a comprehensive battery of cognitive tests was administered. In addition, careful assessment was made of a number of variables, including DUP, that are potentially related to prognosis for those patients. The data were analysed for the purpose of assessing the relationship of DUP and other variables to indices of cognitive functioning.
METHOD
Participants in this study were 113 patients presenting with their first episode of a psychotic disorder to the Prevention and Early Intervention Program for Psychosis (PEPP) in London, Ontario, Canada. All patients were diagnosed as having a psychotic disorder for which they had not previously received treatment for a period greater than 4 weeks.
Untreated psychosis can vary in its course, with some individuals experiencing symptoms continually from onset of the disorder until effective treatment begins, while in other cases the psychosis has a more intermittent course. Hypotheses about the possible toxic effects of psychosis have not specified whether it is the cumulative experience of active psychosis or the time since the initial onset of any psychotic symptoms that is most relevant. The information collected in this study was, therefore, used to estimate both. Onset of treatment was defined as commencement of antipsychotic therapy within PEPP. The period from initial onset of psychosis to treatment is referred to as DUP(onset), and the estimated cumulative period of active psychosis as DUP(active). In addition information was collected by which to estimate duration of untreated illness (DUI), which was defined as the period between the onset of any psychiatric symptoms and initiation of treatment.
Both DUP estimates and DUI were rated for each patient on the basis of all information from structured interviews with patients and relatives (using a modified version of the Interview for the Retrospective Assessment of the Onset of Schizophrenia, Reference Hafner, Riecher-Rossler and HambrechtHafner et al, 1992) and review of hospital records. To establish interrater reliability, estimates of DUP as well as DUI were independently assessed by two clinicians (a psychiatrist and a clinical psychologist) on 12 randomly selected patients. The intraclass correlation coefficients for these ratings were all within acceptable limits (0.81 to 0.98). The correlation between DUP(active) and DUP(onset) was 0.87 (P<0.001).
As part of the standard assessment in PEPP, information was collected on the number of years of completed education, judged role of substance use or misuse in precipitating psychosis and history of substance misuse. Handedness was also assessed through questioning and observation of the hand used for tasks such as writing, throwing and using scissors. In addition, a diagnostic interview based on the Structured Clinical Interview for DSM-IV Disorders (Reference First, Spitzer, Gibbon and WilliamsFirst et al, 1997) was carried out and the Premorbid Adjustment Scale (Reference Cannon-Spoor, Potkin and WyattCannon-Spoor et al, 1982) was completed.
As soon as possible after the participant's entry into PEPP, a battery of cognitive tests was administered by an experienced technician under the supervision of a psychologist. If patients were experiencing acute symptoms of psychosis or disorganised thinking that could interfere with their comprehension of test instructions or their ability to complete the tests, then the assessment was delayed until such symptoms resolved. The mean interval between entry into the programme and the administration of the test battery was 10 weeks (median 7 weeks). Among the instruments used were the following tests.
Wechsler Adult Intelligence Scale and National Adult Reading Test
The Wechsler Adult Intelligence Scale (WAIS-III) and National Adult Reading Test (NART) were used to estimate current and premorbid IQ, respectively. Given that the effects of DUP might be more clearly detectable in indices reflecting deterioration from premorbid levels of functioning, the NART (Reference NelsonNelson, 1982) was used as an index of premorbid verbal, performance and full-scale IQ (Reference Crawford, Parker and BessonCrawford et al, 1988). Estimates of cognitive deterioration were based on current full-scale, verbal and performance IQ as assessed by WAIS-III minus the relevant NART estimates of premorbid IQ.
Wechsler Memory Scale
The Wechsler Memory Scale III (WSM-III) provides a standardised assessment of several areas of memory function including immediate and delayed auditory and visual memory and working memory (Reference WechslerWechsler, 1997).
Paced Auditory Serial Addition Test
The Paced Auditory Serial Addition Test (PASAT) provides a measure of sustained attention and speed of processing (Reference GronwallGronwall, 1977). A tape-recording of 60 randomly arranged numbers between one and nine is played to the patient, who is required to add the most recently presented number to the number immediately preceding it and report the answer verbally.
Wisconsin Card Sort Task
The computerised version of the Wisconsin Card Sort Task (WCST) is a measure of ‘executive function’ involving abstract concept formation and ability to shift and maintain set (Reference BergBerg, 1948). The most frequently used indices of performance on the WCST are the number of categories completed and percentage of perseverative errors.
Stroop Colour and Word Test
In the Stroop Colour and Word Test respondents have to use selective attention and inhibition to identify the ink colour in which the words ‘red’, ‘green’ and ‘blue’ are printed. The score was calculated as the total number of correct responses in a 90-second period (Reference GoldenGolden, 1978).
Trail-making Test
The Trail-making Test (TMT) is a measure of visuomotor coordination in which subjects must connect circles in one form (A) on the basis of a simple rule of consecutive numbers and in the second form (B) by alternating between numerical and alphabetical sequences. For both forms, A and B, time for completion was used as the primary index of performance (Reference ReitanReitan, 1958).
Thurstone Word Fluency Test
The Thurstone Word Fluency Test assesses written verbal fluency (Reference Thurstone and ThurstoneThurstone & Thurstone, 1962). Subjects are asked to list as many four-letter words as possible in 5 minutes beginning with the letter S and in 4 minutes beginning with the letter C. Oral verbal fluency was assessed through a semantic naming test in which subjects were asked to name as many animals as possible within 1 minute.
Continuous Performance Test
The Continuous Performance Test (CPT) assesses the capacity for sustained attention. The particular version of the CPT used was the identical pairs using numbers (Reference Cornblatt and KeilpCornblatt & Keilp, 1994). The primary index of performance is d′, which reflects the discrimination of a signal from background noise.
Prospective Memory Screening
Prospective memory (remembering to carry out actions) is an aspect of memory functioning that is important in everyday life and is not explicitly included in the Wechsler Memory Scales (Reference Dalla Barba, Boiler and GrafmanDalla Barba, 1993). The self-report memory questionnaire included in the Prospective Memory Screening (PROMS) includes an assessment of prospective memory (Reference Sohlberg, Mateer and GeyerSohlberg et al, 1985). The PROMS was introduced into the cognitive assessment battery later than other tests and, therefore, results using this test are based on a reduced sample of 54 patients.
Cognitive Failures Questionnaire
The Cognitive Failures Questionnaire (CFQ) was developed to assess self-reports of everyday slips or errors in cognitive functioning. The CFQ has demonstrated sensitivity to everyday cognitive errors that are frequently not revealed in a laboratory setting, and appears to be uncorrelated with measured intelligence and educational level (Reference Broad bent, Cooper, Fitzgerald and ParkesBroadbent et al, 1982).
RESULTS
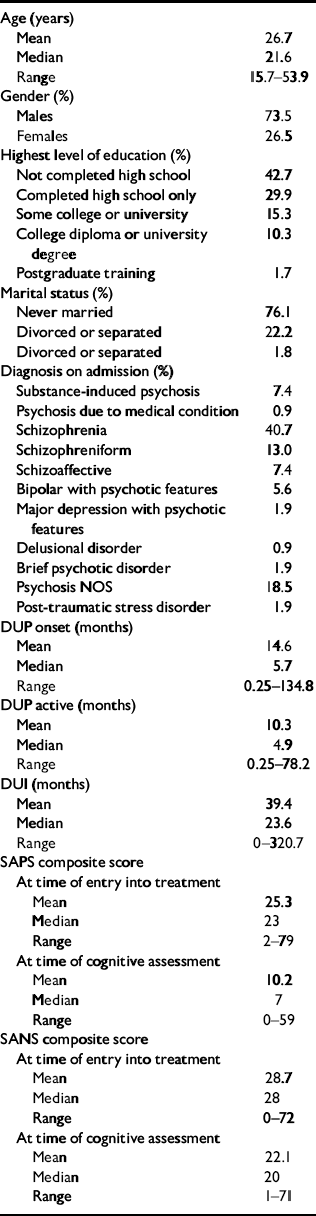
Table 1 lists the demographic and clinical characteristics of the participants at the time of the cognitive assessment. As would be expected for a first-episode sample, subjects were predominantly young (two-thirds being 25 years of age or younger) with a very large proportion being unmarried and not yet having completed high school.
Table 1 Demographic and clinical characteristics of sample (n=113)
| Age (years) | |
| Mean | 26.7 |
| Median | 21.6 |
| Range | 15.7-53.9 |
| Gender (%) | |
| Males | 73.5 |
| Females | 26.5 |
| Highest level of education (%) | |
| Not completed high school | 42.7 |
| Completed high school only | 29.9 |
| Some college or university | 15.3 |
| College diploma or university degree | 10.3 |
| Postgraduate training | 1.7 |
| Marital status (%) | |
| Never married | 76.1 |
| Divorced or separated | 22.2 |
| Divorced or separated | 1.8 |
| Diagnosis on admission (%) | |
| Substance-induced psychosis | 7.4 |
| Psychosis due to medical condition | 0.9 |
| Schizophrenia | 40.7 |
| Schizophreniform | 13.0 |
| Schizoaffective | 7.4 |
| Bipolar with psychotic features | 5.6 |
| Major depression with psychotic features | 1.9 |
| Delusional disorder | 0.9 |
| Brief psychotic disorder | 1.9 |
| Psychosis NOS | 18.5 |
| Post-traumatic stress disorder | 1.9 |
| DUP onset (months) | |
| Mean | 14.6 |
| Median | 5.7 |
| Range | 0.25-134.8 |
| DUP active (months) | |
| Mean | 10.3 |
| Median | 4.9 |
| Range | 0.25-78.2 |
| DUI (months) | |
| Mean | 39.4 |
| Median | 23.6 |
| Range | 0-320.7 |
| SAPS composite score | |
| At time of entry into treatment | |
| Mean | 25.3 |
| Median | 23 |
| Range | 2-79 |
| At time of cognitive assessment | |
| Mean | 10.2 |
| Median | 7 |
| Range | 0-59 |
| SANS composite score | |
| At time of entry into treatment | |
| Mean | 28.7 |
| Median | 28 |
| Range | 0-72 |
| At time of cognitive assessment | |
| Mean | 22.1 |
| Median | 20 |
| Range | 1-71 |
The single most common diagnosis on entry into PEPP was schizophrenia, with psychosis not otherwise specified (NOS) and schizophreniform psychosis being the next most frequent. The comparatively high rate of psychosis NOS is undoubtedly due to the early stage of the illness at which many of these individuals were being seen. Experience in PEPP suggests that the great majority of individuals diagnosed with schizophreniform disorder or psychosis NOS on entry progress to a diagnosis of schizophrenia or schizoaffective disorder.
Although only about 7% of the patients were diagnosed as having substance-induced psychosis, alcohol and/or drug misuse was judged to have been a significant contribution to onset of psychosis in 23.1% of cases.
The average DUPs and DUI for this sample are within the range reported by other investigators such as Haas et al (Reference Haas, Garratt and Sweeney1998) and Larsen et al (Reference Larsen, McGlashan and Moe1996), and each shows a positively skewed distribution. Log transformation of the three estimates resulted in a non-skewed distribution and these transformed variables were used for all analyses relating DUP and/or DUI to other variables.
At the time of cognitive assessment, 16 patients were not receiving any antipsychotic medication, four were receiving haloperidol, three flupenthixol and four were in a double-blind drug trial. All the others were receiving treatment with novel antipsychotic agents (primarily risperidone and olanzapine).
The data showed substantial levels of dispersion on all cognitive indices, and the ranges and standard deviations were comparable to those reported by others (Reference Spreen and StraussSpreen & Strauss, 1991).
Predictors of cognitive functioning
Before examining the relationship of DUP to cognitive functioning, it seemed appropriate to examine the possible relationship of cognitive functioning to several other factors: gender, medication, handedness, diagnosis, education, substance use and misuse and premorbid adjustment. In each case, given the number of cognitive variables being examined, the 0.01 level was used for identifying the statistical significance of any relationship.
Gender
There were gender differences on several of the cognitive indices, each of which suggested a better level of functioning by men. Men had significantly higher estimated full-scale, verbal and performance IQ on the WAIS-III (t=3.70, P < 0.001; t=3.30, P < 0.01; and t=3.27, P < 0.01, respectively). The differences in mean IQs ranged between 13 and 15 points. Males also showed significantly superior performance on the information, comprehension, picture completion, block design, matrix reasoning, object assembly sub-tests and the verbal comprehension and perceptual organisation indices of the WAIS-III. Evidence of a discrepancy such that estimated premorbid IQ is greater than current IQ is often interpreted as reflecting deterioration. Given that there were no significant gender differences on the estimates of premorbid IQ on the NART, the WAIS-III differences also resulted in females showing significantly greater estimated deterioration (using the NART-WAIS-III contrast) in full-scale, verbal and performance IQ than did males (t=4.28,P < 0.001; t=4.07, P < 0.001; andt=3.6, P < 0.001, respectively). Males also showed significantly fewer perseveration errors on the WCST (t=3.49,P < 0.01).
Age of onset
Age of onset of psychosis was not found to be correlated with any of the cognitive indices except TMT B performance wherein later age of onset was associated with poor performance (r=0.33, P < 0.01).
Medication
Medication being received by the patient at time of cognition assessment was examined. The only three medication conditions for which there were 10 or more patients were no medication (n=14), risperidone (n=48) and olanzapine (n=26). Contrasts were carried out between these three conditions to assess whether there were significant differences on any of the cognitive indices. None of the differences in mean performance reached the 0.01 level of significance.
Handedness
Of the 113 participants, 101 were right-handed and 12 were left-handed. Cognitive indices on which left-handed subjects showed poorer performance than right-handed subjects were the letter-number sequencing and digit symbol sub-tests and processing speed index on the WAIS-III, and all indices of visual and auditory memory (immediate, delayed and general), and the working memory index on the WMS-III.
Diagnosis
The only cognitive variable to which overall category of diagnosis was related at the 0.01 level was the matrix reasoning subscale of the WAIS-III, on which those considered to be suffering from a substance-induced or medically related psychosis performed substantially better than the other groups.
Substance misuse
There were no significant differences in cognitive performance between those for whom substance misuse was an apparent contributor to onset and those for whom it was not.
Education
Years of education were positively related to verbal, performance and full-scale WAIS-III IQ (r=0.51, 0.34 and 0.44, respectively, allP < 0.01) as well as all WAIS-III sub-scores except picture completion, block design and object assembly. More education was also related to better performance on the NART (r=0.47, P < 0.001), Stroop test (r=0.30, P < 0.01), written word fluency test (r=0.33, P < 0.01), d′ on the CPT (r=0.37, P < 0.001) and the immediate and delayed auditory memory and working memory indices of the WMS-III (r=0.32, 0.32 and 0.34, respectively, P < 0.01).
Premorbid adjustment
The Premorbid Adjustment Scale (PAS) provides ratings of premorbid adjustment for childhood (up to age 11 years), early adolescence (ages 12-15 years), late adolescence (16-18 years) and adulthood (19 years and over), as well as a general assessment of premorbid adjustment prior to onset of illness. Because of the young age of most of the sample, only premorbid adjustment in childhood and adolescence was examined as a predictor of cognitive functioning. Better premorbid adjustment in childhood was associated with better performance on many of the indices of cognitive functioning including full-scale, verbal and performance IQ as assessed by the WAIS-III as well as most of its sub-tests; all WMS-III indices; NART estimated premorbid IQ; written word fluency; and CPT performance. Better premorbid adjustment during early or late adolescence was related to fewer cognitive indices at the 0.01 significance level — letter-number sequencing and comprehension on the WAIS-III; WMS-III delayed visual memory, immediate auditory, working memory and general memory indices; and CPT performance as reflected ind′.
Relationship of DUP and DUI to cognitive performance
Table 2 reports the first-order correlations of log transformed DUP(onset), DUP(active) and DUI with the cognitive performance indices. Only one of the correlations was significant at the 0.01 level. The one significant result was a correlation of −0.26 between DUP(active) and the index of deterioration in verbal IQ, suggesting less deterioration being associated with longer periods of active untreated psychosis. Six-month or 1-year cut-offs have sometimes been used by those examining the significance of DUP (e.g. Reference McGorry, Edwards and MihalopoulosMcGorry et al, 1996; Reference Haas, Garratt and SweeneyHaas et al, 1998). When DUP or DUI were dichotomised around either of these cut-offs,t-tests revealed no significant findings of longer DUPs or DUI being related to poor cognitive functioning.
Table 2 Correlations of DUP and DUI with cognitive performance

| Cognitive index | DUP onset | DUP active | DUI |
|---|---|---|---|
| WAIS-III | |||
| Full-scale IQ | -0.07 | -0.08 | 0.04 |
| Verbal IQ | -0.06 | -0.07 | 0.04 |
| Performance IQ | -0.05 | -0.06 | 0.08 |
| Vocabulary | 0.02 | 0.05 | 0.11 |
| Similarities | 0.02 | 0.00 | 0.07 |
| Arithmetic | -0.07 | -0.08 | 0.07 |
| Digit span | 0.01 | 0.02 | 0.10 |
| Information | -0.06 | -0.06 | -0.02 |
| Comprehension | -0.18 | -0.23 | -0.10 |
| Letter/number/space sequence | -0.04 | -0.07 | 0.05 |
| Picture completion | -0.07 | -0.02 | -0.02 |
| Digit symbol | -0.03 | 0.02 | 0.05 |
| Block design | -0.22 | -0.15 | -0.04 |
| Matrix reasoning | 0.00 | -0.03 | 0.14 |
| Picture arrangement | 0.05 | -0.02 | 0.14 |
| Symbol search | -0.13 | -0.07 | -0.06 |
| Object assembly | -0.07 | -0.07 | 0.04 |
| Verbal communication index | -0.02 | -0.02 | 0.05 |
| Perceptual organisation index | -0.08 | -0.08 | 0.04 |
| Processing speed index | -0.11 | -0.05 | -0.02 |
| NART estimate | |||
| Full IQ | 0.01 | 0.07 | 0.10 |
| Verbal IQ | 0.01 | 0.07 | 0.10 |
| Performance IQ | 0.02 | 0.08 | 0.10 |
| Stroop word/colour | -0.01 | 0.07 | 0.06 |
| WMS-III | |||
| General index | -0.02 | -0.08 | -0.08 |
| Auditory immediate | -0.01 | -0.10 | -0.12 |
| Auditory delayed | 0.00 | -0.07 | -0.03 |
| Auditory recognition | -0.09 | 0.16 | -0.02 |
| Visual immediate | 0.11 | 0.11 | 0.00 |
| Visual delayed | 0.08 | 0.07 | -0.05 |
| Immediate memory | 0.03 | -0.03 | -0.10 |
| Working memory | -0.12 | 0.11 | -0.02 |
| WCST categories | -0.11 | -0.09 | -0.03 |
| % perseverative errors | 0.09 | 0.08 | 0.04 |
| Trail-making test | |||
| A | 0.14 | 0.00 | 0.06 |
| B | 0.06 | 0.05 | 0.00 |
| Written word fluency | -0.01 | -0.03 | 0.07 |
| Oral word fluency | 0.04 | 0.13 | 0.10 |
| PROMS | 0.09 | 0.02 | 0.11 |
| CPT d′ | 0.00 | 0.02 | 0.02 |
| Deterioration estimates based on NART—WAIS—III | |||
| Full scale | -0.19 | -0.24 | -0.12 |
| Verbal | -0.21 | -0.26* | -0.12 |
| Performance | -0.16 | -0.19 | -0.10 |
| CFQ | 0.09 | 0.02 | 0.13 |
The possibility exists that some relations between DUP and cognitive functioning are being masked by other variables. An important consideration in this context is the extent to which DUP (or DUI) is correlated with any of the above variables that might be expected to influence cognitive functioning. Both DUP(onset) and DUP(active) were found to be significantly correlated with poor premorbid adjustment during early and late adolescence (r values between 0.27 and 0.33, P < 0.01). Furthermore, DUP and DUI were significantly greater for patients who were not receiving antipsychotic medication at the time of cognitive testing (F[1,111]=17.4, 16.3 and 10.2 for DUP(active), DUP(onset) and DUI respectively, all P < 0.01). This is a particularly interesting finding, the possible implications of which we shall return to later.
Partial correlations between log transformed DUP and cognitive indices were calculated removing the variance attributable to years of education, premorbid adjustment, handedness, gender and whether or not the patient was receiving antipsychotic medication. In no case were significant relationships found that would indicate that longer DUPs were associated with poorer cognitive performance.
Bilder et al (Reference Bilder, Degreef and Pandurangi1988) suggested that neuropsychological indices are more likely to reflect structural abnormalities in the brain when level of premorbid functioning is controlled. The measures of premorbid functioning used by Bilder et al were age-standardised WAIS sub-test scores for vocabulary and information. Another index likely to reflect premorbid functioning that was included in this study is premorbid IQ as estimated by NART. When partial correlations were calculated controlling for either of these estimates of premorbid functioning, the results did not show evidence of a significant negative correlation between DUPs, DUI and any index of cognitive performance.
DISCUSSION
DUP and cognitive functioning
Our findings yield no evidence of longer DUP or DUI being associated with more impaired performance on cognitive tests. This fails to support the hypothesis of a neurotoxic effect of psychosis, at least to the extent to which such effects would be reflected in neurocognitive performance.
The estimation of DUP and DUI is challenging, but the methods used in the current study yielded good interrater reliability. Furthermore, the indices of DUP, DUI and cognitive performance showed dispersion comparable to previous reports and so restricted variation does not appear to be a plausible explanation for our negative findings.
There was evidence of a significant negative correlation between DUP, particularly the period of untreated active psychosis, and an index of deterioration in verbal IQ based on the discrepancy between WAIS-III and NART scores. Finding that longer DUP is associated with less evidence of cognitive deterioration is counter to the hypothesis of psychosis having toxic effects, but could reflect the ability of individuals with less deterioration to function for longer periods without treatment.
Consistency with other reports
The only other report of which the authors are aware that examines the relationship between DUP and cognitive functioning is a paper by Barnes et al (Reference Barnes, Hutton and Chapman2000). In a smaller sample and using a somewhat different cognitive battery, they too found no relationship of longer DUP or DUI to poorer cognitive function. Should future studies similarly fail to find relationships between DUP (in particular) and indices related to brain functioning, it would clearly call into question the hypothesis that the experience of psychosis, in itself, has a major and at least partially irreversible influence on brain functioning.
The differences found in cognitive performance as a function of handedness, education and premorbid adjustment parallel those reported by others (Reference Bilder, Lipschutz-Broch and ReiterBilder et al, 1992; Reference Albus, Hubmann and MohrAlbus et al, 1997). The finding that males performed better on several cognitive indices than did females may seem surprising given that women are often reported to have a better response to treatment than men (Reference Castle and MurrayCastle & Murray, 1991). Nevertheless, there is evidence that past findings of greater cognitive deficits for males are not always replicated and/or may be restricted to chronic patients rather than those early in the course of such illness (Reference Hoff, Wieneke and FaustmanHoff et al, 1998). Our finding of no relationship between age of onset and cognitive impairment is also consistent with recent evidence (Reference Heaton, Gladsjo, Palmer, Kuck, Marcotte and JostoHeaton et al, 2001).
Other possible mediators of the effects of DUP
If the experience of longer untreated psychosis does not result in deterioration of brain functioning, why, then, is there some evidence (e.g. Reference Loebel, Lieberman and AlvirLoebel et al, 1992; Reference McGorry, Edwards and MihalopoulosMcGorry et al, 1996) that patients with shorter DUP may have a better response to treatment, at least for the first year or two? There are several potential mediators of a relationship between DUP and response to treatment, including the extent of psychological engulfment by the illness, and compromised social support (e.g. Reference Erickson, Beiser and laconoErickson et al, 1989; Reference Aguilar, Haas and ManzaneraAguilar et al, 1997). Another possibility is that longer DUP is associated with a tendency to less adherence to an antipsychotic medication regimen. There have been some reports suggesting that individuals with longer DUP may have had a tendency to take sporadic or token amounts of medication (e.g. Reference Haas and SweeneyHaas & Sweeney, 1992; Reference Larsen, McGlashan and MoeLarsen et al, 1996). As noted earlier, there was some association in our study between longer DUP and decreased likelihood of receiving antipsychotic medication at time of testing. A review of case notes and discussions with treating clinicians of such patients in our sample revealed that a common reason for not receiving medication was reluctance on the part of the patient to take an antipsychotic drug. It will be important to investigate the possibility that common factors such as denial, embarrassment and distrust of medical treatment could result in both prolonged DUP and reluctance to adhere to treatment, and that the latter may be one mediator of any relation of DUP to treatment outcome.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Duration of untreated psychosis (DUP) does not appear to be related to cognitive functioning early in the course of treatment.
-
• Any advantages of early intervention for psychosis may be mediated through other factors such as reduced likelihood of psychological engulfment, compromised social support, etc.
-
• The possible relationship of DUP to adherence to treatment regimen needs further examination.
LIMITATIONS
-
• Results of long-term follow-up of cognitive functioning were not included.
-
• Any neural toxic effects of DUP may become apparent with use of physical measures of brain functioning or structure.
-
• Potential mediators of the impact of DUP on clinical outcome, other than neurotoxicity as assessed through cognitive functioning, were not examined.





eLetters
No eLetters have been published for this article.