Food insecurity affects more than 680 million people across the world(1), with serious implications for many chronic conditions, including diabetes and obesity. In the USA, 11·8 % of households are food insecure. The largest federal programme targeted at alleviating food insecurity is the Supplemental Nutrition Assistance Program (SNAP; formerly Food Stamps), an income-eligible entitlement programme used by one in seven US residents. Recent scholarship on the monthly SNAP benefit distribution schedule has found that longer duration from SNAP distribution is associated with poorer diet quality, energy restriction and higher likelihood of skipping meals(Reference Kharmats, Jones-Smith and Cheah2–Reference Sanjeevi and Freeland-Graves7), all of which can have detrimental impacts on diet-related chronic diseases. Additionally, poverty and food insecurity pose significant barriers to proper self-management of chronic disease(Reference Silverman, Krieger and Kiefer8). Chronic disease self-management has been shown to reduce symptoms from chronic conditions, such as pain and fatigue, and reduce emergency room and outpatient medical visits among chronically ill populations. Effective self-management includes a medically recommended diet, appropriate exercise and use of medications, communication with family and medical providers, and awareness of treatment options(Reference Lorig, Ritter and Stewart9, Reference Ory, Smith and Ahn10).
The associations between income, food insecurity and chronic disease morbidity and mortality have been well documented. In the USA, overall chronic disease rates are higher among households with annual income below $US 35 000(Reference Blackwell, Lucas and Clarke11). Compared with an adult with no chronic conditions, an individual’s odds of food insecurity increases along with the number of chronic conditions he/she has(Reference Tarasuk, Mitchell and McLaren12). Food insecurity has been associated with poorer self-rated health and higher risk of hypertension, hyperlipidaemia, osteoporosis, diabetes mellitus, CVD and obesity(Reference Alley, Soldo and Pagán13–Reference Ford19). Studies have shown food insecurity is adversely associated with health behaviours, including poorer LDL-cholesterol control(Reference Berkowitz, Baggett and Wexler20), increased odds of HIV risk behaviours(Reference Wang, Zhu and Evans21–Reference Tsai, Hung and Weiser23), poorer adherence to antiretroviral therapy and self-care among people with HIV(Reference Whittle, Palar and Seligman24–Reference Weiser, Yuan and Guzman26), and cost-related medication underuse among those who are chronically ill, especially among individuals who are Hispanic, Black or suffer from multiple chronic conditions(Reference Berkowitz, Seligman and Choudhry27). Among SNAP recipients, CVD mortality rates are higher for non-Hispanic White and non-Hispanic Black individuals compared with both income-eligible and higher-income non-SNAP participants(Reference Conrad, Rehm and Wilde28). It has also been found that SNAP participants across all races/ethnicities have higher diabetes mortality compared with non-participants(Reference Conrad, Rehm and Wilde28).
Diet-related chronic disease self-management and outcomes among SNAP participants are critically understudied, particularly in light of the lower overall diet quality found among the SNAP population compared with non-participants(Reference Andreyeva, Tripp and Schwartz29). Most of the existing SNAP cycle research has used large administrative data sets to quantify the effects of the monthly benefit cycle. The present mixed-methods study adds to the literature by using both survey data and in-depth qualitative inquiry to allow SNAP recipients to express in their own voice the particular challenges of chronic disease management within the context of SNAP benefit receipt and the volatility of the monthly SNAP benefit cycle. The qualitative approach in our study enables a richer, exploratory investigation of the experience of the SNAP cycle and provides the possibility of a wider range of participant responses than do closed-ended quantitative methodologies.
Methods
The current paper presents data from a prospective, mixed-methods study following two sequential cohorts of adult SNAP recipients (n 18) in Philadelphia, PA, USA, between 2016 and 2017. We recruited participants through word-of-mouth, with the assistance of several non-profit agencies in the Philadelphia area, and in-person at Children’s Hospital of Philadelphia outpatient clinics. The first cohort was assembled for a clinical study; the second cohort was intended to augment the first.
Eligibility for the study required that participants were the primary food shopper for their household, at least 18 years of age and currently receiving SNAP benefits. For the first cohort, study participants (n 12) were food insecure, overweight or obese (BMI = 25·0–39·9 kg/m2) African-American mothers of young children. For the second cohort, we used purposive sampling to diversify the sample (n 6) to be more reflective of the SNAP population in Philadelphia. This sample included adults without children, seniors and people with disabilities, as well as participants of other racial and ethnic backgrounds. Across both phases of the study, we screened ninety-one people, of whom eighteen were eligible and consented to participate in the study.
Participation in both study cohorts lasted for one month and included a screening assessment at recruitment, followed by three study visits: one each at the beginning, middle and end of the SNAP month. Screening included an eligibility questionnaire and the US Household Food Security Module(30). Study visits took place both in a clinical setting (cohort 1) and at locations selected by the participants where they either prepared or acquired food (cohort 2). Visit locations for cohort 2 included participant homes, grocery stores, food pantries and soup kitchens. Visits included surveys collected using REDCap, a secure online survey and data management tool(Reference Harris, Taylor and Thielke31), and semi-structured interviews that were audio-recorded and transcribed verbatim. The surveys covered six main topics: (i) income and expenses; (ii) management of household finances; (iii) food shopping behaviours and attitudes; (iv) SNAP use patterns; (v) opinions about SNAP; and (vi) self-reported health. Interviews were largely open-ended and participant-guided with the interviewer using questions loosely adapted from the SNAP Food Security In-Depth Interview Study to prompt participants as needed(32). The range of interview topics was determined by the research team after review of the literature and the open-ended interview guide was piloted prior to data collection. Topics covered included: (i) experience of the SNAP cycle; (ii) coping strategies for managing SNAP and food insecurity; (iii) food shopping and meal patterns; (iv) use of the charitable food sector; (v) financial volatility; (vi) social networks; and (vii) personal health experiences, among others. The interviews were typically 30–90 min in length.
Analysis of interview transcripts and surveys
Survey data were analysed using the statistical software package Stata version 14.2. For the semi-structured interviews, two members of the research team performed a line-by-line reading of a subset of transcripts to identify recurrent concepts. The transcripts were coded by both researchers using NVivo version 11 qualitative data analysis software, with 93·3 % agreement. Consistent with the COREQ (Consolidated Criteria for Reporting Qualitative Research) guidelines for qualitative research, the researchers summarized the findings by code and these summaries were used to guide group discussion and iterative interpretation of the data by the study team to identify cross-cutting themes that integrated findings across codes and across the two study cohorts(Reference Giacomini and Cook33–Reference Pope, Ziebland, Mays, Pope and Mays36).
The study was approved by the University of Pennsylvania and Children’s Hospital of Philadelphia Institutional Review Boards.
Results
Table 1 describes the characteristics of the eighteen participants across both cohorts. The mean age was 37 years and the majority (89 %) of participants were female. Among the sample, 56 % reported very low household food security, meaning that at times during the past year, one or more household members cut or skipped meals and food consumption declined because they lacked the resources with which to procure food. Nearly two-thirds of participants (61 %) reported having or caring for a household member with a diet-related chronic disease. When including overweight/obesity as a chronic condition, this was 100 %.
Table 1 Sample characteristics of both study cohorts: adult primary food shoppers from households receiving Supplemental Nutrition Assistance Program benefits (n 18), Philadelphia, PA, USA, 2016–2017

* This includes individuals who do not work, are currently searching for work, unable to work because of a disability and unable to work because of a felony conviction.
† Self-reported monthly income from wages, tips, unemployment payments, disability payments, social security, retirement payments, cash welfare, child support (court mandated and informal), Subsidized Child Care Program, loans, gifts and prizes.
‡ Self-reported monthly expenses from rent/mortgage, homeowner’s/renter’s insurance, electricity, heating fuels, transportation (car payments, gas, parking tickets, public transit), telephone, cable, Internet, child care, adult care, health insurance, medical co-pays, uninsured medical bills and student loans.
While participants were not recruited based on their experiences managing chronic diseases, all of them either had a chronic disease or were managing one within their family. The reported chronic conditions included ones either explicitly diet-related or those with serious dietary implications: diabetes (types 1 and 2), Crohn’s disease, CVD, phenylketonuria (PKU), HIV, Alagille syndrome (a rare genetic disorder), hypertension, overweight/obesity (all participants in cohort 1 and 50 % of cohort 2), lactose intolerance, severe food allergies, hypothyroidism, high cholesterol and pancreatitis (Table 2). Stemming from these chronic illnesses, participants reported during the interviews a wide range of physical and emotional side-effects and co-morbidities such as pain, neuropathy, blindness, fatigue, depression and anxiety, hair loss, rapid weight loss, brain damage, liver and kidney problems, anaphylaxis, insomnia, skin rashes, fear and loneliness.
Table 2 Diet-related chronic diseases, management and consequences within the pooled study sample of adult primary food shoppers from households receiving Supplemental Nutrition Assistance Program benefits (n 18), Philadelphia, PA, USA, 2016–2017
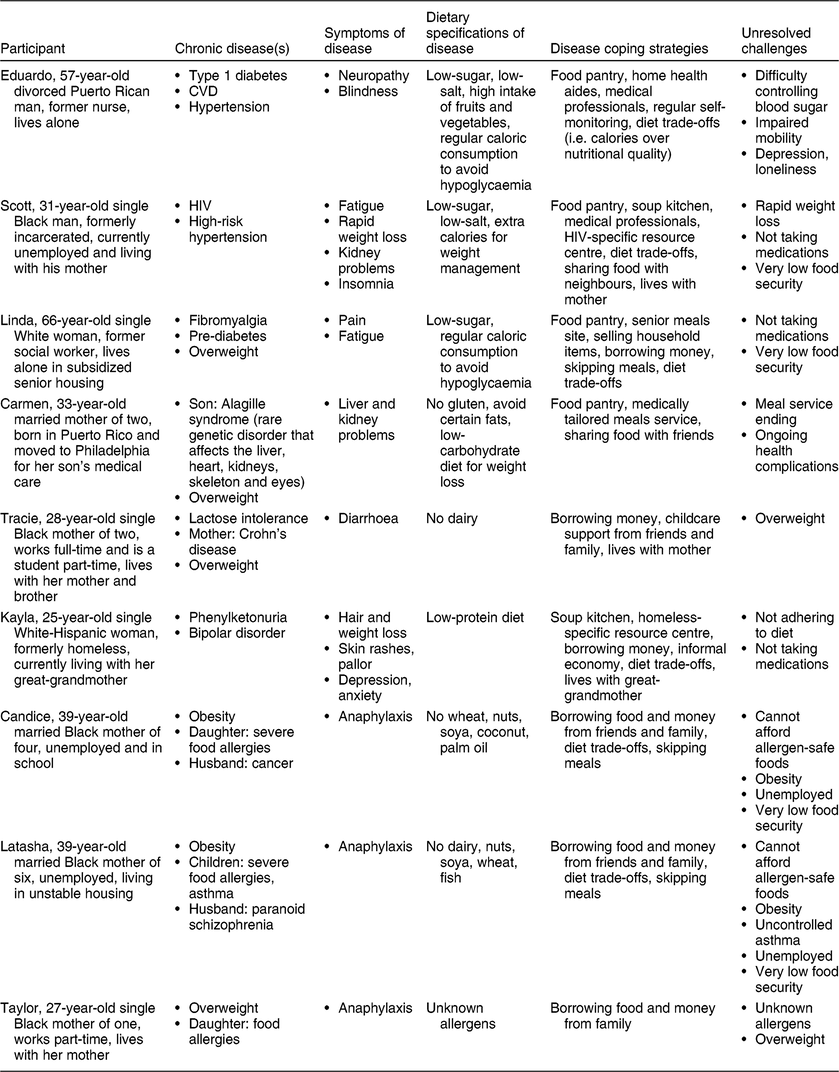
Diet management during the SNAP cycle
An essential component of self-managing chronic diseases described by participants was a near-constant vigilance and monitoring. With respect to diet, this often took the form of regular consumption or avoidance of certain foods (e.g. sugar, salt, nuts, dairy, fruits and vegetables), as well as monitoring of nutrient intake (e.g. counting carbohydrates) and tracking health indicators (e.g. checking blood sugar levels). For participants with types 1 and 2 diabetes, sugar-free and low-carbohydrate food products were important staple items in their diet. As EduardoFootnote *, who has type 1 diabetes, explained:
‘I’ve just gotta be aware of my carbs, like … I gotta figure out how many carbs is in there. Like if I get – a half a banana would be, I think, maybe 50 carbs. I don’t know. But there are some bananas that are sweeter than others.’
Latasha and Candice, both of whose children have wheat allergies, discussed searching for and purchasing gluten-free items. Based on inclusion criteria for the first study cohort, the majority of participants were overweight or obese and several were following specific diets to lose weight. For Kayla, who has PKU, a low-protein diet is critical for proper management of her illness. The range of dietary requirements represented across our study sample (Table 2) illustrates the heterogeneity of food needs between SNAP households.
Often specialized diets necessitated the purchase and preparation of different foods within households. During a home visit, Carmen opened her refrigerator to display the three kinds of milk she purchased to accommodate her family’s different dietary needs: coconut milk for herself (as part of a weight-loss programme), almond milk for her children (for lactose intolerance) and regular milk for her husband. Carmen was also was on a highly restrictive low-carbohydrate diet for weight loss that required preparation of separate meals from those she made for the rest of her family. Latasha, who has six children, several of whom have different food allergies, struggles to keep up with the varied food items that are safe for each child.
The end-of-month period was highlighted by participants as being particularly difficult financially, which often had repercussions on diet and chronic disease management. The average SNAP benefit allotment per household within the sample was $US 241 and despite techniques for budgeting SNAP resources, all participants reported that their SNAP ran out before benefits were renewed – typically between the second and third week of the cycle. Several participants noted skipping meals in the final weeks of the SNAP cycle, which sometimes resulted in low blood sugar. For Eduardo’s diabetes management, the necessity of eating to avoid hypoglycaemic incidents was paramount, which included trying to keep snacks and juice on hand at all times. To do this, he relied on monthly trips to the food pantry. For Linda, who was pre-diabetic, keeping food in the house at all times was challenging, as her SNAP benefit was only $US 16 per month, which meant that by the end of the month when she had no money left she resorted to creative strategies for obtaining food such as getting a slice of pizza on credit or having a yard sale with items from her apartment.
For a number of participants, the end-of-month period was also accompanied by less healthy eating patterns. Eduardo explained that a can of soup was his go-to meal when SNAP would run out:
‘Chicken noodle. Yeah. Just 99 cents at ShopRite. The little can, Campbell? Yeah. Can of soup and bread. And you know like survive … But then on the other hand my health is not surviving.’
Reliance on low-cost, high-sodium foods like canned soup at the end of the benefit month allowed Eduardo to feed himself, but was bad for his hypertension and deregulated his blood sugar levels.
Key themes
In addition to the overarching study topic of diet and chronic disease self-management during the SNAP cycle, participant interviews revealed four key themes: (i) cost of medically appropriate diets; (ii) interplay between health and financial instability; (iii) relationships with formal support systems; and (iv) constraints of depending on the charitable food sector.
Cost of medically appropriate diets
Despite high awareness of their dietary needs for disease management, participants recounted difficulty staying ‘on-diet’ because of limited financial resources. For example, Scott was suffering from rapid weight loss associated with HIV and had been advised by his nutritionist to eat more calories, which he feared was not affordable given his limited SNAP benefit and inconsistent cash income. He said:
‘They want me to go on 3600 calories a day. That’s a lot. And that’s expensive, so I don’t know how that can happen. …They did not tell me how to pay for it, but they gave me a printout of what to buy. I’m like, who’s gonna pay for that? That’s not gonna happen.’
Scott felt that doctors and nutritionists he visited did not understand the realities of poverty or of depending on SNAP benefits to buy food and therefore did not make feasible suggestions for diet management.
Participants often talked about the extra expense of foods for specialized diets (e.g. almond milk, gluten-free products), compared with their regular alternatives. For some participants, spending more of their budget on food caused significant financial strain. Candice and Latasha, both of whom have children with severe food allergies, lamented the challenge of finding safe foods that were not too cost-prohibitive. In addition to reporting that they could not afford special foods for medical conditions, many participants expressed a feeling of being unable to buy ‘healthy’ foods like fruits and vegetables on a SNAP budget because those items cost more than less healthy, often highly processed options.
Another participant, Kayla, expressed frustration that she was not able to use her SNAP benefits to purchase the low-protein foods recommended for the management of her PKU because they are available only through online websites where SNAP cannot be used. As a result, she explained, she eats whatever foods she can, even if that means going off-diet, because she cannot afford to buy the medically tailored foods with cash:
‘There’s websites that I can order food from, special low-protein foods. It’s just for people with my diet. But I can’t afford it.’
For Kayla, dependence on SNAP and the long-term consumption of foods that are non-adherent to medical recommendations for her PKU have resulted in pallor, underweight and hair loss, and could result in brain damage in the long run.
Interplay between health and financial instability
Living with a chronic disease was marked by a high degree of instability and unpredictability. Unexpected health complications were frequent, oftentimes imposing unanticipated expenses such as medical bills (e.g. uninsured ambulance rides) or special post-surgery foods. The unpredictable nature of chronic illness also made it difficult for participants to plan, travel or keep regular work. Linda, an older woman suffering from fibromyalgia, recounted frequently cancelling or rescheduling appointments because of flare-ups in her pain or fatigue:
‘My fibromyalgia is really bad in the winter and my arthritis is really bad in the winter. I have about 50 % less energy. So it’s this unpredictability which is why I couldn’t get up at seven o’clock in the morning and have to be at work at nine. I could never do it.’
The unpredictability of Linda’s illness exacerbated her financial instability, as it made keeping regular commitments, such as a job, nearly impossible.
Participants often framed their experiences around life before and after the illness. Living with a chronic disease was frequently marked by a transition period and required adjustment to new routines. For some, this meant moving to a new city to access better medical care or social service resources. Participants suffering from physical impairment as a result of their chronic disease (e.g. blindness, difficulty walking) expressed missing the physical independence they used to have. These transitions, and sometimes drastic changes in lifestyle, caused many participants to feel lonely, frustrated and depressed.
Like Linda, four other participants had lost their jobs (27·8 %), either because their illness made working too challenging or because managing their child’s illness caused them to miss too many days of work. As Carmen explained, she was forced to leave her job at a pharmacy after using all her vacation and sick days taking her child to the doctor. For Carmen, not only did managing her son’s chronic disease cause her to lose her job, but she was also forced to file for bankruptcy to manage the medical bills. Several mothers in the study had children with severe asthma which, while not a diet-related chronic illness, posed significant financial challenges that impacted household food security. For example, Latasha was forced to resign from her nursing job after missing too many shifts due to her son’s asthma resulting in emergency room visits. After losing her job, she fell behind on bills and the family was eventually evicted from their home. The time burden of managing chronic illness created financial instability in the lives of many participants, which only compounded the end-of-month deficits they experienced as part of the SNAP cycle.
Lastly, a number of participants, including Latasha, remarked on the psychological challenge of no longer being able to work; they missed the financial independence of having a full-time job, as well as the routine, social interactions and mental stimulation:
‘So I wanna go back to work. I wanna live a normal life again. It felt really, really good doing it, getting up in the morning, going to go get hot tea and a bagel and going to work. That was – people need that.’
Relationships with formal support systems
To aid in chronic disease management and fill in the gaps throughout the SNAP benefit month, participants utilized a variety of local community organizations, resource centres and health-care experts. All participants consulted regularly with some form of medical or social service provider. Several participants had established strong relationships with more comprehensive community resource centres targeted at specific vulnerable populations. For example, Scott received a range of services from a local non-profit dedicated to serving the HIV-positive community, including medical care, food assistance, legal aid, post-incarceration resources and job training. For Kayla, who had formerly been homeless and frequently had unstable housing arrangements, a homeless resource centre was instrumental in her survival, providing not just meals, but clothing, body care supplies, health screenings and even a steady address at which she could receive her mail, which she needed to maintain her SNAP benefits. As she explained:
‘This is my favourite place … I’m not on the streets now, but I still come here … They got personal care. They got [subway fares] for people who need it … The lady who doesn’t work here no more, she helped me apply to [community college]. They help you.’
Organizations such as these provided much needed instrumental support for the participants in our study.
A critical way that local social welfare resource providers supported participants was through individualized care. When Eduardo was struggling financially, his social worker came by his house with several bags of food and put his name on a waitlist for a health-focused food pantry. Linda, who lives alone and survives off her social security benefits, described how several times in the prior months she had run out of money before her benefits were renewed and had called the food pantry to reschedule her monthly visit so that she could go in for food a week earlier. Carmen, whose son is chronically ill, recounted how an employee at the medically tailored meals delivery programme she used pulled some strings to extend the service beyond the typical three-month period. Participants emphasized how critical the personalized attention they received was in helping them maintain a positive mental outlook, ‘get back on their feet’ and manage their chronic disease.
Constraints of depending on the charitable food sector
In addition to receiving SNAP, more than half our participants frequented community food assistance facilities such as food pantries or congregate meal sites (e.g. soup kitchens, churches, senior centres). The usage patterns of community food assistance varied, with some participants incorporating these resources into their regular weekly or monthly food acquisition strategies, while others relied on these programmes particularly at the end of the month when SNAP had run out. Participants who used community food assistance felt these resources were critical in ensuring that they were able to eat in the final days and weeks of the benefit cycle. As one participant stated:
‘[B]y the second week, almost close to the third, I run out. So then I have no choice but to come here or starve.’
Others described using food assistance resources regularly throughout the month, not just at the end, to stretch their SNAP benefits. Kayla, who had formerly been homeless, ate nearly daily – sometimes multiple meals per day – at local churches and homeless resource centres. She displayed an intimate knowledge of the free meal network in the city:
‘We tend to go to all the places that they feed during the day, throughout the day. We know where to go on a Monday, where to go on a Tuesday. We know all the days of the week where to go.’
For many of the households who used community food assistance resources, these places were not just last resorts during an emergency, but rather had become regular components of their food procurement strategies.
While community food assistance facilities were vital resources in managing food insecurity throughout the benefit month, participants felt they did not always offer nutritionally adequate items, with serious implications for chronic disease management. During one of our visits together at a resource centre for the HIV-positive community, Scott complained that the food pantries he visited largely offered canned or processed foods which were high in sodium and did not meet the standards recommended to him by a nutritionist for management of his hypertension. Scott also recounted being offered cake for breakfast at a local soup kitchen, as well as fast-food vouchers and Hungry-Man® meals. Several participants felt that they had no choice but to eat the foods they were offered. As Kayla described of the meals she received at free meal sites:
‘I have a genetic disorder called PKU, so I’m not supposed to eat meat. [If I eat it] my phenylalanine goes up, my levels, my blood. Little symptoms, little things start happening. Then long-term is brain damage … I’m going to eat it anyway, because I’m hungry. It’s really all that I have.’
By virtue of depending on these community resources as regular and vital sources of their monthly food supply, participants often lacked control over the foods they were eating.
Despite noted inadequacies, charitable food assistance sites often played an integral role in the chronic disease management of participants. Several participants regularly visited one food pantry in North Philadelphia that followed nutritional guidelines for the foods it offered (often called a ‘Green Light Pantry’), including an emphasis on fresh fruits and vegetables, whole grains and low-sodium items. Carmen, who visited this pantry each month, was grateful that the food offerings aligned with the dietary requirements for her son’s chronic illness. When grocery shopping, Carmen often selected the same brands or products at the store, demonstrating her approval of the foods offered at the food pantry.
Discussion
To our knowledge, the present study is the first to explore self-management of diet-related chronic disease within the context of SNAP benefit receipt and the monthly SNAP cycle. Drawing from nearly 50 h of in-depth qualitative interviews with SNAP participants, the study highlights the dual cognitive burden of poverty and chronic disease and elucidates the particular challenges of food procurement and maintenance of diet quality throughout the benefit month faced by SNAP households with diet-related chronic diseases. The emergent themes from this research point to the two key issues discussed below: (i) affording the dietary needs of chronic disease with SNAP; and (ii) the importance and limitations of formalized care in managing chronic disease within low-income populations. Table 3 also provides policy recommendations by emergent theme, which will be further discussed below.
Table 3 Themes, sample quotes and policy recommendations from in-depth qualitative interviews with adult primary food shoppers from households receiving Supplemental Nutrition Assistance Program (SNAP) benefits (n 18), Philadelphia, PA, USA, 2016–2017
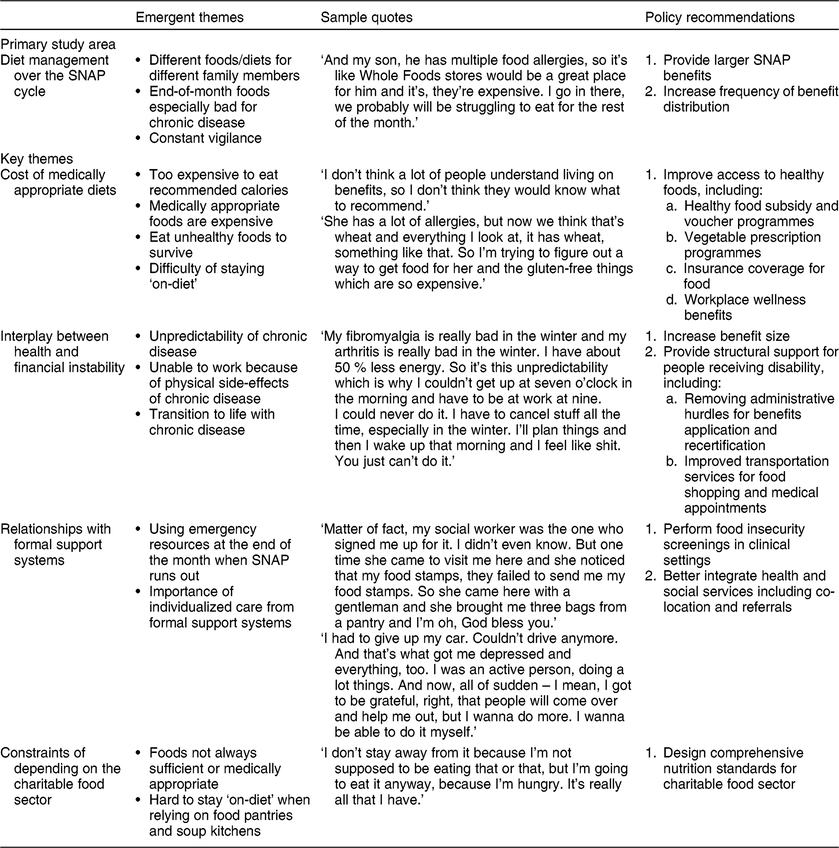
Affording chronic disease dietary needs with SNAP
A key finding from the present study is the inadequacy of SNAP benefits, either in lasting for the full monthly benefit cycle or for routinely purchasing healthy foods. While consistent with prior SNAP literature(Reference Wilde and Ranney3, Reference Shapiro4, Reference Whiteman, Chrisinger and Hillier6, Reference Andreyeva, Tripp and Schwartz29, Reference Hastings and Washington37), our study highlights the particular challenges faced by households managing diet-related chronic diseases as a result of the insufficiency of SNAP benefits. In our interviews, participants highlighted multiple ways in which relying on SNAP constrained or challenged their ability to purchase foods that supported healthy disease management, including not being able to afford more expensive, specialized diet foods (e.g. gluten-free alternatives) and struggling to purchase adequate calories for weight or blood sugar maintenance. Running out of SNAP at the end of the month also impacted self-management of chronic disease, as the emphasis in those final weeks of the benefit month was frequently on sufficient consumption, rather than the healthfulness of foods consumed, which highlights the degree to which participants were surviving, and not thriving, in times of financial shortfall. This finding within our participants aligns with a recent study by Seligman and colleagues demonstrating that low-income patients admitted to hospital for hypoglycaemia increased by more than 25 % by the end of the month compared with the beginning of the month, while no such pattern existed within higher-income patients(Reference Seligman, Bolger and Guzman38).
For households who are managing diet-related chronic conditions, the regular consumption of healthy diets high in fruits, vegetables and whole grains and low in added sugar, salt and fat is essential for positive disease outcomes. However, extensive prior literature around the differential cost of healthy and unhealthy foods supports the challenges of affordability our participants expressed. Energy-dense foods, such as those including refined grains, added sugars and fats, have been found to be less expensive than recommended, nutrient-dense foods including fresh fruits, vegetables and lean meats(Reference Drewnowski39–Reference Rao, Afshin and Singh42). Furthermore, while several studies have shown that some nutrient-dense foods are available at lower price points, these items are not always socially acceptable or palatable to low-income shoppers(Reference Darmon and Drewnowski43, Reference Maillot, Darmon and Drewnowski44). In addition, studies have found that foods for specialized medical diets, such as gluten-free foods, are both less available and more expensive than their conventional alternatives(Reference Lee, Ng and Zivin45, Reference Singh and Whelan46). Along with the findings from our participants, these studies emphasize how SNAP households managing chronic illnesses are hard pressed to adhere to recommended dietary guidelines throughout the month and particularly in the final days of the benefit cycle. This challenge is heightened by the higher costs of healthy foods and specialty diet food items.
Given the disparities by income and race in chronic disease prevalence within the USA, as well as the higher mortality rates among SNAP participants for CVD and diabetes, critical attention to disease-specific diet quality within this population is essential. Recent literature has highlighted how important food is for health – a concept sometimes referred to as ‘food is medicine’ – including a recent study demonstrating that SNAP enrolment was associated with lower estimated annual health-care expenditures(Reference Berkowitz, Seligman and Rigdon47). Several recent food provision interventions among populations with HIV and/or diabetes have found significant improvements in medication adherence, glycaemic control, fruit and vegetable intake and self-efficacy(Reference Palar, Napoles and Hufstedler48, Reference Seligman, Lyles and Marshall49). Additionally, studies evaluating healthy food subsidies or incentives within the SNAP population have shown significant increases in vegetable and fruit consumption(Reference Bartlett, Klerman and Olsho50, Reference Harnack, Oakes and Elbel51). Targeting improvements in chronic disease outcomes, a recent study using stochastic modelling showed that expanding a SNAP vegetable and fruit subsidy nationwide would be expected to reduce type 2 diabetes incidence by 1·7 % and myocardial infarction by 1·4 %(Reference Choi, Seligman and Basu52). This model also predicted significant societal cost savings from long-term reductions in diabetes and CVD. This research suggests that subsidizing or incentivizing the purchase of certain disease-specific healthy foods (e.g. fruits, vegetables, low-sodium foods) may improve the chronic disease self-management and outcomes of SNAP participants.
Other policy recommendations to address the high cost of medically appropriate diets and end-of-month insufficiency, detailed in Table 3, include increasing the size of benefits and distributing SNAP benefits more frequently during the month. While increasing benefit size is a politically challenging proposition, evidence suggests that increasing benefit size could significantly reduce emergency department medical claims and Medicaid expenditures(Reference Ojinnaka and Heflin53, Reference Sonik54), meaning this investment in food security could potentially both improve population health and reduce government medical spending.
Formal assistance, individualized care and scalability
As a coping strategy to fill in the gaps after benefits had run out, SNAP participants in our study turned to a constellation of other largely community-based resources, many of which, while instrumental in their food, financial and disease management assistance, had limitations of their own. The charitable resources on which participants relied (e.g. food pantries, soup kitchens) often could not provide adequate or appropriate foods for effective disease management. The low nutritional quality and insufficient supply of the foods described by our participants at many food assistance programmes aligns with findings from previous studies(Reference Poppendieck55–Reference Akobundu, Cohen and Laus59). These perceived inadequacies resulted in many participants feeling that they could not rely on these resources to alleviate food insecurity or supply the necessary foods for their chronic disease management. Despite these noted limitations, it is remarkable that some food pantries have found innovative ways to address the myriad health needs of their clients, including offering products tailored to certain chronic diseases, using nutritional guidelines for stocking requirements, and providing health screenings and counselling(Reference Seligman, Lyles and Marshall49, Reference Martin, Wu and Wolff60, 61).
That said, those households who did rely regularly on formal community assistance programmes generally expressed gratitude for the services they provided, even if the foods received were not always aligned with their particular needs. Most notably, the flexibility and individualized care of community-based resources were highly valued by participants, particularly in contrast to the rigidity of federal welfare programmes. The individualized care that participants described as instrumental in their survival – home health aides tracking SNAP benefits, social workers putting their name on the waitlist for a food pantry – reduced some of the ongoing stress and juggling of multiple priorities participants experienced. Ultimately, this care may have positive impacts on the SNAP cycle and chronic disease self-management.
These accounts of individualized care, however, point to a broader problem within our social safety net. The experiences of our study participants highlight the degree to which SNAP households with chronic diseases need help navigating not only food resource systems, but also health-care and social service systems. The US social service programmes – Medicaid, SNAP, Social Security Disability – are incredibly challenging to navigate(Reference Magasi62, Reference Aizer63) and, in the case of the SNAP households in the present study, often required assistance from highly individualized formal support systems. This type of targeted and high-touch care has become necessary for the survival and well-being of many low-income Americans, particularly as income volatility has increased(Reference Hacker and Jacobs64, Reference Ziliak, Hardy and Bollinger65) and the social safety net has been dismantled through funding cuts, punitive work requirements and political ill-will towards the poor(Reference Tach and Edin66). Not everyone has access to these highly individualized resources, however, and this model of care is not scalable or sustainable within our current political context. One strategy that can address these disparities in access to care, recommended by numerous American medical associations, is for medical professionals to screen for food insecurity in the clinical setting and work with patients and social workers to adjust the medical plan with food access in mind(Reference Smith, Malinak and Chang67–69). Another strategy to provide structural support for individuals with disabilities to reduce the burden of navigating the benefit system, could include reducing administrative hurdles for benefits application and recertification(Reference Mullainathan and Shafir70).
Study limitations
The convenience sample located entirely within Philadelphia, which is a high-poverty urban area, is not generalizable for the national SNAP population, which includes large numbers of rural recipients(Reference Lauffer71). Given the interview format of data collection and the sensitive nature of the topic matter, participants’ responses may have been influenced by social desirability bias. Additionally, responses about chronic disease incidence and self-management were self-reported. Future research with a larger and more representative SNAP population is needed to better understand the challenges and implications of chronic disease self-management among SNAP recipients.
Conclusion
The prevalence and severity of challenges managing diet-related chronic diseases among SNAP participants demonstrated by our study draw attention to a critically understudied topic within the SNAP literature. Recent studies demonstrating the effectiveness of subsidizing certain foods on both healthy food consumption and chronic disease management suggest that evaluations of further interventions are warranted.
Acknowledgements
Acknowledgements: The authors wish to thank the participants for sharing their time and experiences. The authors would also like to acknowledge the following people for their contribution to this study: Taylor White-Welchon, Elizabeth Stulpin, Dr Virginia Stallings, Dr Terri Lipman and Dr Lisa Servon. Financial support: This work was supported by the University of Pennsylvania Leonard Davis Institute of Health Economics (M.O.); the University of Pennsylvania Graduate and Professional Student Assembly Provost Award for Interdisciplinary Innovation (M.O., E.W.K.); the National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases Pediatric Endocrine Fellowship Training in Diabetes Research (M.O.); and the Investment for the Future Initiative in Community Practices, University of Pennsylvania School of Nursing (C.C.C.). The sources of financial support had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: E.W.K., M.O., C.C.C. and A.H. formulated the research questions and designed the study. E.W.K. collected and analysed the data and wrote the manuscript. M.O. collected data. R.D. analysed data. All authors edited and approved the manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the University of Pennsylvania and Children’s Hospital of Philadelphia Institutional Review Boards. Written informed consent was obtained from all subjects.
Author ORCIDs
Eliza Whiteman Kinsey, 0000-0003-4972-431X. Roxanne Dupuis, 0000-0003-3161-6310.





