INTRODUCTION
Escherichia coli O157 is the most commonly isolated enterohaemorrhagic E. coli (EHEC) serotype in the UK, USA, Canada and Japan, with cattle and sheep considered to be its main reservoirs [Reference Strachan, Macrae and Ogden1, Reference Topping2]. Symptoms include abdominal pain followed by bloody diarrhoea progressing to haemolytic uraemic syndrome (HUS) in 2–15% of reported cases, most often in children aged <10 years [Reference Tarr, Gordon and Chandler3]. In Scotland, which has the highest reported incidence of E. coli O157 infection/100 000 population worldwide [Reference Locking and Cowden4], E. coli O157 infections are now more likely to be environment related than food-borne, with a higher incidence in rural areas relative to urban areas [Reference Strachan5].
Direct contact with farm animal faeces [Reference Locking6–Reference Pritchard8] and contaminated public and private drinking water supplies [Reference Licence9, Reference Hrudey10] are implicated as environmental infection routes in past cases in rural areas. Indeed, there have been repeated calls by researchers over the last 12 years for a better understanding of, and response to, the increasing risk to rural residents and visitors posed by E. coli O157 [Reference Coia11–Reference Solecki13]. The expectation of health protection professionals is that the public adopt suitable protective behaviours, i.e. ‘simple precautions’ [Reference Locking and Low14], to reduce personal risk and outbreak. However, popular understandings of E. coli O157 and particularly how farmers and visitors to rural areas view the environmental risk of infection is not known.
This paper reports exploratory research undertaken to assess implications of E. coli O157 for residents and visitors in two rural areas with contrasting incidences of infection. Specific objectives were to determine:
• levels of awareness of E. coli O157;
• views on the illness: including severity, symptoms and sources of infection;
• protective behaviours undertaken.
We had no expectations of popular understandings other than an apprehension that people may not have heard of E. coli O157 if it was not a part of their occupation or professional role. We therefore included food workers in the study as an occupational group who have training in microbiological safety and could be anticipated to have a discernible awareness of E. coli O157. Prompted by the outbreak at Godstone Farm in the UK in August 2009 [15], when 65 visitors to the farm attraction were infected with E. coli O157, the focus of this paper is the awareness and understanding of visitors to livestock farming areas compared to that of residents.
METHODS
Study population
Research focused on four groups of people in two rural study areas: farmers, non-farming residents, visitors, and food workers (butchers and abattoir workers) in Grampian (comprising the counties of Aberdeenshire and Moray in northeast Scotland; population 519 979), and North Wales (comprising Anglesey, Conwy, Denbighshire and Gwynedd; population 630 152). In Grampian there has been an average of 10·8 cases of E. coli O157 disease reported per 100 000 of the population per year for the last 12 years compared with 2·5 cases/100 000 per year in North Wales [Reference Rotariu16].
Study design
The research utilized a paper-based, self-complete questionnaire and convenience sampling of participants who were recruited by natural opportunities presented to the research team. Questionnaire returns were acquired through: a mailing administered by the National Farmers Union Scotland (NFUS) for Grampian farmers receiving the NFUS newsletter; dissemination at agricultural shows and farmers' meetings, assisted by the National Farmers Union Cymru and the Farmers Union of Wales, for North Wales farmers (both Welsh and English-language versions of the questionnaire were made available); dissemination at popular countryside locations for rural residents and visitors in both study areas; and attendance at meetings of local groups, including community councils and primary schools, for additional responses from non-farming residents in rural Grampian; and abattoir workers and butchers at their places of work. Participants were drawn widely from across the two study areas between April 2008 and January 2009 with their fully informed consent. The study was approved by the University of Aberdeen School of Geosciences ethics committee.
The questionnaire comprised closed ‘yes/no’, choice and Likert-type scale response questions and an open question to gather descriptions of intentional action to avoid E. coli O157 infection. An initial routing question asking participants if they had heard specifically of ‘E. coli O157’, rather than ‘E. coli’ or ‘stomach bugs’, allowed respondents knowing the term ‘E. coli O157’ to be extracted from a set of respondents who had not heard of ‘E. coli O157’ and who gave views on ‘E. coli’ or ‘stomach bugs’.
Presented in this paper are analyses of responses to:
• the routing question on awareness of E. coli O157: ‘Had you heard of E. coli O157 before you read this questionnaire?’
Three questions, assessing understanding:
• How seriously ill do you think you would be if you were infected with E. coli O157?
• Which of the following do you think are symptoms of an E. coli O157 infection?
• How likely are people in general to get E. coli O157 from the following where you live?
and an open question on protective behaviour:
• Do you intentionally do things to reduce your risk of getting E. coli O157? If ‘yes’, please describe what you do.
There was no previously reported research on differences between people's awareness of E. coli O157 with which to determine the size of sample required to detect differences and therefore we collected as many responses from each the four groups (farmers, visitors, non-farming rural residents, food workers) as time and resources allowed (Table 1 b).
Table 1. Awareness of E. coli O157 by respondent groups: comparison of (a) the groupings formed for comparing visitors' and residents' understandings of E. coli O157 symptoms and sources of infection with (b) the initial groups used for preliminary analysis of awareness

Data analysis
Numeric data were analysed using PASW Statistics 17 software (IBM SPSS Statistics, USA). Significant relationships (non-independence) across groups of respondents' awareness of E. coli O157, infection and illness captured via categorical data were examined by cross-tabulation and logistic regression and tested using Pearson or Wald χ2. Exploratory analyses of the data using the original four groups in the two areas exposed differences in awareness and particularly between farmers in Grampian and visitors to rural North Wales (Table 1 b). In direct response to the concern about visitors' exposure to E. coli O157 in farm livestock after the outbreak at Godstone Farm we explored further these differences between visitors who were resident outside either of the two rural areas and residents within the areas. We grouped respondents as: farmers living in a rural area in Grampian; farmers living in a rural area in North Wales; residents in rural Grampian who were not farmers; residents in rural North Wales who were not farmers, and visitors to either rural area who were resident outside the area thus using a subset of 1889 respondents (Table 1 a) from the total sample of 2031 (Table 1 b). Analysis of variance and the F test was used for ordinal data on symptoms and sources with a tendency to normality; applying Bonferroni's correction in post-hoc tests.
Analysis of text responses was conducted within NVivo version 8 qualitative data analysis software (QSR International Pty Ltd, Australia) to assist identification of major persistent themes [Reference Thomas17].
RESULTS
Awareness
From a total of 2031 completed questionnaires, 1090 responses (54%) were obtained from individuals who indicated that they had heard explicitly of E. coli O157 (Table 1 b). Specific awareness of the expression ‘E. coli O157’, and not the more general ‘E. coli’, was more common among farmers, food workers and non-farming residents living in rural Grampian. Ninety-one percent of farmers resident in rural Grampian indicated they had heard of E. coli O157 compared with only 28% of visitors coming from homes outside the two rural areas studied (Table 1 a). Demographic and confounding factors influencing differences in awareness between all 2031 respondents were examined using logistic regression (Table 2). ‘Hearing about E. coli O157’ was associated with being a farmer, responding in Grampian, being male, being a carer to children, and increasing age.
Table 2. Logistic regression of factors associated with respondents who had ‘not heard of E. coli O157’

OR, Odds ratio; CI, confidence interval.
B is the coefficient for the factor in the regression and when positive increases the level of not knowing about E. coli O157. The regression yields 72% prediction accuracy.
Odds ratios are given for not hearing about E. coli O157 and are significant where the upper and lower confidence intervals do not include 1. For example the odds are higher for rural visitors and non-farming rural residents not to have heard of E. coli O157 than farmers. The odds for respondents completing the questionnaire in North Wales are higher than those completing the questionnaire in Grampian; the odds that respondents have not heard of E. coli O157 are lower with increasing age and so on.
*** Significant at 1% level, ** significant at 5% level.
Understandings of E. coli O157
Opinions on the severity of illness caused by E. coli O157, common symptoms and sources of infection were analysed from 1013 respondents in the groupings of farmers, visitors, and rural residents who had heard of E. coli O157 (Table 1 a). Despite most (83%) signifying it was a ‘serious’ illness, farmers in Grampian had the highest proportion (24%) indicating they would have only a ‘mild’ illness if infected (Table 3).
Table 3. Comparison between Grampian farmers and all other respondents' views on the seriousness of their illness if infected with E. coli O157
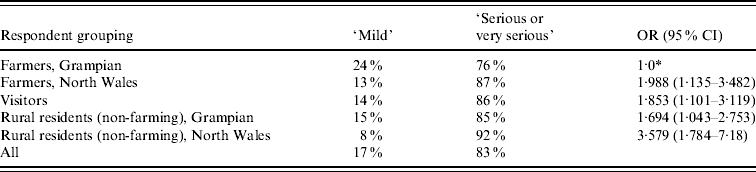
OR, Odds ratio; CI, confidence interval.
Odds ratios presented for respondents considering personal illness if infected as ‘serious or very serious’ compared with the views of Grampian farmers. Thus the odds that non-farming residents in North Wales consider personal illness will be serious or very serious if infected with E. coli O157 is higher than the odds for farmers in Grampian.
* Reference group.
Respondents most frequently selected vomiting as a symptom of E. coli O157 infection from a list of 15 symptoms and not bloody diarrhoea, which was the fourth placed symptom and there was no statistical difference between groups for any of the eight most commonly selected symptoms when examined singly (Fig. 1). However, there was a difference when the combination of symptoms selected by respondents were analysed. A score for this combination, or overall symptom recognition, was significantly different at the 5% level between Grampian farmers who had the highest mean score and visitors who had the lowest score (Table 4). Computation of the score for symptom recognition using all 15 symptoms is described in Table 4.
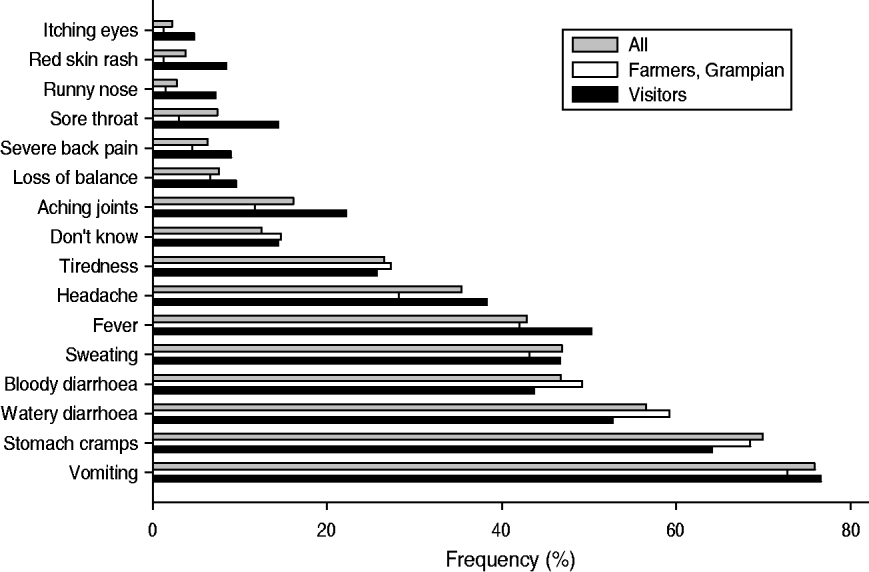
Fig. 1. Respondents' views on the symptoms associated with E. coli O157 infection: comparing the views of all respondents; farmers in Grampian; and visitors to the countryside from outside the study areas.
Table 4. Comparison of farmers, visitors and residents symptom scores discriminating for symptom precision of E. coli O157 infection
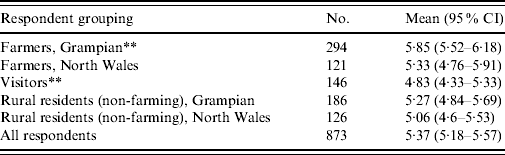
CI, Confidence interval.
A symptom score was computed for each respondent as the sum of scores for each symptom they indicated as symptoms of E. coli O157 infection. Symptoms were scored as follows: stomach cramps, 3; bloody diarrhoea, 3; watery diarrhoea, 3; vomiting, 1; fever, 1; headache, −1; sweating, −1; tiredness, −1; sore throat, −1; aching joints, −1; red skin rash, −1; itching eyes, −1; loss of balance, −1; runny nose, −1; severe back pain, −1. Thus a respondent ticking vomiting, watery diarrhoea, stomach cramps, and headache would have a score of 1+3+3+ (−1)=6. The symptom score can range from −10 to +11. Scores for a symptom reflect perceived knowledge on common clinical features (‘Report of the study of infectious intestinal disease in England, FSA, 2000, p. 9) and are used as a tool for discrimination not an indication of correctness. Symptoms vary between cases.
** Difference in mean score is significant at 5% level.
Participants were asked to rate the likelihood that ‘people in general’ would get E. coli O157 from 12 sources using a five-point scale from 1 (‘very unlikely’) to 5 (‘very likely’): ‘contact with animal faeces’, ‘eating undercooked meat’ and ‘handling farm animals’ all achieved mean scores >3 (‘a slight chance’) while ‘breathing outside air’ and ‘mains tap water’ had mean scores <2 (‘unlikely’) (Fig. 2). Despite this obvious similarity likelihood ratings for all sources except ‘breathing outside air’ differed significantly between groups implying complex variations in the importance of sources between respondents. Pair-wise comparisons across five respondent groups for the 12 sources showed statistically significant differences between groups at the 1% level for 62 of 120 tests and for simplicity a few notable divergences only are mentioned here. Respondents in North Wales were more likely than farmers in Grampian to view undercooked meat as a source of E. coli O157; Grampian residents were more likely than visitors to see handling farm animals as a source; farmers in North Wales were more likely than farmers in Grampian to view toilets and wash hand basins as possible sources.
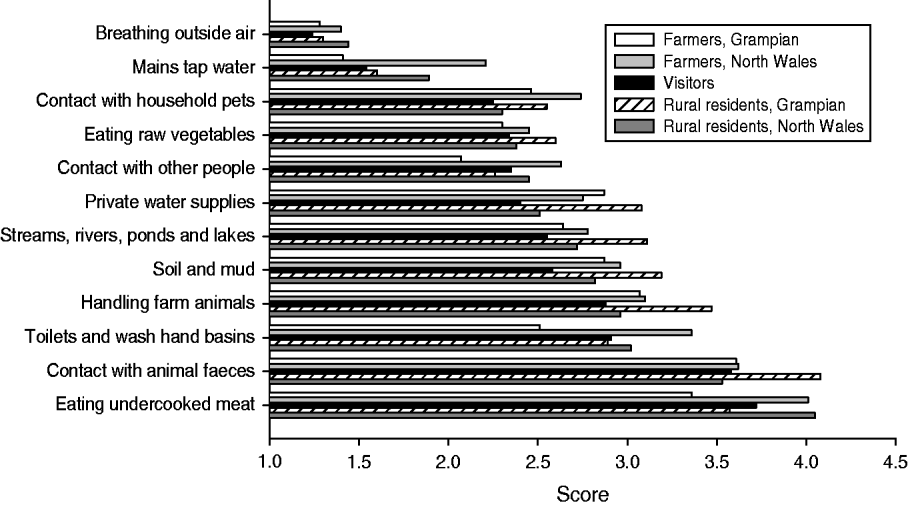
Fig. 2. Comparison of the views of farmers, rural residents (non-farming) and visitors to the countryside on the likelihood of ‘people in general get[ting] E. coli O157’ from different sources; scored as: 1, ‘very unlikely’; 2, ‘unlikely’; 3, ‘a slight chance’; 4, ‘likely’; and 5, ‘very likely’.
Risk reduction behaviour
Five hundred and seventy-three respondents provided written descriptions of ways they intentionally act to reduce their ‘risk of getting E. coli O157’. Their descriptions, which follow in summary and are not shown in tabulated form, covered a wide range of personal strategies and most commonly (~90%) included ‘cleanliness’ with the self the most frequent focus (~65%) of cleanliness, and food the second most frequent (~40%). Cleanliness was often described as ‘basic hygiene’ and ‘common sense’ implying it was performed ordinarily as everyday practice. Hand washing was the single most commonly described protective behaviour.
Respondents described reducing risk when cooking food (e.g. ‘cooking thoroughly’), particularly when handling raw meat. Many (n=109) mentioned food storage and preparation practices to avoid cross-contamination between uncooked meat and cooked meat or other foods eaten raw. Beef, minced beef or burgers were mentioned in 86 descriptions. Salads, fruit and vegetables were also mentioned but less frequently as foods to be prepared with particular caution (e.g. ‘washed thoroughly’).
Actions to reduce risk were overwhelmingly described taking place indoors: in the house or home, usually the kitchen, surfaces, toilets, bathrooms and only 33 of the 573 respondents described ways they reduced their risk when outdoors in the countryside or garden. Places cited outside the home included restaurants and public toilets. While 47 respondents from 573 describing their intentional protective behaviour against E. coli O157 mentioned animals, only 15 specifically mentioned farms and only six mentioned cattle. Cleanliness, food and the home were uppermost in people's deliberate strategies to reduce their risk from E. coli O157.
DISCUSSION
The findings provide novel data on common awareness and understandings of E. coli O157 and unsurprisingly show awareness to be highest in farmers living in an area of high disease incidence. Level of awareness among all farmers from both high- and low-incidence areas was similar to that of food workers where training in microbiological safety has been supported over many years and its effectiveness scrutinized in successive investigations of major E. coli O157 outbreaks from food [18, 19]. Visitors were the least aware. This widespread lack of awareness about E. coli O157 in visitors to rural North Wales and Grampian is pertinent when considering the Godstone Farm outbreak in September 2009 where 65 visitors to the farm attraction became ill with E. coli O157 resulting in 93 reported cases during the 8 weeks of the outbreak [15].
Nearly three quarters of visitors in our study had not heard of E. coli O157 and those who had heard of it were more likely to be naive about the risk of contracting E. coli O157 from sources other than food. Moreover, visitors may be naive about livestock, refining their protective behaviours for urban residency indoors. Concomitantly, they may also be immunologically naive to pathogens more common in rural areas [Reference Belongia20] and this has obvious implications for the probability and outcome of infection. The implications here are important when considering that about six million people visit rural Wales and five million visit Scotland's countryside each year [21]. Respondents knowing about E. coli O157, whether farmers, rural residents or visitors, intriguingly implied an almost uniform representation of the illness it produces as serious food poisoning with vomiting its main symptom. Most had no experience of E. coli O157 disease and may anchor this representation on a stomach upset, with which they are probably familiar. Tam and colleagues [Reference Tam, Rodrigues and O'Brien22] have shown that people with bloody diarrhoea are more likely to present to their GP than people without bloody diarrhoea. However, a countryside excursion may be overlooked by both GP and patient if bloody diarrhoea is not recognized as a key symptom of a disease acquired from farm livestock and this has obvious consequences for disease control.
The common view of E. coli O157 infection as vomiting by food poisoning (similar to Salmonella or Campylobacter) rather than dysentery with environmental origin has probably arisen from greater public attention to outbreaks than to sporadic infections of the organism over the last 20 years. Prominent news reports include outbreaks from undercooked beef burgers in the USA and the 2005 South Wales outbreak with 157 cases from contaminated beef in schools. The Public Inquiry into the 2005 South Wales outbreak was underway concomitantly with this research and may well have influenced responses gathered from residents in Wales. Inquiry hearings were reported regularly between February and July 2008 by Welsh TV and print journalists describing food hygiene failures by processor John Tudor & Son who supplied meats to schools. Thus respondents in our study having no direct experience of E. coli O157 might well anchor their propositional knowledge on media representations [Reference Breakwell23]. The food poisoning representation is perpetuated by news media even when epidemiology differs, for example Sky News reported E. coli O157 at Godstone Farm as a ‘vomiting bug’ [24].
A quarter of the Grampian farmers questioned in our study held different views from other respondents. Although they stated that E. coli O157 was harmful (data not shown) they also indicated that they would be only mildly ill themselves if infected (Table 3). Their views may well be interpreted using a theoretical framework of risk perception in which known hazards are thought of as lower risk than unknown hazards [Reference Slovic25]. However, it has been shown that farm workers regularly exposed to E. coli O157 might develop immunity [Reference Silvestro26] and the views of these Grampian farmers, based on personal experience, could be right. If so, the description of E. coli O157 dominant in literature reporting cases of human infection as a ‘rare’ and ‘nasty bug’, may describe only a part of the picture: the part seen by medical practitioners. The part of the picture seen by this subset of Grampian farmers suggests that exposure to E. coli O157 is more common and has serious outcomes in a few susceptible people. This conclusion could have implications for disease mitigation, shifting emphasis from reducing exposure to understanding susceptibility and resistance.
It may be informative for communicating E. coli O157 risk to rural visitors, to consider the mechanisms by which farmers gain knowledge of E. coli O157. These can be thought of as professional in the agricultural industry and social in the rural community. Farm businesses in the UK are subject to a range of regulation and guidance that directly and indirectly address risk to human health from E. coli O157, for example Control of Substances Hazardous to Health [27], Clean Livestock Policy [28] and The Water Environment (Diffuse Pollution) (Scotland) Regulations [29], to name but a few. Although E. coli O157 is not notifiable in livestock it is a recognized zoonosis and everyday farm practice incorporates prerequisites from legislative control. Professional demands for awareness of E. coli O157 risk are augmented by living in a high-incidence area. In Grampian, coverage of local outbreaks such as the New Deer Millennium Scout Camp and at Beechmar Grange, Auchinclech, by TV and newspapers may increase awareness of E. coli O157 as something local [Reference Bell and Crighton30]. Many rural residents in Grampian also maintain private water supplies and are informed about protecting against E. coli O157 via implementation of Private Water Supplies (Scotland) Regulations 2006 [Reference Hunter31]. Stories of recent and past E. coli O157 illnesses are heard often in Grampian, for example in livestock auctions, rural post offices and school playgrounds and the stories repeated and re-told (data not shown). In rural areas, some families have close connection with cases such as the death of 2-year-old Ellie Russell from Ballantrae in 2006. Local stories may have a profound influence on local understandings of E. coli O157 and comprise the context and composition of place in health and illness [Reference Cummins32].
We have been cautious to discuss our results in the context of the people studied and not extrapolate to the general population as the use of convenience sampling to obtain respondents limits generalizability. Although we recruited respondents using a wide range of extant social and professional structures such as businesses, unions, rural events, schools and visitor attractions from over 40 locations to avoid bias, the samples of farmers, non-farming rural residents, rural visitors and food workers may not be representative. These exploratory findings are robust for the 2031 respondents who gave their views on E. coli O157 and they provide a sound basis for future investigation.
This study suggests how different awareness of individuals may affect their likelihood of E. coli O157 infection through the environmental pathway implying visitors are more at risk in rural areas. The findings may also be relevant for other infectious pathogens that are food-borne and environmental-borne such as Campylobacter spp. and Salmonella spp. Our research touches upon the roles of the individual and the professional in personal and public health protection [Reference Ali33]. We suggest that understandings of E. coli O157 are influenced by popular representations and local experiences and lead to the development of behaviours, formed by local and personal circumstance, that are considered to be protective. Biomedical knowledge of the pathogen and epidemiology of the disease can coalesce with local understandings and assist professional public health obligations to the population through acknowledging and endorsing culturally appropriate health protective behaviours [Reference Douglas34]. The vulnerability of visitors can be addressed through location-specific practical guidance delivered imminently in-situ in high-risk areas where large numbers of people are likely to come into contact with cattle and sheep, e.g. farm attractions open to the public.
ACKNOWLEDGEMENTS
We thank NFU Scotland, NFU Cymru, Farmers Union of Wales, rural primary schools in Aberdeenshire and Moray, Greengrocer Inverurie, and all our co-researchers in the ‘Reducing Escherichia coli O157 risk in rural communities’ multi-disciplinary research team at Aberdeen, Bangor, and Manchester Universities and the London School of Hygiene and Tropical Medicine (http://www.abdn.ac.uk/reluecoliproject/index.htm). The work was funded by ESRC/BBSRC Grant award – award number: RES-229-25-0012 through the UK Research Councils' Rural Economy and Land Use (RELU) programme. RELU personnel had no role in study design, or in data collection and analysis, or in the writing of this paper.
DECLARATION OF INTEREST
None.








