Introduction
Application of mobile telecommunications technology in healthcare delivery has been well demonstrated in many developed and some developing countries (Epstein and Bing, Reference Epstein and Bing2011; Car et al., Reference Car, Gurol-Urganci, de Jongh, Vodopivec-Jamsek and Atun2012). The impacts on healthcare delivery and health-related outcomes have been invaluable (Guy et al., Reference Guy, Hocking, Wand, Stott, Ali and Kaldor2012; Tamrat and Kachnowski, Reference Tamrat and Kachnowski2012). However, in health systems that are naïve to the use of these technologies, planning a telecom-backed healthcare service delivery and investment of public fund in acquisition and application of such technologies require adequate understanding of patients’ disposition to such interventions as well as the prevailing circumstances in healthcare service delivery that need to change (Källander et al., Reference Källander, Tibenderana, Akpogheneta, Strachan, Hill, ten Asbroek, Conteh, Kirkwood and Meek2013).
Public-funded health facilities are critical to healthcare delivery in developing countries such as Nigeria; where the burdens of poverty and disease coexist with a predominance of out-of-pocket payment for healthcare services (Hargreaves, Reference Hargreaves2002; Olakunde, Reference Olakunde2012). In Nigeria, anecdotal experience indicates that healthcare delivery at most public health facilities are characterized by a mix of patient overload with a shortage of human and material resources. For instance, in the south-western city of Lagos, which is Nigeria’s largest city, a situation that is commonly encountered at public hospitals is large crowd of people waiting for long hours before receiving healthcare services. This is particularly common at the General Outpatients Departments (GOPD) of general hospitals, which are supposed to be secondary healthcare facilities.
The GOPDs are first contact clinics that do not mandate patients to present referral letters before accessing care. Thus, they are walk-in units that provide treatment and referral services; and are extensively used as primary care units. Partly accounting for overcrowding at GOPDs is the current state of the primary healthcare delivery system; which in most parts of the country is characterized by poor infrastructure, inadequate equipment and insufficient manpower. Ineffective primary healthcare system compels individuals to present directly at the GOPD of general hospitals (Adeyemo, Reference Adeyemo2005; Onwujekwe and Uzochukwu, Reference Onwujekwe and Uzochukwu2005).
As shown by studies on overcrowding in the emergency department, the consequences of overcrowded waiting rooms and long waiting time in healthcare settings are multidimensional; including negative impacts on care processes, unsatisfactory patient experience and poor treatment outcomes (Hoot et al., Reference Hoot and Aronsky2008; Gilligan et al., Reference Gilligan, Joseph, Bartlett, Morris, Mahajan, McHugh, Hillary and O’Kelly2015; Kagobora and Ntomkibifile, 2014). In addition, overcrowded waiting rooms can encourage the spread of infectious diseases such as tuberculosis. In addition, anecdotal experience suggests that individuals are discouraged from seeking healthcare because of logistic concerns. This can promote delay in presentation and impact negatively on morbidity and mortality. The situation is also unhealthy for health workers who are often overworked by unplanned work schedules in tense clinic environments (Collins, Reference Collins2010).
We approached the study from a willingness dimension because in this research context, deployment of telecommunications-based solution for appointment scheduling is situated at the intersection of patients’ preference and the need to pay. Considering that willingness to pay is a valuation methodology employed in surveys for quantifying the degree of consumer preference for a service (Corso et al., Reference Corso, Hammitt, Graham, Dicker and Goldie2002; Marra et al., Reference Marra, Frighetto, Goodfellow, Wai, Chase, Nicol, Leong, Tomlinson, Ferreira and Jewesson2005), we avoided skewing the study into the quantitative domains of willingness to pay by adopting willingness to utilize the proposed system as an encapsulation of patients’ preference and the qualitative dimensions willingness to pay.
At present, none of the GOPD at public hospitals in Lagos operates an appointment scheduling system. This study aimed to evaluate the willingness of patients to utilize a proposed patient-financed phone-based appointment scheduling system.
The system described to the patients in this study is based on the short message service (SMS; also called text message), which is now a widely available application on most telecommunication platforms in the country. Our objectives included evaluation of patients’ disposition towards and willingness to utilize a proposed appointment system as well as exploration of current trends in waiting time and patients’ worries about accessing healthcare services at public healthcare facilities.
Methods
Setting
This study was conducted at the family medicine unit of adults GOPD, General Hospital Orile-Agege, Lagos, Nigeria. The study was approved by the hospital review board. The hospital is a secondary care facility providing inpatient and outpatient services to a large semi-urban population. Patients are not required to present referral letters from other care providers before accessing the hospital’s services. Thus, a significant proportion utilizes the centre for primary care. The family medicine unit is one of the five first contact clinics that make up the GOPD. New cases are randomly assigned to each of the clinics. All non-emergency cases presenting at the hospital are first seen and managed at the GOPD. Internal and external referral services are also provided. The GOPD clinics run from 8am to 4pm on Mondays to Fridays. An average of 350 patients is seen on each working day.
Study design and data collection
This study employed a descriptive design. We interviewed patients who were assigned to the family medicine unit over a three-month period (January–March 2011) about their willingness to use a SMS-based appointment scheduling system for organizing their clinic visits to the facility or at any other public hospital in the state. Interviews were conducted only with patients who verbally consented to participate after the purpose and methods of the study were explained to them at the end of their consultations. However, the study was introduced to all patients who were randomly assigned to the family medicine unit during the study period. The interview was brief and consisted of five question items that were presented semi-formally to encourage respondents to provide factual information and express their frank opinion. The interview explored: respondent’s estimated arrival time at the hospital; respondent’s single most important worry whenever they had to seek for healthcare services at public hospitals in Lagos; if respondent owned a mobile phone at the time of the interview; if respondent would be willing to utilize a phone-based appointment scheduler for booking hospital/clinic visits; and if respondent was willing to pay for the proposed service. Finally, each respondent was asked to suggest a tariff for a phone-based appointment system in which patients would send a SMS to a designated number to book a clinic appointment, receive booking confirmation details and also receive an appointment reminder 24 h before the appointment date, that is, a three SMS booking system. Questions were presented in simple non-technical language. Explanations and clarifications were provided when necessary to ensure that respondents were clear about the aim of each question item. Local language and Pidgin English were also employed to ensure that each participant understood the question sufficiently to provide a reliable ‘short phrase’ or Yes/No response.
The study questions were developed from an assessment of patient inputs required for operating a voluntary SMS-based appointment system. This was conducted during discussions with patients and health workers at our hospital. There was a consensus that patients would need access to mobile phones, awareness about the feasibility of using SMS for the purpose appointment scheduling and the financial wherewithal to utilize the service. The question item focusing on patients’ worries about healthcare delivery at public hospitals was included to explore the concordance between patients experience and what we sought to alleviate through the proposed intervention.
Data on respondent’s socio-demographic profile (including age, sex, highest level of education and occupation) and the starting time for the consultation were obtained from the patient’s folder. Starting time for consultations were carefully documented on the case folder of each participant by the investigating clinician all through the study period.
Data management and statistical analysis
All study data including socio-demographic information and interview responses were immediately documented in the study data collection forms. Data were then transferred to a spreadsheet for storage and backup. Data analysis were performed using GraphPad Prisms version 5 statistical package for Windows. Estimated waiting time was derived as the time interval between patient estimated arrival time and consultation starting time. Descriptives statistics such as percentages and frequencies were evaluated for categorical variables while means and standard deviation were determined for continuous variables. Inferential statistics such as unpaired t-test, Fisher’s exact test and one-way analysis of variance (ANOVA) were also appropriately evaluated. For all statistical tests P-value<0.05 was considered significant.
Results
Participants’ characteristics
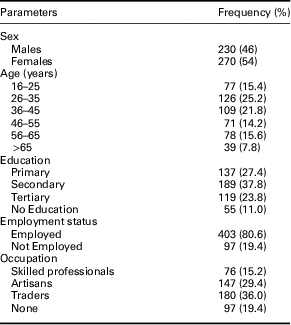
A total of 500 patients provided consent and participated in this study. Socio-demographic characteristics of the participants are summarized in Table 1. Females comprised 54% (n=270) of the study population. Participants were aged 16–86 (42.1±15.4) years. Differences in the mean ages of males [16–78 (42.4±16.7) years] and females [19–86 (41.8±14.2) years] were non-significant (t=0.434, P=0.664); 11% (n=55) of the respondents had no formal education. Respondents who had no formal education were significantly older than those with at least primary education [35–86 (58.2±11.5) versus 16–78 (40.1±14.6) years; t=8.87, P<0.0001]. The proportion of female respondents among the non-educated sub-population was significantly higher than that of males (78.2% versus 21.8%; P=0.0002, Fisher’s exact test). However, the distribution of highest educational attainment did not differ significantly between females and males (χ 2=3.453, P=0.178). Majority of the respondents were traders (n=180, 36%) or artisans (n=147, 29.4%). Less than one-fifth of the participants were skilled (professional) workers (n=76, 15.2%). Distribution of occupations differed significantly between males and females (χ 2=100.1, P<0.0001); the latter accounted for 79.4% of traders while the former accounted for 70.8% of artisans.
Table 1 Socio-demographic characteristics of the 500 study participants
Willingness to utilize and pay for the proposed service
Figure 1 shows the summary of our major findings. Nearly all the participants favoured a SMS-based appointment system (n=486, 97.2%). Patients who were undecided were as many as those opposed to the system (n=7, 1.4%). Nearly all undecided respondents were females (n=6), while slightly more males (n=4) than females (n=3) expressed absolute opposition to the system. In addition, almost all patients who favoured the phone-based appointment system were willing to pay for the service (n=484, 99.6%). However, about one-fifth [n=95, (19.6%)] of those who expressed their willingness to pay for the service could not suggest a tariff considered as acceptable service charge. More female respondents were found in this sub-set than males (64.9% versus 35.1%; P=0.016).

Figure 1 Summary of the main findings
Waiting time
Estimated waiting time ranged from 1 to 7.5 h (3.9±1.1). Differences between the estimated waiting times among male 1–7.5 (3.9±1.2) and female 1–7 (3.9±1.1) respondents were statistically non-significant (t=0.071, P=0.943). In addition, in sub-group analysis that adjusted for education level and occupation, respectively (Table 2), non-significant differences in the mean waiting time were observed across (one-way ANOVA) and between groups (post-hoc: Tukey’s multiple comparison) P>0.05 for all.
Table 2 Comparison of waiting time across and between occupation groups and education levels

ANOVA=analysis of variance.
a P-values across (one-way ANOVA) and between (Tukey’s post-hoc test) groups were statistically non-significant.
Participants’ worries about public hospitals
Two overlapping themes emerged as patients’ most important worries about public hospital services viz: ‘long queues people waiting for long to receive healthcare services in crowded waiting halls’ and ‘long waiting time’. Only two (0.4%) respondents stated that they had no worries about the service delivery process at public hospitals.
Mobile phone ownership and suggested tariff for proposed SMS service
Ownership of mobile phones was found in 96.4% (n=482) of the study population. Majority of respondents who had no mobile phones were females (n=14, 77.8%; P=0.052). Tariffs suggested for the proposed three SMS booking system ranged from 0.03 to 20.83 (1.53±2.11) US dollars. Differences between the tariffs suggested by males [$0.08–$20.83 (1.59±2.51)] and females [$0–$8.33 (1.45±1.63)] were statistically non-significant (P=0.691).
Sub-groups analyses for differences in suggested tariffs which adjusted for age, education and occupation, respectively, are shown in Table 3. Statistically non-significant differences were found across and between age quartiles, education levels or occupation groups.
Table 3 Comparison of suggested tariff across and between sub-groups under occupation and education

a One-way analysis of variance with Tukey’s post-hoc test.
b Independent t-test.
As at the time of the study telecom service providers charged 15 Naira (Nigeria’s official currency) per SMS. This was equivalent to about 0.125 US dollars ($), based on official exchange rate of 120 Naira to $1 at that time. Thus, the cost of three text messages was about $0.375. Relative to the retail cost of three texts at study time, 89.8% (n=349) of all respondents suggested a tariff that was greater than the retail cost of three SMS texts.
Discussion
Main finding
We evaluated patients’ willingness to utilize a SMS-based appointment scheduling system at a Family Practice unit in Lagos, Nigeria. Our main finding was that a vast majority of the patients studied were willing to utilize and pay for a SMS-based appointment scheduling service for clinic visits.
Participants’ characteristics and waiting time
We observed some differences in the socio-demographic characteristics of male and female participants that are in consonance with the prevailing gender disparities in education and employment opportunities in contemporary Nigeria (Adeyemi and Akpotu, Reference Adeyemi and Akpotu2004; Okpara, Reference Okpara2006, National Population Commission and ICF Macro, 2009). The observed duration of waiting time in this study is in line with concerns raised by the authors as a justification for this study. It would also partly explain the support expressed for the phone-based appointment scheduling system by the participants as well as their willingness to pay for the service. We are convinced that the observed waiting time in this study reflects the natural occurrence at this centre; and this is evidenced by the lack of significant differences in waiting times between males and females, as well as across and between age quartiles or educational levels.
Participants’ worries about public hospitals
The emergence of two themes that are related to waiting time as the chief concerns for most patients seeking healthcare services from public hospitals underscores the centrality of waiting time to healthcare accessibility as well as its multidimensional impact on patients’ perception of the quality of health services provided by public-owned facilities. Similarly, studies of patients’ satisfaction with healthcare services at public hospitals in eastern and northern parts of Nigeria found that waiting time domains were scored lowest by respondents (Iliyasu et al., Reference Iliyasu, Abubakar, Abubakar, Lawan and Gajida2010; Iloh et al., Reference Iloh, Ofoedu, Njoku, Odu, Ifedigbo and Iwuamanam2012; Reference Iloh, Ofoedu, Njoku, Okafor, Amadi and Godswill-Uko2013).
Mobile phone ownership and willingness to use the proposed service
Ownership of mobile phones by a vast majority of respondents would also contribute to the expression of support for the proposed phone-based appointment system by most of our subjects. The willingness to pay for the service indicates a desire for a more efficient healthcare services delivery which will eliminate wastage of productive time that is currently associated with seeking for healthcare at public hospital. In addition, the respondents’ desire for this change possibly underlies the observation that a clear majority suggested tariffs that are higher than the current market costs of the proposed service. It is also noteworthy that close to one-quarter of those who did not own mobile phones still favoured the proposed system. They stated that they would still benefit from it by using phones owned by friends or family members. In addition, when asked how they intended to overcome the challenge posed by inability to compose or read a message, respondents who had no formal education (majority of whom had mobile phones and were willing to use the proposed system) identified the ready availability of support from family members and friends.
Study findings in relation to existing literature
To our knowledge this study is possibly the first to have evaluated patient’s willingness to utilize a SMS-based appointment system in a developing country in which the use of such technologies in public hospital systems is still very rare. However, in developed countries where phone-based appointment systems are already in use, several studies have evaluated patients’ satisfaction with the system and also assessed comparative effectiveness of different modalities of phone-based appointment systems (Car et al., Reference Car, Gurol-Urganci, de Jongh, Vodopivec-Jamsek and Atun2012; Gurol-Urganci et al., Reference Gurol-Urganci, de Jongh, Vodopivec-Jamsek, Atun and Car2013; Kannisto et al., Reference Kannisto, Koivunen and Välimäki2014).
A recent study which investigated the use of different appointment registration systems and the factors influencing patients’ registration system choices across different regions of China found that nearly two-thirds of the 1009 patients surveyed used one form of phone-based appointment scheduling or the other, while about one-third preferred non-scheduled appointment. Statistically significant differences in gender, education and residence location were found between the scheduled appointment and non-appointment groups (Yu et al., Reference Yu, Yu, Hu, Duan, Liu and Wang2013). It is possible that the differences may have been influenced by individual preferences. This is because reports from previous studies (in which the vast majority of the study participants favoured phone calls or SMS reminders) indicated that some patients declined the use of phone-based appointment scheduling because of complaints of disturbance by appointment reminders (Fairhurst and Sheikh, Reference Fairhurst and Sheikh2008; Parikh et al., Reference Parikh, Gupta, Wilson, Fields, Cosgrove and Kostis2010; Griffin et al., Reference Griffin, Hulbert, Vernon, Nelson, Hagel, Nugent, Baines, Bangerter and van Ryn2011).
The choice of SMS system in this study was based on the lower cost and further reduction in the cost of service that can be negotiated for large volume subscription as compared with telephone call. This is further supported by evidence from a recent randomized controlled trial which showed that text messaging was as effective as, but more cost-effective than, phone call reminder in reducing missed appointments at an academic primary care clinic (Perron et al., Reference Perron, Dao, Righini, Humair, Broers, Narring, Haller and Gaspoz2013).
Limitations and strengths of the study
Limitations of this study include the use of a hospital-based population whose characteristics and perceptions may not be representative of the community or larger population. However, the need to situate this study within the context of patients’ current experiences with healthcare access makes the setting appropriate. In addition, the study sample included respondents from different demographic and socio-economic strata, which would likely enhance the external validity of our findings.
Our study is also possibly limited by the non-availability of data on monthly income, a potentially relevant variable, especially in testing whether suggested tariffs were driven by income or individual purchasing power. We opine that monthly income would not have had any objective value considering that only less than one-fifth of our study population belonged to the formal sector of the economy. In our study setting, traders and artisans are not able to provide reliable income estimates owing to continuous fluctuations in their earnings. Thus, we consider occupation and employment status as satisfactory proxy-variables for income in this context. In addition, the inability of socio-demographic factors to explain our observations underscores the significance of our findings. In this setting, studies evaluating the implementation of pilot projects on phone-based appointment scheduling systems are still needed. Such studies would have to assess its impact on patient satisfaction and overall cost of healthcare services.
Conclusion
This study has shown that our patients are willing to utilize and pay for a phone-based appointment scheduling system. It will be desirable if healthcare policy makers consider exploring this to improve access to healthcare services.
Acknowledgement
The authors are thankful to all the patients who participated in this study.
Financial Support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Conflicts of Interest
None.







