Introduction
Sport-related concussions (SRCs) have been at the forefront of sport medical concerns at all levels of sport. Concerns are especially focused on children aged 10–19 given their high prevalence of concussions1 and considering the importance of this time period with respect to brain development.Reference Harris, Jones, Rowe and Voaklander2 The increasing awareness of chronic traumatic encephalopathy (CTE) has added to the concern about the long-term implications on quality of life in later years. Alosco et al.Reference Alosco, Mez and Tripodis3 reported on 211 tackle football players who donated their brains and determined that the onset of CTE symptoms increased 2.44 years earlier for every year before the age of 12 that the individual started playing football. Although the signs were deemed to be mild, 3 of 14 (21%) high school football players tested positive for CTE at autopsy.Reference Mez, Daneshvar and Kiernan4
The Center for Disease Control (CDC) reported 2.8 million traumatic brain injury (TBI)-related US emergency department (ED) visits in 2013. The rate of ED visits for sport-and-recreation (SR)-related injuries more than doubled among children 19 years and younger between 2001 and 2012.1 Zhang et al.Reference Zhang, Sing, Rugg, Feeley and Senter5 reported on insurance-based data that included 8,828,248 patients of which 43,884 patients were diagnosed with a concussion between 2007 and 2014. Youth, aged 15–19 years, had the highest incidence (16.5/1000 patients), followed by those 10–14 years (10.5/1000 patients), 20–24 years (5.2/1000 patients), and 5–9 years (3.5/1000 patients). During that 7-year span, there was a 60% increase in concussions.
According to the Canadian Hospitals Injury Reporting and Prevention Program (CHIRPP), the prevalence of concussions from 2011 to 2016 was 12% of all sport-related injuries. Of those, males 15–19 years incurred the most concussions reportedly in rugby (22.7%), ice hockey (20.2%), football (17.4%), and basketball (10.4%). Conversely, concussions in female athletes 15–19 years in this same time period represented 18% of all injuries including ringette (44.37%), ice hockey (36.6%), rugby (27.7%), and basketball (17.7%).Reference Bryan, Rowhani-Rahbar, Comstock and Rivara6
Harris et al.Reference Harris, Jones, Rowe and Voaklander2 reported on SR-based head injuries (HI) from five hospitals in the Edmonton region from 1995 to 2007. Of the 63,219 SR-related injuries recorded, 4935 (7.8%) were HI. Patients less than 18 years of age sustained 69.8% of all SR head injuries.
In 2016–2017 alone, 46,000 concussions were diagnosed in Canadian hospital EDs for children aged 5–19. Ice hockey, rugby, and ringette accounted for the most concussions (ranging from 27% to 44%). Males accounted for more concussions (54%) than females (45%).Reference Register-Mihalik, Linnan, Marshall, McLeod, Mueller and Guskiewicz8
In 2016, the Federal, Provincial and Territorial (F-P/T) Ministers responsible for sport, physical activity, and recreation acknowledged that concussions were an important public health issue. The federal government committed 1.4 million dollars over 2 years to develop a national strategy to prevent and treat SRCs.7
High School Concussion Rates
There is very little data regarding the prevalence of concussions in high school sports. Register-MihalikReference Register-Mihalik, Linnan, Marshall, McLeod, Mueller and Guskiewicz8 reported that 53.3% of surveyed participants reported having sustained at least one SRC.Reference Pakzad-Vaezi and Singhal12 McCrae et al.Reference McCrea, Hammeke, Olsen, Leo and Guskiewicz9 reported that of 1532 varsity football players from 20 US high schools, 29.9% reported a previous history of concussion and 15.3% reported sustaining a concussion during the current football season. Gessel et al.Reference Gessel, Fields, Collins, Dick and Comstock10 reported that 8.9% or 396/4431 high school athletic injuries in 2005–2006 were diagnosed as concussions. Marar et al.Reference Marar, McIlvain, Fields and Comstock11 reported on 1936 concussions in athletes also from 20 US high school sports over a 2-year period. The authors reported a rate of 2.5 per 10,000 athlete exposures (AEs). The injury rate was greater during competition (6.4). Only Pakzad-Vaezi and SinghalReference Pakzad-Vaezi and Singhal12 reported on Canadian, albeit indirect school data. The authors reported that 29.6% of the 27,466 SR activity injuries reported at the Vancouver Children’s Hospital between 1992 and 2005 occurred at school. In this same timeframe, head injuries represented 11.3% of all injuries and 20.6% of all admissions to hospital.
Unreported Injuries
As concerning as the prevalence of concussions may be, concussions are deemed to be underreported.Reference Meehan Iii and Bachur13 As many as 50% of concussions go unreported.Reference Register-Mihalik, Linnan, Marshall, McLeod, Mueller and Guskiewicz8, Reference Meehan Iii and Bachur13–Reference Kerr, Register-Mihalik, Kroshus, Baugh and Marshall15 Most studies are based on concussions reported to EDs.Reference Caine and Purcell16 Concussions that may not be captured in the data include those who report to their family physician, athletic therapist, or walk in clinic and so on. KerrReference Kerr, Register-Mihalik, Kroshus, Baugh and Marshall15 reported that football players were least likely to report a concussion (68.3%) and males were least likely to report than females. MeehanReference Meehan Iii and Bachur13 suggests that trained observer data are significantly higher than self-reported data. McGuineReference McGuine, Pfaller, Post, Hetzel, Brooks and Broglio17 determined that the reporting of concussions increases from schools with low- to medium- to high-level access of on-site athletic trainers. Only 50% of those athletes with low access to an athletic trainer followed a return to play protocol. McCreaReference Kerr, Register-Mihalik, Kroshus, Baugh and Marshall15 reported that the most common reason for not reporting was lack of awareness of the seriousness of a concussion (66.4%) followed by fear of being withdrawn from participation (41%) and unable to recognize a concussion (36.1%).
Research indicates that concussion education may have an effect on the reporting rate.Reference Taylor and Sanner18–Reference Kurowski, Pomerantz, Schaiper, Ho and Gittelman20 TaylorReference Taylor and Sanner18 conducted a systematic review of four studies, three of which demonstrated an association between education and increase reporting of concussions. In a study of Korean athletes, Lee et al.Reference Lee, Resch, Han, Miles and Ferrara21 reported that, of the 8.9% of participants who reported having sustained a concussion, only approximately 50% reported the incident.27
Education also affects the athlete’s decision to return to play. KurowskiReference Kurowski, Pomerantz, Schaiper, Ho and Gittelman20 reported that there was a significantly lower proportion of athletes who continued to play despite having symptoms of concussion in those schools with concussion education (72%) compared to students who did not receive concussion education (78%). In the Korean high school study, 63.9% of the athletes who reported SRC symptoms made their own return to play decisions.Reference Lee, Resch, Han, Miles and Ferrara21 EaglesReference Eagles, Bradbury-Squires, Powell, Murphy, Campbell and Maroun22 reported that although concussion knowledge was maintained over time, attitudes did not change from baseline. KroshusReference Kroshus, Garnett, Baugh and Calzo28 reported that SRC education resulted in an increase in athlete intention to encourage teammates to report a concussion but no effect on their intention to report their suspicions to a coach or athletic trainer.
The purpose of this research was to determine the incidence of concussions in Canadian high school sport, athlete knowledge of the signs, symptoms and consequences of SRC, and how likely student athletes are to report a concussion.
Methods
Research Design
A cross-sectional survey of athletes from five high schools in a single school division in the Winnipeg area was administered between December 2015 and May 2016. All athletes who competed in all high school sanctioned sports were invited to participate. A survey questionnaire was explained using a prescribed script and administered in a group setting by two research assistants at each school. The survey collected information on their concussion history, knowledge of concussions, and attitude toward reporting a concussion. Ethics approval was granted by the University of Winnipeg Human Research Ethics Board (UHREB).
Survey Instrument
The survey was a modified version of that validated by Register-Mihalik.Reference Register-Mihalik, Guskiewicz, McLeod, Linnan, Mueller and Marshall14 Based on discussion with the author, amendments were made to some questions including a revised list of sports to coincide with Canadian high school sports. Questions 1–10 collected demographic information including their sport participation and if they ever received education about concussions. Questions 11–25 determined the level of knowledge regarding concussions. Questions 26–29 investigated the athlete’s attitude toward concussion specifically looking at their attitude toward returning to play with a concussion. The signs and symptoms as listed on the SCAT 5 were included in the survey as were four false statements to serve as distractors (chest pain, skin rash, bleeding nose, and black eye). Questions 30–39 formed the second section of the survey, and specifically focused on those athletes who sustained an SRC while in high school. This section began by defining a concussion and its symptoms followed by questions to determine the incidence of concussions in sport and practices. The remaining questions collected information related to the rate of reporting and the attitudes and barriers that may have an effect.
Procedure
Approval from the school division was obtained. The physical education supervisor for the school division coordinated contact personnel in each school. The most convenient date and time was arranged with each contact person. Letters to the parents with attached athlete assent and parent consent forms were sent to the school contact person for distribution. Participation was completely voluntary. The survey was administered in paper form to athletes as a group at each high school at a predetermined date and time. Each student submitted a signed athlete assent and parental consent form prior to commencement of the survey. The research assistant provided prescripted directions to ensure consistency between schools. The students were informed to complete the first section of the survey and notify the research assistant when it was completed. Research assistants were available to answer any specific questions restricted to the logistics of the questionnaire. The first completed section was collected before the athlete continued with the second section of the survey. The survey required approximately 20 minutes to complete. Responses from the questionnaires were logged into an excel spreadsheet formatted to quantify the data.
Analysis
General descriptive statistics were used to examine the incidence of concussions, athlete knowledge and attitude scores, and concussion-reporting behaviors.
Results
A total of 225 athletes agreed to participate including 127 (56.7%) males and 97 females (43.3%). One individual did not respond to the gender question. The mean age was 15.5 years ±1.1. Athletes who participated in high school sanctioned sport including football (19.9%), hockey (18.6%), soccer (8.1%), basketball (21.3%), volleyball (29.4%), lacrosse (0%), track & field (1.8%), and field hockey (0.5%) were included in the study. Students were distributed across all four grades including grades 9 (27.%), 10 (33.3%), 11 (22.7%), and 12 (16.9%). Varsity and Junior varsity athletes accounted for 53.2% and 46% of the total participants, respectively. Table 1 outlines the subject demographics. Participation per school was distributed accordingly (names of schools have been deleted for confidentiality): high school 1 (34.2%), 2 (15.6%), 3 (16%), 4 (14.7%), and 5 (19.6%).
Table 1. Athlete demographics
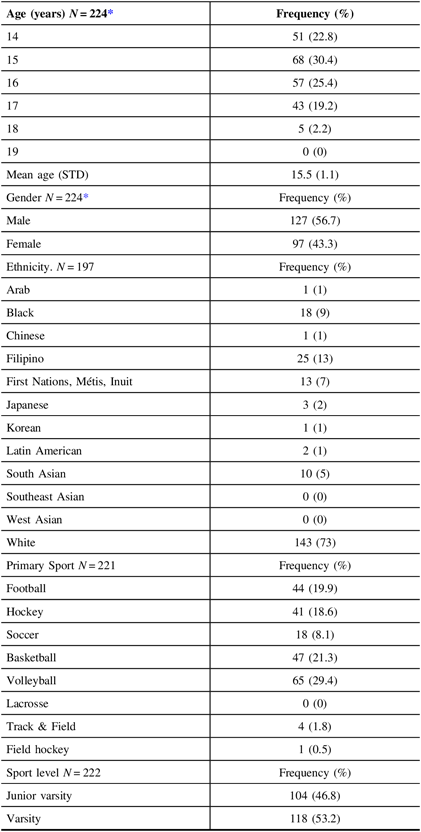
* One person did not respond.
Almost 70% (68.9) of the participants had some education about what constitutes a concussion or what to do in the event of a concussion (Table 2). Of those who reported having received this education, coaches (44.9%) and parents (48%) were most often the source of information. Physicians and athletic therapists were consulted by 30.7% and 21.8% of respondents, respectively. The latter likely reflects the fact that physicians and athletic therapists are not easily available to high school athletes. Of the 225 respondents, 40.2% (90) reported having sustained at least one concussion from all activities including sport. Seventy-eight (35.3%) of the respondents reported having sustained an SRC (Table 3).
Table 2: Athlete source of concussion information
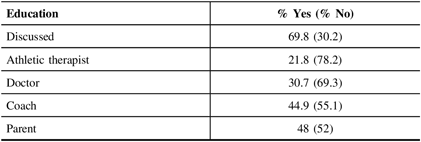
Table 3: Reported concussions
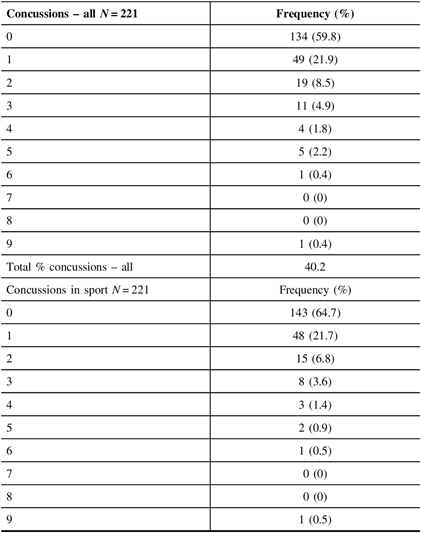
Total % concussions in sport 35.3.
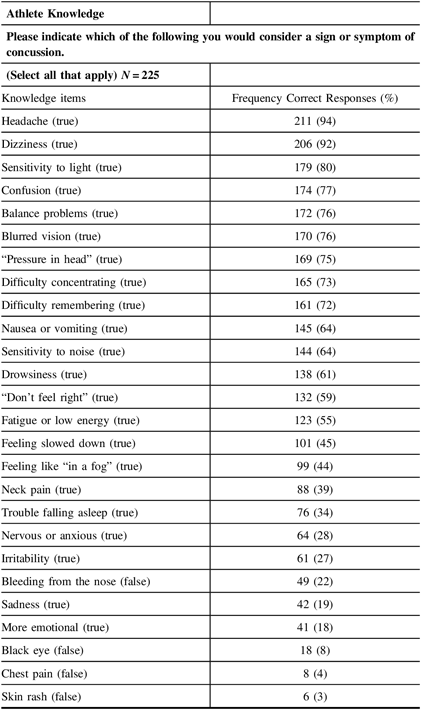
The knowledge items which had 60% or more positive responses were primarily physical and cognitive in nature. Concussion signs and symptoms recognized less than 60% of the time were more “feeling” and emotional in nature (Table 4). High school students are less likely to relate “feeling” issues as a consequence of a concussion including not feeling right (59%), fatigue or low energy (55%), feeling slowed down (45%), and feeling like in a fog (44%). Emotional issues were even less likely to be associated with a concussion including being nervous or anxious (28%), being irritable (27%), sadness (19%), and more emotional (18%). Interestingly, neck pain (39%) and trouble falling asleep (34%) were also not commonly associated with concussions. For the most part, respondents were less likely to identify those symptoms that were not commonly associated with a concussion including bleeding from the nose (22%), black eye (18%), chest pain (4%), and skin rashes (3%).
Table 4: Athlete knowledge items
With respect to general knowledge (Table 5), most participants were aware that sustaining a concussion was not dependent on loss of consciousness (84%). Most (83%) were aware that one should not return to play when experiencing any signs or symptoms of concussion. Similarly, most respondents were aware that a concussion was an injury to the brain (90%) as opposed to the skull (6%).
Table 5: General athlete knowledge items
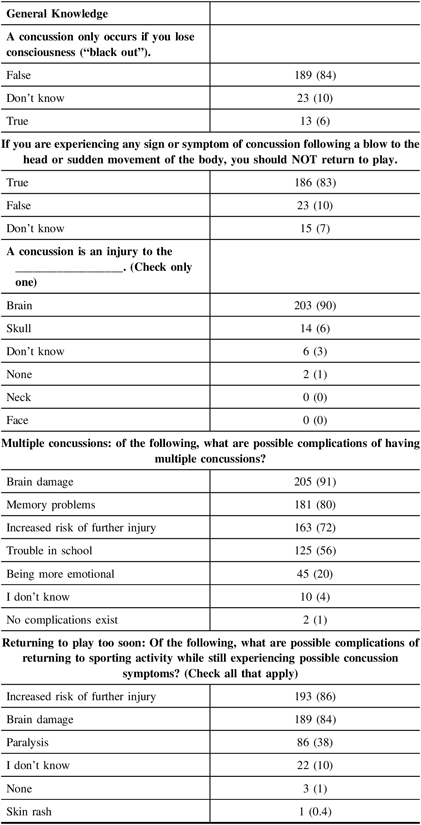
Most respondents recognized that brain damage (91%) and memory problems (80%) were possible complications of multiple concussions. Fewer (72%) were aware of the risk of further injury (such as second impact syndrome). Trouble in school was associated as a complication of multiple concussions by only 56% of respondents. Once again, only 20% of participants recognized the effect of multiple concussions on emotional health.
Respondents were aware that early return to play before full recovery could result in an increase in further injury (86%) and further brain damage (84%). The increased chance of paralysis was deemed to be a possibility by only 38% of respondents.
Respondent attitude toward concussion is generally positive and in support of getting more information about concussions and the importance of reporting a concussion to a coach or medical personnel. Similarly, there was a generally positive attitude with regard to how they would feel about reporting the signs and symptoms of a concussion in a game or practice situation. The only two notable feelings are feelings of difficulty to report (3.5/7) and feelings of embarrassment (3.4/7) (Table 6).
Table 6: Athlete attitude
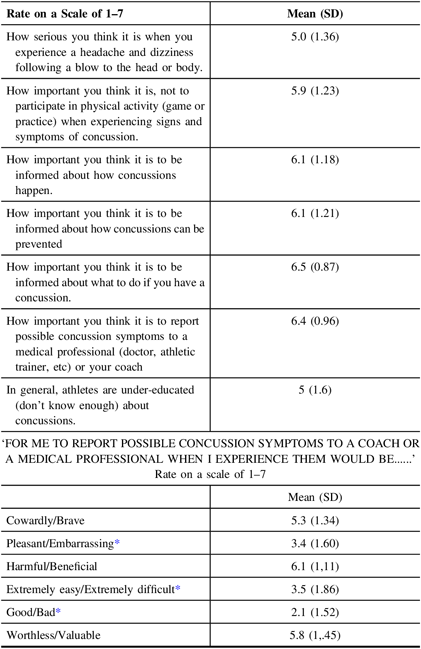
* These indicate reverse values where a low score is more indicative of a positive attitude.
Even though there is general agreement that concussions should be reported, 38.4% of all respondents indicated having continued play with signs and symptoms of a concussion incurred during a game situation and 33.8% during practice (Table 7). In contrast, most respondents indicated that they would report their concussion to a medical professional or coach (N = 222, Mean 5.9/7, SD 1.4). In keeping with these results, when asked what reasons would lead them to not report a concussion, 35.3% of respondents indicated they would report the concussion regardless. Notably, 45.6% of respondents would not report a concussion thinking the concussion was not serious enough. Approximately one-third (32.2%) of respondents may not report a concussion because they would not know it was a concussion or they would not want to be removed from the game. There was strong agreement (Mean 5.91/7, SD 0.09) when asked if they intend to report a concussion should they experience one in the future (Table 8).
Table 7: Continued to play in game or practice with symptoms

Table 8: Barriers to reporting a concussion

As indicated in the procedures, once respondents completed the first section of the questionnaire, they were given the second portion of the survey. This section began by first outlining the signs and symptoms of a concussion and focused on collecting data specifically from athletes who sustained an SRC in a game or practice situation.
USE THE FOLLOWING DEFINITION TO ANSWER THE QUESTIONS IN THIS SECTION (SECTION 2)
A concussion is an injury caused by a blow to the head or sudden movement of the body followed by a variety of signs and symptoms that may include any of the following: headache, dizziness, loss of balance, blurred vision, “seeing stars”, feeling in a fog or slowed down, memory problems, poor concentration, nausea, or throwing up. Getting “knocked out” or being unconscious does NOT always occur with a concussion.
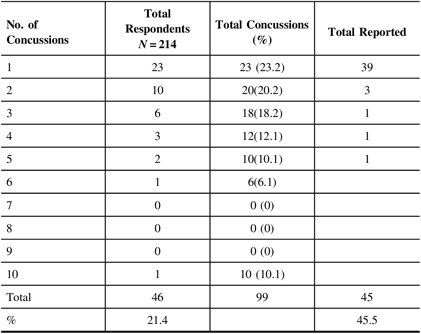
Using this definition of a concussion, respondents were once again asked to report on the number of concussions they sustained during their high school years in either games or practices. In this case, 73 (32.7%) of all respondents reported having sustained a total of 156 concussions during a game. Of the total game-related concussions, 71/156 (45.5%) were reported to a medical professional or coach (Table 9). Only 45/99 (45.5%) of concussions incurred during practice were reported (Table 10).
Table 9: Athlete report of concussion post definition during games
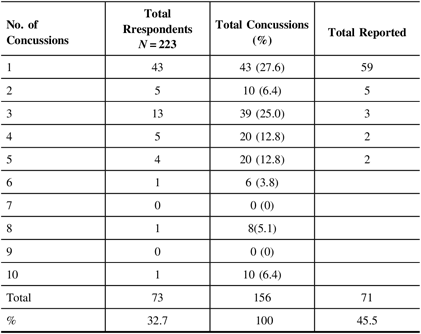
Table 10: Reported concussions in a practice situation
Of those respondents who indicated having chosen not to report at least one concussion, 52% did not think it was serious enough to report, 31.5% would not want to let their teammates down, 26.8% did not want to let their coaches down, 37.0% did not know at the time it was a concussion, 25.2% did not want to be removed from a practice, and 45.7% did not want to be removed from the game. The perceived feelings toward reporting a concussion were similar in those who indicated not having reported a concussion and the feelings of all respondents. Being embarrassed (3.1/7, SD 1.31) and extremely difficult (3.1/7 SD 1.71) were the most notable concerning feelings expressed.
Discussion
There are a number of interesting insights from this study. The rate of reported concussions in this study coincided with that reported by some studies,Reference Zhang, Sing, Rugg, Feeley and Senter5,Reference Bryan, Rowhani-Rahbar, Comstock and Rivara6,Reference Register-Mihalik, Guskiewicz, McLeod, Linnan, Mueller and Marshall14 but higher than that reported in some studies.7,Reference McCrea, Hammeke, Olsen, Leo and Guskiewicz9,Reference Gessel, Fields, Collins, Dick and Comstock10,Reference Pakzad-Vaezi and Singhal12,Reference Giannotti, Al-Sahab, McFaull and Tamim23 The fact that 40.2% of high school athletes in this study reported an SRC points to the need for a concerted preventative effort. The Federal Government of Canada allocated 1.4 million dollars to a concussion strategy based on the fact that 39% of children and youth 10–18 years who visit an ED in Canada were diagnosed with a concussion. A further 24% were designated possible concussions. Most athletes in the study were well versed on the physical signs and symptoms of a concussion but less so on the cognitive and emotional symptoms. Lee et al.Reference Lee, Resch, Han, Miles and Ferrara21 reported that none of the Korean athletes surveyed were able to identify all of the nine SRC signs and symptoms. Given the close relationship an athlete has with their peers, it is important that they are able to identify and relate changes in mood and personality to a concussion so that a concussion is reported early, properly identified, and managed. The primary source of education was from parents and coaches and less so from physicians and athletic therapists. This would suggest the importance of educating parents and coaches.
Athletes are still choosing to return to practice and games even though they are experiencing signs and symptoms of concussion. Wanting to remain in the game seems to be a major motivator for not reporting symptoms. Being embarrassed in front of their friends appears to contribute to the difficulty athletes experience when it comes to reporting a concussion. A lack of knowledge regarding the signs, symptoms, and/or an inability to recognize a concussion may contribute to the lack of reporting. Studies have acknowledged the positive impact of education on reporting.Reference Taylor and Sanner18,Reference Bramley, Patrick, Lehman and Silvis19,Reference Lee, Resch, Han, Miles and Ferrara21
There is some suggestion that athletes should not participate in tackle football until the age of 18 to account for the degree and importance of brain development occurring before then. There may be room for further investigation in the high school athlete’s capacity to project forward the potential long-term consequences of severe or repetitive concussions and decisions to hide symptoms and return to play when still symptomatic.
Canadian high school athletes, in particular, are of interest given that they are not normally supported by medical personnel as a regular part of their team. Pryor reported that 70% of US high schools offer on-site athletic training services.Reference Pryor, Casa and Vandermark24 Only 37% of the athletic trainers in this study are full time. This limits comprehensive coverage for games and practices. Only one private high school in Manitoba hires a full-time athletic therapist. The Manitoba High School Football Association hires certified athletic therapists to be on-site for high school football games. Future consideration should be given to including athletic therapists either full or part time as part of the teaching faculty in Manitoba high schools.
Governments in Canada are increasingly becoming more aware of the impact of SRCs in youth.Reference Bryan, Rowhani-Rahbar, Comstock and Rivara6,7,25–27 A national strategy is being funded by the Federal government and the Province of Ontario as enacted the Rowan’s Law. Manitoba has tabled similar legislation that calls for more education and medical oversight to prevent and manage concussions. Insights to the incidence, awareness, and reporting tendencies of high school athletes will better inform the implementation of the law when it is enacted in Manitoba.
Conclusions
The prevalence of SRCs in Manitoba high schools warrants more attention. Educating athletes regarding the signs and symptoms especially the cognitive and emotional symptoms may reduce the prevalence of returning to play with concussion symptoms or the lack of reporting to medical professionals or coaches. Coaches and attending medical professionals should be aware of the predisposition to hide the symptoms. More than half of the concussions in this study went unreported in both game and practice situations. Athletes need to be better educated regarding the importance of reporting. Coaches and team medical staff must be trained to be vigilant for the mechanism, signs, and symptoms of injury in both game and practice situations. The Manitoba Concussion Youth Act27 proposes to require a medical assessment by a physician or nurse practitioner for all youth who sustain a concussion. This will provide the opportunity to educate the athlete on the pathological process of recovery, the importance of full recovery, and future preventative strategies. Return to play protocols should be emphasized to prevent early return while still symptomatic. The stigma associated with concussions should be addressed with athletes to overcome the embarrassing feelings that negatively affect the propensity to report a concussion.
Disclosures
The author has no conflicts of interest to declare.
Acknowledgements
The author would like to acknowledge the contributions of Jessica Thomas, Pamela Ryczko and Ashley Phommarath for their assistance in conducting the pilot questionnaire, athlete surveys and data collection.












