The articles by Geddes & Wessely (Reference Geddes and Wessely2000, this issue) and Lelliott (Reference Lelliott2000, this issue) describe the current evidence base and guidelines from which clinical standards can be developed in mental health. They highlight some of the issues and complexity surrounding the development of standards. It could be argued, however, that an even greater challenge lies in getting clinical standards used in routine practice.
The current policy direction (indicated, for example, by National Service Frameworks, clinical governance and professional revalidation) is towards greater standardisation of practice. The implementation of clinical standards and guidelines will, therefore, increasingly become an issue which medical and clinical directors will need to address.
Where is the evidence?
Much of the research about promoting improvements in health care has drawn on ideas from outside medicine. In practice, the health service has been slow to adopt successful approaches from commerce, an illustration of this is the contrast between the success of pharmaceutical companies in the marketing of their products and the relative failure of professional bodies to promote the uptake of clinical standards (Reference Duffett and LelliottDuffett & Lelliott, 1998).
Fields which have informed current thinking about implementation of clinical standards
-
(a) Health service research.
-
(b) Psychology.
-
(c) Education and learning.
-
(d) Sociology.
-
(e) Social policy.
-
(f) Management theory.
-
(g) Marketing.
-
(h) Philosophy.
What is the evidence about approaches to implementing clinical standards?
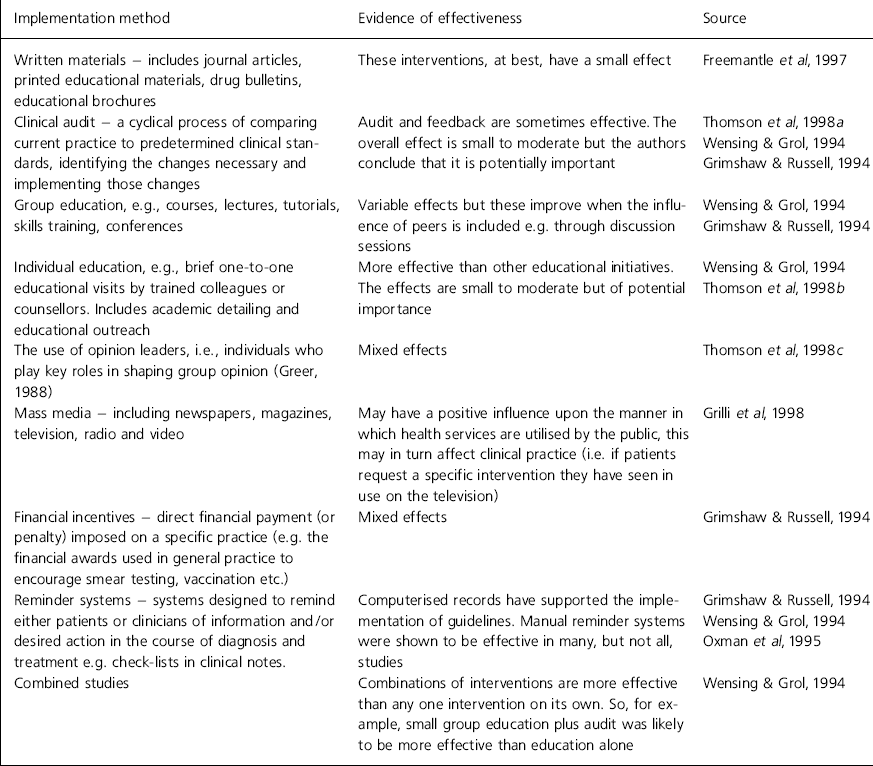
Although it is a relatively new field of inquiry, there is a body of research evidence about what promotes uptake of clinical guidelines and standards. This is summarised in Table 1.
| Implementation method | Evidence of effectiveness | Source |
|---|---|---|
| Written materials - includes journal articles, printed educational materials, drug bulletins, educational brochures | These interventions, at best, have a small effect | Reference Freemantle, Harvey and WolfFreemantle et al, 1997 |
| Clinical audit - a cyclical process of comparing current practice to predetermined clinical standards, identifying the changes necessary and implementing those changes | Audit and feedback are sometimes effective. The overall effect is small to moderate but the authors conclude that it is potentially important | Reference Thomson, Oxman and DavisThomson et al, 1998a |
| Reference Wensing and GrolWensing & Grol, 1994 | ||
| Reference Grimshaw and RussellGrimshaw & Russell, 1994 | ||
| Group education, e.g., courses, lectures, tutorials, skills training, conferences | Variable effects but these improve when the influence of peers is included e.g. through discussion sessions | Reference Wensing and GrolWensing & Grol, 1994 |
| Reference Grimshaw and RussellGrimshaw & Russell, 1994 | ||
| Individual education, e.g., brief one-to-one educational visits by trained colleagues or counsellors. Includes academic detailing and educational outreach | More effective than other educational initiatives. The effects are small to moderate but of potential importance | Reference Wensing and GrolWensing & Grol, 1994 |
| Reference Thomson, Oxman and DavisThomson et al, 1998b | ||
| The use of opinion leaders, i.e., individuals who play key roles in shaping group opinion (Greer, 1988) | Mixed effects | Reference Thomson, Oxman and DavisThomson et al, 1998c |
| Mass media - including newspapers, magazines, television, radio and video | May have a positive influence upon the manner in which health services are utilised by the public, this may in turn affect clinical practice (i.e. if patients request a specific intervention they have seen in use on the television) | Reference Grilli, Freemantle and MinozziGrilli et al, 1998 |
| Financial incentives - direct financial payment (or penalty) imposed on a specific practice (e.g. the financial awards used in general practice to encourage smear testing, vaccination etc.) | Mixed effects | Reference Grimshaw and RussellGrimshaw & Russell, 1994 |
| Reminder systems - systems designed to remind either patients or clinicians of information and/or desired action in the course of diagnosis and treatment e.g. check-lists in clinical notes. | Computerised records have supported the implementation of guidelines. Manual reminder systems were shown to be effective in many, but not all, studies | Reference Grimshaw and RussellGrimshaw & Russell, 1994 |
| Reference Wensing and GrolWensing & Grol, 1994 | ||
| Reference Oxman, Thomson and DavisOxman et al, 1995 | ||
| Combined studies | Combinations of interventions are more effective than any one intervention on its own. So, for example, small group education plus audit was likely to be more effective than education alone | Reference Wensing and GrolWensing & Grol, 1994 |
Communication and marketing
The first step is to ensure the intended audience is aware of the standards. A series of questions are shown below which it may be useful to ask when developing a local or national communications strategy for clinical standards.
Many NHS trusts employ communications officers who are highly skilled in marketing techniques and who may be able to help.
Questions to ask about a dissemination strategy for clinical standards
-
(a) Who needs to know about the standards?
-
(b) Who needs to use them in practice?
-
(c) How will you ensure that everyone who needs to know about the standards will get to hear about them, and how will you know when you have achieved this goal?
-
(d) Who are the ‘gatekeepers’ through which information is channelled (e.g. to get information to staff nurses do you need to go through ward managers?)?
-
(e) Do the standards originate from a credible source, for example, the Royal College of Psychiatrists, National Institute for Clinical Excellence etc.
-
(f) Are there different formats that can be used to make information about the standards more accessible or appealing for different individuals or groups, for example, key bullet points, use of colour, use of graphs etc?
-
(g) Are there different channels that can be used for dissemination, for example, one-to-one situations, during meetings where others may support you, at educational events etc.?
-
(h) What is it about the clinical standards that will be of interest and value to clinicians, managers, the medical director, the continuing professional development lead, the clinical audit team etc.? For example, the potential to: improve patient care, relate to local targets, address an area of personal interest, reduce litigation, save money etc.
Leadership
Change requires leadership and it is important to get the appropriate leaders ‘on board’ early in the process.
Leaders will include a range of people, for example clinical directors, service managers, team leaders, and will vary according to the content of the standards.
As well as people who are leaders through the nature of their job, it is important to consider ‘opinion leaders’, that is, people to whom others listen. These are not necessarily the same people as those in formal leadership positions. Hayward et al (Reference Hayward, Wilson and Tunis1996) found that endorsement of guidelines by a respected colleague is the most important factor affecting whether or not they are adopted by trainee doctors.
Training
The local leaders for training (e.g. clinical tutors, trust training departments, director of continuing professional development etc.) may be a priority target for dissemination in order that they develop training to enable clinicians to understand:
-
(a) the potential benefits of using the clinical standards;
-
(b) how and why the clinical standards were developed;
-
(c) the content of the standards and how it specifically applies to them;
-
(d) what they are being asked to do with the standards;
-
(e) how they can monitor the use of the standards and ensure that they improve patient care.
Once training needs have been identified, the best way to deliver training should be considered (see Table 1).
Peer support (social influence)
People most commonly learn and formulate new opinions through discussion with their peers (Reference Mittman, Tonesk and JacobsonMittman et al, 1992). For example, once a set of clinical standards is introduced to a group of clinicians, it is likely that they will talk to others in their peer group to find out general opinions about the standards before they decide whether to incorporate them into their practice. They will ask each other questions such as:
-
(a) Are the standards valid?
-
(b) Will the standards apply to my work and the patients I see?
-
(c) Will the standards improve patient care, or may they have a harmful effect?
These conversations happen in social groups and are just as likely to occur while taking the lift or over lunch as they are in formal situations. Providing opportunities for discussion, for example, in team meetings, training sessions, is likely to have a beneficial effect on the adoption of clinical standards (and, just as important, prevent the use of potentially harmful standards) (Reference LomasLomas, 1993; Reference GreerGreer, 1994; Reference Kanouse, Kallich and KahanKanouse et al, 1995).
Resource allocation and management
The likelihood of successful implementation increases when resources are made available for dissemination and implementation (Reference RogersRogers, 1983). As well as money, the other resource which is always scarce is time. Stocking (Reference Stocking1985) found that the amount of time ‘product champions’ (local enthusiasts who tend to ‘sell’ ideas to their colleagues) have to spend on disseminating a message directly relates to their level of success.
As well as resourcing the implementation process itself, the content of the clinical standards may also have resource implications. For example, the Royal College of Psychiatrists' guidelines on electroconvulsive therapy (Royal College of Psychiatrists, 1995) require adequate facilities, the provision of an anaesthetist and adequate training of staff.
Practical support: reminder systems and clinical audit
Even the best dissemination and implementation strategy may fail. Clinicians, of all disciplines, are busy people and often work in chaotic and stressful situations. Decisions often have to be made very quickly. In the middle of the night a trainee psychiatrist faced with a potentially violent patient is not going to drop everything and reach for their copy of the Royal College of Psychiatrists' clinical practice guidelines on the Management of Imminent Violence (Royal College of Psychiatrists, 1998). Creativity and planning are needed to make it more likely that clinical standards will be adhered to under such circumstances. ‘Context-specific’ reminders play an important role here.
Examples of reminders used to support the implementation of clinical standards
Clinical standard
Drug X to be used instead of Drug Y.
Reminder: stickers attached to packets of Drug Y kept in medication cupboard on ward, saying ‘Think about using Drug X instead!’.
Clinical standard
Patients with a diagnosis of X to be assessed by an occupational therapist before discharge.
Reminder: Leaflet given to all patients with a diagnosis of X tells the patient that they must see an occupational therapist before discharge.
Patient reminds clinician.
Clinical standard
All patients over 65 to have nutritional status assessed on admission.
Reminder: Computerised clerking-in system produces automatic reminder, triggered by ‘date of birth’ field.
Clinical audit
Clinical audit can be used both as a method for encouraging implementation of clinical standards and as a method of monitoring the extent of implementation. Clinical audit support staff will be valuable allies in this process. In addition, participation in clinical audit has significant ‘Hawthorn Effect’ and this in itself encourages the adoption of clinical standards.
The results from clinical audit must be fed back to the clinicians whose practice is audited in a way which is blame-free and enables them to reflect upon their practice and agree areas for improvement. This may mean that the practice of each clinician as measured against the clinical standards is kept confidential to all except the individual. Alternatively, it may mean presenting feedback to groups of peers, rather than having all grades and disciplines discuss the findings as one large group.
Finally, clinical audit should be used to make the link between the implementation of clinical standards and real improvements in patient care and/or outcomes. Feeding this information back to clinicians will create further incentive to use the standards.
Recognition and reward
Most feedback to clinicians and NHS staff is negative - complaints, critical incidents, prescribing errors, lateness arriving at clinics etc. This can be both demoralising and demotivating and runs counter to the principles of quality management applied in successful commercial companies. Recognising and acknowledging achievements can, in contrast, be motivating and uplifting for staff.
Recognising that clinicians have made an effort to implement standards, achieved improvements in practice as demonstrated through clinical audit, or learn something new can be achieved through individual performance reviews, during team meetings, through the trust newsletter, formal award ceremonies etc. In the same way, managers and others should be recognised for the support they give to the process for example by making resources available, giving up some of their time, helping with communications etc. It often takes very little to say ‘well done’ and it can go a long way to predisposing clinicians and others to implement clinical standards in the future.
Comment
Implementing clinical standards is not a linear process of ‘information provision=implementation’. It is not even as simple as ‘information+training+resources=implementation’. It is a complex and ‘messy’ process. An individual implementation method, or even combination of methods, may work for one individual or group but not another. It appears from the research in this area that the best implementation strategy is one which uses a wide range of different approaches in the hope that it will provide something which works for the maximum number of people.
A wide range of methods have been used to implement information within health services, including clinical standards and guidelines, from which some useful messages arise:
-
(a) Ensure people know about the clinical standards.
-
(b) Use as many different channels for information as possible, for example, written information, presentations, reminders in clinical notes, discussion in meetings, use of information technology systems.
-
(c) Consider how different types of channels and settings can be used, for example, educational, administrative/organisational, social, clinical (such as ward handovers, ward rounds, clinical meetings, audit meetings).
-
(d) Consider the presentation of the key messages and how these messages can be ‘sold’ to the different audiences for the clinical standards.
-
(e) Be imaginative about format - catch people's eye, use formats that are familiar to them etc.
-
(f) Promote the credibility of the source of the clinical standards.
-
(g) Target leaders and individuals (or groups) who have influence over how others think and act (i.e. ‘opinion leaders’).
-
(h) Ensure that resources and training are available - at the very least there must be sufficient to enable clinicians to use the clinical standards.
-
(i) Provide opportunities for peer support and social influence.
-
(j) Consider the use of practical support mechanisms such as reminders and clinical audit.
-
(k) Remember to recognise the efforts and achievements of individuals and groups.




eLetters
No eLetters have been published for this article.