INTRODUCTION
In April 2009, a novel influenza virus, influenza A(H1N1)pdm09, was identified in Mexico and the USA, and spread worldwide to become the first pandemic of the 21st century [Reference Dawood1]. The estimated global death toll was more than 284 000 and the cumulative symptomatic attack rate was highest in children aged 0–17 years, ranging from 4% to 33% [Reference Dawood2]. The number of paediatric deaths in children in the USA was four times that recorded in the previous five influenza seasons [Reference Cox3]. Children with underlying metabolic and neurological conditions were identified as being at highest risk for severe complications [Reference Stein4].
In Ireland, two waves of influenza activity occurred between April 2009 and May 2011: one wave during the pandemic period (2009/2010) and one post-pandemic wave in the 2010/2011 season. The first wave began in July and August 2009, 14 weeks after the first case of influenza A(H1N1)pdm09 was confirmed in Ireland in May 2009. This wave began with relatively low levels of influenza activity, with sentinel General Practitioner (GP) influenza-like illness (ILI) consultation rates increasing above baseline levels between mid-July and August 2009. During this initial increase in activity, the majority of cases were in teenagers associated with outbreaks in residential summer language camps. The Irish school holidays in July and August may have limited further spread among children and thus hospitalizations in children during this time. Influenza activity increased significantly with the return to school in September 2009 and peaked during mid-October 2009. During this pandemic wave the peak age-specific ILI rates occurred in children aged 5–9 and 10–14 years in mid-October 2009. The post-pandemic wave occurred between December 2010 and February 2011 and was characterized by a short sharp rise and fall in influenza activity. This wave was associated with higher numbers of critical care admissions and influenza-associated deaths.
In Ireland, during the pandemic period, antiviral therapy (AVT) was recommended for all children with ILI who were either: aged <5 years, or hospitalized with their illness, or with underlying predisposing medical conditions. This advice continued during the 2010/2011 season, and was actively promoted via guidelines and clinical algorithms provided to GPs and emergency departments.
Pandemic vaccination became available in early November 2009. Initially children in risk groups defined by the National Immunisation Advisory Committee (NIAC), and those aged <5 years were vaccinated. Subsequently all other children were offered vaccination in schools, clinics or general practice settings [5]. During the 2010/2011 influenza season, vaccination was recommended for children in the NIAC risk groups. The risk groups were expanded in the 2010/2011 season to include children with any condition that could compromise respiratory function (e.g. spinal cord injury, seizure disorder, or other neuromuscular disorder) especially those attending schools/day centres for children with intellectual and/or physical disabilities.
International papers have compared A(H1N1)pdm09 in children with previous seasonal influenza viruses, and found that influenza A(H1N1)pdm09 affected an older age group and those with a history of asthma and chronic disease, particularly neurological and metabolic conditions [Reference Libster6–Reference Engelhard8]. There is, however, limited literature comparing the A(H1N1)pdm09 pandemic with the subsequent 2010/2011 influenza season [Reference Bolotin9–Reference Altmann11].
The objectives of this paper are to describe influenza A(H1N1)pdm09 in hospitalized children during the pandemic in Ireland and compare it to circulating influenza viruses during the 2010/2011 season; and to identify risk factors for severe influenza in children, defined as admission to a paediatric intensive care unit (PICU).
METHODS
Data collection
In April 2009, enhanced surveillance was undertaken on all cases of confirmed influenza A(H1N1)pdm09 in children aged ⩽14 years deemed to require admission to hospital for management of their condition. All laboratory-confirmed cases of influenza in Ireland were notified to regional departments of Public Health, and for each case notified, they established whether the person had been hospitalized. Regional departments of Public Health or the treating hospital clinician completed the enhanced surveillance form on hospitalized cases. Data collected included demographic details, pre-morbid medical conditions, AVT, length of hospital stay (LOS), admission to PICU, and outcome [Reference Cullen12]. Data were checked by departments of Public Health for completeness and cases identified with missing or inconsistent data were followed up and the information was corrected. Surveillance and laboratory information was entered into the Irish Computerized Infectious Disease Reporting system (CIDR). For those children admitted to a PICU, intensive-care staff completed an additional form on admission and discharge from the PICU. This included information on medical interventions, complications and clinical outcome while in the PICU.
Epidemiological studies and study period
Influenza A(H1N1)pdm09 cases by time, place, and person were described. A retrospective cohort study was conducted to identify risk factors for PICU admission.
Two study periods were compared and analysed; the pandemic [week 17 (2009) to week 32 (2010)] and the 2010/2011 influenza season [week 40 (2010) to week 20 (2011)].
Laboratory methods
Ireland's Health Service Executive (HSE) recommended that all children admitted to hospital with ILI be tested for influenza. The majority (84·2%) of specimens were tested at the National Virus Reference Laboratory for influenza A and B using multiplex reverse transcription polymerase chain reaction (RT–PCR) [Reference Carr13]. Influenza A-positive specimens were further subtyped using multiplex RT–PCR. A small percentage (15·8%) of samples were tested in three other sites, using either in-house real-time RT–PCR assays, or Prodesse ProFlu™+ and Prodesse ProFAST+; or an in-house uniplex system for influenza A. A small proportion of influenza A-positive specimens were not subtyped (23/665, 3·4%).
Analysis of data
Confirmed influenza age-specific hospitalization rates per 100 000 population were calculated. Population data were taken from the Irish 2011 Census.
Descriptive, univariate and multivariate analyses were conducted using SPSS version 16.0 (SPSS Inc., USA) and Stata version 12.0 (StataCorp., USA). In the univariate analysis we calculated proportions, means and medians for each study period. We used Student's t test to analyse differences in normally distributed continuous variables and non-parametric Mann–Whitney and Kruskal–Wallis methods for comparison of skewed data. The χ 2 or Fisher's exact test were used to compare categorical variables between groups. For the multivariate analysis we used a log-linear model with log-link function and a Poisson distribution to obtain adjusted risk ratios. We performed two different models: one to assess risk factors for being admitted to a PICU during each period separately, and the second to observe the effect of the number of medical conditions on the risk of PICU admission for both study periods. Age, gender and any variables with P values <0·25 in the univariate analysis were added to the model and a backward variable selection procedure was used for both models [Reference Hosmer and Lemeshow14]. Non-typed and H3N2 influenza A were excluded from the model and the use of AVT was not included, as we did not have information on timing of use.
Ethical approval
Ethical approval was not required for the collection of these data, as it was part of national surveillance conducted under the Infectious Disease Regulations, 1981 as amended [15].
RESULTS
Age-specific hospitalization, PICU and mortality data
Table 1 provides age-specific hospitalization, PICU and mortality rates per 100 000 population for each season. Overall, the age-specific hospitalization and PICU rates decreased with increasing age in each period. There was a shift in the age-specific hospitalization and PICU admission rates towards the younger age group (<1 year) during the 2010/2011 season.
Table 1. Age-specific, hospitalization PICU admission and mortality rates (per 10 000 population) for laboratory-confirmed cases, by pandemic period and 2010/2011 influenza season, Ireland
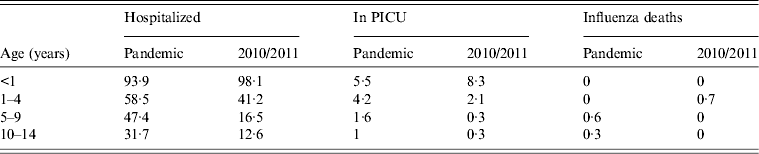
PICU, Paediatric intensive care unit.
Rate calculated using Central Statistics Office Population Census, 2011.
Descriptive analysis
Table 2 compares the pandemic period and the 2010/2011 influenza season in hospitalized children. Children hospitalized with confirmed influenza during the pandemic period were older and were treated more frequently with AVT compared to those in the 2010/2011 season. There was no significant difference in the likelihood of treatment with AVT by age during the pandemic period. However, during the 2010/2011 season (using the <1 year age group as reference), only children aged 10–14 years were 1·6 times more likely to receive AVT (P = 0·034, 95% CI 1·09–2·35).
Table 2. Demographic characteristics, length of stay in hospital, outcome, and underlying medical conditions in hospitalized children and children in PICUs, by period in Ireland
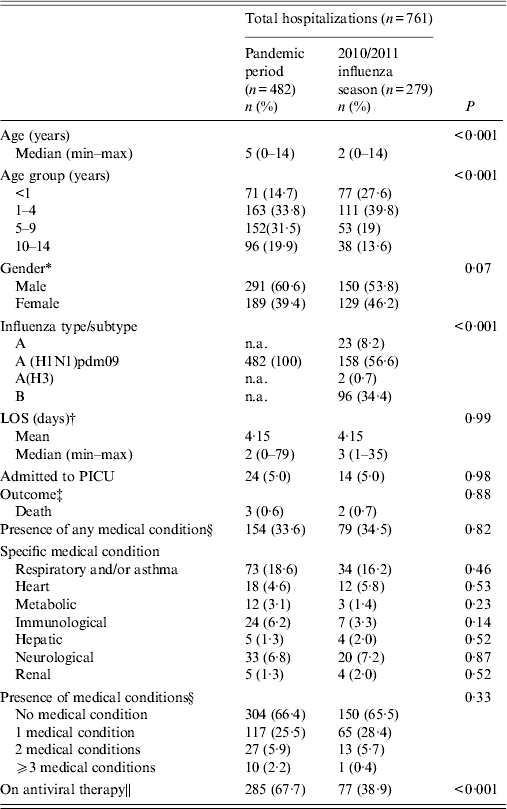
PICU, Paediatric intensive care unit; n.a., not applicable; LOS, length of stay.
* n = 480 for total hospitalizations in the pandemic period.
† n = 480 for total hospitalizations in the pandemic period and n = 217 for total hospitalizations in the 2010/2011 influenza season.
‡ n = 378 for total hospitalizations in the pandemic period and n = 277 for total hospitalizations in the 2010/2011 influenza season.
§ n = 458 for total hospitalizations in the pandemic period and n = 228 for total hospitalizations in the 2010/2011 influenza season.
|| n = 18 for PICUs in the pandemic period and n = 11 for PICUs in the 2010/2011 influenza season.
There was a significant association between increasing age and the presence of underlying medical conditions in both the pandemic period and the 2010/2011 season (Table 3).
Table 3. Relationship between (a) age and presence of underlying medical conditions, or (b) being on antiviral therapy, for all hospitalized children during the pandemic period and 2010/2011 influenza season, Ireland
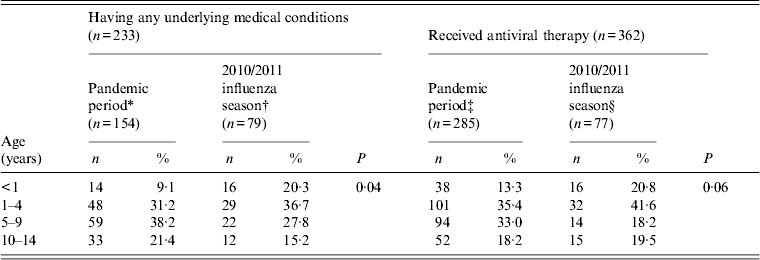
* The P value for differences of having medical conditions in age groups within the pandemic period is P = 0·02.
† The P value for differences of having medical conditions in age groups within the 2010/2011 influenza season is P = 0·02.
‡ The P value for differences of having received antiviral therapy in age groups within the pandemic period is P = 0·56.
§ The P value for differences of having received antiviral therapy in age groups within the 2010/2011 influenza season is P = 0·09.
Vaccination status was only available for PICU admissions during the 2010/2011 influenza season. Information on vaccine uptake was not available for the hospitalized population in general. In the 2010/2011 season, of the 14 children admitted to ICUs, 11 were aged >6 months. Of these 11, eight had underlying medical conditions, and therefore were in risk groups for seasonal flu vaccination. Only one (12·5%) of these children had been vaccinated. This child had also not received pandemic vaccination. Six of the 11 children had also been eligible for pandemic vaccination. Of the six children aged ⩾2 years at onset of illness during the 2010/2011 season, three (50%) had received pandemic vaccine.
PICU clinical course and outcome
In the analysis of all children admitted to PICUs in both study periods; 29 (76·3%) underwent mechanical ventilation, 19 (51%) had acute respiratory distress syndrome (ARDS) and two (5·6%) had acute kidney injury. Complications included primary influenza viral pneumonia in 29 (80·6%), secondary bacterial pneumonia in eight (22·2%) and sepsis/multi-organ failure in four (11·1%). No child required extracorporeal membrane oxygenation (ECMO) and no child developed myocarditis or encephalitis. The median LOS in PICU was 7 days, and three (8·6%) patients admitted to a PICU died. There was no significant difference in the clinical course and outcome between children with and without underlying risk factors.
Effect of the number of medical conditions on risk of PICU admission
Both univariate and multivariate analysis showed that the risk of being admitted to a PICU increased with the number of underlying conditions present (Table 4). After adjustment by age and gender, the risk of PICU admission during the pandemic period was 4·8, 10·91 and 73·12 times higher in children that had one, two, and three or more medical conditions, respectively. The increase in risk with the number of underlying conditions present was similar in the 2010/2011 season.
Table 4. Univariate and multivariate analysis of the effect of the number of medical conditions on risk of PICU admission, for hospitalized children during the pandemicperiod and 2010/2011 influenza season (n = 687), Ireland
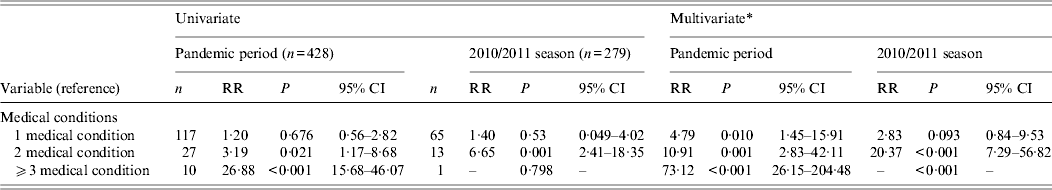
PICU, Paediatric intensive care unit; RR, risk ratio; CI, confidence interval.
* Adjusted by age and gender.
Risk of PICU admission
Table 5, shows that during the pandemic, the risk of PICU admission was lower in males and higher in those with respiratory conditions/asthma, heart conditions, immunological or renal conditions. Some of the numbers affected with these conditions were, however, quite small. Age was not a risk for PICU admission during the pandemic. In the 2010/2011 influenza season, influenza A(H1N1)pdm09 emerged as a risk factor for PICU admission, with the risk of admission being seven times higher with A(H1N1)pdm09 than with other flu strains. The majority of these were influenza B (Table 2). The risk of admission was also raised in those with neurological or metabolic conditions. There was no increased risk associated with age or gender.
Table 5. Univariate and multivariate analysis of risk factors for PICU admission for hospitalized children, by period, Ireland
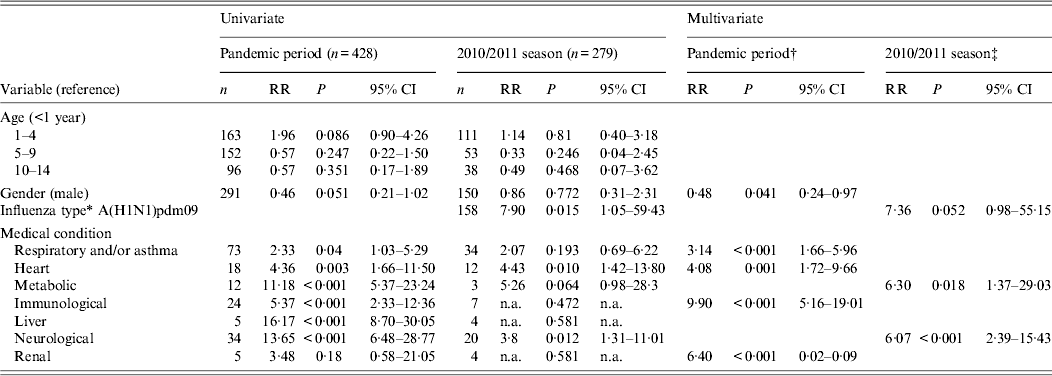
PICU, Paediatric intensive care unit; RR, risk ratio; CI, confidence interval; n.a., not applicable.
* Results only for the 2010/2011 influenza season, because the pandemic period had only had one type of influenza.
† Variables taken out from the log-linear model for the pandemic period were: age, metabolic, liver and neurological conditions.
‡ Variables taken out from the log-linear model for the 2010/2011 season were: age, gender, respiratory and/or asthma, heart, metabolic, immunological and liver conditions.
DISCUSSION
This is the first detailed comparison of influenza during the pandemic period and the 2010/ 2011 season in hospitalized children in Ireland. As there is a national enhanced surveillance system in place, age-specific hospitalization, PICU, and mortality rates could be calculated.
In Ireland during the pandemic, children were affected disproportionately, with relative sparing of the older population, similar to findings elsewhere [Reference Dawood2]. The 2010/2011 influenza season was shorter but more intense than the pandemic, with a slightly higher overall ILI rate and significant pressure on adult ICUs [Reference Domegan16]. In children the age-specific ILI rates were much lower during the 2010/2011 season, but still higher than those recorded in influenza seasons prior to the pandemic. The age-specific hospitalization and PICU admission rates were lower for all ages with the exception of children aged <1 year. The lower impact in children during the 2010/2011 season may reflect the effect of interventions such as vaccination, as well as exposure to A(H1N1)pdm09 in the paediatric population. Unfortunately, there are no Irish seroepidemiological data which could confirm this. In Ireland, pandemic-specific vaccination uptake was high in children (61·5% in those aged 0–4 years and 53·1% in those aged 5–14 years) [Reference Cotter17].
Our pandemic hospitalization data showed similarities with other countries: the median age (5 years) of children hospitalized was similar to that found in large studies in Canada and Korea, but slightly lower than that found in Japan [Reference Bettinger18–Reference Kobayashi20]. The proportion (34%) with underlying medical conditions was lower than that seen in some countries, e.g. 43% in Germany, and 42% of cases in Australia [5, Reference Larcombe21], but in line with or higher than other large population-based studies (32% in the USA, 27·5% in Madrid and 22·4% in Korea) [Reference Libster6, Reference Ko22, Reference Del23].The proportion of hospitalized children requiring PICU admission was low at 5% when compared with that found in Canada and Argentina at 16·8% and 19% respectively, but similar to Australia at 4·6% [Reference Libster6, Reference Larcombe21, Reference O'Riordan24, Reference Tran25]. It has been noted in previous analyses that Irish data are similar in demographics, admission rates and bed occupancy to those in Australia and New Zealand [Reference Nicolay26]. However this may also reflect different thresholds for admission to a PICU. There were more males than females hospitalized in Ireland during the pandemic, as was found in many other studies [Reference Costello19, Reference Wieching27, Reference Çiftçi28]. LOS was similar during the pandemic period and the 2010/2011 season, and also similar to that found in other studies [Reference Stein4, Reference Tran25].
The presence of medical conditions increased with age, apart from the older age group (10–14 years). This was also found in Germany by Altmann et al. in his study of children admitted to PICUs, and by Bettinger et al. in Canada, who found that a third of hospitalized children aged <2 years had at least one medical condition vs. 72% in older children [Reference Bettinger18, Reference Altmann29].
Significant differences were observed in the age of those hospitalized between both periods. Post-pandemic, hospitalized children were younger. A sentinel surveillance system for severe influenza in England found that in hospitalized children there was a shift away from the 5–14 years age group in the post-pandemic season, and an increase in the rate of hospitalization in children aged 0–4 years, with a trend of decreasing hospitalization rates with increasing age in both periods [Reference Bolotin9].
Other studies comparing pandemic influenza with previous seasons have found that children admitted with influenza A(H1N1)pdm09 were older than those admitted with seasonal influenza A in the years prior to the pandemic [3, 7, 8, 26, 30–33]. Apart from age, no other differences were found in hospitalized and PICU cases during the pandemic period and the 2010/2011 season. This was a similar finding to a Canadian study which also found no differences in the proportions requiring PICU admission or in the mortality rates [Reference Tran25].
Unfortunately, we found an extremely low vaccination uptake in children at high risk in the 2010/2011 season. Only one child in a PICU of those eligible for vaccination had been vaccinated. A similar pattern was seen with fatal cases in the USA during the 2010/2011 season [33]. Of 74 children who died aged ⩾6 months, and in whom vaccination records were available, 39 had high-risk conditions and only one third of these had been vaccinated.
Antivirals were used more frequently during the pandemic than in the 2010/2011 season. This is of concern, as the same recommendations for use were made during both influenza seasons, i.e. to treat all those sick enough to be hospitalized with antivirals. They were promoted strongly to GPs, consultants in emergency medicine, and paediatricians. This has also been found elsewhere. In the USA, the use of antivirals in hospitalized children also fell from 77% to 56% in the post-pandemic season [Reference Garg34]. In our study, when use of antivirals was compared by age group, an increase was seen in their use in those aged <5 years in the 2010/2011 season vs. the pandemic period, whereas in older children, they were less used. This may reflect a welcome heightened awareness of the risk of influenza in younger children, but highlights the need to re-emphasize the benefits of AVT in all hospitalized children.
We were able to identify and compare risk factors for PICU admission with influenza during the pandemic period and the 2010/2011 season. During the pandemic, the risk of PICU admission was higher in female children, and in those with underlying medical conditions. This finding of female predominance is in contrast to previous published studies showing male predominance of severe disease associated with influenza A(H1N1)pdm09 [Reference Xu35, Reference Choi36]. This was not explained by a higher incidence of medical conditions in girls. Age group was not a risk factor for PICU admission. A comparison of pandemic with prior seasonal influenza showed similar findings [Reference Morris7].
During the 2010/2011 season the risk of PICU admission was higher in those with influenza A(H1N1)pdm09, and in those with underlying medical conditions, but was not higher in females. In a study on seasonal influenza subtypes in children, it was found previously that disease due to influenza A(H3N2) was significantly more severe than that due to influenza A(H1N1) and influenza B [Reference Esposito37]. Our findings provide evidence that disease due to influenza A(H1N1)pdm09 is also more severe than that due to influenza B. We also demonstrated a clear incremental relationship between the number of underlying medical conditions and the risk of PICU admission with influenza.
There are some limitations to this study. Not all hospitalized children with influenza might have been clinically suspected or tested and identified, and so the true numbers may be underrepresented. There were some limitations to the data collected. We were unable to capture data on the timing of administration of antivirals, and so we were unable to assess whether the use of antivirals affected risk of PICU admission. The data on respiratory conditions and asthma were not sufficiently detailed to allow us to separate them into discrete categories. The numbers overall in PICUs were small, and this limited our analysis.
CONCLUSIONS AND RECOMMENDATIONS
In a large national population-based surveillance system, the epidemiology of influenza A(H1N1)pdm09 was described and contrasted with subsequent seasonal influenza. Risk factors for severe illness in hospitalized children with influenza were identified, including the fact that having influenza A(H1N1)pdm09 subtype is a risk factor for PICU admission.
The significantly increased risk of a serious episode of illness in those with underlying conditions, and also the incremental relationship between the number of medical conditions present and the risk of a severe episode present powerful evidence of the importance of targeting vaccination programmes to children with complex underlying medical conditions. These findings should be used to influence and encourage vaccination in these extremely vulnerable groups. The findings also reinforce the importance of using antivirals in these children.
The use of AVT in all hospitalized children should also be promoted, with a focus not only on young children, but also those aged >5 years, given our findings.
This study demonstrates that the collaborative efforts of clinicians, intensivists, GPs, public health and surveillance staff in surveillance activities can yield significant new information for action and response.
ACKNOWLEDGEMENTS
We thank Ajay Oza for his work on the database for patients admitted to PICUs, and enabling us to merge this dataset with the national Computerized Infectious Disease Reporting system (CIDR). We thank Sylvanus Fonguh from the Belgian Scientific Institute of Public Health for his advice regarding statistics. We thank staff in departments of Public Health, Paediatric Intensive Care Units, General Practitioners in the sentinel GP surveillance scheme, the Irish College of General Practitioners, the National Virus Reference Laboratory, University College Galway, Cork University Hospital, and staff at the Health Protection Surveillance Centre for their contribution to surveillance.
DECLARATION OF INTEREST
None.







