Gluten is a mixture of proteins, gliadin and glutenins, found in wheat, barley and rye(Reference Elli, Branchi and Tomba1). Wheat, the world’s primary source of food in both developed and developing countries, is the prime source of gluten intakeReference Tovoli, Masi and Guidetti(2). In addition to wheat-based foods, gluten is now massively used by food industries, especially baking industries, as an ingredient in other products. Indeed it has the ability to retain air in the protein matrix, facilitating baking and improving texture and volume of ultra-processed products(Reference Parada and Araya3, Reference San Mauro Martín, Garicano Vilar and Collado Yurrutia4). Thus, gluten is abundantly consumed in the diet. However, recently, more and more people avoid gluten. Originally, gluten avoidance is the only treatment for coeliac disease (CD). CD is an autoimmune inflammatory disorder estimated to affect an average of 1 % of the Western population(Reference Fasano, Berti and Gerarduzzi5). It causes, in genetically susceptible people, damage to the absorptive villi of the duodenum, which leads to malabsorption of important nutrients(Reference Lebwohl, Sanders and Green6). However, in the past decade, avoidance of gluten has occurred outside the diagnosis of CD(Reference Aziz, Lewis and Hadjivassiliou7, Reference Rubio-Tapia, Ludvigsson and Brantner8). For example, in New Zealand, a study has reported that 5 % of children avoided gluten whereas 1 % had a CD(Reference Tanpowpong, Ingham and Lampshire9). Besides, a US study showed that among the people following a gluten-free diet (GFD), only 18 % had been diagnosed with CD, and 6 % with non-coeliac gluten sensitivity (NCGS)(Reference Sapone, Bai and Ciacci10). NCGS is a disorder characterised by intestinal and extra-intestinal symptoms occurring after the ingestion of gluten(Reference Elli, Branchi and Tomba1). Contrary to CD, no sensitive and specific biomarkers have been identified for this disorder, and a lot of people self-reported NCGS without medical diagnosis.
The majority of people following a GFD are therefore likely healthy people leading to the explosion of the gluten-free market(Reference Elli, Branchi and Tomba1, Reference Igbinedion, Ansari and Vasikaran11–Reference Gaesser and Angadi13). Indeed, market of gluten-free products showed an annual growth rate of 34 % between 2009 and 2014 and 10·4 % between 2014 and 2019 in the USA and Europe, respectively(Reference Elli, Branchi and Tomba1, Reference Igbinedion, Ansari and Vasikaran11). The number of people who avoid gluten is very large and varies, according to the studies and the geographic locations, between 3·7 % and 17·2 %(Reference Aziz, Lewis and Hadjivassiliou7, Reference Ontiveros, López-Gallardo and Vergara-Jiménez14–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18). Of the few studies that examined gluten avoidance in the general population, most of them focused on the motives and the symptoms related to gluten ingestion. These studies reported that people avoiding gluten were more likely to be women, with other food intolerances like lactose(Reference Ontiveros, López-Gallardo and Vergara-Jiménez14–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18). Regarding the motives underlying gluten avoidance, the most common reported were weight control, perception that it is healthier and symptoms triggered after gluten ingestion(Reference Cabrera-Chávez, Granda-Restrepo and Arámburo-Gálvez16–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18). These studies(Reference Cabrera-Chávez, Granda-Restrepo and Arámburo-Gálvez16–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18) reported that people without CD who avoid gluten included healthy persons and persons that considered themselves to be suffering from NCGS.
The majority of consumers who avoid gluten perceived gluten-free products more healthful than their gluten-containing counterparts(Reference Gaesser and Angadi13, Reference Dunn, House and Shelnutt19). However, no medical evidence suggests that the general population would be better off by excluding gluten from their diet(Reference Gaesser and Angadi12, Reference Marcason20). In addition, this diet may result in nutritional consequences because gluten-free foods contain more energy, carbohydrates, Na and lipids and less protein than their gluten-containing equivalents(Reference Miranda, Lasa and Bustamante21). However, very few studies examined the nutritional characteristics of people without CD avoiding gluten and these provided inconsistent findings(Reference DiGiacomo, Tennyson and Green22–Reference Devlin25).
As many other countries worldwide, French dietary integrate mainly wheat-based products. Thus, our aim was to estimate the prevalence of gluten avoidance in French non-coeliac adults, as well as the motives for avoidance. Furthermore, we sought to compare demographic and nutritional characteristics between people who avoid gluten and those who do not avoid it.
Materials and methods
Study population
Participants were selected from the NutriNet-Santé study, a web-based observational prospective open cohort study launched in France in May 2009, including internet-using adult volunteers aged 18 years and older(Reference Hercberg, Castetbon and Czernichow26). The NutriNet-Santé study aims to investigate the relationship between nutrition and health, as well as the determinants of dietary behaviours and nutritional status. At baseline, participants completed a set of self-administered questionnaires about socio-economic conditions and lifestyle, health status, diet, physical activity and anthropometrics characteristics. These data are yearly updated. Moreover, during follow-up, additional and optional questionnaires are regularly proposed on various aspects of dietary behaviours and health.
Ethics
The NutriNet-Santé study is conducted in accordance with the Declaration of Helsinki and was approved by the ethics committee of the French Institute for Health and Medical Research (Inserm institutional review board no. 0000388FWA00005831) and the National Commission on Informatics and Liberty (CNIL nos. 908450 and 909216). All subjects provided their informed consent with an electronic signature. This study is registered in EudraCT (no. 2013-000929-31) and in ClinicalTrials.gov (NCT03335644).
Data collection
Definition of participants avoiding gluten
An optional questionnaire was sent to 121 266 participants of the cohort on 9 September 2016 and was available for completion over a 4-month period. Information on food exclusions and their motives were asked. The questionnaire included three parts: self-reported exclusion of eighty-three types of foods, specific diets with their motivations and allergies. Participants were asked the following question: ‘Do you exclude products containing wheat/barley/rye/oats (gluten) from your diet?’ and the responses were ‘yes totally/yes partially/no’. Thus, participants were classified into three groups: total avoiders, partial avoiders or non-avoiders.
Participants reported a CD as they answered ‘yes’ to the question ‘Do you have a coeliac disease?’ and that they reported a medical diagnosis or other type of ‘diagnosis’ answering the following question ‘Was it diagnosed by a general practitioner, a specialist, a dietitian?’
Sociodemographic and lifestyle data
Demographic, socioeconomic and lifestyle characteristics were collected upon enrollment and each year thereafter. The baseline questionnaires were compared against traditional assessment methods(Reference Touvier, Méjean and Kesse-Guyot27). These characteristics included sex, age, marital status, household composition, number of children, geographical region, education level, occupational category, income, smoking status and physical activity. Monthly household income was divided by consumption unit (CU), where one CU was attributed for the first adult in the household, 0·5 CU for other individuals aged 14 years or older, and 0·3 CU for children under 14 years, following national statistics methodology and guidelines(28). Physical activity was assessed using a short form of the French version of the International Physical Activity Questionnaire(Reference Hagströmer, Oja and Sjöström29). BMI (in kg/m2) was calculated as the ratio of weight to squared height and then classified following the WHO guidelines(30).
Dietary data
At baseline and every 6 months, participants were invited to complete web-based, self-administered 24-h dietary records using validated tools(Reference Touvier, Kesse-Guyot and Méjean31, Reference Lassale, Castetbon and Laporte32). These records were randomly assigned over a 2-week period, on three non-consecutive days (two weekdays and one weekend day). Participants reported all foods and beverages consumed at each eating occasion, as well as portion sizes according to photographs from a validated picture booklet(Reference Le Moullec, Deheeger and Preziosi33). The values for energy, macro- and micronutrients were estimated using a published nutrient database, completed for recent market foods and recipes. The modified Programme National Nutrition Santé Guidelines Score (mPNNS-GS), that reflects adherence to the French dietary recommendations(Reference Estaquio, Kesse-Guyot and Deschamps34) (maximum value = 13·5, reflecting the highest level of adherence to the French dietary guidelines), was calculated. Reported foods and beverage items have been reduced to eighteen food/beverage groups: fruits, vegetables, legumes, potatoes and other tubers, meat, fish and seafood, processed meat (and fish), whole starchy foods, refined starchy foods, breakfast cereals, dairy products, eggs, added fats (including butter, margarine, sauces), oils, salty/sweet and fatty foods, sugary drinks, sugar-free drinks and alcoholic beverages.
Statistical analysis
For the present analysis, we selected participants who had completed at least three 24-h dietary records during the 2-year period preceding the food exclusions questionnaire. Thus, the analysis included all the records made in the 2 years preceding the questionnaire (mean 7·65, sd 3·69). People reporting a CD were excluded as well as those with missing data on the covariates and living overseas.
To adjust our sample to the actual percentage in the French population, weighting was calculated for each sex via the SAS CALMAR (CALage sur MARges) macro developed by the Institut National de la Statistique et des Etudes Economiques (INSEE)(35) based on the following information: sex, age, educational level, occupational categories, marital status and geographical area of residence. All analyses were weighted according to this CALMAR macro.
First, description of sociodemographic characteristics between total avoiders, partial avoiders or non-avoiders was performed and P values referred to χ 2 tests or ANOVA. Comparison of the eighteen food group consumptions and nutrients intake between the three groups was also realised. Macronutrients were considered as the percentage of energy intake. Micronutrient intakes were adjusted for energy intake using the residual method(Reference Willett and Stampfer36). Then, adjusted mean for age and sex and 95 % CI from ANCOVA were reported. Food group consumptions were also adjusted for daily energy intake.
A factor analysis, using principal component analysis, was performed to extract dietary patterns (DP) that are independent linear combinations of the eighteen food groups, thereby maximising the explained variance in dietary intake. The number of retained patterns was determined using eigenvalues of each factor, Cattel’s scree test (plot of the total variance related to each pattern) and interpretability of the factors. For each participant, the individual pattern score was calculated by summing the intake of the eighteen food groups that were weighted by their factor loading. Then, the dietary pattern scores were categorised into quintiles to allow better interpretation of the food intake associated with each one the DP obtained.
To assess the association between the exclusion of gluten and each DP (in quintiles), multivariable polytomic logistic regression models were performed. Adjusted OR with their 95 % CI are presented. A first model was minimally adjusted for age (continuous) and sex. The multivariable model was adjusted for age, sex, educational level (no diploma or primary studies/secondary studies/higher educational level), occupational category (nine classes), income level (<1200 € per CU/1200–2300 € per CU/>2300 € per CU), smoking status (never smoker/former smoker/occasional smoker/regular smoker), physical activity (low, moderate, high), number of 24-h dietary records, alcohol and total daily energy intake without alcohol.
All tests of significance were two-sided and a P value <0·0001 was considered significant, given the high number of statistical tests performed and the large sample size. Statistical analyses were conducted with SAS (version 9.4, SAS Institute, Inc.).
Results
Sample selection
From the initial 121 266 subjects who received the questionnaire on food exclusions, a total of 34 781 answered the questionnaire. Within this sample, we excluded participants that reported a diagnosed CD, with missing data regarding the socioeconomic characteristics, living overseas and those with missing data on food intake. The final sample available for analysis included n 20 456 individuals (Fig. 1), of whom 375 declared to be total gluten avoiders, 1661 partial avoiders, and 18 420 non-avoiders. The weighted prevalence rate of respondents who were gluten avoiders was 10·31 %, of which 1·65 % were total gluten avoiders.

Fig. 1. Flowchart of the study.
Sociodemographic and individual characteristics
Sample weighted characteristics are presented according to the gluten avoidance, as well as for the whole sample (Table 1). Compared with non-avoiders, total and partial gluten avoiders were more likely to be women, older people, non-smokers, to have children and lower educational level.
Table 1. Sociodemographic and lifestyle characteristics according to the gluten avoidance after weighting
(Percentages; mean values and standard deviations)
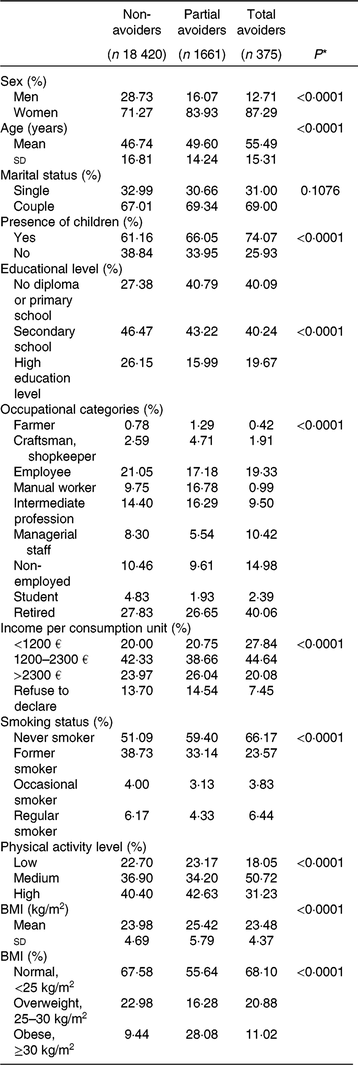
* P values are based on the χ² test or the one-way ANOVA test as appropriate.
Total avoiders are distinguished from partial avoiders: they were more likely to be retired, non-employed or managerial staff than manual worker or self-employed, had lower income and a moderate physical activity. Partial gluten avoiders were more often manual worker, with an intermediate profession or self-employed than employee or managerial staff. They were also more likely to have higher income and to present obesity.
Food choice motives
People avoiding gluten reported more frequently health (physical well-being and belief of a long-term health impact) and taste as their main motive (Table 2). The main motive for participants who were total gluten avoiders was suffering from allergy and/or intolerance. Gluten avoiders were also more likely to follow a lactose-free diet, to exclude other foods and report higher number of allergies (online Supplementary Table S1).
Table 2. Motives (%) for avoiding gluten
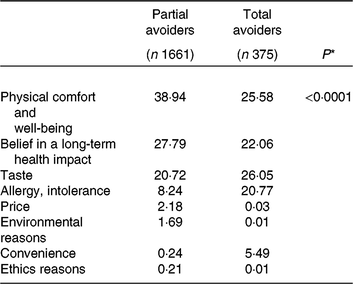
* P values are based on the χ² test.
Food consumptions
Gluten avoiders had a higher consumption of vegetables, fruits, whole starchy food, fish and seafood, eggs and oils, and a lower consumption of refined starchy food, dairy products, salty/sweet and fatty foods and alcohol. A trend was observed from non-avoiders to total avoiders. Potatoes were largely consumed by total avoiders, and legumes and added fats were largely consumed by partial avoiders. Partial gluten avoiders had a lower consumption of meat and sugary drinks, whereas non-avoiders had a higher consumption. Partial and non-avoiders had also higher consumption of processed meat. Regarding the adherence to nutritional guidelines, partial gluten avoiders had the highest mean mPNNS-GS compared with total and non-gluten avoiders (Table 3).
Table 3. Comparisons of mean intakes of eighteen food groups (in g/d) included in the principal component analysis between total, partial and non-gluten avoiders
(Mean values and 95 % confidence intervals)
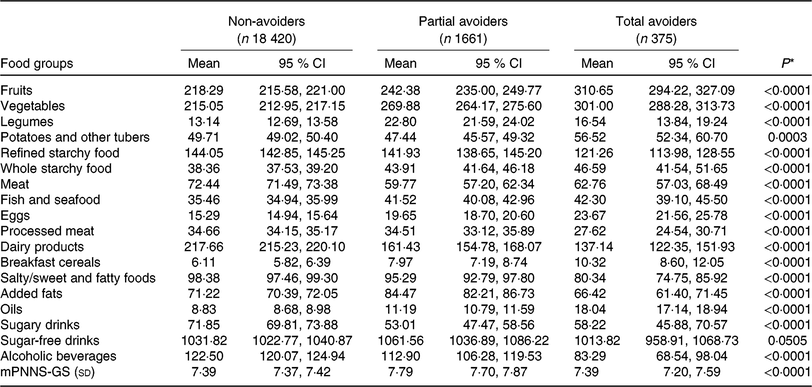
mPNNS-GS, modified Programme National Nutrition Santé Guideline Score.
* P values are based on the ANCOVA test adjusted for total energy intake, age and sex.
Energy and nutrient intake
Total energy intake was lower in participants with total avoidance, whereas it is higher in participants with partial avoidance (Table 4). Gluten avoiders had a lower percent energy from proteins (total avoiders > partial avoiders > non-avoiders) and higher percent energy from fat. They had the lowest mean contribution of SFA to energy intake and the highest for PUFA and MUFA. They (partial and total) also had lower daily intake of alcohol and cholesterol and higher intake of fibres, n-3 and n-6 PUFA. Total avoiders had lower intake of complex carbohydrates and higher intake of simple carbohydrates compared with partial avoiders. Regarding micronutrients and minerals intake, gluten avoiders exhibited higher intake except for Ca, retinol, Zn and Na (total avoiders > partial avoiders > non-avoiders).
Table 4. Energy intake, contribution of macronutrients to energy intake and mean micronutrient intake among total, partial and non-gluten avoiders
(Mean values and 95 % confidence intervals)
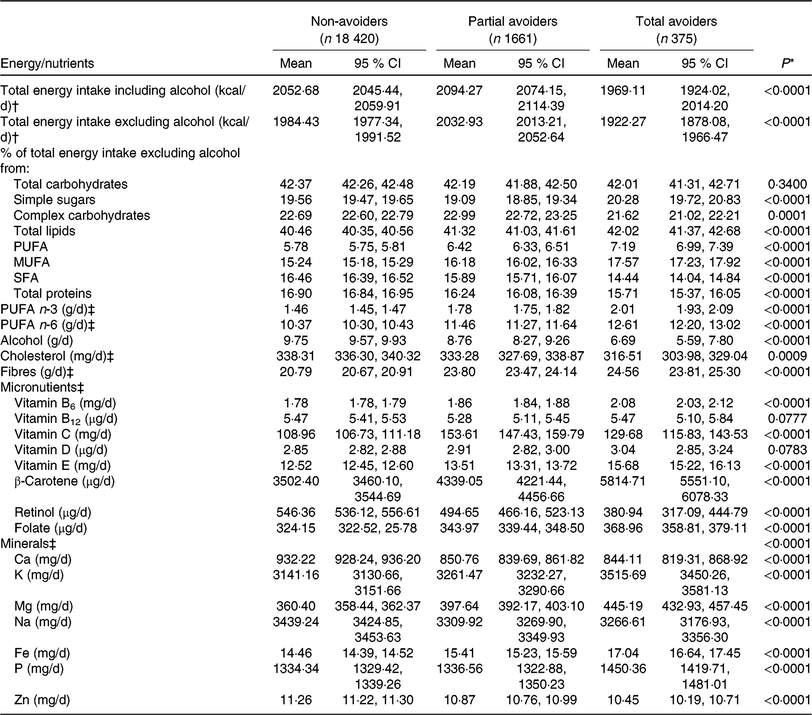
* P values are based on the ANCOVA test, adjusted for age and sex.
† To convert energy in kcal to kJ, multiply by 4·184
‡ Adjusted for total energy intake (without alcohol) using the residual method.
Dietary pattern
Three DP explaining 27·57 % of the total variance were identified (online Supplementary Table S2). The first DP was labelled ‘healthy’, it was characterised by a high consumption of fruits, vegetables, legumes, whole starchy foods, oils, sugar-free drinks and a low consumption of meat, processed meat, refined starchy foods, salty/sweet and fatty foods, sugary drinks, alcoholic beverages. The second DP was labelled ‘traditional’, it was characterised by a high consumption of potatoes and other tubers, added fats, meat, legumes, refined starchy foods, processed meat, alcoholic beverages and a low consumption of breakfast cereals. The third DP was labelled ‘unhealthy snack’, characterised by a high consumption of dairy products, salty/sweet and fatty foods, breakfast cereals and a low consumption of fish, eggs, alcoholic beverages and oils.
The multinomial logistic regression analysis linking the three groups of gluten avoidance and DP is presented in Table 5. Based on the first model, individuals with higher adherence to the ‘healthy’ DP were more likely gluten avoiders (Q5 v. Q1: OR 3·30 (95 % CI 2·82, 3·86) for partial gluten avoiders, and OR 14·38 (95 % CI 8·82, 23·43) for total gluten avoiders). For the ‘traditional’ DP, an association was only observed among partial gluten avoiders (Q5 v. Q1 only). The ‘unhealthy snack’ DP was negatively associated with gluten avoiding. Results were quite similar after accounting for confounders except for the ‘traditional’ DP showing a positive association with total gluten avoiding (Q5 v. Q1: OR 2·46 (95 % CI 1·65, 3·66) for total avoiders).
Table 5. Multinomial logistic regression analysis showing the association between dietary pattern and gluten avoidance
(Odds ratios and 95 % confidence intervals)

Q, quartile.
* Model 1 adjusted for age and sex.
† Model 2 adjusted for age, sex, education level, occupational category, income, physical activity, smoking status, alcohol, total energy intake without alcohol and number of 24-h records.
Discussion
In this study based on participants from a large nutritional cohort study, investigating for the first time the sociodemographic and dietary characteristics of people avoiding gluten, we found that the percentage of people who avoid gluten was 10·31 %. This prevalence was higher than those reported in the UK, Argentina, Salvador and Mexico but lower than those reported in Australia and Colombia(Reference Aziz, Lewis and Hadjivassiliou7, Reference Ontiveros, López-Gallardo and Vergara-Jiménez14–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18).
Similar to our findings, all previous studies found a greater proportion of women in gluten avoiders(Reference Aziz, Lewis and Hadjivassiliou7, Reference Ontiveros, López-Gallardo and Vergara-Jiménez14, Reference Cabrera-Chávez, Granda-Restrepo and Arámburo-Gálvez16–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18, Reference DiGiacomo, Tennyson and Green22, Reference Christoph, Larson and Hootman24, Reference Reilly37, Reference van Gils, Nijeboer and IJssennagger38). Concerning age and level of education, gluten avoiders in our study were more likely to be older people and with a lower educational level. Some studies are in line with our results(Reference Ontiveros, López-Gallardo and Vergara-Jiménez14, Reference Cabrera-Chávez, Granda-Restrepo and Arámburo-Gálvez16, Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18, Reference DiGiacomo, Tennyson and Green22, Reference Christoph, Larson and Hootman24), whereas others are not(Reference Cabrera-Chávez, Dezar and Islas-Zamorano17, Reference van Gils, Nijeboer and IJssennagger38). The other studied characteristics were not reported in previous studies. However, we observed that gluten avoiders were more likely to have children in the household but an opposite association was reported in a previous study(Reference Christoph, Larson and Hootman24). In our study, occupational category, income level and the BMI were also different between people who totally or partially avoiding gluten. Regarding the BMI, total avoiders were not different to non-avoiders, whereas partial avoiders presented more often obesity. While our study is cross-sectional limiting causal inference, some studies reported a large increase in BMI after adopting a GFD, but they focused only on patients with CD(Reference Dickey and Kearney39, Reference Kabbani, Goldberg and Kelly40). However to the best of our knowledge, no published data support a weight loss or a weight gain among people without CD following a GFD. Beside the fact that gluten avoiders exhibited higher energy intake, several hypothesis can explain this finding: first, many studies reported that people who avoid gluten often declared weight control as motives(Reference Gaesser and Angadi12, Reference Gaesser and Angadi13, Reference Cabrera-Chávez, Dezar and Islas-Zamorano17, Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18). It is possible that these participants who avoid gluten to lose weight are therefore overweight(Reference Julia, Péneau and Andreeva41). A second hypothesis would be the consumption of gluten-free substitutes, known to contain more energy, carbohydrates, Na and lipids(Reference Miranda, Lasa and Bustamante21).
Concerning the reasons to avoid gluten, our results are in line with previous studies reporting that a GFD is perceived healthier, but also for personal taste or preference(Reference Golley, Corsini and Topping15–Reference Dunn, House and Shelnutt19, Reference Lu, Zhang and Luoto42). Our results showed that participants avoiding gluten were also more prone to exclude foods not containing gluten, to have allergies and also to adhere to a lactose-free diet. This is in accordance with previous studies that reported multiple food sensitivities and allergies(Reference Aziz, Lewis and Hadjivassiliou7, Reference Golley, Corsini and Topping15–Reference Cabrera-Chávez, Dezar and Islas-Zamorano17, Reference Volta, Bardella and Calabrò43, Reference Tavakkoli, Lewis and Tennyson44), particularly lactose intolerance(Reference Golley, Corsini and Topping15–Reference Cabrera-Chávez, Dezar and Islas-Zamorano17, Reference Volta, Bardella and Calabrò43, Reference Gaillard45). In 2015, an Australian study, using data obtained through the Commonwealth Scientific and Industrial Research Organisation (CSIRO) Food and Health Survey and including adults aged 18 years and older reported that more than half of people avoiding gluten also avoided dairy products(Reference Golley, Corsini and Topping15). In New Zealand, a study showed that medical diagnosis of lactose intolerance was a strong predictor of gluten avoidance in children(Reference Tanpowpong, Ingham and Lampshire9).
Studies that reported nutritional intake in GFD have mainly focused on people with CD(Reference Vici, Belli, Biondi and Polzonetti46–Reference Wild, Robins and Burley48). The few studies conducted in healthy people provided inconsistent results and involved small samples(Reference DiGiacomo, Tennyson and Green22–Reference Devlin25, Reference Tavakkoli, Lewis and Tennyson44). Unlike our study, the study conducted by Delvin(Reference Devlin25), including fifty-eight participants (twenty-five persons with GFD) reporting their food consumption over a 5-d period, found inadequate intake such as lower intake of carbohydrates, fibres, folate, Ca and vitamin B, but higher intake of lipids and Na in those with GFD. Several studies did not detect any difference in energy and macronutrients intakes comparing people who avoid or not gluten(Reference DiGiacomo, Tennyson and Green22, Reference De Palma, Nadal and Collado23, Reference Tavakkoli, Lewis and Tennyson44). Similar to a previous study conducted in 2018 in the USA(Reference Christoph, Larson and Hootman24), our results suggested that individuals avoiding gluten have an overall better nutritional profile. However, information about the consumption of gluten-free substitutes was limited in our sample, which may have affected the estimation of nutrient intakes related to these foods. Nevertheless, participants avoiding gluten reported greater consumption of fruits and vegetables and fewer sugary drinks. Their diet is also characterised by a low consumption of processed foods (salty/sweet and fatty foods including cakes, fatty foods), which generally contain more gluten, and by increasing the consumption of unprocessed foods such as fruits and vegetables. People avoiding gluten exhibited a healthier diet as shown by the analysis of DP. This result was is in line with the study conducted by Christoph et al. (Reference Christoph, Larson and Hootman24) that reported a healthy behaviour among people avoiding gluten. In this study, people avoiding gluten-valued unprocessed foods and had a higher consumption of fruit and vegetables. This point is also in accordance with the health-related motives advanced by the participants.
Our study was subject to some limitations. First, participants enrolled in our study were volunteers in a nutrition cohort and had probably higher health consciousness and interest in nutritional issues than the general population. This may lead to particular characteristics, in particular, a healthier food profile, when compared with the general French population(Reference Andreeva, Salanave and Castetbon49, Reference Andreeva, Deschamps and Salanave50). In addition, the optional nature of the questionnaire on food exclusions may have exacerbated this selection bias, and this can result in an overestimated prevalence of individuals excluding foods. To counteract this issue, all analyses were weighted on the national census data. Second, data collection was based on self-reported questionnaires which are prone to measurement errors. A third limit concerns the list of motives in the questionnaire which were the same for different types of selective diet and were not specific to gluten. In particular, different gastro- and extra-intestinal symptoms related to gluten consumption were not assessed. Fourth, food exclusion questionnaires did not collect information about the date of beginning a gluten-free avoidance and dietary records did not take into account gluten-free products. Hence, it was not possible to know when a person declared eating a product (i.e. bread) if it was gluten-free or not. Taking dietary records into account over a 2-year period preceding the questionnaire may seem inappropriate and a shorter period could have been chosen, because we have no information on their date of beginning of avoidance. However, it would not be representative of a person’s dietary habits. As food consumption presented large differences between people avoiding gluten and those do not avoid it, this limitation should have low impact on our results, and if it was the case, the differences would probably be even underestimated. Finally, our study was cross-sectional, and because of a potential reverse-causality, participants who adopted a healthy diet may be more likely to avoid gluten.
Our study had also important strengths. First, to the best of our knowledge, this was the first study evaluating the sociodemographic characteristics and dietary profile of people who avoid gluten within such a large sample from the general population, and especially in a French sample. Second, given the large sample size of the NutriNet-Santé cohort, and because participants are interested in nutritional issues, we had an access to a large population of gluten avoiders. This led to a high statistical power and to have a variety of DP. Third, the variety of available data allowed to control for confounding factors. Fourth, all analyses were weighted on national data to be more representative of the French population. Then, we used validated tools to assess dietary data, using repeated and detailed dietary records(Reference Touvier, Kesse-Guyot and Méjean31, Reference Lassale, Castetbon and Laporte32). All these data allowed us to describe the sociodemographic and nutritional characteristics, as well as the lifestyle of people who avoid gluten. Indeed, previous studies were generally limited to sociodemographic characteristics and motives. Finally, we used a questionnaire including a very large number of food exclusions, not specific to gluten, unlike some studies(Reference Ontiveros, López-Gallardo and Vergara-Jiménez14, Reference Cabrera-Chávez, Granda-Restrepo and Arámburo-Gálvez16–Reference Ontiveros, Rodríguez-Bellegarrigue and Galicia-Rodríguez18) allowing a comprehensive depicting.
Conclusion
The present study is the first to provide a comprehensive description of dietary pattern related to gluten avoiding among persons without CD. More research is needed to confirm the association between healthy dietary pattern and gluten avoidance taking into account accurate data about nutrient composition of gluten-free foods as well as intake of non-nutritional components. Finally, further longitudinal studies are required to assess the long-term health effects of avoiding gluten among people without CD.
Acknowledgements
The authors warmly thank all the volunteers of the NutriNet-Santé cohort. We also thank Younes Esseddik, Frédéric Coffinieres, Thi Hong Van Duong, Paul Flanzy, Régis Gatibelza, Jagatjit Mohinder and Maithyly Sivapalan (computer scientists), Cédric Agaesse (dietitian), Julien Allègre, Nathalie Arnault, Laurent Bourhis, Véronique Gourlet, PhD and Fabien Szabo de Edelenyi, PhD (data-managers/biostatisticians) and Nathalie Druesne-Pecollo, PhD (operational coordinator) for their technical contribution to the NutriNet-Santé study.
This study is part of the GlutN project that was supported by the French National Research Agency (Agence Nationale de la Recherche) in 2017 (AAPG ANR 2017).
The NutriNet-Santé cohort study is funded by the following public institutions: Ministère de la Santé, Santé Publique France, Institut National de la Santé et de la Recherche Médicale, Institut National de la Recherche Agronomique (INRA), Conservatoire National des Arts et Métiers (CNAM) and Paris 13 University. The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript. Study sponsors had no part in study design, collection, analysis and interpretation of data and the writing of the article and the decision to submit it for publication.
The study sponsors played no role in the design and conduct of the study; collection, management, analysis and interpretation of the data; and preparation, review or approval of the manuscript.
The authors’ contributions were as follows – L. P. and E. K. G.: designed the research; B. A., C. B., C. R., C. J., S. H. and E. K. G.: conducted the research; L. P.: performed statistical analysis and drafted the manuscript; E. K. G.: supervised statistical analysis and the writing; L. P., B. A., C. B., C. R., C. J., S. H. and E. K. G.: contributed to the data interpretation and revised each draft for important intellectual content. All authors read and approved the final manuscript. E. K. G. had primary responsibility for the final content; she is the guarantor.
The other authors declared no support from any institution for the submitted work.
Supplementary material
For supplementary material for this article, please visit https://doi.org/10.1017/S0007114519001053









