Background
Severe health anxiety is a highly disabling and costly disorderReference Fink, Ornbol and Christensen1,Reference Tyrer, Cooper, Crawford, Dupont, Green and Murphy2 affecting approximately 1–5% of the adult population.Reference Fink, Ornbol, Toft, Sparle, Frostholm and Olesen3,Reference Sunderland, Newby and Andrews4 It is characterised by exaggerated rumination with fears of suffering from a serious illness.Reference Fink, Ornbol, Toft, Sparle, Frostholm and Olesen3 In DSM-5, health anxiety is now classified as illness anxiety disorder or somatic symptom disorder if severe somatic symptoms are present, respectively.5 Even though empirically supported psychological therapies for health anxiety exist,Reference Cooper, Gregory, Walker, Lambe and Salkovskis6 the limited availability and barriers to treatment challenge the dissemination and potential impact. Common barriers to psychological treatment are the geographical distance to treatment, the interference with work and daily life, and the fear of stigmatisation.Reference Perreault, Lafortune, Laverdure, Chartier-Otis, Belanger and Marchand7–Reference Rusch, Angermeyer and Corrigan9 In patients with self-identified health anxiety, a study found that only 20.7% currently received therapy or counselling, and 53.4% reported past experiences with either of these.Reference Soucy and Hadjistavropoulos10 This treatment gap is also widely recognised for common mental disorders.Reference Kohn, Saxena, Levav and Saraceno11 Although patients with health anxiety are frequently seen in medical care settings, they are hesitant to mention their illness worriesReference Tyrer, Cooper, Crawford, Dupont, Green and Murphy2,Reference Tyrer, Eilenberg, Fink, Hedman and Tyrer12 and thus risk a chronic, undetected course.Reference Fink, Ornbol and Christensen1 These barriers call for new approaches to improve access to psychological treatment.
The potential role of self-referral
In many countries, referrals are initiated by a general practitioner (GP) in primary care who serves as a gatekeeper to more specialised services. One of the explicit ideas is that this will result in reduced demand for specialised care, since health clinicians are better informed than patients to make the right referrals.Reference Pichlhofer and Maier13 However, the use of patient self-referral and internet-delivered treatment programmes are recent developments that may improve treatment access and reduce barriers for patients with severe health anxiety.Reference Hoffmann, Rask, Hedman-Lagerlof, Ljótsson and Frostholm14 These innovative programmes consist of highly structured online modules with homework assignments and communication with a clinician via email, telephone or an embedded online forum.Reference Andrews, Basu, Cuijpers, Craske, McEvoy and English15,Reference Andersson and Titov16 The content mirrors the same techniques and material as in traditional face-to-face treatment. Additionally, self-referral where the patients themselves and not healthcare clinicians initiate the treatment contact may help reduce barriers to treatment.
In recent years, self-referral has become increasingly used partly because of the increased amount and quality of online health information making patients more knowledgeable about their conditions and treatment options.Reference Kim, Linker, Coumar, Dean, Matsen and Kim17 However, the accuracy is dependent on patients’ ability to preliminarily self-assess their problems and their need for treatment. At best, self-referral may provide access for patients who for years have remained untreated for their health anxiety.Reference Kohn, Saxena, Levav and Saraceno11 Still, a common concern among healthcare providers is whether the already limited services will primarily be used by people with mild symptoms and limited impairment instead of by those with the highest treatment demand.Reference Brown, Boardman, Whittinger and Ashworth18 Therefore, knowledge about the appropriateness of self-referral among patients with health anxiety as well as which patients use it is needed. This is important for several reasons. First, this question relates to the generalisability of findings from treatment studies. That is, if there are marked differences between patient populations self-referred and clinician-referred, comparisons of effect estimates may be done with caution. Second, knowledge about potential differences or similarities is of great relevance for healthcare providers and policymakers when making prioritisations within a limited healthcare budget. Third, this information is valuable for treatment developers as treatments can be tailored to fit the patients most likely to receive it.
Aims
The present study aims to (a) evaluate the accuracy of self-referral for health anxiety based on the number of patients being clinically assessed to have sufficient levels of health anxiety after a self-referral procedure in relation to a trial of internet-delivered treatment; and (b) explore self-referred patients’ demography (for example age, gender, education) and clinical characteristics in comparison with clinician-referred patients recruited to a trial of face-to-face treatment in the same clinical setting.
Method
Setting and participants
This study took place at the Research Clinic for Functional Disorders and Psychosomatics at Aarhus University Hospital, Denmark, which is a specialised unit with a combined research objective and a routine clinical function. Participants were retrieved from two separate randomised controlled trials (RCTs, trial registration: clinicaltrials.gov: NCT01158430 and NCT02735434) conducted in the research clinic. In the primary trial, the patients were recruited through self-referral from April 2016 to May 2017 to an internet-delivered acceptance and commitment therapy programme (iACT),Reference Hoffmann, Rask, Hedman-Lagerlof, Ljótsson and Frostholm14 whereas in the comparison trial the patients were recruited from March 2010 to April 2012 by clinicians working in other hospital settings or in general practice referring patients to a group-based acceptance and commitment therapy programme (ACT-G).Reference Eilenberg, Fink, Jensen, Rief and Frostholm19 Study information was available on the clinic's webpage and sent to GPs in the catchment areas. In the iACT trial, information was also provided on a nationwide anxiety association webpage. In both trials, the recruitment, diagnostic interview and treatment were performed at the research clinic. The treatment content in iACT was based on ACT-G. Thus, the main differences between the two trials were the mode of referral and the face-to-face versus online treatment delivery.
The eligibility criteria were, in general, comparable in the two trials (Table 1). The main exception was the different age limit, which was 18 years or older in the iACT trial compared with 20–60 years in the ACT-G trial. The different catchment areas were both large thus minimising the risk of geographic interference. Furthermore, recent changes in anxiety medication were only an exclusion criterion in the iACT trial where patients, if on pharmacological treatment for their anxiety, had to be on a stable dose for 2 months prior to treatment initiation. In total, 227 patients with severe health anxiety were included; 101 self-referred patients from the iACT trial (the self-referred group) and 126 clinician-referred patients from the ACT-G trial (the clinician-referred group).Reference Eilenberg, Fink, Jensen, Rief and Frostholm19
Table 1 Recruitment and eligibility criteria

ACT-G, group-based acceptance and commitment therapy programme; iACT, internet-delivered acceptance and commitment therapy programme; SCAN, Schedules for Clinical Assessment in Neuropsychiatry.
a. Trial reported by Eilenberg et al.Reference Eilenberg, Fink, Jensen, Rief and Frostholm19
b. Diagnostic, empirically-based criteria by Fink and colleagues.Reference Fink, Ornbol, Toft, Sparle, Frostholm and Olesen3
c. Established cut-off for non-clinical cases based on Whiteley Index-7 score >21.4 (scale range 0–100).Reference Fink, Ornbol and Christensen1
d. Schedules for Clinical Assessment in Neuropsychiatry: a semi-structured clinical diagnostic interview.
The two studies were approved by the Ethical Committee in Central Region Denmark (iACT ID: 1-10-72-321-15 and ACT-G ID: 20090201) and the Danish Data Protection Agency (iACT case: 1-16-02-51-16 and ACT-G case: 1-16-02-40-13). All participants provided written informed consent.
Referral and assessment procedures
In the iACT trial, patient self-referral was carried out through a web portal through the research clinic's webpage. The self-assessment and referral was enhanced by extensive online information encompassing two patient videos about health anxiety and internet-delivered treatment, a guide on how to self-refer, and core criteria on health anxiety. Interested patients logged in using their unique Danish personal identification number and completed a baseline questionnaire. All self-referrals were preliminarily screened by a psychologist from the research clinic (D.H.) in accordance with the eligibility criteria. Subsequently, patients were invited for a diagnostic interview.
In the ACT-G trial, the clinician-referrals were primarily carried out by the patient's GP or by a clinician in another hospital department. The referrals were subsequently screened by medical doctors from the research clinic in accordance with the eligibility criteria and eligible patients were invited for a diagnostic interview. Patients completed a baseline questionnaire prior to this interview. This procedure has been thoroughly described elsewhere.Reference Eilenberg, Fink, Jensen, Rief and Frostholm19
Patients in both groups underwent a thorough diagnostic interview with the semi-structured interview Schedules for Clinical Assessment in Neuropsychiatry (SCAN) assessing both health anxiety and comorbid disorders.20 In both groups, experienced clinicians trained in using SCAN conducted the diagnostic interviews (one psychiatrist and four to five psychologists in each trial). However, patients in the clinician-referred group underwent the interview face-to-face, whereas patients in the self-referred group underwent the interview via video conferencing. The video-based SCAN interview was modified and shortened based on a procedure from a large Danish epidemiology studyReference Dantoft, Ebstrup, Linneberg, Skovbjerg, Madsen and Mehlsen21 (1–2 h) compared with the longer face-to-face interview (3–4 h). This modification pertained primarily to the length of history taking and amount of psychoeducation provided at the time of the interview. Both versions covered clinical questions regarding health anxiety, depression and obsessive–compulsive disorder (OCD). The number of questions regarding other anxiety disorders and somatoform disorders were reduced in the video session. Video-recorded diagnostic interviews were discussed, and consensus rating among the assessors was frequently performed in order to secure diagnostic validity and reliability. Non-face-to-face assessment of diagnoses has proven to be a reliable method.Reference Mohr, Burns, Schueller, Clarke and Klinkman22,Reference Hajebi, Motevalian, Amin-Esmaeili, Hefazi, Radgoodarzi and Rahimi-Movaghar23
Study design
This study was a secondary and exploratory analysis based on data from two separate RCTs. We evaluated the accuracy of self-referral by comparing the number of excluded patients in the group of self-referred and clinician-referred patients, respectively. The accuracy of referrals was evaluated based on (a) the number of clinician-excluded patients prior to the diagnostic interview following the initial screening at the research clinic in accordance with the eligibility criteria, (b) the number of patients failing to attend the interview, (c) the number of patients excluded by clinicians following the interview because of ineligibility, (d) the number of patients declining participation, and (e) the total number of eligible patients in the two trials. To explore demographic and clinical characteristics of self-referred patients (for example do they represent less severe cases of health anxiety or do they differ in terms of age, gender, education), eligible self-referred patients were compared with the other sample of clinician-referred patients with severe health anxiety. Demographic variables were measured by self-report questionnaires. Clinical characteristics partly comprised self-report measures, as well as clinician-assessed illness onset, duration and comorbidity assessed at the diagnostic interview. In both groups, all questionnaires were administered before treatment start.
Measures
Accuracy of self-referral versus clinician-referral
The accuracy of self-referral was evaluated based on the number of excluded self-referred and clinician-referred patients prior to the diagnostic interview, following the diagnostic interview and in total.
Sociodemographic characteristics
This included the self-reported variables of age, gender, living status, highest education qualification, employment status and current sick leave.
Clinical characteristics
Health anxiety severity
We measured health anxiety severity using a seven-item version of the Whiteley Index (Whiteley-7),Reference Fink, Ewald, Jensen, Sorensen, Engberg and Holm24 assessing worrying and convictions about illness. The Whiteley-7 employs a five-point Likert scale from 1, ‘not at all’ to 5, ‘a lot’ with a scale range from 7 to 35. It includes items such as ‘Do you worry a lot about your health’. Higher scores indicate more health anxiety. The Whiteley-7 has demonstrated satisfactory internal validity in a Danish primary care sample and good external validity for screening DSM-IV somatisation disorder and hypochondriasis.Reference Fink, Ewald, Jensen, Sorensen, Engberg and Holm24,25 In the present study, the internal consistency was α = 0.88 and 0.77 for ACT-G and iACT, respectively.
Health anxiety onset and duration
This was calculated based on the patient-reported onset of health anxiety noted by the clinician at the diagnostic SCAN interview.
Clinically assessed comorbidity
Comorbidity encompassing depression, anxiety disorders and OCD was summarised based on the diagnostic SCAN interview using the diagnostic classification of the 10th edition of the International Classification of Diseases and Related Health Problems (ICD-10).26
Emotional distress, somatic symptoms and obsessive–compulsive symptoms
These were all measured using questions from the Symptom Checklist scale (SCL-92).Reference Olsen, Mortensen, Bech, Elsass, Ivanouw, Poulsen, Olsen, Mortensen, Bech, Elsass, Ivanouw and Poulsen27 All questions employ a five-point Likert scale from 1, ‘not at all’ to 5, ‘a lot’. Emotional distress was measured on eight items assessing anxiety and depression (SCL-8).Reference Fink, Ornbol, Huyse, De Jonge, Lobo and Herzog28 Items include ‘feeling fearful’ and ‘feelings of worthlessness’ with a scale range from 8 to 40. Higher scores indicate more emotional distress. This brief screening tool has shown good validity in non-psychiatric medical settings in Denmark,Reference Fink, Orbol, Hansen, Sondergaard and De Jonge29 and in the present study, the internal consistency was α = 0.86 in both samples. Somatic symptoms were measured on the 12-item somatisation subscale (SCL-SOM)Reference Derogatis and Cleary30 with a scale range from 12 to 60. This subscale checks for 12 common physical symptoms such as headaches or pains in the heart or chest. Higher scores indicate more symptoms. The internal consistency of the SCL-SOM in this study was α = 0.84 for ACT-G and α = 0.83 for iACT.
Obsessive–compulsive symptoms were measured on the ten-item obsessive–compulsive subscale (SCL-OCD)Reference Kim, Dysken and Kuskowski31 with a scale range from 5 to 50. Higher scores indicate more symptoms, and the subscale includes items such as ‘Having to check and double check what you do’. In the present study, the internal consistency of SCL-OCD was α = 0.85 and 0.88 for ACT-G and iACT, respectively.
Health-related quality of life
We measured on two dimensions of the 12-item Short-Form Health Survey (SF-12),Reference Bjorner, Damsgaard, Watt and Groenvold32,Reference Ware and Maruish33 namely the physical component summary (PCS) and the mental component summary (MCS) with a scale range from 12 to 47. Higher scores indicate better physical and mental health. The internal consistency was high in a large Danish population-based sample, namely α = 0.90 for PCS and α = 0.85 for MCS.Reference Christensen, Ehlers, Larsen and Jensen34
Psychological flexibility
We measured psychological flexibility with the Acceptance and Action Questionnaire (AAQ-II),Reference Bond, Hayes, Baer, Carpenter, Guenole and Orcutt35,Reference Hayes, Strosahl, Wilson, Bissett, Pistorello and Toarmino36 which is a seven-item measure encompassing questions like ‘I'm afraid of my feelings’. Overall, psychological flexibility assesses patients’ ability to behave flexibly when distressing thoughts and feelings are present. Items are rated on a seven-point Likert scale from 1, ‘never true’ to 7, ‘always true’ with a scale range from 7 to 49. The scale was reversed with higher scores indicating more flexibility and less experiential avoidance. The AAQ-II has shown a mean Cronbach's alpha coefficient of 0.84 (ranging from 0.78 to 0.88) and good test–retest reliability at 12 months (α = 0.79) across six different samples.Reference Bond, Hayes, Baer, Carpenter, Guenole and Orcutt35 In the present study, the internal consistency was α = 0.88 for ACT-G and α = 0.86 for iACT.
Non-reactivity
We measured non-reactivity with the seven-item subscale of the Five Facet Mindfulness Questionnaire (FFMQ non-react).Reference Baer, Smith, Lykins, Button, Krietemeyer and Sauer37 This facet of mindfulness covers the ability to be non-reactive towards inner experiences such as thoughts, feelings and bodily sensations. Questions such as ‘I perceive my feelings and emotions without having to react to them’ are rated on a five-point Likert scale from 1, ‘never or very rarely true’ to 5, ‘very often or always true’ with a scale range from 7 to 35. Higher scores of non-reactivity indicate less avoidance. The FFMQ has shown good psychometric properties with a Cronbach's alpha coefficient ranging from 0.72 to 0.92.Reference Baer, Smith, Lykins, Button, Krietemeyer and Sauer37 Non-reactivity is the only subscale of the FFMQ found to mediate a positive treatment outcome in treatment for severe health anxiety across two studies.Reference Eilenberg, Hoffmann, Jensen and Frostholm38,Reference Hedman, Hesser, Andersson, Axelsson and Ljotsson39 In the present study, the internal consistency of the FFMQ non-react was α = 0.76 for ACT-G and α = 0.88 for iACT.
Statistical analysis
The number of patients with clinically relevant health anxiety consenting to treatment was compared using equality of proportions z-test based on excluded patients following self-referral and clinician-referral. The distribution of all other data was judged by inspection of QQ plots. Sum scores that followed a normal distribution were summarised using the mean and standard deviation, whereas sum scores not following a normal distribution were summarised using the median and interquartile range. The mean differences in continuous data were compared between the two groups using independent two-sample t-tests, whereas categorical data were analysed using χ2-tests or Fisher's exact test for small sample sizes. All symptom scales were converted into a scale range 0–100 points (((score – min)/(max – min)) × 100). One variable – duration of health anxiety – was not normally distributed and was thus analysed using the Wilcoxon rank-sum (Mann–Whitney) test. To check the impact of the different age criteria in the two groups, a subanalysis comparing only participants from 20 to 60 years of age across the groups was performed. The multiple variables compared between these study populations are exploratory; hence we did not do any formal correction for P-values. Instead, we provided exact P-values for each test. Analyses were performed using Stata version 13 for Windows. Statistical significance was set at P<0.05 using two-tailed tests.
Results
Accuracy of self-referral versus clinician-referral
In total, 151 patients self-referred to the iACT trial and 254 patients were referred by a clinician to the ACT-G trial (Fig. 1). Out of these patients, 101/151 (67%) self-referred patients were finally included for the primary trial compared with 126/254 (50%) of the clinician-referred patients for the comparison trial (z = −3.39, P = 0.001). This significant difference pertained to pre-assessment where clinician-referred patients to a larger extent failed to attend the diagnostic interview (z = −3.03, P = 0.003) and were excluded based on the eligibility criteria by the screening clinicians in the research clinic (z = −2.68, P = 0.007). There were no differences found in eligibility for trial participation between patients undergoing the diagnostic interview in the two groups. The overall participation rate was high in both trials, i.e. 98/101 (97%) self-referred patients and 116/126 (92%) clinician-referred patients completed questionnaires at the end of treatment (z = −1.08, P = 0.282).

Fig. 1 Flow chart of recruitment.
Sociodemographic characteristics
Sociodemographic characteristics of the included patients in the two trials are displayed in Table 2. The mean age of self-referred patients was significantly higher than those referred by a clinician with a mean difference of 3.4 years (95% CI 0.9–5.8, t(225) = 2.69, P = 0.008). A secondary analysis controlling for the different age criterion in the two trials by excluding patients in the iACT trial younger than 20 years and older than 60 years found a significant 3.3-year mean difference in age between groups (95% CI 0.9–5.7, t(219) = 2.76, P = 0.006). Furthermore, there was a significant difference in educational qualification between the groups showing that 25/101 (25%) of self-referred patients had more than 4 years of higher education (for example university-level education) compared with 15/123 (12%) of the clinician-referred patients (χ2(4) = 10.69, P = 0.030). There were no differences in gender distribution, living status or employment status. Even though not significant, a higher proportion of clinician-referred patients were on full-time sick leave (15%) than the self-referred patients (7%) (χ2(3) = 3.91, P = 0.271).
Table 2 Demographic characteristics
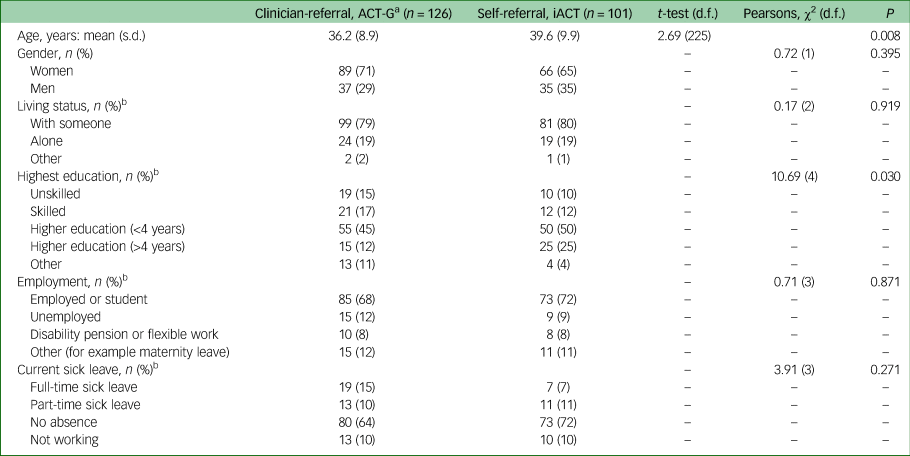
ACT-G, group-based acceptance and commitment therapy programme; iACT, internet-delivered acceptance and commitment therapy programme.
a. Eilenberg et al.Reference Eilenberg, Fink, Jensen, Rief and Frostholm19
b. Missing data in the ACT-G sample for living status (n = 1), highest education (n = 3), employment (n = 1) and current sick leave (n = 1).
Clinical characteristics
Self-referred patients reported more symptoms of health anxiety compared with the clinician-referred patients (Table 3). The mean difference between groups was 5.6 points (95% CI 1.0–10.2, t(224.80) = 2.38, P = 0.018). Patients in both groups had an average onset of health anxiety in their early twenties, and no difference in health anxiety duration was found. In terms of clinical comorbidity, self-referred patients had fewer clinician-assessed comorbid anxiety disorders (χ2(1) = 12.86, P<0.001).
Table 3 Clinical characteristics
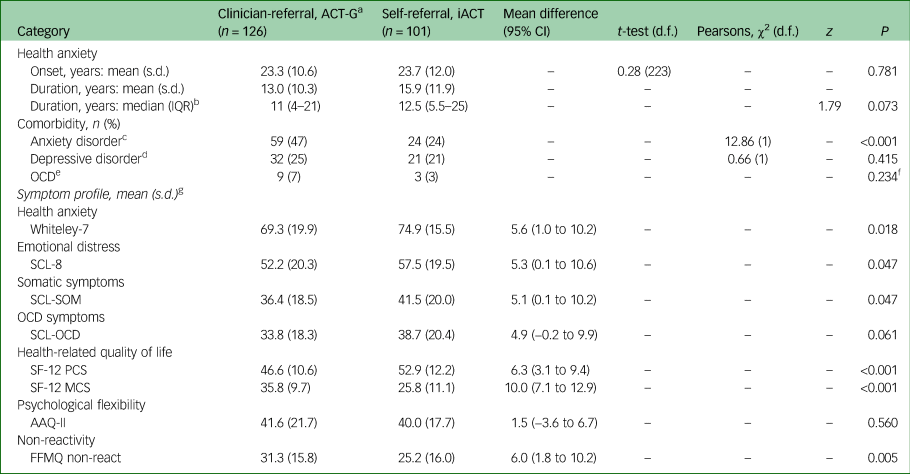
ACT-G, group-based acceptance and commitment therapy programme; iACT, internet-delivered acceptance and commitment therapy programme; z, Wilcoxon rank-sum (Mann–Whitney); OCD, Obsessive–compulsive disorder; SCL, Symptom Checklist; SOM, Somatisation; SF-12, Short-Form Health Survey; PCS, Physical Component Summary; MCS, Mental Component Summary; AAQ, Acceptance and Action Questionnaire; FFMQ, Five Facet Mindfulness Questionnaire.
a. Eilenberg et al.Reference Eilenberg, Fink, Jensen, Rief and Frostholm19
b. Median and interquartile range reported because of a skewed distribution.
c. ICD-10 (F40.0-F40.2; F41.0-F41.1).
d. ICD-10 (F32.0-F32.2; F33.0-F33.2).
e. ICD-10 (F42.0-F42.1).
f. Fisher's exact test.
g. High score, more symptoms, except for health-related quality of life, psychological flexibility and non-reactivity.
As opposed to this, the self-referred patients reported higher levels of emotional distress and somatic symptoms compared with the clinician-referred patients. Also, they had a lowered mental health-related quality of life with a mean difference of 10.0 points (95% CI 7.1–12.9, t(201) = −6.85, P<0.001) in comparison with the clinician-referred patients, whom in contrast reported 6.3 points lower physical health-related quality of life (95% CI 3.1 to 9.4, t(201) = 3.92, P<0.001). There was no difference between the two groups’ level of obsessive–compulsive symptoms.
Moreover, the self-referred patients were more reactive compared with the clinician-referred patients as shown by a 6.0 points lower non-reactivity towards distressing thoughts, feelings and images (95% CI 1.8 to 10.2, t(224) = −2.83, P = 0.005). In addition, both groups had comparable and low psychological flexibility namely 40.0 (s.d. = 17.7) in the self-referred group and 41.6 (s.d. = 21.7) in the clinician-referred group. Both groups were below the suggested cut-off score for clinically relevant distress of 50.0–59.5 (scale range 0–100, i.e. >24–28 (scale range 7–49) on the original non-reversed and transformed scale).Reference Bond, Hayes, Baer, Carpenter, Guenole and Orcutt35
Discussion
This study evaluated the accuracy of self-referral in patients with severe health anxiety. The main findings were the greater percentage of patients found to have sufficient levels of health anxiety after a self-referral procedure in relation to a trial of internet-delivered treatment compared with clinician-referred patients recruited to a trial of face-to-face treatment in the same clinical setting. The broader question for this study was whether patients with severe health anxiety seeking treatment through self-referral differed on clinical characteristics from clinician-referred patients in these two trials. Overall, the results suggest that relevant patients self-referred. In fact, the self-referred patients had more symptoms of health anxiety, emotional distress and poorer mental health-related quality of life. In addition, they were more reactive towards distressing thoughts, feelings and images. This indicates that their need for treatment was at least comparable with the clinician-referred patients.
On the other hand, the self-referred patients had less clinician-assessed psychiatric comorbidity and better physical-health-related quality of life, which might suggest a more distinct symptom profile of self-referred patients. Furthermore, the self-referred group had a somewhat higher educational level and was slightly older, but there was no statistically significant difference in age at onset and duration of health anxiety between the groups. Even though the two patient groups differed, the differences were relatively minor. All in all, this suggests that self-referral can be an accurate method to recruit patients with health anxiety and possibly is non-inferior compared with clinician-referral.
Accuracy of patient self-referral
We found that 19% less clinician-referred patients were eligible for the diagnostic interview compared to the self-referred patients. This was partly because of more patients being excluded by clinicians at the research clinic (for example only presenting subclinical health anxiety symptoms) and partly because the clinician-referred patients more frequently failed to attend the diagnostic interview (i.e. declining participation without a reason or having improved in symptoms).
There can be several reasons for declining participation such as low motivation, lack of acceptance of the diagnosis and the treatment plan or barriers to assessment (for example transportation, going to a hospital). Self-referring patients may be more motivated when they initiate the treatment contact themselves, and barriers may be reduced when patients can undergo the diagnostic interview via video conferencing in their own home. However, many clinician-referred patients’ symptoms also improved during the relatively longer waiting time for the diagnostic interview as compared with the faster procedure following self-referral. This might suggest that the more direct and faster pathway through self-referral may result in treatment initiation of some patients whose condition would have improved anyway. On the other hand, health anxiety tends to fluctuate but reoccur if left untreated.Reference Fink, Ornbol and Christensen1 Hence, self-referral may increase chances of timely treatment initiation.
There may be many possible explanations why self-referral seemed to be more accurate than clinician-referral in this study (for example motivation, less barriers to assessment and a faster procedure). As our results are based on only one trial applying a specific self-referral procedure with extensive patient educational material in a particular setting (Danish public healthcare system), we cannot draw any conclusions regarding self-referral for health anxiety in general. Only one other trial relied solely on self-referral for recruiting patients with health anxiety.Reference Newby, Smith, Uppal, Mason, Mahoney and Andrews40 In this internet-delivered cognitive–behavioural therapy trial, 495 patients commenced self-referring, 197 never completed the online procedure and only 102 patients were found eligible. This resulted in a total of 102/298 (34%) patients compared with 101/151 (67%) patients in our trial undertaking the treatment. Therefore, the accuracy of self-referral may depend on the individual procedure. Unfortunately, the self-referral procedure was not described by Newby and colleagues hampering a further comparison between the trials. However, it may well be that simply advertising is not sufficient. Our self-referral procedure was based on patient education material consisting both of clinical information and patient videos. This may have enhanced the accuracy in our study. Most clinical trials on health anxiety use a combination of self-referral and clinician-referrals from hospital settings or general practice.Reference Cooper, Gregory, Walker, Lambe and Salkovskis6 However, an efficient self-referral system has the potential to be cost-effective in that clinicians do not use resources related to referral, and therapists do not waste as much time waiting for unmotivated patients failing to attend an assessment.
Patient characteristics preceding recruitment
Self-referral has often been used as one recruitment method alongside clinician-referral in internet-delivered trials and results show that relevant patients tend to be captured across different psychiatric disorders.Reference Titov, Andrews, Kemp and Robinson41–Reference Wootton, Titov, Dear, Spence and Kemp43 However, self-referred patients generally tend to be better educated,Reference Andersson and Titov16 which was also the case in our study. We also found some support for the suggestion that self-referred patients may have a more distinct symptom profile in terms of less comorbidity and better physical-health-related quality of life compared with patients referred from primary care. This may seem contradictory since the self-referred patients also had higher levels of self-reported health anxiety symptoms and overall distress. However, the results also showed that self-referred patients were more reactive towards inner experiences compared with clinician-referred patients.Reference Baer, Smith, Lykins, Button, Krietemeyer and Sauer37 This is proposed to be a central mechanism in health anxiety,Reference Eilenberg, Hoffmann, Jensen and Frostholm38,Reference Hedman, Hesser, Andersson, Axelsson and Ljotsson39 and patients who are more reactive towards inner experiences might also be more inclined to search the internet for reassurance and seek treatment in a peak episode of health anxiety.Reference Muse, McManus, Leung, Meghreblian and Williams44 Therefore, the higher levels of distress could reflect that patients self-referred in a peak episode of health anxiety.
Self-referral may address patients with certain characteristics, or even require certain levels of illness recognition or health literacy to find and use a self-referral system.Reference Bo, Friis, Osborne and Maindal45 Even though these speculations need further investigation, it is important to consider possible health inequalities if access is only granted through self-referral. On the other hand, only relying via clinician-referral may limit access to the more avoidant patients who tend to avoid health professionals and hospitals because of their fear of illness.
Strengths and limitations
The strengths of this study were the large number of participants from two RCTs carried out in the same research clinic. The amount of similar clinical data available in both trials enabled a comprehensive comparison. Furthermore, the empirically established diagnostic criteria and diagnostic interviews applied in the two trials ensured that the differences between the two patient groups were less likely to be caused by inclusion of different patient populations. The main limitation of this study was the different catchment areas entailing a risk that the patients may differ as a result of geographics rather than recruitment method. However, the catchment areas were both large (i.e. 2.5 to 5.7 million people), which reduces the risk considerably. Furthermore, the different recruitment periods with a few years in between might suggest that the two patient groups differ as a consequence of changing referral patterns over time rather than the different referral procedures and treatment preferences per se. However, ACT-G was also available in regular care, during the period when iACT recruited patients through self-referral, and information about both treatments was available on the clinic's webpage and through the GPs. Thus, patients self-referring to iACT probably preferred this treatment format. Also, as for the clinician-referred patients, we do not know the relative proportion of GP and hospital clinician referrals. There could be a difference in accuracy between specialties, that is, GPs might be more literate in picking up health anxiety, which would mean the results do not generalise to all clinicians. This needs further investigation.
Finally, the slightly different eligibility criteria may have affected the characteristics of the included patients. The main difference in inclusion criteria between the trials was the age criteria, which turned out not to affect the results. Even though the two RCTs were not set up for this comparison, the large trials and overall comparability enabled an investigation of an important but largely unexplored area.
Clinical implications and future perspectives
Although the results of this study may primarily inform future study designs regarding the choice of recruitment method, they were based on two trials that were both embedded in a specialised hospital unit with a routine clinical function. Therefore, the results may also have some clinical implications. This study found that self-referral for psychological treatment seemed to work well in a patient population that most commonly seek medical reassurance or simply avoid the healthcare system. Patients with severe health anxiety were capable of preliminary self-assessment and self-referral to treatment. From a broader clinical perspective, self-referral and internet-delivered treatment ensure equal access to treatment for patients living in rural areas or patients simply not wishing to have face-to-face treatment. Instead of treating all patients similarly, different ways of accessing treatment and modes of delivery enable a higher degree of individually tailored treatment. The increase in behavioural intervention technologies may have considerable implications for the delivery of future healthcare services.Reference Mohr, Burns, Schueller, Clarke and Klinkman22
National initiatives such as the English Improving Access to Psychological Therapy (IAPT) harness the internet to bridge the treatment gap by employing internet-delivered treatment and now self-referral for the treatment of depression and anxiety.Reference Clark46 They have found that self-referred patients more accurately mirrored the general population including minority groups, who are often underrepresented among clinician-referrals. Harnessing technology in the dissemination of healthcare services has only just begun, and the future implications are numerous.Reference Holmes, Ghaderi, Harmer, Ramchandani, Cuijpers and Morrison47 To start with, self-referral may generalise to other psychiatric disorders, and in the case of severe health anxiety, it may be a feasible supplement to clinician-referral. There is a need for studies directly comparing different recruitment methods in the same clinical trial to further investigate patient preferences and possible predictors for treatment outcome such as motivation.
In conclusion, patient self-referral and clinician-referral are both feasible and valid methods for recruiting patients with severe health anxiety although they may recruit patients with different characteristics. We found that the self-referred patients had higher levels of health anxiety and poorer mental health-related quality of life compared with the clinician-referred patients, underlining that self-referral is not primarily undertaken by people with mild symptoms and limited impairment. In addition, the self-referred patients were slightly older, better educated and had less comorbid anxiety disorders. Thus, allowing self-referral may lower barriers to treatment for a group of patients with considerable distress and a more distinct symptom profile.
Funding
This research was supported by the Danish foundation TrygFonden (grant numbers: 102644). The funding sources were not involved in designing and conducting the study or preparing this manuscript for publication.
Acknowledgements
We would like to thank PhD Tina Carstensen, psychologists Greta Lassen Lund and Katrine Ingeman Beck from the Research Clinic for Functional Disorders and Psychosomatics at Aarhus University Hospital for assisting with the diagnostic interviews and treatment. Also, we thank Jens S. Jensen for statistical assistance and Malene Skjøth for language revision. We would also like to thank all participants in our study.







eLetters
No eLetters have been published for this article.